Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Can My Loved One Prevent Aspiration Pneumonia in ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Manuela, as part of my 1:1 consulting and advocacy service! Manuela’s dad is with a breathing tube and on a ventilator in ICU. Manuela asks how she can make sure that her dad with COVID is well managed in ICU.
How Can I Make Sure That My Dad with COVID is Well-Managed in ICU?

Manuela: I just had a few questions about my father. He’s currently in the ICU. We’re doing a live check-in right now with a doctor. So I’ll just let you hear this really quickly.
Doctor: He’ll open his eyes just a little, but… He’ll open them a little. And then he’s still getting fed and doing well with that. He’s still urinating a good amount. That’s good. And his blood gases are doing well, so they don’t want to turn the paralytic back on. So he’s holding strong for now.
Doods: Okay, awesome.
Doods: Yeah.
Doods: I’m excited.
Doctor: Yeah. Yeah.
Doods: Okay. Oxygen levels, are the numbers the same?
Doctor: So he’s 60% on the ventilator, and he’s been between anywhere between like 91 and 97 today. He had one little coughing where he dropped down to 86, but he was able to bring himself back up. I didn’t even have to go in.
RECOMMENDED:
Doods: Oh, okay.
Doctor: And mess with him. Yeah. So he just needed a minute to recover and he was fine.
Doods: Okay. Yeah. He’s a strong person. He’s a fighter. He…
Doctor: Yeah. I can tell.
Doods: He has nine kids and he keeps us in line. So, yeah.
Doctor: Yeah.
Doctor: Okay, and did you have any questions?
Manuela: No questions at the moment.
Doctor: Okay. Oh my, I apologize again. I’m so sorry I missed your call earlier.
Doods: No, it’s fine, it’s my fault. It’s just that I’m the only one there. So, you know…
Doctor: I appreciate you guys.
Doods: A quick question..
Doctor: Yeah.
Doods: Is there any way we can do a quick Zoom, before you guys leave?
Doctor: Yeah, let me figure it out. Wait, do you want to just do what we did last time?
Doods: Yeah. I think it was with the iPad you used, right?
Doctor: Okay, yeah. So give me just one minute, okay?
Doods: Okay.
Doctor: Are you ready now or no?
Doods: I have to update everyone in the family. I’ll send back a text real quick.
Doctor: Okay.
Doods: Or I can call back.
Doctor: Yeah, call me back whenever you’re ready and then I’ll go in there and do some stuff and get him all set up. Okay?
Doods: Okay, awesome.
Doctor: All right. I’ll talk to you soon.
Doods: Yep.
Doctor: Okay. Bye.
Manuela: All right. How are you doing Patrik? Can you hear me?
Patrik: I can. I can.
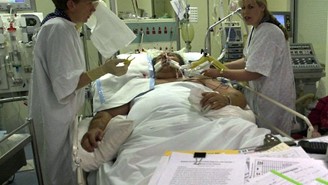
Manuela: Okay. So that was just an update of my father. He’s right now fighting COVID-19. So he’s been on the ventilator since last weekend. So it would be a week today. He did the proning. He did really well on his proning position. He had about four or five sessions of proning. He did really well on that. The reason he was on a ventilator is because he went in that over the weekend and by Sunday night, his oxygen levels had dropped to 40. So critically low with the COVID.
Manuela: Now he’s been battling COVID prior to that Sunday. He was dealing with it throughout that week and he thought he could do it on his own, decided to, to the hospital. They tried the BiPAP machine and his oxygen dropped low with the BiPAP machine. So now you heard the numbers. His oxygen on the vent is 60%.
Patrik: 60%.
Manuela: Yes, 60% yep. And 91 to 97, his blood gas.
Patrik: Blood gas?
Manuela: Yeah. So I just wanted to call to how to make sure this process is not being prolonged. They had him on the paralytics but he’s off that now, so that’s good. So I just wanted to find out, how to make sure that he’s being treated. Which I do, they’re very hospitable, and the doctors he’s at now. Just wanted to get some information on how to make sure that he’s getting the right treatment and ultimately trying to get him off the ventilator and making sure they’re doing everything they can to help him recover.
Patrik: Yeah. The person that was talking on the phone at the moment was that your father’s nurse?
Manuela: Correct.
Patrik: Right, right. Look there’s definitely some bits and pieces in there that are valuable, but in order to determine whether your dad is getting all the right care and treatment, it would really come down to asking more questions. The devil is really in the detail, right? I could list you a number of questions. You can ask the questions. Whether you can interpret the answers, that’s a different story.
Recommended links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
Patrik: The nurse was saying he’s on 60% of oxygen. That’s great information. But there’s 10 other numbers that I would like to know from the ventilator before I can put the 60% oxygen into context. Right. It’s just a number. Yeah, I understand what it means, but unless I’ve looked at other 10 numbers that are currently going on, on the ventilator, it doesn’t mean anything. Right.
Patrik: So, I can give you a list of questions, no issue there, but what do you do with the answers? And what out of an answer, there is a counter question, depending on the answer, right? It’s not as simple as, “Yep. I’ll do this, this, this, and this. Or I’ll ask this, this, this, and this.” What do you do with the information? It’s such a highly specialized area. That I can give you a series of questions. There’s an article on our website, a free article that I can send you a link to. All the questions are there. It’s not a secret. But what do you do with the answers?
Patrik: I mean, I looked after thousands of critically ill patients over the years and I’ve seen so much. Again, an answer triggers another question. Okay. The doctor or the nurses are telling me, “Yep, we’re doing this and we’re doing that.” Okay. What do you make out of this? Anyway, you can see where I’m going with this. Let me ask you this. Is your dad still prone at the moment?
Manuela: No, they had him on his back. He’s been doing well for the last two days.
Patrik: Right.
Manuela: They’ve had no need to prone him anymore.
Patrik: Okay, good. Good. How old is your dad?
Manuela: He’s 57.
Patrik: That’s very young. Previously fit and healthy?
Manuela: No. He’s a smoker.
Patrik: Okay.
Manuela: Okay. Also, an obese.
Patrik: Okay.
Manuela: Okay. He deals with… What is it? Not the high blood pressure. Mild diabetes? I think type II the one that’s…
Patrik: Type 1 or type 2? Insulin?
Manuela: I’m not sure which type, but it’s the type that you can reverse.
Patrik: Oh, okay. Type 2. Is he taking insulin?
Manuela: Yes.
Patrik: Right. Okay. Look, your father is in the higher risk group of people for COVID and with that pre-medical history. But the other question for now is, have they talked about a trach, a tracheostomy? Have they talked about that?
Manuela: They mentioned if he has to keep proning, or if his levels don’t increase, they were talking about ECMO. They mentioned tracheostomy and then they mentioned ECMO most previously, if he wasn’t improving. They mentioned briefly tracheostomy.
Suggested links:
Patrik: Okay. I like what I’m hearing in terms of that they’re mentioning ECMO. A lot of COVID patients and a lot of COVID patients that passed away, missed out on ECMO because it’s such a scarce resource, ECMO. But I’m glad that they’re talking about it and I’m glad that they are considering it in case things don’t improve. Are they having ECMO available in this particular hospital?
Manuela: Yes, I believe so.
Patrik: Good. Good. That’s good. That’s really good. Just quickly talking about tracheostomy, because I don’t know how much research you’ve done.
Manuela: Yes. I’m familiar with that.
Patrik: Right. If he was to have a trach, are you aware of that, one of the next steps after a trach could be to send him to LTAC? Do you know what I mean by that?
Manuela: No, sir.
Patrik: Okay. So a lot of patients, when they have a trach they’re often being sent to facilities that are called LTAC. LTAC stands for long-term acute care, which is more or less a facility where they’re trying to wean patients off the ventilator. From my experience, especially now with COVID as well, patients are having a trach, they’re being sent off to LTAC prematurely. I guess, we would have to cross that bridge if a trach was being suggested, but just to be very mindful, a lot of ICUs are not telling families the full story. They just tell you, you got to consent for a tracheostomy, but they’re not telling you what’s on the other end. On the other end is often the LTAC.
Recommended:
Patrik: I’m very much opposed to people in a critical condition to go to another facility. If you need anything during a critical illness, it’s consistency of care. You don’t need to go to another facility. People have enough issues to deal with. But that is unfortunately how the system is structured. And there are ways to keep patients in ICU for longer than what the ICU wants. But you need to be mindful of that. If the topic of a tracheostomy comes up, you need to ask them what are their next steps if they do a trach?
Manuela: Okay.
Patrik: That’s really, really important.
Patrik: Sure. Yeah. Okay. There would be some LTACs up your end. I’ll tell you the ideal scenario. The ideal scenario for your dad is that he can be weaned off the ventilator and that he doesn’t need a trach. That is the ideal scenario.
Manuela: Okay.
Patrik: Right. So you’re saying last weekend. He got on the ventilator last Sunday?
Manuela: Correct.
Patrik: So it’s one week?
Manuela: Correct.
Patrik: So that’s day seven. I would imagine that in two days, or by Wednesday this week they would be starting to talk about a trach. If your dad can’t come off the ventilator. There is another risk factor if God forbid, your dad needs ECMO. God forbid. If he needs ECMO, he will end up on heparin. Heparin is a blood thinner. Patients that go on ECMO need heparin because the risk for a blood clot is very high on ECMO. If he ends up on heparin and he can’t come off the ventilator while he’s on ECMO, he can’t have a tracheostomy or the tracheostomy will be delayed. Because if you’re on a blood thinner, a tracheostomy is a surgical procedure. You can’t do a surgical procedure if you’re on a blood thinner, because you could bleed to death, literally, right?
Patrik: So there are numerous risk factors that your dad is dealing with, as you can see. And that’s what I’m saying. As much as I would like to simplify everything for families, as you can see, the risk factors if someone is in ICU is, you look left, you look right. There are risk factors everywhere, but it’s a case of being mindful of the risk factors and dealing with it. Yeah, a lot of patients end up on ECMO and they can’t have a trach just simply because they’re on heparin. That’s something for you to keep in the back of your mind.
Patrik: I’m just trying to think of what else would be important. Ideally, if the proning works, that’s great. But if he’s still on 60% oxygen, I’m sure he would have been on a hundred percent early in the week. Do you know?
Manuela: It was early in the week. Earlier in the week, his oxygen levels have been around the 70 mark, 68-70, throughout this last week. So they were turning his levels down throughout the whole week. They’ve been turning his levels down.
Patrik: Good. Good.
Manuela: Yeah.
Suggested links:
Patrik: Look, I would love to talk to a doctor or to a nurse. I can get all the information you will need from the nurses as well. It sounded to me like the nurse knew what he was talking about. That’s I believe where I can help you the most in terms of getting more clinical information and then guiding you with the next steps. That would be my recommendation as a next step.
Patrik: But obviously there is a cost in both for that, if you wanted that, so that’s then up to you, what I will do Manuela, I will send you a link to a blog post that we wrote a while ago with all the questions you can ask, they’re pretty generic, but they are very generic for someone that’s critical in ICU on a ventilator. So you can use that and ask the questions and see what comes back. Are you able to visit?
Manuela: No, there is no visitation, but we do Zoom calls with him. We do Zoom calls with him every day.
Patrik: Is he awake?
Manuela: Right now, he is awake. He’s opening his eyes. They just took out the paralytic two days ago. So he’s starting to open his eyes again.
Patrik: If they ask him to, for example, to squeeze hands, can he do that?
Manuela: Oh, well, we have not found that out yet.
Patrik: Okay. Keep focusing on that because, number one, it’ll tell you whether he’ll wake up. Number two, it’s also important, for example, if God forbid, let’s just say he’s not obeying simple commands, which is squeezing fingers, poke out tongue, simple things like that. If he can’t do that, they should probably check if he had a neurological event such as a stroke.
Manuela: Okay.
Patrik: Okay. Right. Because if he’s not waking up, yeah, there often is a delay just because being on paralytics and sedation , but if he’s not waking up in the next couple of days, if he can’t follow simple commands, there is a risk that he might have had a stroke while he was in an induced coma. One way to find out if he had a stroke is simply by doing a CT scan of the brain. But also checking eyes with a torch.
Manuela: Okay.
Patrik: Okay, checking pupil reaction. I need to go. I’ll send you a link to that article that I was talking about. I will also send you my consulting and advocacy options. If you want to proceed any further, if you wanted more of my time, if you wanted me to talk to the doctors or to the nurses, I’d be very happy to do that. Look out for an email.
Manuela: Okay. I have one last question if you don’t mind. So I asked the doctor today, how are they actually fighting the COVID infection? And what they said was, they’re giving him..
Patrik: Dexamethasone?
Manuela: Yeah and another one. What I found out is that it shuts down the immune system so that inflammation doesn’t continue. So my question to you is how in the medical world, okay, you can shut down the immune system, but how do you guys actually fight the actual infection itself?
Suggested links:
Patrik: As, as you may be aware, the COVID is a viral infection. It’s not a bacterial infection. So if you have a bacterial infection, you give antibiotics, okay. With a viral infection, there is no antiviral therapy for a virus. So hence why they’re going back to the dexamethasone, which is a steroid. And then they’re also giving, have you asked, have they given Remdesivir? Have you heard of that?
Manuela: Yeah he did a five-day period.
Patrik: Right, right. That’s all they’re doing. There is not much more they can do at the moment. They haven’t found anything else yet, but that’s part of the challenge dealing with COVID. It’s not treatable with an antibiotic.
Manuela: Gotcha.
Patrik: So as far as I’m aware, I haven’t practiced in ICU probably for the last 18 months. I actually just stopped practicing in ICU just before COVID hit. Not that I knew at the time that COVID would hit, but my practice here is way too busy, I can’t work in ICU any longer. But anyway, what I am saying is with a viral infection, whether it’s pneumonia, whether it’s any other infection, it’s not much you can do besides trying steroids. You can only really manage the symptoms, but not the cause, which is why they’re now getting everybody vaccinated.
RECOMMENDED:
Manuela: Gotcha.
Patrik: There is no quick fix unfortunately.
Manuela: Gotcha. Okay. Thank you. That explains that.
Patrik: Yeah. So if that doing the Remdesivir and the dexamethasone, they are doing what all the research is suggesting they should be doing. I haven’t seen anything else besides the Remdesivir and the dexamethasone that anybody else is suggesting. I haven’t seen anything else.
Manuela: Okay.
Patrik: Okay.
Manuela: That makes sense.
Patrik: I need to run Manuela.
Manuela: Okay thank you.
Patrik: I need to run. Pleasure. I will send you an email.
Manuela: Okay.
Patrik: Hope it goes well. Thank you so much. Thank you. Bye-bye bye.
Manuela: Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!







