Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode was
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to continue answering the next questions regarding James’ and Christine’s Dad in ICU who’s had a haemorrhagic stroke.
James’ and Christine’s Dad had a brain decompression where they evacuated a large bleed from his brain after the haemorrhagic stroke. And their Dad also underwent a craniectomy (removal of skull) to decrease the brain pressures after the bleed.
James’ and his sister Christine were getting their Dad in one of the best hospitals in the USA, the Cleveland clinic in Ohio.
In the meantime, their Dad was getting a tracheostomy because he couldn’t be weaned off the ventilator and the breathing tube. He also had a PEG tube for feeding inserted.
He also had ongoing seizures due to the stroke and his anti-seizure medications needed to be optimized so he could “wake up” and progress to Neurology Rehabilitation.
In today’s episode of “YOUR QUESTIONS ANSWERED”, I answer a series of questions from James again about the day to day challenges his Dad is facing whilst being in Intensive Care. James also wants his Dad to stay in ICU and not go to LTAC (Long-term acute care).
We therefore also discuss strategies around staying in ICU for as long as is needed.
Today’s consulting and advocacy session is another excerpt from various 1:1 phone/email consulting and advocacy session with me and the topic this week as part of this series of 1:1 consulting and advocacy session with me and the topic this week is
How to get best care and treatment when your loved one has seizures and is ventilated with tracheostomy!
You can also check out previous episodes of the 1:1 consulting and advocacy questions with James and Christine here
James writes
Hi Patrik,
My Dad’s Glucose is 149 when standard range is 74-99, please advice.
James
Hi James,
Many Patients in ICU suffer from high blood sugars during their stay in ICU.
This is a stress response from the body because of the critical illness.
Stress releases cortisol and cortisol increases the blood sugar.
Furthermore, your Dad might have been or might still be in steroids for the head injury to bring the swelling down in the brain and steroids will increase the blood sugar as well.
Most Patients who are non-diabetic and have raised blood sugars during their ICU stay have their sugars back to normal by the time they leave ICU.
The important bit is to know that it can happen for non-diabetics and that it simply needs to be managed.
Hope that helps.
Give me a call anytime.
Kind Regards
Patrik
Hi Patrik,
My father seems to be very sedated again today from the Vimpat ??
The ICU said this would be less sedating than than the Dilantin (Phenytoine).
Now they are trying to wean him off of it and just leave him on Keppra.
The epilepsy team is doing this.
Please advice.
Thanks
James
Hi James,
How much Keppra, Dilantin and Vimpat is he or was he on?
Do you have dosages (usually in gram or milligram)
Also, when was the last CT/MRI scan of the brain?
Do you have a score for the Glasgow coma scale?
Also, you told me that you never get a straight answer to your questions and I’m not surprised about that.
They will be feeling pretty threatened by the amount of knowledge you have already gained in recent days.
Don’t let that stop you and keep asking. Knowledge is power only if you use it.
Take one day at the time and keep focusing on the positives and also expect some setbacks!
Also, make sure you look after yourself first and foremost as I can hear you’re getting pretty tired. You are the most important person in all of this. Make sure you stay healthy, rested and sane!
Your father will need the best version of you!
Kind Regards
Patrik
Hi Patrik,
My father had five clinical seizures last night. The ICU does not seem capable of controlling his seizures. I am concerned.
Also, my father had the Tracheostomy and PEG done today and is doing well. Still trying to control seizures, Dilantin was added back yesterday.
Hope you are well,
James
Hi James,
One of the challenges your Dad is facing with the ongoing seizures is that they are trying to control them with Keppra, Dilantin (Phenytoine) and Vimpat.
This usually works once all of those medications are optimized and well balanced.
The team of doctors and nurses hasn’t achieved that yet.
One of the biggest challenges when managing acute seizure activity is to not keep your Dad too sedated, especially since he now has a tracheostomy.
One of the goals of a tracheostomy is to wean off the ventilator as quickly as possible.
You may remember that when your Dad was still having the breathing tube/endotracheal tube he needed to be sedated so he was able to tolerate ventilation with the breathing tube.
To a degree that also prevented seizures because he was sedated with Fentanyl and Midazolam (Versed). Midazolam (Versed) is a Benzodiazepine which is a drug preventing seizures but it’s also a strong sedative, designed to keep Patients in Intensive Care in an induced coma.
Now that your Dad is having a tracheostomy he won’t need the Midazolam (Versed) and the Fentanyl any longer because a tracheostomy is so much more comfortable and easier to tolerate.
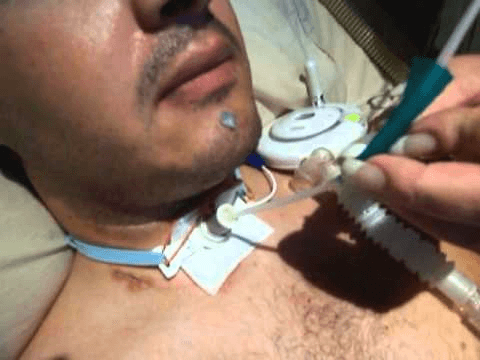
Therefore your Dad is more awake and therefore also more prone to seizures.
The next thing they need to work out is to find the right does of Dilantin (Phenytoine), Keppra (Levetiracetam) and Vimpat to keep your Dad seizure free if possible at all.
They will hopefully be able to work that out over the next few days. Ask them about their plans.
Now it’s also time to ask for
- ventilator settings (picture ideally)
- Chest x-ray result
If you could send me some of that information it would be great so we can determine how quickly your Dad can be weaned off the ventilator.
Kind Regards
Patrik
Recommended:
Hi Patrik,
my father is doing pretty well all things being considered. His eyes are opening and has GCS is 11.
He seems very weak but hopefully aware of his surroundings. He goes for the tracheostomy a lot.
They are going to stop his vimpat tomorrow in preparation for moving him to LTAC (Long term acute care).
He will need help weaning off the ventilator.
I would like for him to stay in the ICU as long as possible. And wanted to discuss the ways of stalling.
I know you can’t stay there forever but another week would be ideal. I feel he is getting very good attention and is making good progress and I don’t want anything to interfere with that.
Thanks
James
Recommended:
Hi James,
That’s pretty good for now James.
GCS 11 is the maximum anyone with a tracheostomy can score. From that perspective he’s doing pretty good and reducing Vimpat might have been the right thing to do as long as he stays seizure free.
As discussed in our last phone call, LTAC I believe would be a disaster because his level of care would drop significantly, he would lose the skill, expertise and professionalism that Intensive Care professionals bring to the table.
No such thing exists in LTAC and the needs for your Dad as long as he stays on the ventilator and tracheostomy are that he needs ICU nursing staff and an ICU doctor.
LTAC’s are designed to empty ICU beds quickly without looking at clinical needs. ICU’s are so busy and they need their beds which is one of the reasons ICU’s want to do a tracheostomy at the first sign that weaning off the ventilator and the breathing tube takes longer than their financial budget allows.
Related article/video:
That’s an absolute tragedy and money or perceived funding should never dictate clinical care.
Clinical pictures, diagnosis and prognosis is what needs to determine clinical care and treatment.
Think about it, in LTAC there are no ICU nurses, often there are nursing aides looking after your Dad who just spent 4 weeks in ICU at the brink of death.
Furthermore, LTAC stands for long-term acute care.
Now James, this implies LONG- TERM.
What a nightmare for somebody on a ventilator and tracheostomy. Nobody should be long-term ventilator and tracheostomy dependent.
Recommended:
The only reason a Patient ventilator and tracheostomy dependent should leave ICU is to go home with a service like INTENSIVE CARE AT HOME. Then your Dad would still be looked after by ICU nurses.
Again, LTAC’s are designed to save money, reduce the level of expertise and keep ventilating Patients long-term. LTAC’s don’t have the same level of skills and expertise compared to ICU or to INTENSIVE CARE AT HOME.
The longer LTAC’s can keep their Patients the more money they are making. Why isn’t LTAC named STAC like short term acute care???
That would put the pressure on to try to wean Patients off ventilation and tracheostomy.
Now in ICU the pressure is on and they can usually also handle it with the expertise and skill the doctors and the nurses have, including the respiratory therapists.
The goal need to be for your Dad to stay in ICU and as I mentioned keep pushing them to keep your Dad there by asking them all the questions we discussed on our call.
Recommended:
Just keep focusing on things like
- Continuity of care
- Skill level in ICU compared to LTAC
- Keep mentioning that you just don’t feel comfortable with the LTAC they have offered you.
I can’t tell you how many families call us at INTENSIVECAREHOTLINE.COM who want to get their loved ones out of LTAC.
I think what we’ll do next is to get on the phone to the head doctor of the ICU and talk to him.
Set up a meeting and I will make myself available.
Kind Regards
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!




