Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another frequently asked question from one of my clients and the first question in last week’s episode was
What are the chances of survival after a tracheostomy?
You can check out last week’s question by clicking on the link here.
In this week’s part 5 episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next questions from one my clients RICHARD as part of my 1:1 consulting and advocacy service!
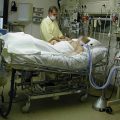
Richard’s mother suffered from a fractured bone due to a fall. His mother was then transferred to the ICU due to cardiac arrest and had a tracheostomy during her stay in the ICU.
I don’t think the ICU wants to help my mother to fully recover and get off the ventilator. How can I find out?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Richard here.”
Patrik: That’s right. I said to him, “By not being transparent in your decision making …” If they had told you yesterday, “Oh we’ve sedated her because we want to improve ventilation.” Well, you probably could have accepted that.
Richard: Well, they didn’t say that to me. They definitely did not say that to me at all. I agree with you. It would have been helpful information to understand that that was their true or false, but that was their presentation.
Heather: Yeah because the way things are going now with that sedation, Richard may have missed, I’m sorry Richard to say this, your last chance to have a communication about consent and whatever with your Mum and her wishes.
Richard: I believe that unless something’s changed that’s almost certain. That’s my feeling at the moment. Looking at where she’s at, looking at the drugs, looking at medication, look her situation in terms of what I call zero alertness I think whatever window that did happen was very limited, because of what had been going on, but that that’s now gone. I was very clearly, I was wishing to do that, was endeavouring to do it, but Mum wasn’t ready at that point. She was too unwell. In that very moment they gave me, a very short period of time for me to step back. Quite frankly I had a clear though of how things going on, including obviously navigating that systems. You know already how difficult is that. That’s slowing me down in terms of any true ability to work with my Mum on that.
Richard: Hello?
Patrik: Hi, Richard. It’s Patrik again.
Richard: Hello?
Patrik: Can you hear me?
Richard: I had a call but-
Patrik: Yeah, I took me, I couldn’t get through straight away that’s why it took a minute. That’s okay. I should be back now. So you know he was, he kept-
Richard: -Can I just ask one?
Patrik: Yeah, yeah of course Please.
Richard: That’s fine. That’s perfect. Thank you.
Patrik: He did ask where I was. He asked me when I last saw her and I said to him ‘Look, I’m overseas.’
Richard: He came around to it?
Patrik: Yeah it was no big deal at all…
He knew … Well he was under the impression that the Australian healthcare system might be a little bit more advanced than the Irish, but it might have been just to appease me or-
Heather: To take your side probably.
Patrik: That’s right, that’s right.
He kept referring back to that 30-day mark, because he did ask me ‘Oh, would you keep a patient ventilated for longer than 30 days?’ And I said to him ‘Look, of course you would if there is a hope for improvement.’
Richard: Yeah.
Recommended:
Patrik: Right?
Whereas from my perspective, it sounded to me like, in their mind it’s sort of the 30-day mark, if people are not improving-
Richard: -Yeah.
Patrik: … we’ll change tacts.
Heather: Yeah.
Richard: Yeah. I agree with that. That feels… I feel like that’s the way I feel. I agree.
Patrik: Mm.
Heather: Yeah. They will start saying ‘Hmm, their quality of life won’t be great.’
Richard: Yeah.
Patrik: That’s right.
Richard: But they have their own which they have seen this twice. I’ve had it about 14 days ago and now this time. And they were like ‘We don’t think she’s getting any significant improvement. It would cruel, untimed, undignified to carry on leaving her in that state with no sign of improvement.’ They kept on saying ‘No sign of improvement.’ And I believe there has been improvement.

Heather: And it’s coming up to Easter here which is always busy in A&E.
Patrik: Absolutely. And expensive because it’s public holiday.
Heather: Yes.
Richard: Ah, okay. Absolutely, yes.
Patrik: Mm-hmm (affirmative). So there’s all of that. So I tell you what I think is next, especially since… Once I had the insights that I thought I needed. As I said, one thing that stood out to me. He tried to keep the conversation going to sort of you know almost tell me what I should tell you.
Right? Right?
Because to a degree, he probably felt like, well you know, I know what I’m talking about. And he thought ‘Okay, well you know-
Find more information about staying positive for the patient:
Richard: You could make it in very simple terms.
Heather: Yeah.
Patrik: Right, right. So, I think what’s important from this point onwards is that given that he said they sedated her in order to improve her ventilation. Right? That’s …
Richard: Yeah.
Patrik: I think that’s your hook for now.
Richard: Okay.
Heather: Okay.
Patrik: Right? Because-
Richard: -Once they improve her ventilation that’s meant to improve her breathing. Is that what you’re saying?
Patrik: Very much so. Very much so. I mean, if you go out then, if you go back into the unit now… The last picture that you sent me. Her volumes were about around 400 mils and they should almost be double.
Richard: I think it’s even 350. But, yes, it was either 400 or 350.
Patrik: Yeah, right, that’s right. They should almost be double. You know, and if they’re not achieving that. Well what’s the point of sedating her?
Richard: Right, okay. Is that a mechanical setting that was trying to help her breathing in some way?
Patrik: Say again?
Richard: That’s in odd terms, to make the 400 in 800 in simple terms?
Patrik: Sorry, I didn’t get that. Say that again, please?
Richard: When you say, if you are talking about let’s say in simple numbers, 400 to 800.
Patrik: Mm-hmm (affirmative)
Richard: Is that something that they can control to make it 800?
Patrik: Oh, yeah, yeah. Yes, indeed. Yes. Definitely.
Richard: It’s their controls of their machines in simple terms.
Patrik: Very much so-
Heather: -One caveat there …
Richard: One second.
Heather: Sorry. One caveat. I’m not sure… There is one thing that the anesthesiologist had said all along. It takes absolutely minimal sedation, as in amount of stuff, to sedate her. I don’t know if that has any bearing on this conversation or not.
Patrik: I think it does. I think it does and I tell you why. You shared with me earlier that she’s about 118 kilo. At the moment, from the pictures that you sent me, she is getting four milligrams of morphine and four milligrams of Midazolam.
Richard: Exactly. I was going to ask you about that level. Is that high or low?
Find more information about weaning a ventilator:
Patrik: Well, well-
Richard: -Is that going to be reduced?
Patrik: Yeah. So if there was somebody with a body weight of 60 kilo. Right? That would be a lot. Now with your mother’s sort of weight, I’d say, if they were really working her up for an end-of-life situation she would probably on ten and ten.
Richard: Okay, right. Ten and ten.
Patrik: Right?
Richard: Okay. Thank you.
Patrik: So I can give him the benefit of the doubt probably for about 24 hours, that he says ‘We’re doing this to improve ventilation.’
Richard: Okay.
Patrik: Right? If she was on ten and ten, I would say there’s no way. But with four and four, I can give him the benefit of the doubt for about 24 hours. You know, they might have good intentions, but you know I wouldn’t be sure. You will probably know in the next 24 hours.
Richard: Okay, thank you.
Recommended:
Patrik: So the other thing that he suggested is … So have you heard of the drug named Propofol?
Richard: Yes, I think I saw it on your website. And I think it’s what they were using.
Patrik: I’m sure they have. I’m sure they have.
Richard: They could add some morphine at the very beginning as well I think. I can’t quite remember. I think they did some at the very beginning. But then they thought she had a neck injury, and all sorts, which she didn’t have at all.
Patrik: Right. So, because you know, what he is saying is that once they’ve improved the ventilation that they will also change her sedation.
Richard: Right, right.
Patrik: Okay. Which, again, I’m not sure whether he just said that to sort of you know put a different ‘spiel’ on the whole situation or whether that’s really-
Heather: Yeah.
Patrik: Look, I think we can safely give him the benefit of the doubt for 24 hours, but then-
Heather: -I’d agree. If that had come from the other consultants, I wouldn’t believe them. I’d be more like give them a margin, yes.
Richard: Different margin.
Heather: Yes.
Richard: The thing I would say, in case this affects anything you want to you sign so that I think possibly those levels and those drugs may well have been prescribed by a talented doctor.
Patrik: Yeah, yeah. Sure.
Richard: She also seemed a very generally speaking, a positive person in terms of relatively good reputation, faith in her. Although I’ve only seen her once, it’s only based on hearsay and people have told me.
But that’s not to say she hasn’t been influenced by other people, other factors.
Heather: Yeah.
Richard: And just in terms of him, actually making those decision choices of which drug or amount, it may well have been the order of the doctor, not him. I don’t know if that makes any sense. Or in conjunction. Or in conjunction possibly. Right? It seemed to have started at from 13 in the morning.
Heather: I haven’t…
Richard: 43
Heather: Yeah.
Richard: 44
Heather: Yeah.
Richard: Maybe. Possibly. I’m not sure because at that stage.
Patrik: Mm-hmm (affirmative).
I also think that he had enough insight to know that the situation is causing you so much stress and anxiety that he felt that he had to take this call because he realized they’ve almost cornered you in a situation where you feel very upset about this.
So he had enough insights to know ‘Okay, well I really need to take this call because enough anxiety has been experienced by them as well.’
Find more information and recommended articles about controlling the situation:
Heather: Already.
Patrik: Right. Already. Exactly. Right. So he had enough insight there.
Heather: Yeah. The ward sister who organized that phone call today would be of the same minds.
Patrik: We might.
Richard: She formed the opinion quietly so-
Heather: -Correct, yeah.
Richard: It felt a bit confused, unsure of herself. Almost panicking because not giving them trust. I explained very politely but nicely. The communication is just a wall sometimes, hasn’t been what it should be, but she couldn’t understand on how she could..
Patrik: Right.
Richard: He handled it. And even with him, this is intensively for him. And Mom was saying ‘Please, help. I don’t understand. I’m thinking in a box’. So I think what you’re saying is spot-on off. And he was a bit more aware that things hadn’t gone right.
I hadn’t felt that I’d been supported. I support my mum. Thank you.
Patrik: And that’s what I said to him. I said all you are looking for is number one, transparency, and number two, inclusion in decision-making.
Now the other thing that I found a little bit strange in the beginning. And I don’t want to get too medical here but when I first asked him about ‘Why, the sedation?’. He said to me that when you ventilate somebody you give them sedation. And generally speaking, I agree with that. However, because I knew she had a tracheostomy, I said to him ‘Why would you sedate somebody with a tracheostomy?’ Right?
And initially it almost sounded like that he had forgotten that she had the tracheostomy. And I just thought ‘This is really strange.’
Maybe it was a test for him to see whether I am, I do know about the topic. It could have been a test from his side. Right? But I found it very strange that he says to me ‘Well, you know that we’re sedating patients when we’re ventilating them. ‘I said ‘Of course I do, but not with a tracheostomy.’
And that’s when he said ‘Oh yeah, that’s because we want to improve the volumes … because she’s not coping at the moment.’ But I found it very strange that he went in those roundabout ways.
Heather: Yeah. To cut a long story short. From talking to the nurse, I would suggest that was a test.
Patrik: Right.
Heather: Here when we’re dealing with stuff over the phone.
Patrik: Right.
Recommended:
Richard: That sounds very exactly what you’re saying. that he was basically checking what you basically thought of what he was suggesting. In simple terms, he wanted somebody that was on a par with him.
Patrik: Yeah.
Richard: And if you weren’t, he could obviously then outwit you. And if you were on the page, then it would be more difficult for him to outwit you if that makes sense?
Patrik: That’s right. And…. Go on.
Heather: I was going to say it’s also kind of partially a legality type thing to make sure that they have, we have given our consent. And that they do the person given to them does have knowledge. You know. We’re not friends who do not have knowledge. Yeah.
Patrik: Okay, okay. The other thing that I mentioned to him is, and I say that to everyone, because I’ve been dealing with those situations for a long time. Whether it’s what I’m doing today or whether I’ve done it in clinical practice. Right?
People … and I said that to him. I said ‘People can accept death and dying. People can accept end of life. The way professionals go about it with families, that will make or break the acceptance.’
Heather: Yeah.
Richard: Yeah. Absolutely. That’s very, very important. Yes, I agree.
Patrik: Right.
Richard: And there’s where one of my patients. It’s going to be a tough journey. But what I don’t want is, in terms of the living now, without the honesty, transparency and decency to talk it through by saying ‘We’ve done everything.’ And know they’ve done everything. etc. etc.
Heather: Yeah, because we made a promise to your mother-
Richard: -Yeah.
Heather: … and we’re keeping it.
Richard: Yeah. At least we will do our best by her.
Patrik: Or your mom.
Richard: Or Mom. Absolutely, including Mom.
The first thing that I think although her speech was obviously aware a few days ago there were definite signs of her having some awareness, some alertness.
But she certainly wasn’t depressed right now. But now, apart from hearing herself, she can’t even talk right now etc. etc.
So she simply can’t do that on her own.
But thank you very much. Yes, I agree with you that the approach of the family should be the truth when you handle.
Recommended:
Patrik: Mm, yeah, yeah.
So what do you think you are going to do next from here? What do you think are your next steps from here?
Richard: I was going to ask you the same.
Patrik: Okay, yeah, yeah, yeah. No, you can, you can.
I, even though he was nice and to a degree understanding, I do not trust him. I do not trust him in terms of that he said ‘ Oh, yeah. We’re sedating her because we want to improve her ventilation.’ I do not trust him on that.
You will find out in the next 24 hours, but I would hold him accountable for that.
Richard: Yeah.
Patrik: Right?
I would certainly also ask him about that 30 day mark. I mean, you know, maybe she only needed 35 days to improve.
And the other thing. Yes, sorry. I forgot about that. The other thing that I didn’t get an explanation for was … I said to him ‘How can she go from being mobilized and breathing spontaneously to being back in a controlled ventilation mode? And not mobilized and back in an induced coma?’ Right?
I said to him ‘Why would you?’ To a degree he was a bit wishy-washy then. On the one hand he said ‘Well, if people are not improving after 30 days and there’s no outlook for quality of life then we obviously have to do what’s quote unquote in the best interest of a patient.’ Well I don’t agree with that.
And number two, saying that her clinical condition deteriorated that they had to put her back in a controlled mode and back on sedation. I said to him ‘ I still can’t believe how she can go from getting out of bed two days ago and now she’s fully ventilated again.’
Related article/video:
Heather: Yeah. Why wasn’t somebody called in and before the last three-day deterioration? Why wasn’t somebody called in earlier than those three days?
Patrik: Correct.
Heather: You know the ball. It was an intern who just attending them or whatever they called. You know.
Richard: I’m running on battery. We’ll carry on once we can and make the decision on the phone if needed. But will for the minute just explain in case it drops. Thank you.
Heather: Yeah. And in case you see a different number come up.
Richard: Yeah, exactly.
Patrik: Sure, sure.
But for now I think you need to hold them accountable for reducing the sedation once her ventilation has been optimized. Right? Because she needs to be woken up to be informed about what’s happening to get some response from her.
You know, the other excuse that he made was that it’s difficult to communicate with somebody with a tracheostomy. Well, we know all of that. That’s not news. That’s no news.
Heather: Yeah. We had the lip needle organized.
Patrik: We had the lip needle organized except obviously with no heavy sedation. That’s how it worked.
Heather: Yeah.
Patrik: Right, right. And I think that should be the goal. To wake her up and get a response from her. I think that would be really important. I think it would be very important for you as a family, for your own peace of mind.
Richard: I appreciate we made a quick decision, Just your general opinion.
Patrik: Say that again please?
Richard: I think she’s had deteriorated I think. Did you at any point had this conversation.
Patrik: Sorry, sorry. You’re dropping out. What deteriorated?
Richard: Sorry. There were two things. You mentioned about the album in the possible contingency. Could that?
Patrik: No. I didn’t, I didn’t.
Richard: Okay.
Patrik: And what was the other thing?
Richard: To me that was the main thing was that…
Patrik: No, no.
Richard: Okay, thank you.
Patrik: I didn’t. No.
Richard: I’ve got a point about the ABG (Arterial Blood Gas). Did you discuss ABGs at all?
Patrik: Not in detail, but he pretty much … For an intensive care professional, it goes without saying that if she goes from a spontaneous mode to a controlled mode, that her ABGs have deteriorated.
Patrik: The other reason it goes without saying is, when you’ve shown, when you’ve spent the last pictures, her oxygen was down to 89%. And her CO2 was up which means that would show up in her ABG. Right? That goes without saying.
Richard: Thank you.
Heather: Yeah.
Patrik: Yeah. So how do we know the ventilation is sorted enough to reduce sedation? How can we work that out?
Patrik: Yeah, yeah. What you need to do now is … If what he says is that goal, they should sedate her and give her more volume and then her CO2 should come down. Right?
Richard: Right, okay.
Patrik: That would be one goal.
And the other thing is, excuse me, it should then show up in the numbers on the screen. And it should show up in her blood gases.
Richard: Right, okay. If we sent you an image tomorrow?
Patrik: Yeah.
Richard: Then that would actually be able to show you the change her ventilation. Thank you.
Patrik: Very much so. And also you would see whether they’ve lowered her sedation or not.
Patrik: Pardon?
Richard: Sorry. If she stays on four and four over the next 24 hours … then I don’t know, you can’t see the patients, you can only see the monitors and everything. My simple thing is will she last 24 hours? Obviously, if she doesn’t, then all this, 24 hours’ time. She’s gone. She’s left.
Is there anything that I can look out for? Obviously if they ring and say in the morning to say that she’s got more sever in her condition, hanging onto a piece of string and that she could die at any time.
But do you think, somebody said that if they keep on ventilating her and they don’t change it, I’m thinking if they don’t increase the station and her condition doesn’t get significantly worse. Then she just stays in limbo, but she may then still be alive tomorrow. But which many be enough to invalidate that …
Find information about tracheostomy weaning:
Patrik: Very much so.
Richard: Is that exactly right?
Patrik: That’s exactly right.
Richard: I’m happy to wait. I’m happy to wait until it happens. That’s fine.
Patrik: Yeah.
Richard: Because If, I’m only speculating here, which obviously on a very bad day, if you get to that point when the figures are all the same which in a sense shows that what he’s saying doesn’t make sense. How do I then change that? Because I can then say of course ‘things need to change.’
But not being a technical person, I might need your support again and the doctors are here or whoever.
Heather: Our e-mail. You have then writing what you want.
Richard: Yeah, exactly.
Patrik: I think going via e-mail with the doctors may not be a bad thing because what’s documented is always better than-
Heather: -Agreed. That was more accepted.
Richard: -lots of issues and conversations that could be manipulated.
Heather: Yeah.
Richard: Okay, thank you.
Recommended:
Patrik: You’ve made some good starts there already by taking notes in the meetings. And I think you should be doing that.
I do believe … look I’ll tell you what that I also believe. I do believe these doctors are here … I think over all he seems to be a decent guy. However, what I do believe is he’s probably under pressure from everybody else.
Would you think that?
Heather: Yeah.
Patrik: Right, right.
Richard: That’s possible, possible.
Patrik: So to a degree he’s a scapegoat for probably for Dr. Miller?
Richard: Yeah, yeah.
Heather: His job would be set if he had hired anaesthesiology.
Patrik: Right, right.
Richard: Did you hear?
Patrik: Yeah.
Richard: That’s a good start. So I think today we’re just going to spend time at my mum. And do what we can. I think there may be that’s the way things work.
Heather: Which is why I’m just going to turn off now.
Richard: Yeah.
Heather: I know the answer right here.
Richard: Yeah, okay. Fine. So that’s great, Patrik.
Heather: Thank you!
Richard: Thank you so very much. Does anybody else want to add or discuss? I know it’s getting very late for you. Sorry. Yeah.
Patrik: I think really we can give them the benefit of the doubt for 24 hours, but then you’ve got to watch their actions and not their words. Which you’ve been doing all the way along anyway.
Richard: Yeah, right. Great. Thank you.
Patrik: And that would be my advice. Just wait and see what happens.
Richard: Okay, good.
Heather: Alright.
Richard: Thank you very much indeed.
Patrik: You’re very welcome. You’re very welcome.
Richard: It means a lot what you’ve done today. And can’t thank you enough.
Should I regroup tonight and send you a text?
Patrik: Yeah, yeah, yeah.
Richard: Fingers crossed. We’ll just see what happens. And the feeling for tomorrow. If that’s okay with you. Is that possible?
Patrik: Absolutely. It’ll be easier for me, well not easier, just I will have more time … I’ve made time now of course. But it will be easier for me over Easter weekend anyway because it’s quieter with usually. But whatever you decide is fine. We’ll take it from there.
Heather: And thank you!
Patrik: You’re very welcome. I’ve had, you’re not my first client from Ireland. And I can tell you, I’ve worked with so many wonderful Irish nurses over the years. Always been very pleasant. Always been very pleasant.
Heather: Okay.
Richard: Thank you.
Heather: Bye!
Patrik: Thank you.
Richard: Really appreciate this.
Patrik: You’re very welcome. All the best. All the best for now. Your welcome. Bye-bye.
Richard: Bye-bye now.
Patrik: Bye.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!