Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode was
You can check out last weeks question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to continue answering the next questions regarding James’ and Christine’s Dad in ICU who’s had a haemorrhagic stroke.
James’ and Christine’s Dad had a brain decompression where they evacuated a large bleed from his brain after the haemorrhagic stroke. And their Dad also underwent a craniectomy (partial removal of skull) to decrease the brain pressures after the bleed.
James’ and his sister Christine were getting their Dad in one of the best hospitals in the USA, the Cleveland clinic in Ohio.
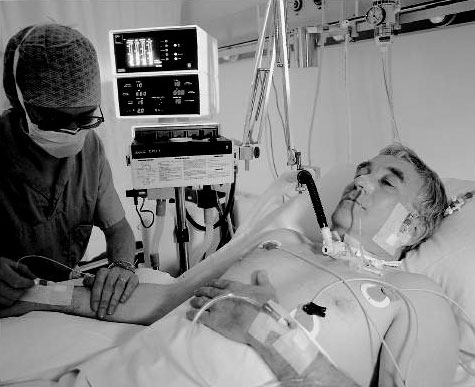
In the meantime, their Dad was getting a tracheostomy because he couldn’t be weaned off the ventilator and the breathing tube. He also had a PEG tube for feeding inserted.
He also had ongoing seizures due to the stroke and his anti-seizure medications needed to be optimized so he could “wake up” and progress to Neurology Rehabilitation.
In today’s 1:1 consulting and advocacy sessions with James and his sister Christine, we look at some setbacks their Dad is going through.
He had to be put back on the ventilator due to a Pneumonia and he also ended up with a central line (CVC) and arterial line again.
In the meantime he has come off the ventilator but still has the tracheostomy after over 5 weeks in ICU.
This series of 1:1 consulting and advocacy is a real testimony for getting advice, run with it and get results.
If you want to avoid LTAC and a nursing home for your loved one, you need to read all of the consulting and advocacy sessions with James and Christine!
So in today’s episode of “YOUR QUESTIONS ANSWERED”, I answer a series of questions from James and his sister Christine again that are excerpts from various 1:1 phone/email consulting and advocacy session with me and the topic this week as part of this series of 1:1 consulting and advocacy session with me and the topic this week is
Dad’s off the ventilator after 5 weeks in ICU, now they try and drug him up to avoid seizures, what should we do?
You can also read or watch previous episodes of 1:1 consulting and advocacy with James and his sister Christine here
James: Should Dad have his Cranioplasty done ASAP, what do you think?
Patrik: Sorry. So with the cranioplasty I don’t know what to advise because that is outside of my area of expertise.
Christine: Okay.
James: Patrik, what I was asking when I had lost you was they were talking about downsizing the tracheostomy because he is breathing so well.
Patrik: Yep. Good idea.
James: What was that all about?
Patrik: Good idea. I’ve taken … Do you know what size he’s got? Size 8, at the moment?
James: I don’t know.
Patrik: Right, that’s okay, but if they can then-
James: Whatever … Probably whatever the largest size is.
Patrik: Right. If they can downsize, absolutely, great idea. Great idea. The more … If they can get rid of the tracheostomy, great, that’s one less thing to worry about.
James: So, it’s not a matter of just taking the tracheostomy out, then? Do they do it gradually and downsize it?
Patrik: So some patients they can just take it out. In your dad’s case, I would imagine they have to … Have they assessed his swallowing?
James: No, we’ve been waiting for them to do that.
Patrik: Right, okay, well I do believe that should happen simultaneously. They should assess the swallowing simultaneously. But if they can downsize, that’s definitely a good sign. If he’s breathing well, fantastic. Is he still on oxygen?
James: Christine, are you there?
Christine: What do you mean-
James: On the tracheostomy collar?
Christine: No, I don’t think he’s on it. You mean like the ventilator?
Patrik: No, no.
James: No, that hose that they put up to his throat.
Christine: You mean … Oh, I didn’t know that was oxygen. They just said it was like a little humidifier that goes over the trach.
Patrik: Yeah, and this … Yeah.
Christine: Is that oxygen that goes through it?
Patrik: Yes, well, that’s the question. It could just be the humidifier, but they might have added in some oxygen too. If it’s just the humidifier-
Christine: No, when I see an oxygen …
Patrik: No, you wouldn’t.
Christine: When I see like the-
Patrik: No because when it would come out of-
Christine: Oh, I thought that was always the humidity. Okay.
Patrik: Right. He might have to-
Christine: I got to say, I don’t think he is on oxygen.
Patrik: Okay.
Christine: No I don’t think he is.
Patrik: Yeah, good, good.
Christine: Because we’ve taken that off because it’s loud and they just told me it’s humidity water and it’s really not that important.
James: It’s oxygen too.
Christine: You think it is?
James: Yeah, they told me it was.
Christine: Oh, okay.
James: Right, right.
Christine: I didn’t know that.
James: Right.
Patrik: Just ask them if you can. I mean a little bit of … It’s not, you know, if they can wean down the tracheostomy size, if they can put in a smaller tracheostomy, that’s great. You know, the sooner they can get rid of the tracheostomy, the better. No doubt about that.
Christine: Yeah. Yeah.
Patrik: Yeah, I mean … As I said, I can’t, you know, I’d say maybe bring him home closer to your family a while might help and if you think you have a doctor there that is cooperating with what you want, that might be helpful too.
Christine: Well, yeah, I don’t know. You know? It’s crazy because it’s all insurance driven. What are the things that would make my dad stronger now? Downsizing the size of the tracheostomy?
Patrik: Yep.
Recommended:
Christine: Getting his phone back on maybe? They don’t really seem to want to bring his seizure medicine down. I don’t think they really want to keep us here much longer and bringing the seizure medicine down, it’s a careful thing, you know?
Patrik: It is, it is.
Christine: You know. So I don’t know.
Patrik: What would make him stronger? Definitely waking up more, and also when I was asking James earlier whether they tried to stand him up or not. Have they-
Recommended:
Christine: Yeah, they don’t try to stand him up.
Patrik: Yeah. And that, I believe, needs to happen too. I don’t know whether that’s achievable, but you know, at least they need to try and report back to you, and say, “Okay, we tried, it’s either working or it’s not working.” You know?
Christine: How could he stand up when he’s on all this medicine. You know?
Patrik: Yeah, that’s what I’m, you know, that’s what I’m trying to-
Christine: Oh.
Patrik: You think it’s not possible at all. Is that what you’re saying?
Christine: Yesterday he was out of it, today he’s a little bit more alert.
Patrik: Mm-hmm (affirmative).
James: How did they do today, Christine, when they took him outside?
Christine: Oh, this is the other thing Patrik. They give him the two medicines together, the two seizure medicines together. The Keppra, and there’s a new one. The seizure doctor that … I mean, it’s like a double whammy in the morning.
James: Yeah.
Christine: In the morning. They’re giving him, when I look at the list of medicines. What’s that new one James? Zonegran?
James: Is is the Zon-
Christine: They’re giving him the Zonegran … Zoni …
Patrik: Yeah. Zonisamide. Yeah.
Christine: And the Keppra together. Yeah.
Patrik: And then he falls into a hole. Is that what you’re saying?
Christine: Well, they gave him Keppra 1500 in the morning, and a hundred milligrams of the Zonisamide.
Patrik: Yeah. And that knocks him out.
Christine: So do you think that … Yeah. And then how does he function all day when he takes that first thing in the morning?
Patrik: You see the-
Christine: And then they give it together at night.
Patrik: Yeah, yeah. Nighttime, it-
Christine: So.
Patrik: Yeah. You see, it almost sounds like, especially since they drug him up, you know, it almost sounds like that’s the recipe to get him ready for nursing home. Because there would be a lot of drugged up people in nursing home.
Christine: Yeah. I like them. I don’t think they’re bad. But I don’t like the direction where things went this week. It was very strange. You know? We had, you know, drug him up, you know, psychiatrist come in, let’s put him in a nursing home.
Patrik: Yeah.
RECOMMENDED:
James: Why were they giving him a psychiatric evaluation?
Patrik: That’s a good question. Why are they … Probably-
James: I guess last Monday they, I guess last Monday the nurse came in and said are you ready for your shot today, and he said no.
Christine: Yeah, you know, the thing with Patrik, I told you this. Everything’s been perfect here. This one nurse came on Monday and Tuesday. My brother left town. It was very strange. And then I went to get some soup. I came back. His wife’s in the room with her sister. And all of a sudden, they said, “Your dad refused his medicine. Psychiatry’s coming up.” And I said, “What? Nobody ever gave him a choice on the medicine. Why would he be given a choice all of a sudden after five weeks of being here?” And she’s like, “Well, I just had to ask him, and he said no. And now we have to put it through psychiatry that he’s not cognitive so his wife can make all the decisions.”
Patrik: Right.
Christine: And I was like, okay. And then I went in the room and I said, “Dad, you gotta take your medicine.” You know, right then and there, this late, they were trying to go the nursing home path, or whoever was. And so then he said, “Okay, I will.” And the doctor went in before psychiatry came and said, “Will you take the medicine?” And he said yes. But they still had to bring the psychiatrist in, and it was somebody very inexperienced, a young resident.
Patrik: Right.
Christine: To mark that down. I mean, he’s not 100%. We know that’s what he was doing-
Patrik: No.
Christine: … Quite well. It’s the weekend.
Patrik: Yeah, how can they-
Christine: But now, it’s marked in his record.
Patrik: Yeah, yeah. How can they make a psychiatric assessment if he can’t talk? I mean, by all means. You know? I mean, that’s-
Christine: Right, but they-
Patrik: How can they-
Christine: … that was why, you make a good point. Yeah.
Patrik: How can they make-
Christine: He couldn’t talk.
Patrik: That’s exactly right. How can they make a psychiatric assessment. Do you remember, we were talking about earlier, Glasgow Coma Scale. We were talking about this a couple of weeks back. You know, he’s got the Glasgow coma scale and it is still not 15. I’m bound to say it’s almost irresponsible to do a psychiatric assessment if a patient is not Glasgow Coma Scale 15. Right?
Christine: What is that Glasgow Coma Scale?
Patrik: Yeah, so you and I talking now, we are Glasgow Coma Scale 15. Right? We are 100% alert, we can talk. Right? Your dad’s Glasgow Coma Scale would be probably an 11 still, because he can’t talk yet. So, you know, making a psychiatric assessment on somebody who can respond to questions makes sense. But making a psychiatric assessment on somebody who is not cognizant 100%, that’s like … That doesn’t make sense to me. It wouldn’t be accurate.
Christine: Well, the psychiatric assessment was was he cognitive or not.
Patrik: Okay, so they were basically asking a simple question.
Christine: So, and they deemed him not cognitive.
Patrik: Okay.
Christine: They wanted to deem him as not cognitive so someone could say he had to take his medicine and override when he said no, which is a safety thing and probably what they needed to do.
Patrik: Okay.
Christine: But because he flat out refused it, hospital protocol is to bring a psychiatrist in to say, “No, he’s not cognitive.” And the doctors need to override it and say he needs his medicine, or his wife.
Patrik: I see. I see. Okay. So it wasn’t the full-
Christine: I mean, I wasn’t really comfortable … Yeah, no. It wasn’t the full psychiatric …
Patrik: Assessment. Okay. Okay.
Recommended:
Christine: And what is that full psychiatric thing? Isn’t there a determining thing about someone’s cognitivity? There’s a scale, right?
Patrik: There would be a scale.
Christine: I forgot.
Patrik: I mean, we’re talking about the Glasgow Coma Scale to begin with. But the psychiatric assessment, again, that does happen in intensive care or in a step down, but it doesn’t happen all too often. Because patients are not … You know, I go back to the Glasgow Coma Scale 15. It would be very difficult to make that decision if people are not cognitive. If they’re not 100% cognitive.
Christine: Right.
Patrik: So I think, it sounds to me like it was a simple psychiatric assessment, just basically figuring out is he cognitive or not?
Christine: Do you know what the PRI is? Personal Review Instrument? Or the ADL? Is this thing-
Patrik: Oh, ADL would be Activities of Daily Living.
Christine: Okay.
Patrik: Right. That would be a-
Christine: PRI?
Patrik: PRI, I have not heard of. But ADL would be Activities of Daily Living. So they would be assessing how functional is your dad. So, you know, can he get out of bed himself? Can he eat? Can he drink? Can he walk? Can he talk? All of that. Can he get himself to a shower? That is an important assessment to make. And it would determine what level of care he would need going forward, and it would determine, you know, any support going forward. For sure.
Christine: In your opinion, with what we’re at. If they really make us leave here, and they really are strong about us not doing rehab here, if we have three choices … And I know, you know. If we have three choices, either an LTAC in Cleveland, or a skilled nursing home in Buffalo, or the hospital, the hospital transfer with a doctor that we know and knew my father before all this who’s a neurologist. What do you think would be the best situation? And that transfer to the hospital, they’ll give him the bedside rehab and do all that there.
James: He’s not a neurologist. He’s a neurosurgeon.
Christine: Oh. I’m sorry. Neurosurgeon.
Patrik: Right. Look, I would definitely stay away from the skilled nursing home. I would, at this stage, still tend to the hospital-to-hospital transfer. You know, I think … I don’t know who the ultimate decision maker will be for the neuro-rehab. I don’t know whether that’s a team decision, whether, you know, that’s just the neurology, so the neurosurgeon. I don’t know who the ultimate decision maker is. I would think it’s sort of a combination of decision makers. But you’ve probably got to work out who is that decision maker? But I would definitely stay away from a skilled nursing home. That’s worse than an LTAC.
Christine: Yeah. So. Right. So I wonder, also, if we do the hospital-to-hospital transfer, not to over-analyze it, but if it will be hard to get the referral to Rochester. From Buffalo to Rochester. Is it just a matter of a doctor writing a referral? Are they going to kick back and say, “Well, you’re in Buffalo. There’s … ” I don’t really think there is a neuro-rehab there, so we could say we need neuro-rehab. It’s probably not going to be a problem with insurance. I’m wondering if we’ll have a better chance of insurance covering neuro-rehab in Chicago with a referral from Cleveland Clinic, or-
Patrik: Oh, I see.
Christine: … a referral from Buffalo.
Patrik: Yeah, yeah, yeah. Well, I mean. I don’t know. I don’t know what, you know, what the best … It’s usually, you know, if you have an intermediate step, yes it could weaken, sort of, the proposal of going to rehab. If you say, “Hey, we’re going to neuro-rehab next week.” You know, it sort of takes one step out, and it also takes cost out for the insurance. So yes, you may have a point there.
Christine: Right.
Patrik: You may have a point there. I-
Christine: We’re going to have to as the doctor in Buffalo.
Patrik: I think so. I think so.
Christine: Yeah.
Patrik: And I think, you also gotta ask the doctor, probably even in Cleveland now, if he wants to go on to neuro-rehab, you know, should there be an intermediate step? Should we got there straight away? I think the more clear you can be in your questions, as well as in your expectations, the more clear you can be, hopefully the answers will come.
Christine: Right. Well, they told me in Chicago that they really wanted him off the vent for a few weeks. I mean, he’s only been off the ventilator for like a week.
Patrik: Yeah.
Christine: I mean, how could we got to Rochester next week? That’s only really two weeks off the ventilator, you know? And then start doing some heavy rehab. I don’t know. So. I’ll have to see.
Watch out for the next episode of “YOUR QUESTIONS ANSWERED” where we continue with Christine and James!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!



