Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
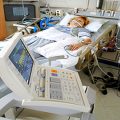
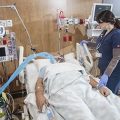
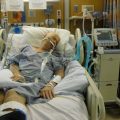
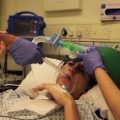
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Stephanie as part of my 1:1 consulting and advocacy service! Stephanie’s mother is a post cardiac arrest patient in the ICU and Stephanie asking if there is a possibility that the hospital can get guardianship of her mom if they want to.
My Mother Had a Cardiac Arrest in the ICU. Can the Hospital Get My Mom’s Guardianship in Their Favor?

Stephanie: Mm-hmm (affirmative)
Patrik: Okay.
Stephanie: The one you just talked to-
Patrik: Yeah, yeah. Yeah, yeah. Yeah.
Stephanie: He’s pretty junior…
Romina: Come again?
Stephanie: No, no, Dr. Brian, he was just wondering whether he is a resident.
Patrik: So, he’s a senior doctor, is he?
Stephanie: I do not know.
Romina: It’s Dr. Brendon.
Stephanie: Dr. Brendon.
Romina: Oh, Dr. Brendon. He means Dr. Brendon.
Stephanie: Where was he last night? Dr. Brendon.
Russell: Uh, Brendon.
Stephanie: Brendon.
Recommended:
Romina: You can talk to him later.
Stephanie: Is he a middle-aged man?
Romina: Yeah, I have no idea what age he is so discreet.
Stephanie: He didn’t seem to be well-informed. Almost every question we asked, he was like, “I don’t know”, “I haven’t been told that”, “Yeah, so that’s all”.
Russell: Yeah, he thought the other newly admitted patient. I apologise.
Stephanie: She just kept saying, “Nothing’s changed for today”, “Nothing’s changed for today”, “Nothing’s changed for today”. Because we asked about the lungs being flooded, and he said, “well, I’m not aware of that, nobody told me the lungs were flooded”. Dr. Reynolds showed her the charts and, on the scan, and he said in the meeting as well, “The lungs are half full”. So, what else were we to think?
Russell: You’re right, you’re right. I apologise. What we try to tell patients and the family, we try to tell them like the possible outcome. We know, you know? Dr. Reynolds and I, we know.
Stephanie: Some of us just lost the patience. And I understand that, that’s just the way it is. But the one good thing that he did help us to understand is that, even though she has fluid in her lungs, at the present time, it wasn’t necessary for you guys to up her oxygen.
Russell: Right.
Stephanie: So, it wasn’t like it was… decided. It was confirmed but not quite as… in front of everybody else.
Russell: Has good lung capacity. I mean, how long to go off the ventilator. She’s doing good.
Stephanie: Okay. Bottom line. Thank you, I appreciate it. Good day.
Russell: Welcome, good day. If anything, you can ask the Doctor on duty.
Stephanie: Yeah, I got you. I got you. Okay, all right. Sounds good. Thank you.
Patrik: Say that again please.
Stephanie: People are responsive today.
Patrik: Right, I see. I see.
Stephanie: How are you going to do your oxygen? 39? 29? Well, that’s good. That’s very good. Yeah. I’m sorry, go ahead.
Patrik: So, and let me ask you this… over the last few days you would say their attitude towards you has changed? Would you say that attitude…? I mean he seemed to be very friendly, he didn’t seem to be avoiding any of my questions.
Stephanie: No, he wasn’t. That’s not how he has been the whole time. He has been irritable with me the whole time. And so was Doctor-. Good thank you. Yeah, and so was Dr. Brendon. They put her on antibiotics and she put the antibiotic drip on Carmen.
Patrik: Right.
Stephanie: Mm-hmm (affirmative)
Recommended:
Patrik: So, you would say, you know, their attitude has slightly improved, with you?
Stephanie: Yes. Without a doubt, yeah, without a doubt.
Patrik: Without a doubt, okay, okay.
Stephanie: Because, because, because. They weren’t like, informative and responsive you know, the first thing they come telling you, made her comfortable, that you want her to be like this weakling if that what they mean, you don’t know what you don’t know. How would you feel if she is bedridden? You know what I mean?
Patrik: Absolutely, absolutely.
Stephanie: And no one wants to help give you the right answers.
Patrik: And now I can hear from them, they’re not making any promises, but they’re saying, “Look it’s up to the family to decide what’s next”, you know? And that’s all you want for now.
Stephanie: That’s it. You’re right. I’m going to be looking at next is, seeing if, I’m going to see if they’re going to try to push her to LTAC. And that would be a problem. You know what I mean? They know we don’t want that. I’m not going to say anything, I’m just going to watch and see what direction they go. They can try and help her a little bit, they’re not going to be able to push her out, okay? Not with water in her lungs.
Patrik: No, no. I wasn’t bringing up the topic of LTAC yet because I didn’t want to say anything that you don’t want. I mean, why would you bring up a negative-
Stephanie: I don’t. I’m glad. I don’t want you to. And I’m not bringing it up either. We will cross that bridge when we get there.
Patrik: Correct, correct. It’s way too early-
Stephanie: It is too early for end of life. Let them bring it up.
Recommended:
Patrik: Yeah, for sure.
Stephanie: Now that, now that we asserted what we want, they quieted down a little bit about that, okay?
Patrik: Very much so.
Stephanie: Because they say, “Oh she’s not stable, she’s not stable”, No, you not, you not-. Let me tell you, they know that we let our friends know what’s going on. The way you questioned him, yeah, they know. They know they need to be very careful about what they do.
Patrik: Yeah, yeah. No, no, that’s fine. That’s fine. And again, so far, we have not taken a confrontational stand-
Stephanie: No, we have not.
Patrik: And there’s no need for that.
Stephanie: Cooperation.
Patrik: Yeah, cooperation, absolutely.
Stephanie: We’re all on the same page.
Patrik: Yes, yes. Absolutely. So far, we get all our questions answered, it’s all good. So, let’s get the trach done and then there’s no reason to jump too far ahead. There is, I think for now, we’ve achieved what we’ve wanted to achieve. Which is, okay, well, she’s going to have a trach, there’s no more talk about end of life.
Stephanie: Right, right. Right.
Patrik: And that’s all we can, that’s all we can do for now.
Stephanie: Yeah, so, I’ll take that I don’t have to have- I don’t have appointment for tomorrow but I can still talk to you on Thursday, right?
Recommended:
Patrik: Where are we up to… I’ll have a quick look, I think you can call me on Thursday, I think so… I’ll have to look, I’ll have to have a look. I think so.
Stephanie: Because we have a one day that we need to get for the conference with the doctors and ask their plan of care. And after that, I just want a couple of more days and we’ll be good. You’ve been excellent anyway. I mean, you’ve done all the above and I appreciate that.
Patrik: Thank you.
Stephanie: I’ve been talking to my family. Literally what they’re- Yes, yes! You’re very welcome, you’re very welcome. Because I’ve been talking to them to see if somebody can take on the heat and for her long-term care. So, they have questions in between that, which is, you know, which is understandable. But at this point, I am dry. But, still I felt the need, even though it’s out of my scope, I still felt the need to do that for my mother. You know, to take care of her. You know, because she did it for my grandmother. She had it, she did it for my grandmother because we took care of her at home, for 2 and a half years. My grandmother did not have any break down in her body, because she was well taken care of. She was at the pinnacle of that and… financially, and we appreciate that. If she’s at a point in her life where she doesn’t have any stroke. She barely got in, you know, she was bedridden but, you know, still… things in life change. 2012… shoot, that was 6 years ago, shoot, yeah.
I appreciate it, one other thing, let me go in the bathroom… Miranda was, she was concerned about guardianship and she said that they could take her guardianship away from her and that could mean Carmen could be awarded to the state if she doesn’t have anything in writing saying that she’s a guardian. So, I told her, you guys verbally, she pretty much verbally told you, if she told you to “Take care of me child, don’t let nobody hurt her, manipulate her or assault her verbally. Do you know anything about guardianship?
Recommended:
Patrik: So, is there anything in writing that Miranda is the guardian now? Is there anything in writing?
Stephanie: No, not at all. She was going to go online and try to fill out form for guardianship, something that had to be signed by 2 doctors, either a lawyer, or something like that. Because if we don’t have it, she was afraid that the hospital will try to take guardianship. Put her anywhere they want to put her.
Patrik: No, no. That is a concern if, and why… so, has the hospital mentioned that at all? That they would like to take away guardianship or that they would question the guardianship status? Has that been a point of discussion?
Stephanie: Not at all.
Patrik: No okay.
Stephanie: No one has not, there has not been… we’re just trying to be proactive and, you know… I would advocate for her I can’t blame her for being proactive on that, I cannot.
Patrik: No, not at all, not at all. So, okay, so… here is what’s important with guardianship. I’ve had a client recently, and again I’ve interviewed this lady, I can send you a link to that as well. I’ll give you the very brief version. This lady had her 20-year-old daughter in ICU and they-
Stephanie: I saw that.
Patrik: Right, right. And they had-
Stephanie: Tried to take it away.
Patrik: No, no, no, they didn’t. But I’ll tell you the story, so you understand in what situations they potentially might think about taking guardianship away. So, she was in ICU with a breathing tube and the ICU wanted to do a trach. The mother objected, the mother was the medical power of attorney, the mother objected and then said, “I’m not going to have my daughter have a trach without trying to get the breathing tube out first”. Okay. Then when I got involved, I said well there is a clear chance that this lady can come off the ventilator and doesn’t need a trach. Okay, so that was very different from your situation. So, the ICU then was basically saying to the lady “We’re going to take away your guardianship because you are not acting in the best interest of your daughter. Right, the hospital was saying that the trach is in the best interest of the daughter and the mother was objecting that. So, to me the signs were clear that this young lady could come off the ventilator and doesn’t need a trach. Now, we believe the hospital at the time, had an ulterior motive and wanted to get the daughter into one of their LTACs.
Recommended:
Stephanie: There you go.
Patrik: Right… and I said no, no, no. And then I said to my client, 2 ways to manage this. The first thing you say to them is you want to get out of this hospital and you want to get to another hospital. And the next thing is, that if they do continue to threaten with guardianship, you bring in a lawyer. So, she did both. She did both. She asked to get to another hospital and she threatened then to get in an attorney. And within 24 hours, the lady was in another hospital and within another week she was off the ventilator and she is now back home.
Stephanie: Wow, yeah. Would you recommend us trying to get her to another hospital?
Patrik: Yeah but the guardianship issue will only… Look, I’m not a lawyer, right? I’m not a lawyer by any means. But what I do recommend is, get that guardianship issue sorted. Make sure there is a piece of paper that Miranda is the guardian. How do you go about that? I don’t know. Probably through something like, there must be an organisation like the public advocate or something like that.
Stephanie: Yeah.
Patrik: Contact them. Get that guardianship issue sorted. Because then she’s got-
Stephanie: That’s what she’s trying to do.
Patrik: Right, right. Then she’s got full control. I’ll tell you what could happen, and that would be the worst-case scenario, I’ll tell you what could happen, but that would really be the worst-case scenario. You’re trying to keep her in ICU and they might say “Oh that’s not in her best interest, blah, blah, blah. And because you’re not acting in her best interest, but we do. We need guardianship”. Right? It’s a bit like, it’s a bit like, look, I’m giving you another… look if someone has kids, and they’re abusing their kids, god forbid, you know, they shouldn’t be the guardian. Right? I mean they shouldn’t be the guardian. So, then an authority must arrive to take away guardianship, but this is not about abuse, this is about the right direction.
Recommended:
Stephanie: Mm-hmm (affirmative)
Patrik: You should get that house in order. Get that piece of paper, absolutely.
Stephanie: Mm-hmm (affirmative). Yeah, we’re going to find out whatever we must do. But she said it’s a big process-
Patrik: Look, I can’t comment on that, I really can’t.
Stephanie: I know, that’s fine. That’s fine. We’re going to do our research, I did all the research myself, so we’re going to do whatever we have to do to-
Patrik: Get that piece of paper. Get that piece of paper, and potentially have a second guardian in line as a… back-up.
Stephanie: I thought of it, my brother. He is unavailable.
Patrik: Right, your brother or… right.
Stephanie: Let me tell you, my brother… I don’t want to be the guardian because… because I don’t take blood. Okay. And so, if they ask me to give her blood, my answer is going to be no, you know. I want you to manage her with non-blood management. I want her to receive quality care but with non-blood management. Because people are doing it left and right hoping they could get everything. But of course, you’re talking about someone who is not quite as compromised as Carmen is compromised, you know. Taking antibiotics, vitamin C, whatever they can give her to fill up her blood. But the thing is, is that I would not be able to authorise that, and I would not want to be responsible for if Carmen passed away and then they’ll be like, “Stephanie, you didn’t give her blood then let her deteriorate”. They can’t prove whether the blood is what kept her alive or not alive, you know what I mean?
Recommended:
Patrik: Absolutely, absolutely.
Stephanie: But I couldn’t put myself in that position.
Patrik: Yeah. Look, look… that’s fine. But just make sure that you as a family, have a back-up, that’s all I’m saying. You know?
Stephanie: But my brother, my brother was like, “Stephanie, I want you to get these papers and back date it for 2 months”, I was like, “Miranda, I can’t do it”, because I’m not going to do that. But I said, “Next thing you know, what if it all falls through?”, you know, you are talking a lost cause. You know what I mean?
Patrik: Absolutely.
Stephanie: That stuff cancels out with you, you know what I mean?
Patrik: Absolutely.
Stephanie: I was like “Nah, we aren’t going that route, we’re going to pray, we’re going to try and do the right thing and pray and let god handle it, and hopefully it’ll go right”. So, that’s just how we want to take it. Yeah so, we’ll work it out, we’ll work it out for sure. I do not want to put more pressure on Carmen, you know, she knows where we are. Everything seems to be, at this point, at this point, they seem to be doing everything that we want them to do and that they’re supposed to be doing, you know. We did have to meet with them for a couple of things, you know what I mean. We had to decide on a couple of things that they weren’t even addressing and after 3 days, she was still kind of hesitant and weak and if they weren’t going to give it to her for what other reason they should have shared that with us. You know what I mean?
Patrik: Very much so, very much so.
Stephanie: She was to get rid of some of that fluid. It wasn’t until that night that we talked to that elder lady on the phone that they started, suddenly everything went into action. You know what I mean?
Recommended:
Patrik: Absolutely, absolutely. And so far, what I can see as well is, there is, which is important, there is no more confrontation now. They seem to be reasonable and cooperative, they’re asking questions. You know, and that’s a basis to build up on, you know? It’s all in all basis to go from. If god forbid, things are not going the way they’re going, the way we all hope they go. It’s a good basis to negotiate on any level.
Stephanie: Yeah, it is. Dr. Brendon he, you know, talks to our family and he’s really concerned about us and I believe that, you know, to a large extent that it’s true. I know he also has his other hidden agenda on the other hand as well. I’m not blind or oblivious to the fact that, you know, he still… he wants your yes attitude. He can’t have people in ICU, it’s his worst-case scenario is to have somebody in ICU indefinitely.
Patrik: Yeah, yeah.
Stephanie: On the phone, if that isn’t true, if that isn’t the worst-case scenario, why don’t you show me, the laboratory work through all the numbers, the serious values so how this one person is not going to kill your numbers. I know what metrics are, I know what your score par is, I have a score par. You know what I mean? In my job, you get paid based on, you know, performance and loyalty for how long. So, I understand that, I understand that dynamic so, you know, it’s okay. I know you care but on the other hand you have 2 things to worry about, I don’t have an agenda.
Patrik: Yes, no, no. Absolutely. And that’s the bottom line, they’re looking at many moving parts, whereas you’re looking at this, and that’s the bottom line. I think going from Saturday or Sunday… you know, where, you know… it was really looking difficult to now, where we have achieved sort of consensus. She’s moving to the trach and then we can reassess. I think that’s a good outcome for now.
Stephanie: Oh, there you are, okay good. I’m good, I’m good, thank you.
Cindy: Any questions?
Stephanie: I’m very well, no. My sister will be back up. No, not exactly right now, but she will be back up.
Cindy: That’s okay then.
Stephanie: Okay, who is on duty now?
Recommended:
Cindy: I think… Elena.
Stephanie: Oh Elena, the one that was here last night. Okay. Thank you.
Cindy: Have a good night.
Stephanie: You too.
Cindy: Okay.
Stephanie: Okay, I’m sorry, I’m back. Thank you for giving us your time, you were making rounds. Patrik are you there?
Patrik: Yes, I’m here, I’m here.
Stephanie: I apologise. So, I’ll get you later in the evening?
Patrik: I think going from a situation on the weekend, where there was either push towards end of life, or push towards trach or LTAC, you know, I think we’ve really put a stop to that for now… I guess one of my concerns is probably, I can’t really talk to that, but I guess one of my concerns is really… I guess you as a family must manage Miranda. I think she is very overwhelmed…
Stephanie: Yeah, thank you for that. Thank you for that advice.
Patrik: She’s extremely overwhelmed, and if she sees that her mother is not improving fast, you know, that could frustrate her even more.
Stephanie: Good god, you can see how she’s expecting too much.
Patrik: Yes.
Stephanie: Too much, too soon. Yeah.
Patrik: Right. And you know, I would always go back to one day at a time.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Stephanie: Yes. Yeah. How do you say that again? You say…
Patrik: Today’s today. Get her through today, and then get there through tomorrow, and then think about Thursday. You know, it’s not… living in the future is not going to serve your situation.
Stephanie: Not at all.
Patrik: And bear in mind, if for whatever reason, she can’t come off the ventilator, there is plenty of time to talk about end of life… plenty.
Stephanie: Right, right.
Patrik: So…
Stephanie: That’s Miranda texting me now.
Patrik: Right, right.
Stephanie: She’s at work and I’m still like “Yeah, that’s my job. I’m telling you, you gotta look out for her”.
Patrik: Right.
Stephanie: I think we’re in a good place right now.
Patrik: Yes, I think so too, I think so too. And all you can do is one day at a time, one day at a time.
Stephanie: Mm-hmm (affirmative), exactly. Yup. So, we’ll leave it at that and we’ll get back to you probably… what were you going to say sorry.
Patrik: Yeah, get back to me after the surgery, if you need me before, please get back to me of course. I can tell you that tomorrow… Wednesday night, if you need me Wednesday night, my availability might be patchy but please try of course. Please try of course. And I will get back to you, I’ll definitely be able to message you, definitely be able to message you. Thursday will be fine…
Stephanie: Okay, that’s good enough. Yeah.
Recommended:
Patrik: And then we’ll take it from there.
Stephanie: Yes, we will. Thank you Patrik, you have been a god send. Thank you so very much.
Patrik: You’re very welcome.
Stephanie: All right, take care now. Have a good one.
Patrik: And you, thank you. Bye.
Stephanie: Thank you, bye-bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!