Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
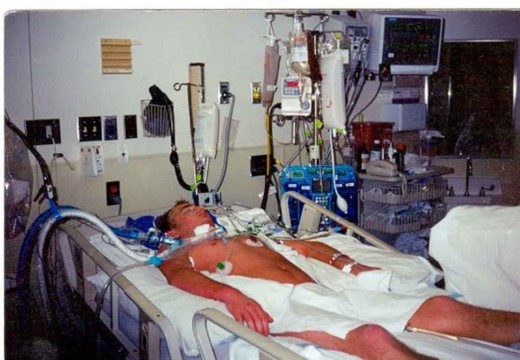
In this week’s episode of “YOUR QUESTIONS ANSWERED”, I am here with a live stream today, where I want to answer your questions if you have a loved one in intensive care. And this is one of the most commonly asked questions for families in intensive care and it’s a question that we get all time. And today’s live stream is about My Dad is Having Multi-Organ Failure in Intensive Care! What’s the Prognosis? Live Stream!
My Dad is Having Multi-Organ Failure in Intensive Care! What’s the Prognosis? Live Stream!
Welcome to another Intensive Care Hotline livestream. I’m your host, Patrik Hutzel from intensivecarehotline.com. Today’s live stream is about, “My dad is in multi-organ failure in intensive care. What’s the prognosis?”
Now, before we go into today’s topic, just a couple of housekeeping issues. I want to welcome you to this live stream and please type your questions into the chat pad. Try and keep them to today’s topic. If your questions are not related to today’s topic, I will get to them at the end of the topic.
Before I get into today’s topic, what makes me qualified to talk about this topic? I have worked in intensive care for over 20 years as a critical care nurse. Out of those 20 years, I have worked for over five years as a nurse unit manager in intensive care, getting enough insights about how intensive care units really operate, getting insights into what’s happening behind the curtains that nobody is telling you about. I have also been professionally consulting and advocating for families in intensive care all over the world since 2013 through intensivecarehotline.com. I’m also owning and operating an Intensive Care at Home nursing service, where we are looking after predominantly long-term intensive care patients with tracheostomy and ventilation.
So, without further ado, let’s dive into today’s topic, “My dad is in ICU with multi-organ failure. What’s the prognosis?” Many families come to us here at intensivecarehotline.com. They say, “Look, the ICU team has told us that my mom, my dad, my brother, my sister, my spouse, my child has multi-organ failure. That it’s therefore, “in their best interest” to remove life support.” Their justification is always around that, with multiple organ failure, life can no longer be sustained and that it’s “futile to sustain life”.
That it’s “futile to sustain treatment,” and therefore sustain life.
Now, what does futility mean? It’s probably a term that we need to clarify before we move along into today’s topic. Futility is a term that’s often being used in intensive care. It means it’s of no benefit for a patient. Now, I argue that this definition is not correct. I argue it’s of no perceived benefit to a patient. Perception plays a big role in all of this.
Many times, when I’ve been in family meetings, either when I was still working in ICU or either here in my professional consulting practice. One of the arguments of intensive care teams is always, “Yep, your loved one is in multi-organ failure. There’s no hope.” It’s again, “in the best interest” of your loved one to stop life support because we can’t, and we wish no longer to support those organs.
RECOMMENDED:
Now first things first, and this is really important, what I’m going to say now because intensive care teams won’t tell you what I’m telling you now. Approximately 90% of intensive care patients survive in intensive care. That means approximately 10% of intensive care patients do not survive. I believe that this is a large number of people surviving intensive care, especially since the intensive care team will never share that with you. You can look up the research. You can look it up on our website or you can look it up on other outlets online as well. That doesn’t matter whether it’s in the U.S., whether it’s in the U.K., whether it’s in Australia, whether it’s in New Zealand, you will see similar numbers. Approximately 90% of intensive care patients survive. There would be many patients that survive that would’ve gone through multiple organ failure and would’ve come out of it. You got to look at those statistics, very important.
Now, also what is important to know is when I talk about survival rate, I am not talking about, how long people survive? What does their quality of life look like after intensive care? I’m not talking about any of that. I’m just talking about getting someone through the critical illness phase and getting them to leave intensive care. We don’t know what their life looks like six months down the line, six weeks down the line. But even if somebody is passing away after intensive care, I believe it’s still very important that families can spend time with their loved ones, especially at the end of their life. How people die plays a huge role for family’s peace of mind, for a patient’s peace of mind. Plays a huge role and it can never be underestimated.
Whereas ICUs often take a one size fits all approach when it comes to end of life. They’re saying, “Your loved one is too critically ill, let’s just stop life support.” You hear it over and over again. You hear it here on our blog because that’s what we are dealing with all day every day. Intensive care units take a one size fits all approach. We know that by at the end of someone’s life, you can’t take a one size fits all approach. It’s very unethical. It’s very immoral. It needs to be tailored towards the individual.
Anyway, coming back to our topic, “Multi-organ failure in intensive care, what’s the prognosis?” Let’s just quickly run through all major organs. Starting from the top, one major organ is the brain. Another major organ is the heart. Another major organ is the lungs. Another major organ is the liver. Another major organ is the kidneys.
When do people start about multi-organ failure? If one organ is failing, people tend not to speak about or talk about multi-organ failure. Intensive care doctors, nurses tend to start talking about multi-organ failure when a minimum of two organs are failing. Now, let’s look at this. Many patients go into intensive care with head or brain injuries, and then as a result of this, they end up on a ventilator.
A head or brain injury is at least temporary organ failure. The lungs being ventilated is at least temporary organ failure. One could argue that someone with a brain injury on a ventilator is in multi-organ failure and technically they are. But treatment is often still being offered. In the early stages of an ICU stay, probably nobody’s talking about multi-organ failure straight away, but it depends on the condition that someone goes into intensive care. Multi-organ failure doesn’t always happen from the minute someone goes into intensive care. It often happens as a result of being in intensive care. It happens as a result of treatment of deteriorating conditions and so forth.
Let’s just stick with the example for now with someone with a brain injury, someone being ventilated, two organs failing. Let’s just say on top of that, they might have got the heart attack and their heart is now supported with medications such as vasopressors, inotropes, they had to go to the catheter lab or they had to have cardiac surgery, whatever the case may be. Now, all of a sudden, you’ve got three organs failing. Not an uncommon scenario in ICU, not at all. On top of that, you might even have the kidneys failing and someone needing dialysis. Again, not an uncommon scenario. Let’s just stick with that for now. You’ve got brain injury, lungs are failing, someone is on a ventilator. Number three, the heart is failing because there has been a heart attack sustained. And number four, the patient is now in kidney failure, needs organ support from dialysis.
Now, the intensive care team might call a family meeting and might spell the bad news for you and might say to you, “Look, your loved one is in multiple organ failure. We think it’s futile to continue treatment.” If I was part of that meeting, my first question would be to dig down deeper, why are the organs failing? Are they reversible courses? Because that is one of the main questions. Are there reversible courses? Can this be reversed? Don’t get me wrong. The more organs that are failing, the more challenging it is to get organs back on track. But that should not leave intensive cares without trying.
Suggested Links:
For example, starting from the top again, starting with a brain. If someone is having a brain injury, it can take a very long time to wake up. Sometimes weeks, sometimes months, can take a long time to wake up. Let’s look at the ventilator. Can someone be weaned off the ventilator? If no, what are the reasons for it? Does the patient need more time? Are they still in an induced coma? Do they have a breathing tube in their mouth, or do they have a tracheostomy? If they have a breathing tube, do they need a tracheostomy that buys them more time to be weaned off the ventilator? Those are all the questions that need to be asked. Whereas intensive care teams just give you the short version and saying, “Well, your loved one is in multiple organ failure. Treatment is futile. Let’s just stop.”
Let’s go to the heart.
If they had a heart attack, can inotropes or vasopressor support the heart? Can vasopressors or inotropes be weaned? Which are also considered life support. Vasopressors or inotropes are also considered life support. It supports blood pressure, it supports the contractility of the heart, and so forth. Next, if there was a heart attack, can the patient have cardiac surgery, open heart surgery to fix the underlying problem? Does the patient need to go to catheter lab to fix the problem? Those are all the questions that need to be answered.
Next, let’s just go to the kidneys. If someone is in kidney failure, can dialysis fix the problem? A lot of patients in ICU go into kidney failure for a number of reasons. They often have dialysis, but it’s temporarily. It’s a temporary thing. Yes, some patients in ICU are newly diagnosed with kidney failure. They then go into temporary kidney failure. Then once they leave the ICU, they’re often off the dialysis. It’s often a temporary supportive measure.
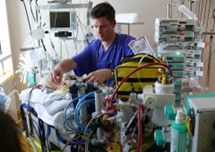
Now, also when you look at all major organs, just as I mentioned, brain, heart, lungs, liver, kidneys; heart, lungs, and kidneys can be supported at least temporarily with equipment. I’ll break this down in a minute. Now, you can’t support the brain with equipment. You can’t support the liver with equipment. You can support the liver by changing medications. You can support the liver by giving certain medications, but the liver is also hard to control. But the most difficult organ to control is the brain. There’s no brain transplant as of 2022. But there is a heart transplant, there is a lung transplant, there’s a liver transplant, there is a kidney transplant. You can see that there might be alternatives if people are resistant to treatment.
Next, if the heart fails and if all of the things that we discuss now are not working such as inotropes, open heart surgery, catheter lab stenting, balloon dilatation and so forth, angiograms, angioplasties, if that’s not working, maybe the next step is to get someone on ECMO (Extracorporeal Membrane Oxygenation). ECMO can be a bridge to a heart transplant. ECMO is basically a bypass machine that can take over the function of the heart and the lung for a period of time. How it’s being used? It’s often a bypass machine. It can be used to replace the function of the heart. Then patients often go on to an RVAD (Right Ventricular Assist Device) or an LVAD (Left Ventricular Assist Device) depending on whether the left or the right side of the heart is failing, as a bridge to a lung transplant. I have done different videos about this specific topic. I’m not going into too much detail there today.
The same is applicable for the lungs. If the lungs are failing and someone can’t be weaned off the ventilator, they are in severe lung failure and ARDS (Acute Respiratory Distress Syndrome), an ECMO can take over the function of the lung as well for the lungs to heal. If that doesn’t work, it can be used as a bridge to a lung transplant. Very important information. Most families in ICU have no idea about. If they haven’t done their research, if the intensive care team is telling you, “The best solution is to stop treatment.” You haven’t heard of ECMO. You haven’t heard of dialysis. You’ll be doomed and you absolutely need to do your research here. You can’t just take intensive care teams’ words for gospel because again, you might be doomed by doing so.
Also, with the supports that I described so far where you can support organs, someone can be in intensive care sometimes for many weeks. Now, there are side effects from people being in intensive care for many weeks. They might come out with disability, they come out deconditioned and they may never live the life again that they had before. But who am I to say what life people should live? And who am I to say how people should live their life? What’s acceptable for them for quality of life? Because that’s often the argument that’s coming from intensive care teams where they say, “Your loved one won’t have any quality of life if we continue to support organs with life support.” What is quality of life? It’s a very subjective measure. It’s not up to me to make judgments about what quality of life is acceptable for you, for your family member or for me. It’s nobody’s judgement. It’s your own decision and your family’s decision, what you want for your loved one.
Then, another scenario that is often leading to multi-organ failure is sepsis, which is what you alluded to, Modema, secondary infection. A lot of patients in ICU, they may not necessarily come with an infection, but if they do come with an infection, that infection might spread and might end up in a “fully blown sepsis.” If someone is in a fully blown sepsis, they often do go into multiple organ failure. Let’s just say someone has pneumonia. For whatever reason they end up with a sepsis. Then one of the side effects is that blood pressure is dropping significantly and then the heart is weakened because of that. Then, inotropes or vasopressors need to be started. You need to check for cardiac output numbers, cardiac index numbers to give you an idea how severe is the heart impacted. When patients go into sepsis, don’t get me wrong, they can die pretty quickly. I’ve seen that.
But I’ve also seen the other side of the spectrum where patients are in sepsis, their organs are failing and yet they get all the right treatment, then there might be septic for a few days and their life literally might be hanging at a threat for a few days and yet they do survive. It can be a very long road to recovery. No question about that. But the worst thing that you can do as a family is to give up. That’s the worst thing you can do.
Recommended:
It’s very important for families to put up a good fight for their loved ones. That’s very important for them mentally, spiritually, culturally, and you never give up hope. The worst thing you can do is give up hope.
Modema, you’re saying, “That’s what happened to my husband, over three weeks’ worth of ECMO, but he sadly didn’t make it.” I’m so sorry to hear that, Modema. You’ve seen ECMO. Was that for heart failure or for lung failure or potentially a combination of both?
While I’m waiting for your answer, Modema, one really needs to keep in mind again, the survival rate in intensive care, 90% and more. Treatment options are available. Knowing how you can support some organs at least for a period of time, very important for you to know that so that you know what options are available.
I see, Modema. Your husband has had Delta COVID, and the lungs were affected. That’s very sad to hear. But I would think that Modema, your husband at least would’ve had the best fighting chance while he was on ECMO to get through this. Because there are so many clients I’ve worked with since COVID started, where their loved one started out with COVID pneumonia or COVID ARDS that then got proned, but they never made it because they didn’t get ECMO as a treatment option. I’m not too surprised because ECMO was in short supply before COVID. The demand for ECMO would’ve gone through the roof. ECMO beds are in short supply, staff that are trained on ECMO are in short supply. There are all these issues.
But another question that you can ask if your loved one is in multiple organ failure, you could also ask that in some situation, is an organ transplant an option? Whether it’s kidney, liver, lungs, heart, not the brain. Like we said, the brain is the organ that cannot be controlled as far as we know in 2022. No options have been found to control the brain at least temporarily.
Now, I’m not advocating here for an organ transplant. Not at all. I’m not the subject matter expert on organ transplant. I have looked after enough heart and lung transplants in ICU. I have seen people being put on heart and lung transplant lists prior to getting the organ. But I’m not the subject matter expert on how people are being chosen to get on a transplant list. I do know the basics there, that age is a factor. Comorbidities or lack thereof is a factor, why people get an organ transplant or not. Really important for you to do your research there, whether that’s an option or not.
You’re saying, Modema, that your husband was a physician himself, but he ended up with COVID sepsis. He had the very best care at Duke University. He was perfectly healthy too and only 47 years old. Oh, my goodness. That’s so sad. Very sad to hear that. At least he had the best care and at least you’ve given him the option. I haven’t heard that many COVID patients that end up with irreversible lung failure have had lung transplants. I haven’t heard much of it. Your husband wasn’t offered a lung transplant for example?
The other question that you need to ask, if you have a loved one with multiple organ failure, one of the most important questions you need to ask is, is it reversible organ failure? Now, if they tell you, it’s not reversible, why is it not reversible? Why do they think it’s not reversible? If they say it’s not reversible, why do they think it’s accurate? Again, that’s where we can help you with a second opinion. Because I’ve seen enough of my fair share of organ failure. I’ve seen enough of my fair share of patients in multiple organ failure survive and leave intensive care alive.
Now Miriam, welcome to the live stream. Now, you’re saying, “My dad has been diagnosed with lung fibrosis, he is 70. This was caused by COVID. We asked for a lung transplant as he was struggling. They paralyzed him. Will that exclude him for the transplant? They gave him paralytic medication last night.” Miriam, even though I’m not the subject matter expert on how people get chosen for a transplant, what I do know is this, the cutoff for an organ transplant is generally speaking at 65. I would argue if your dad was 20 years younger, that he would have a good chance to get on a transplant list. But at the age of 70, I think it’s highly unlikely that he will end up on a transplant list. It’s simply driven by an age cutoff.
The same probably applies to ECMO. Because ECMO can lead to a bridge to a lung transplant or a heart transplant. Therefore, the cutoff for ECMO I’ve also seen is around age 65. It’s very sad. One can open the debate whether that’s right or wrong. As far as I can see, that’s based on my realism after having worked in the industry for over 20 years and after having worked with ECMO patients. For example, again, ECMO machines are in short supply. Staff that can look after ECMO are in short supply. Intensive care is a specialized skill. ECMO is an even higher specialist skill. It’s a niche within a niche. It’s very difficult to look after ECMO patients.
I’m so sorry, Miriam, that I can’t give you any better news here. I’m really sorry. How long has your dad been in ICU with the lung fibrosis? Can you give me a timeline, Miriam?
Now, Modema, you’re saying, “The thrombosis clotting ended up being an issue. Dual hemisphere hemorrhagic brain bleed was the end of him.” Because he was on heparin while he was on ECMO, that unfortunately got him to bleed. I’ve seen this unfortunately, Modema, that patients on ECMO, on heparin end up with a brain bleed as a side effect and it’s deadly. It’s very sad. Very, very sad to hear that. Doesn’t happen often, but it does happen. They may have not titrated the heparin well enough. Maybe they’ve made a mistake there. Have you asked that question?
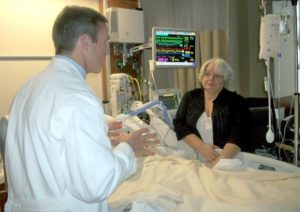
Now Miriam, you’re saying your dad has been in ICU for 60 days. He has a tracheostomy. Do you know the ventilator settings he’s on? If you know that, just type them in because that will help me to hopefully point you in the right direction, if you have the ventilator settings that he’s on.
Miriam, while I’m waiting for your question, with lung fibrosis, the issue is that lung fibrosis basically means there is scar tissue in the lungs. That can make it very difficult to wean someone off the ventilator. But in any case, “PEEP (Positive End-Expiratory Pressure) of 10 and 80% of oxygen”. Those are high settings which will make it very difficult for your dad to come off the ventilator, especially after day 60. Is your dad awake, Miriam? Is your dad awake? Can he interact with you or with other family members or with the doctors?
I’ve got someone else who wants to ask a question, Yagz, I’m not sure whether I’m pronouncing your name correctly, but I’ll just read this out. Yagz says, “I was also told my dad has multi-organ failure. He had the Delta variant and unfortunately passed on the 28th.” I presume 28th of February. “He was 65 and had a kidney transplant in 2017. His ventilator parameters were a 100% saturation and 28 of PEEP.” I questioned that he wasn’t a PEEP of 28. I do question that the highest PEEP that I’ve seen, it’s probably around 20. I’m very sorry to hear that, Yagz, that he didn’t survive the COVID.
Miriam, you’re saying your dad was awake until last night. “He is now on paralytics because his oxygen was on the 70s.” I see. They started to prone him, Miriam? Is that what they’re doing now? Those are tricky situations. I feel like with your dad’s age, that there will be limited options for him. But then again, just because they’re saying he’s got lung fibrosis, do you have any evidence for that? Have you got access to the medical records? All these questions need to be asked. As I said, are they proning him? Those are all the questions. You don’t think they prone him.
Why are you saying he’s no longer rousable or can no longer talk? Why do you think that is? What has happened that they put him back into a coma? I presume that’s what you are referring to, that he’s gone back into a coma. What was the reason for that? His oxygen was in the 70s, which is pretty low. That in and of itself might be enough to get him paralyzed, but it might not be enough. What else is happening? Has he gone into multi-organ failure because he’s septic? Do you know what else has happened to get him go back into the induced coma? Because if he went back into the induced coma with lung fibrosis and they paralyzed him, I’m almost bound to say you should prepare yourself for bad news. You should prepare yourself for the intensive care team, “framing your dad’s situation,” as if the only next thing that would be “in his best interest,” would be to end his life and stop life support. You should prepare yourself for that, unfortunately. But we can help you with the family meetings there.
Miriam says, “He was improving and then started having episodes where his oxygen was dropping.” But why is his oxygen dropping? Have they done a chest X-ray? Have they done a CT (Computed Tomography) scan of the chest? Have they done arterial blood gases? What are the reasons for his deteriorations? “And the CT showed lung fibrosis in both lungs.” How long ago was that Miriam? When did they do the CT scan of the lungs? Because if they’ve paralyzed him and put him back into a coma last night, what’s the reason for that? What’s the reason? “That CT was two weeks ago.” But if his oxygen dropped last night, they should have done some diagnostics last night like chest X-ray, maybe a CT scan of the chest, arterial blood gas. It would be good to know. Did they change the ventilator settings and so forth? That would be very important information to have and to know.
The more information, the better. That’s why I keep saying, the biggest challenge for families in intensive care is simply that they don’t know what they don’t know. It’s one thing for events to happen and they do happen unfortunately in intensive care. Events can sometimes spiral out of control, especially when it’s important to ask all the right questions. Again, my question is, why did he go back into the coma and was paralyzed? Has he had a chest X-ray, arterial blood gas? Has he had a bronchoscopy, chest CT scan? I would want to know that. Is there anything else that’s happened? I don’t know.
Suggested Links:
I was alluding to another case study that I talked about earlier. Did he have maybe a heart attack? God forbid. Always important to ask the right questions. Always important to ask the right questions. You don’t know what you don’t know. There’s a reason for why he’s oxygen levels dropped. It might be directly related to him having lung fibrosis. But all the other questions need to be asked as well.
What other questions do our viewers have? I’ve seen that Helene is on now as well. Welcome, Helene. Nice to see you again. What other questions are there that you have while I’m still doing this livestream? Would be very curious to know what other questions you have.
In the meantime, while I’m waiting for your questions to come through, I just want to thank you for your support and for coming on to the livestream over and over again. If you’re finding value in this, maybe you can spread the word. Maybe you know other families will continue doing them because I really enjoy doing them.
Now, Miriam, you’re saying, “He had a bronchoscopy, but two weeks ago, he was doing great and then he started having anxiety attacks, they said” “It’s tachycardia. They call it sometimes, the distress.” Tachycardia is a symptom of the distress. Tachycardia means the heart rate is above a 100. It’s probably a symptom of the distress. “They wanted us to sign a DNR a month ago.” I presume you haven’t done that, Miriam. Have you signed a DNR?
With the anxiety, Miriam, what often happens is, especially with lung fibrosis, your dad would be physically and potentially psychologically dependent on the ventilator. I’m not surprised he’s got anxiety attacks because with the lung fibrosis, he may not have progressed at all to get off the ventilator. That could cause anxiety. He might feel like he’s not strong enough to get off the ventilator. That might cause anxiety on the other end. That can be a vicious circle.
It sounds to me like your dad is in a very difficult situation. It sounds to me like the next step is not quite clear to you. I would like to know more about what’s exactly going on there. Maybe look at medical records, maybe talk to the doctors so I can guide you there.
But in any case, look, I do want to wrap this up in the next five minutes. If you have any questions, please type them in the chat pad now. I also want to thank Modema and Helene to support Miriam with her grievances about her dad.
Yagz is saying, “Sorry for the interruption, what question should I have asked when my dad was intubated at a 100% oxygen and to 20…” He was on that much PEEP. “23 to 25 of PEEP. CT /X-ray scans showed COVID pneumonia and the blood clot.” My advice there would’ve been when would ECMO have been an option for your dad, Yagz. Other questions that should have been asked is, I’ve done a video and a blog post a while ago where I listed all the questions that should be asked when you have a loved one in intensive care. I have done a video and a blog post about that. All the questions are there.
But it also comes down to, you can’t just look at the lungs in isolation. You also need to look at the other organs, which brings us right back to our initial topic about multiple organ failure. You can’t just look at one organ in isolation. Are the lungs failing because your dad had a heart attack, or your mom had a heart attack? Are the lungs failing because your loved one is in kidney failure and now there’s fluid buildup on the lungs? Are the lungs failing because there’s scar tissue?
This is why I keep saying the biggest challenge for families in intensive care is simply that they don’t know what they don’t know. They don’t know what to look for and they don’t know what questions to ask.
There’s a whole range of questions that you need to ask in a situation like that, Yagz. It’s not a one size fits all. You’re saying, “His kidneys failed and was on dialysis during his time in ICU for three weeks.” In order to give you a conclusive answer, Yagz, I would need to look at medical records. I would need to look what are the other organs doing. Unfortunately, I can’t give you a conclusive answer with the information that you’re sharing. It would need to take an offline discussion, would need us to look at medical records and so forth.
Helene, you’re asking, “Is there a waiting period given to families in order to process the decision to change the DNR (Do Not Resuscitate)?” No, it’s as per need basis. If you decide today you want to sign a DNR for your loved one and you change your mind tomorrow, you change your mind tomorrow. And, they need to revoke it. I have not seen any timelines around that, Helene. It’s really up to your family’s decision of what they want.

I want to wrap this up slowly. I will do another YouTube Live next week around the same time, 11:00 AM Sydney, Melbourne time. It’ll be around at 8:00 PM, Eastern Standard Time in the U.S., 7:00 PM Central Standard Time in the U.S. next Saturday, 6:00 PM Mountain Time in the U.S., and 5:00 PM Pacific Time. Unfortunately, it’s in the middle of the night in the U.K., but you can watch the recording here when it goes live.
Yagz, look, I would love to have you even getting closure now, because that’s sometimes what we do as well. Looking at medical records even when patients have passed away to find closure for people.
Helene, you’re asking, “Should doctors pressure family to change DNR?” Probably depends on which way you want to change DNR, Helene. Because sometimes they may even be in favor of revoking a DNR, but most of the time, they are in favor of having a DNR. I don’t think that families should get pressured to sign a DNR. I don’t believe in that at all. I strongly refuse that notion.
Recommended:
“I will be there to watch, I am in the U.S.”, great. Yep. No, I have been doing them now weekly for quite some time. I had a bit of a break around Christmas time because it’s been so busy with clients. But I’ll try to do them. It’s Sunday morning for me here, but it’s Saturday night for our audience in the U.S. I’ll try to do them every week. I’ll get immense joy out of this because yeah, I’ll enjoy interacting with you guys and answer your questions and seeing your interactions there.
Look, I need to wrap this up.
Now, if you have a loved one in intensive care, go to intensivecarehotline.com. Call us on one of the numbers on the top of the website or send us an email to [email protected].
RECOMMENDED:
If you find value in this video, give it a like, subscribe to my YouTube channel so you get notifications about updates and livestreams for families in intensive care, and click the notification bell for new videos.
I really want to thank you for your support.
This is Patrik Hutzel from intensivecarehotline.com and I will see you again next week around the same time.
Take care for now.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!