Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode was
You can check out last weeks question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to continue answering the next questions regarding James’ and Christine’s Dad in ICU who’s had a haemorrhagic stroke.
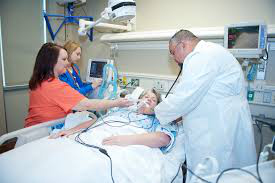
James’ and Christine’s Dad had a brain decompression where they evacuated a large bleed from his brain after the haemorrhagic stroke. And their Dad also underwent a craniectomy (partial removal of skull) to decrease the brain pressures after the bleed.
James’ and his sister Christine were getting their Dad in one of the best hospitals in the USA, the Cleveland clinic in Ohio.
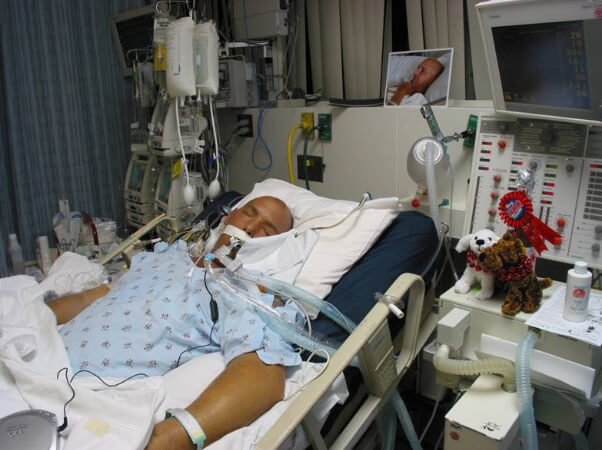
In the meantime, their Dad was getting a tracheostomy because he couldn’t be weaned off the ventilator and the breathing tube. He also had a PEG tube for feeding inserted.
He also had ongoing seizures due to the stroke and his anti-seizure medications needed to be optimized so he could “wake up” and progress to Neurology Rehabilitation.
In today’s 1:1 consulting and advocacy sessions with James and his sister Christine, we look at some setbacks their Dad is going through.
He had to be put back on the ventilator due to a Pneumonia and he also ended up with a central line (CVC) and arterial line again.
In the meantime he has come off the ventilator but still has the tracheostomy after over 5 weeks in ICU.
This series of 1:1 consulting and advocacy is a real testimony for getting advice, run with it and get results.
If you want to avoid LTAC and a nursing home for your loved one, you need to read all of the consulting and advocacy sessions with James and Christine!
So in today’s episode of “YOUR QUESTIONS ANSWERED”, I answer a series of questions from James and his sister Christine again that are excerpts from various 1:1 phone/email consulting and advocacy session with me and the topic this week as part of this series of 1:1 consulting and advocacy session with me and the topic this week is
Dad’s going to step down after 5 weeks in ICU! Where should he go to next?
You can also read or watch previous episodes of 1:1 consulting and advocacy with James and his sister Christine here
Patrik: Hey John, how are you?
James: Good. Are you working it tonight?
Patrik: Yeah, it’s all right. I’m just on a break. It’s all good. So I’ve seen in your email that they want to send your dad to step down tomorrow, do they?
James: Well, that’s what they’re saying, but there’re saying they don’t know if they have a bed available. We talked to the ICU doctor today and he made it sound like the earliest he’d be moved is Monday.
Patrik: Right, Monday. Look, if he’s been off the ventilator for now 48 hours, I do think it’s a good move. I do believe that. Yeah, to get him to step down, and the reason I’m saying that is, you don’t want … the ICU environment is all good for a certain period of time, but it’s not a very conducive environment, you know? And, given that he’s in the hospital, and given that he is close to the ICU, I would be much more worried if they, say … they move him to LTAC tomorrow, you know? But that’s not happening so I think step down is fine if he’s off the ventilator. That’s the main thing.
James: Well, I’m glad that you said that, because I was kind of thinking the same thing. Like, move on, but I’m just concerned that … I mean, first it was, “It could take a month to a year to wean off the ventilator–
Patrik: That’s right.
James: … so he really needs to go to this LTAC (Long term acute care facility).
Patrik: Absolutely.
James: You know? So he really needs to go to the LTAC, and now they manage to get him off the ventilator in four days.
Patrik: Yeah, and that’s very positive. That’s very positive.
James: Well, my question is, are they doing it too rapidly?
Patrik: No, not really. Not … If he’d been in ICU for a week, then I would question that, but if he’s been in ICU now for five weeks … keep in mind he’s off inotropes, off the vasopressors. He will be off life … The minute he stops being ventilated, he’s off life support, right? And that’s really positive.
James: Right, but my question to you is, did they wean him off the ventilator too fast.
Patrik: No, no, no, no, no, no. If he can tolerate that, no. If he can tolerate it, no. Definitely not.
James: Okay.
Recommended:
Patrik: The main thing to look for is, can he tolerate it?
James: Well, they were doing this reinflation every four hours.
Patrik: Yup.
James: And now they’re saying they’re not doing that anymore.
Patrik: That’s right.
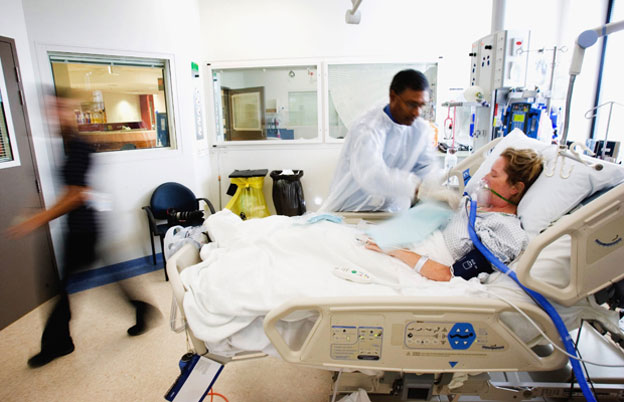
James: I guess … They were putting him on the ventilator every four hours and now they’re just going to … they use this thing every four hours to blow up his lungs and clear his throat.
Patrik: And they might still be able to do that on the ward, or on the step down, right? So that could still be a possibility. Do you know who’s doing that? Is it the physiotherapy or is it the respiratory therapy? Do you know who’s doing that, the inflation?
James: The respiratory therapist.
Patrik: That’s okay. Ask them if they continue to do that. Ask them. I think there’s a good chance they will.
James: Yeah. They said every four hours.
Patrik: Yeah. Yeah. As long as they keep doing all of that, I really do believe going into step down will be good. I feel … as I said-
James: Right.
Patrik: For the right…
James: … understand, they’re not putting him back on the ventilator every four hours. They’re doing it manually with-
Patrik: Right.
Recommended:
James: … all those breathing tests.
Patrik: Right. I think there’s a very good chance they might continue doing that. There’s also a very good chance that the respiratory therapy and the physiotherapy will continue to assess him over the next few days. Right? And that will make sure he’s moving in the right direction.
James: All right, well, that’s good to know. I mean, they made it sound … You know, they change their tune every day and they made it sound yesterday like, “We need to reinflate him every four hours.”
Patrik: Right
James: And I think maybe he wasn’t quite there yet. So now they’re going from pulling out his ventilator, going backwards, and “Now we’re going to use this manual thing to reinflate him instead of the machine.”
Patrik: Right. Look, as I said, I think it’s time that you leave the ICU if you can. The minute he’s off ventilation, he’s off life support … when patients are off life support, that’s the time when they can leave ICU.
James: How long do you think we have in the step down?
Patrik: Say again?
James: How long do you think we will have in the step down?
Patrik: Probably another … Depends. Probably another week, I’d say, but I think the next challenge for you will be not so much how long will he be in step down; the next challenge will be, what will be happening after step down. A rehab bed might not be available straight away.
James: Right, and they do have a rehab facility here with a rehab bed, so-
Patrik: Right, so you need to find out what the next steps are from step down. That’s your next sort of question you need to ask to them.
James: Okay. All right. Well, that’s good advice, Patrik. So, I mean, if my father’s not being put on the ventilator and he’s breathing on his own tonight, should I be worried? Should I be worried???
Patrik: Ah, yes. Yeah. If they put him back on the ventilator tonight, then you’ve definitely got to raise the question whether they can do the same in step down, and in some step downs, they might be able to do that. Right?
James: Right. No, my question is, if he’s breathing on his own tonight, through the night, should I go check on him in the middle of the night, just to make sure he’s okay?
Patrik: No, they will do that. I think what you might want to do is, in the morning, ask them whether he stayed off the ventilator overnight or not. I think that’s a question to ask.
James: You know, I just got kind of a weird conversation, because I was there. They said tonight … they have around 10:00 tonight.
Patrik: Right.
James: And the nurse in charge pulled me aside and said, “We know you and your family has been video recording and voice recording us, and that’s not permitted in the hospital here,” and blah-blah-blah.
Patrik: Right.
James: I really had no idea what the hell she was talking about, and then we got the news that, “Oh, and he’s moving to the step down tomorrow.” I don’t know, these people are just very difficult around here.
Patrik: I tried … Look, they are difficult because you’re asking all the right questions, so take … as I said before, take that as a compliment, but at the same time, you’ve avoided the LTAC. He’s now going to step down, and for now, he’s moving forward. He’s made a lot of progress in the last week. You know? Don’t worry too much what they do or what they don’t do. I would just sort of-
James: Do you know from a hospital setting, are you not allowed to voice record-
Patrik: Look, it depends really. They might have some policies. They might. But, on the other hand, I would just … you know what my response, probably, would be: “Do you have anything to hide?” That would be my question to them. You know? That would be my-
James: That’s the thing.
Patrik: … question.
James: Like, hide in regard to what?
Patrik: Well, what’s so secretive about what they have to say? That would probably be a question I would ask if I was you. You know, what’s so secretive about it? Nothing, really, is it?
James: Right. Exactly.
Patrik: Right, so-
James: That’s funny that you say that.
Patrik: You know? I would just ignore.
James: Yeah, I have. That’s good advice. It just kind of caught me off guard. I think it was just something to try to bother me because I’ve been short with them all week. I mean, it’s been a long week here.
Patrik: It’s been a long five weeks for you.
James: Absolutely. Well, he was in the ICU in New York for a week so he’s been in this ICU for four weeks but I don’t think four weeks in an ICU here, after a craniectomy, is that long. He just started coming around this week and now it’s like, “Well, he’s got to get out.”
Patrik: And he does. He needs to get out. It’s the right place at the right time for a critically ill patient. Your dad is sick but he’s not critical anymore.
James: Right. I agree. I agree. All right. That’s good advice. I appreciate it. I’ll let you go. I’m going to get some sleep.
Patrik: Okay. Okay, you can get me over the weekend anytime.
James: Thank you very much, Patrik.
Patrik: Okay. You’re welcome. Have a good night. Have a good night. Bye-bye.
James: Okay.
Patrik: Bye.
James: Bye-bye.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!