Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
What is the Survival Chance of My Dad with Kidney Failure & on a Ventilator in ICU?
You can check out last week’s question by clicking on the link here.
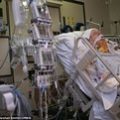
In this week’s episode of “YOUR QUESTIONS ANSWERED”, I am here with a live stream today, where I want to answer your questions if you have a loved one in intensive care. And this is one of the most commonly asked questions for families in intensive care and it’s a question that we get all time. And today’s live stream is about the pros and cons of a tracheostomy in intensive care.
Your Questions Answered Live: The Pros and Cons of a Tracheostomy in Intensive Care
Hi, it’s Patrik Hutzel from intensivecarehotline.com and I want to welcome you to the live stream today. I can see that there’s some people here already. I want to welcome you to this live stream. And today I want to talk about the pros and cons of a tracheostomy in intensive care.
So let’s dive right into it because I’m sure that’s what you want to know while you’re here on this live stream. If you have any questions, please type them into the chat part, and we can get onto those questions. But let me just start about the topic in particular, again, the pros and cons of a tracheostomy in intensive care.
So a lot of families come to us here at intensivecarehotline.com and they want to ask, well, should we be consenting to a tracheostomy in intensive care or should we not be consenting to a tracheostomy in intensive care?
Now let’s quickly look at the answer to that question and the answer to that question really is, you should consent to a tracheostomy in intensive care if the intensive care team has done everything beyond a shadow of a doubt to get your loved one off the ventilator with a breathing tube and an endotracheal tube. And if your loved one has a breathing tube or an endotracheal tube in their throat, that’s very uncomfortable. They need to be in an induced coma and waking up after that induced coma has its challenges, and that’s often when people fail to be weaned off the ventilator, but there’s so many things that can be done to wean someone off the ventilator and the breathing tube before tracheostomy needs to be considered. For example, sometimes sedation needs to be changed. Sometimes ventilation settings need to be changed.
RECOMMENDED:
Sometimes physical therapy or physiotherapy needs to be started before you can remove the breathing tube, but the advantages of avoiding a tracheostomy overall by far outweigh the disadvantages, if, and here’s the big if, if the breathing tube can be taken out within a timeframe sort of, of a 10 to 14 day mark. And why is that? If you leave the breathing tube in for more than 14 days, 10 to 14 days, that one of the biggest challenges is that patients need to stay in an induced coma because the breathing tube is so uncomfortable.
When the breathing tube stays in for more than 14 days, and your loved one stays in an induced coma for more than 14 days, the challenge is that they decondition quickly. They decondition very quickly and then it gets even harder to be weaned off the ventilator because they are deconditioned. The induced coma weakens them. They’re wasting their muscles very quickly and that’s why it’s then getting even more difficult to wean someone off the ventilator. Whereas if you then move to a tracheostomy after 10 to 14 days, you can usually switch off the sedation pretty quickly. You can get patients out of an induced coma fairly quickly, and that helps them to then regain their strength, regain their muscles and breathe by themselves because the tracheostomy overall is not painful.
Suggested links:
Overall the tracheostomy patients don’t report any pain, which means they can be taken out of the induced coma. And that’s when they can have more physical therapy, they can get mobilized easier and it helps them to be weaned off the ventilator once they have a tracheostomy. Also, a tracheostomy is more or less buying a critically ill patient time to be weaned off the ventilator. Whereas, as I explained before, when someone is on a breathing tube, there is a limited time window when they can be weaned off the ventilator. And if they can’t be weaned off the ventilator within that 10 to 14-day window, after that, staying on a breathing tube and an endotracheal tube is defeating its purpose. It’s defeating its purpose. And that’s why you then have to move to a tracheostomy eventually.
Now, for some of you that are listening to this, especially if you’ve been struck or if your loved one has been struck with COVID and is in ICU with ARDS. What we’re definitely seeing at the moment, obviously with the spread of COVID and then patients ending up in intensive care with ARDS or lung failure, is clearly that there are delays with tracheostomies. Why are there delays? Quite simple. A tracheostomy is a surgical procedure, when they cut the hole in the trachea to perform the tracheostomy, the lungs are open, even though it’s only for a short period of time. Obviously, the COVID is sitting in the lungs. The lungs are open.
The spread of COVID is real, which means it’s a big risk for hospital staff, whether it’s the doctors, the nurses. So the risk of hospital staff contracting COVID by doing a tracheostomy is real. And that is why that there are often delays now to see whether the COVID can go away and then once patients are COVID negative, it’s easier to do a tracheostomy. Having said all of that, that doesn’t help a patient again, because, once the 10 to 14 day time window has been more or less gone, to wean someone off the ventilator with a breathing tube, the patient deteriorates often even further. So that’s why the 10 to 14-day time window is so critical.
And that’s why COVID really has made things worse, especially for COVID patients specifically. And we are certainly seeing across the board that the deconditioning of COVID patients seems to be fairly rapid. Not that I want to talk about COVID now, but I just want to quickly mention that, and especially since a lot of COVID patients with ARDS or lung failure are being proned, they go into prone position and they’re often then in an even deeper induced coma, they need more sedation, more opiates. And they often also need muscle relaxants to be paralyzed, to tolerate the proning and the combination of all of that delays tracheostomies even further. It weakens patients even further, they’re deconditioning even quicker. And it’s a whole vicious cycle that’s starting there. So the COVID is definitely a terrible, terrible thing that happened for everyone. But specifically for patients that end up in ICU that go through the proning, go through the induced comas and paralysing.
Recommended links:
But let’s just quickly look now in more detail about the pros and cons of the tracheostomy in intensive care. Let’s just quickly start with the pros. The pros are, you can stop the induced coma most of the time and patients can wake up. You can assess them neurologically because if someone is not waking up after an induced coma, especially if they still have a breathing tube in, well the questions are, have they had a neurological event? Have they had a stroke? Have they had a brain bleed? Have they had maybe underlying seizures and so forth? So once the tracheostomy is done, when someone can’t come off the ventilator, it’s so much easier to assess someone neurologically because you can switch off sedation and you can see are people waking up or not. That is definitely one advantage.
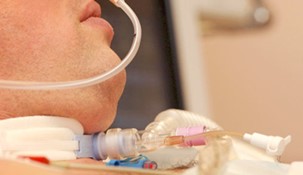
The next advantage of a tracheostomy is it’s easier to tolerate. So you would have seen your loved one with a breathing tube or an endotracheal tube coughing, it’s very uncomfortable, they often if they are awake, they’re pointing to the tube and they want to have it out. And that’s all understandable. So once the tracheostomy has been done, it’s easier to tolerate. Most people with the tracheostomy don’t report any pain, they don’t report any discomfort. There is some discomfort as well with the tracheostomy, it’s mainly around when you change the dressing, when you change the tape, when you change the cannula, that people start coughing that is definitely a disadvantage. And it’s definitely uncomfortable.
The other disadvantage is that when you suction, again, people start coughing, but that is the same on the breathing tube. And it’s less comfortable. It’s more comfortable on the breathing tube compared to the tracheostomy, if there are any questions while I’m talking, type them in and we can, and I can answer those questions once I’ve gone through the pros and cons, so please type in your questions.
So the next benefit of a tracheostomy is that you can mobilise easier and quicker. So why is that? So let’s just say you’re mobilising someone. And when I say mobilisation, I mean getting somebody out of the intensive care bed, getting them in a recliner chair and they’re special chairs in ICU where you can mobilise a person.
Recommended:
There’s a high risk of mobilising someone with a breathing tube or an endotracheal tube. If the tube comes out during mobilisation and that can happen, it can be life-threatening and can be very difficult to reintubate a patient while they are being mobilised. Again, that can be a life-threatening situation. With a tracheostomy for example, if God forbid a tracheostomy comes out or gets dislodged, it’s so much easier to deal with that, it’s just putting in a new cannula. You don’t need to intubate someone, it’s so much easier to deal with it. So that is definitely another advantage.
The next advantage is suctioning. So when you have someone with a breathing tube, you have a very long breathing tube and you need to suction, okay? And you need to suction regularly to clear the airway because patients are not in a position to clear their own secretions while they’re on a ventilator with a breathing tube. So when you suction someone with a breathing tube, you need a long suction catheter. It’s very uncomfortable, patients report that they’re feeling like they’re suffocating. They’re coughing, again, the risk of the breathing tube getting dislodged, coming out is fairly high. And again, that is a life-threatening issue. So then if you are having a tracheostomy and you need suction, you need a shorter suction catheter. It’s much easier to control.
You can also change with a tracheostomy, often have an inner cannula, not all tracheostomies have an inner cannula, but most tracheostomies have an inner cannula. And it’s actually much easier for you to make an assessment. How many secretions are there? If you have an inner cannula, you can have a look, is the tube blocked or is it close of being blocked? It’s almost like a safety valve, if you’re having an inner cannula to check for airway patency. And that is very difficult to assess with a breathing tube. Now just give me one second, I just need to get rid of the lump in my throat.
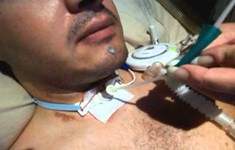
The next advantage of having a tracheostomy is clearly this, and this is probably one of the major ones. So when someone is on a breathing tube and because the breathing tube is so long, right, and people need to be in an induced coma, it’s very difficult to do breathing trials, especially if people can’t tolerate the breathing tube. So when someone is doing a breathing trial on a breathing tube and they can’t tolerate the breathing tube, all they do is they cough, they get very agitated because it’s so uncomfortable, and it’s very difficult to do a spontaneous breathing trial. Whereas with the tracheostomy, it’s very easy doing a spontaneous breathing trial. So when you do a spontaneous breathing trial on a tracheostomy, you could pretty much just remove the ventilator, patients are more awake, generally speaking, and you can put them on some humidified oxygen.
Recommended:
It’s also known as a trach collar, or you can put them on a Swedish nose, on an HME filter and you can see fairly quickly can someone tolerate breathing spontaneously. And I can tell you, even if it’s only 10 minutes in the beginning, if someone has been on a ventilator for two for three weeks and they can only breathe spontaneously in the first 10 minutes, well, that’s a start. That’s 10 minutes more than the three weeks before. So you got to look at the little wins in those situations, and it’s just so much easier to do breathing treatments. Also, it’s so much easier with a tracheostomy to do things like nebulization, right? It’s a normal saline nebulizer, Ventolin nebulizer, Atrovent nebulizer, Pulmicort nebulizer. It’s just so much easier to apply those breathing treatments that often help a critically ill patient to get off the ventilator.
So that is definitely another big advantage. Here’s another advantage. When someone, let’s just say they’re having a size eight breathing tube, there’s different sizes, different size breathing tubes, different size tracheostomy tubes. Okay, let’s just say someone is having a size eight breathing tube, they’re now ending up with a size eight tracheostomy, right? And you can also then start downsizing the tracheostomy, maybe go from a size eight to a size seven. And again, that helps in the process of weaning off the ventilator. You can’t do that with a breathing tube. It’s too complex, too complicated. The risk of changing breathing tubes to different sizes is too high, whereas with a tracheostomy can be done very easily. Okay. So that’s another advantage.
The next advantage with a tracheostomy is that if someone has time off the ventilator, they can also be placed on trial of starting to talk again, even though the vocal cords are generally speaking paralysed, you can then start using a speaking valve. And again, that often doesn’t happen day one, but you know, again, speech therapists can start training someone on tracheostomy to start talking. So that’s another major advantage.
Another advantage is that if someone has time off the ventilator and is not at risk of aspiration, you can also take down the balloon or the cuff of the tracheostomy tube, and you can see can someone cough up their secretions, very difficult to do that with a breathing tube, okay. So that’s another advantage.
Coming back to what I believe is one of the biggest disadvantages, especially for our viewers in the United States, and you might wonder what has a tracheostomy to do whether you’re in a different country? Well, I will elaborate on that in a minute. So for our viewers in the United States, one of the biggest disadvantages of having a tracheostomy is that the ICUs often want to send your loved one to LTAC.
Suggested links:
LTAC stands for long-term acute care facility. Now that generally speaking doesn’t happen in other English speaking countries, like in the UK, Ireland, Australia, New Zealand, people after tracheostomy stay in intensive care. And from my experience, that’s where they should be. There is another alternative INTENSIVE CARE AT HOME, but I’ll come to that a bit later. I just want to explain to you about the disadvantage about LTAC first.
So a critically ill patient in intensive care ends up with the tracheostomy because they can’t be weaned off the ventilator. And then ICUs in America want to send them to LTAC. And that is a disaster waiting to happen, right? LTACs are designed to save money, they’re not designed for clinical need. Now, when someone is critically ill in intensive care and they’re needing a tracheostomy for all the reasons that we just mentioned a minute ago, going to LTAC is an absolute disaster. It’s like staring into the abyss. Why is that?
As you probably know, for our viewers in the US, Medicare, Medicaid, they’re paying 60, sometimes 90 days of ICU. And then people got to move on, irrespective of their clinical condition. And that’s where LTAC comes in. Again, not designed for clinical need, it’s designed to save money. Then patients with a critical illness end up in LTAC.
Now picture this you’re going from ICU, where you have ICU doctors, ICU nurses, respiratory therapists, physical therapists, the whole lot. And then you’re going to LTAC. That’s designed to save money. And then you have one nurse looking after ten patients. That’s not critical care trained. You have one doctor overseeing 30 patients all on ventilation with tracheostomy. It’s a disaster waiting to happen. It’s a tragedy. It’s still a beggar’s belief to me that somebody has invented LTAC in the United States to save money.
And a lot of patients die in LTAC. Unfortunately, a lot of families come to us here at intensivecarehotline.com and they ask us, “Oh, can you help me get my loved one out of LTAC because this is not what we expected.” And we know why, I can see why this is such a terrible tragedy going to LTAC. When someone is critically ill, the last thing you want is disrupting a care episode.
Now, when you look at LTAC, it’s clearly disrupting a care episode in intensive care. We’re talking about disrupting a care episode for some of the most vulnerable people in a hospital. That is beyond belief, from my perspective. On top of that, many LTACs depending on your location, many LTACs want to send your loved ones hours away, potentially to another state because LTACs are not necessarily readily available in your location, right?
We have dealt with families that have been asked to send their loved ones from Los Angeles to San Francisco to an LTAC. We have been dealing with families in Florida that had their loved ones, that where the hospitals wanted to send their loved ones to Georgia, to an LTAC hours away from their family. It’s beyond belief. It’s beyond belief what’s happening there. The system is flawed. And Amy, you’re just saying that, you try your best to keep your dad in ICU. And again, you should be trying to keep your dad in ICU. You should be trying to avoid a tracheostomy in the first place, and you definitely should be trying to avoid LTAC if your dad, for whatever reason does need a tracheostomy. So that’s my advice there. So coming back to the disadvantages here is the LTAC clearly.
And again, from my experience, we have helped many families through our consulting and advocacy to keep their loved ones in ICU when they were on the brink of a discharge to LTAC, because we are clinicians ourselves, and we can advocate for your loved one and say, “Look, these are the reasons why this particular patient needs to stay in ICU.” We know that LTAC is just a disaster area. And if you look at the reviews for many LTAC facilities, if you look up the Google reviews, most reviews are pretty negative. Whereas the hospital is trying to tell you that LTACs are specialised in weaning patients off ventilation, and nothing could be further from the truth. Nothing could be further from the truth. So it’s a very unfortunate situation for many patients that go into LTAC and are stuck there for many weeks on end.
Suggested links:
The other disadvantage on that note is that, think about this. Your loved one is critically ill and is going to LTAC in a very vulnerable state. Chances for something to go wrong are pretty high. Chances that your loved one is bouncing back into ICU is high. And that’s another disruption of a care episode, and there’s no guarantee that A, the LTAC has an ICU attached to the hospital or to their facility, sometimes they do. Or B, that the ICU where your loved one came from still has a bed available. So what that looks like in reality often is your loved one is going to LTAC. They need ICU again, and your loved one then goes back to another ICU, basically in that vulnerable state, they end up in three hospitals. That is ridiculous. No, and it’s not conducive to recovery for a very vulnerable patient in that situation.
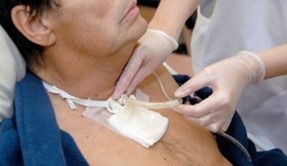
So the other disadvantage of a tracheostomy is clearly that it’s a procedure, it’s a surgical procedure, there’s risks with a surgical procedure, right? Infection risk, bleeding risks, there’s definitely risks attached to that. Having said that from my experience, most tracheostomies that are done, it’s a smooth process, but again, like with any procedure, there is definitely a risk attached with that.
And again, I keep coming back to why that you should only consent to a tracheostomy if the ICU team has done everything beyond a shadow of a doubt to get your loved one off the ventilator and the breathing tube in the first place. Now, and that is sort of, I can’t elaborate in this call on what that is, what boxes need to be ticked. So when that the ICU has done everything being beyond the shadow of a doubt to get your loved one off the ventilator. I will do that in another live video, maybe next week, where I will focus on that specific topic.
But the bottom line is this, you need to know what to look for because your biggest challenge is that you don’t know what you don’t know. Your biggest challenge is that you don’t know what to look for, you don’t know what questions to ask. You don’t know your rights, and you don’t know how to manage the doctors and nurses in intensive care. That’s one part of your challenge in those situations.
So another disadvantage when it comes to the tracheostomy, is that it generally speaking, prolongs hospital stays, generally speaking. So picture this, you have your loved one on a breathing tube, on a ventilator, and you can take that tube out and recovery goes well. Well, that trajectory is hopefully straightforward.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Okay, yes it might include some rehabilitation, but that process should be more straightforward compared to having a tracheostomy, having a prolonged ICU stay, potentially going to LTAC, potentially needing services like INTENSIVE CARE AT HOME. The trajectory of recovery from A, having the breathing tube removed or B, having a tracheostomy is like day and night. There can’t be more contrast than that. Your loved one should be able to leave intensive care much quicker and go to a hospital floor or a hospital ward if they’re having the breathing tube removed, as opposed to having a tracheostomy, because they need more time to be weaned off the ventilator. So whenever you can have that breathing tube removed, you should be going for that. The only time you shouldn’t have the breathing tube removed is when ICU teams talk about, “Oh, we’re doing a “one-way extubation”.”
What does a one-way extubation means? A one-way extubation means we’re going to take the breathing tube out. If your loved one can breathe and maintain their own airway and survive that’s great. If they can’t breathe, if they can’t maintain their own airway when we do that, “one-way extubation”, bad luck. It’s basically a sink or swim approach and you certainly don’t want to have your loved one approaching a sink or swim approach whenever that can be avoided, because that’s basically a life or death situation with no backup plan.
If the ICU team wants to do a trial extubation and is offering the tracheostomy on the other end, that’s fair enough from my perspective, I do believe that a trial extubation should be done. I do believe in that, but if that fails, a tracheostomy definitely needs to be offered on the other end to avoid that “sink and swim” approach.
RECOMMENDED:
So yeah, that’s where I sort of want to slowly come to an end here in terms of the pros and cons of the tracheostomy. Just very quickly, another alternative obviously is, depending on how much research you’ve done. Let’s just say a loved one can’t come off the ventilator with a tracheostomy and is either stuck in ICU or an LTAC. Another alternative for that is definitely INTENSIVE CARE AT HOME.
Intensive care at home offers services, 24-hour services at home with critical care trained nurses for long-term ventilated patients with tracheostomy. And you should be checking out intensivecareathome.com for more information there.
But that is definitely a genuine alternative for long-term ventilated patients with tracheostomy. But again, that is more that if everything that we spoke about so far is failing. I hope I’ve given you enough strategies now that you don’t need to be in a position where you need intensive care at home for your loved one. But it’s also important for you to know that it’s there on the other end. Again, you can check out intensivecareathome.com.
Now for our viewers that are still here, should you have any other questions, please type them into the chat part and I would love to answer them. If you have any questions. Alternatively, you can email me at [email protected].
You can email me your questions there. You can also call me on US 415-915-0090, that is again, if you’re in the US you dial 415-915-0090. If you are in the UK, you dial 0118-324-3018. That is again for our viewers in the UK you can call me on 0118-324-3018. And for our viewers in Australia, you can call me on 041-094-2230. That is again for our viewers in Australia, you can call me on 041-094-2230.
So if there are no other questions, I’ll leave it there. I do see that Amy, if you want to email me later, you’re welcome to do so again, you can email me at [email protected]. I would probably do another live call next week and want to talk about what I mentioned before, what does the ICU team need to do to get your loved one off the breathing tube in the first place?
So, like I alluded to, the ICU team needs to do everything beyond the shadow of a doubt to get your loved one off the breathing tube and the endotracheal tube in the first place to avoid the tracheostomy. And I want to hone in on that next week. And again, thank you for all of you that have come on to this call, Amy, Philine and others, and looking forward to your phone calls and email. Take care for now. And I wish you and your families all the best.
This is Patrik Hutzel from intensivecarehotline.com and I will talk to you in a few days.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!