Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode was
How to wean off ventilation and tracheostomy step by step!
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to continue answering the next questions regarding James’ and Christine’s Dad in ICU who’s had a haemorrhagic stroke.
James’ and Christine’s Dad had a brain decompression where they evacuated a large bleed from his brain after the haemorrhagic stroke. And their Dad also underwent a craniectomy (removal of skull) to decrease the brain pressures after the bleed.
James’ and his sister Christine were getting their Dad in one of the best hospitals in the USA, the Cleveland clinic in Ohio.
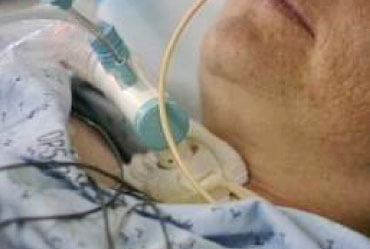
In the meantime, their Dad was getting a tracheostomy because he couldn’t be weaned off the ventilator and the breathing tube. He also had a PEG tube for feeding inserted.
He also had ongoing seizures due to the stroke and his anti-seizure medications needed to be optimized so he could “wake up” and progress to Neurology Rehabilitation.
Since last week’s 1:1 consulting and advocacy session, James’ and Christine’s Dad has been off the ventilator and has been moved from Intensive Care to a step down unit. Their Dad still has the tracheostomy in place but is off ventilation and breathing by himself.
He’s still having occasional seizures and the doctors and nurses are still trying to optimize the seizure medications.
In today’s episode of “YOUR QUESTIONS ANSWERED”, I answer a series of questions from James and his sister Christine again that are excerpts from various 1:1 phone/email consulting and advocacy session with me and the topic this week as part of this series of 1:1 consulting and advocacy session with me and the topic this week is
How to get into Neurology rehabilitation from ICU after a stroke and avoid a nursing home!
You can also read or watch previous episodes of 1:1 consulting and advocacy with James and his sister Christine here
James: Hey Patrik.
Patrik: Hi John. How are you?
James: Good. How are you?
Patrik: Very good thank you. I’ve just seen your email. Besides what you’re saying in your email, how is your dad in general? Besides having had the seizure three days ago, how is he in general? Is he more awake? Tell me a bit more how he’s doing generally.
James: You know, I haven’t been there all week.
Patrik: Oh, I see.
James: But from what I understand, he isn’t as responsive as he was. I hear different things. I don’t know for sure. You’d have to ask my sister.
Patrik: Okay. Yup.
James: You can email us back with something.
Patrik: Yeah for sure!
James: I’d always like to have it in the email. But I think he’s doing okay. I think he was a little tired for a day or two, but I think he’s alright now.
Patrik: Okay. Okay. No, no. I was thinking of emailing you back, but it’s not quite clear from the email to me, how he’s doing, generally speaking. Is he still progressing? Is he the same? You know, all of that.
James: Yeah, I wouldn’t say that he’s made any big leaps and bounds or anything like that. You know, but he’s okay. He’s doing about the same as he was before.
Patrik: Right. Do you feel like, do you and your sister feel like they’re gonna push him out? Is that your feeling?
James: A little bit, but we did talk to everybody after I sent you that email. We talked to the neuro surgery, we talked to the caseworker, we talked to epilepsy, and they didn’t sound like they were really in a hurry to make him leave. But, you know-
Patrik: Okay.
James: They said that eventually that the hospital environment is becoming counterproductive for him and you’ve gotta get moving. And I do happen to agree with that.
Patrik: Yeah. I agree with that too that the hospital environment at some point is counterproductive. I’m just, my biggest concern is why would he go to LTAC (long-term acute care) if he’s off the ventilator? Unless they’re offering something there that I’m not aware of.
James: No, they changed their mind after I sent that email to you. So now, they’re no longer recommending the LTAC. Now they’re recommending a nursing home.
Patrik: That’s worse. I mean-
James: Yeah. I know.
Patrik: That’s worse.
James: I know, I know. And I’m glad that we’re on the same page because it’s very frustrating because they say things that insult your intelligence and then they expect you to just … I mean they say things that would really insult anybody’s intelligence, but I mean I can’t imagine that everyone walking through there is gonna say, “Okay, yeah. We’ll do whatever you say.” I mean it’s just common sense you know? Going to a nursing homes not a good thing, but we’re in a jam here because I don’t really know where to bring him.
Patrik: Yup.
James: And it’s like a chicken and the egg thing because if he gets to the right, if I bring him to the right neuro rehab facility now, they might be able to get his cognition back. He’s not talking yet.
Patrik: Mm-hmm (affirmative).
James: But if I bring him to a nursing home, he may just degenerate.
Patrik: I mean a nursing home is just shocking. Absolutely shocking. So we’ve seen neural rehab, so basically what they’re saying is that he needs to be stronger to go there? Is that sort of what they’re saying? Or not quite.
James: Well they’re basically saying that he’s not, we were going in the direction where the physical therapy, if you read the email again, the Physical Therapist says that he was ready to do three hours of rehab.
Patrik: Yes.
James: And then the Psychiatrist, I don’t think even evaluated him, just looked over his records. I think she tried, she went in and tried to have a conversation with him and he wasn’t really responsive to her. So he wasn’t responding to some commands so she said he’s not ready for three hours of rehab.
Patrik: Right. Well-
James: And then she, yesterday said LTAC (long-term acute care), and then today she said nursing home.
Patrik: And that’s just one person’s opinion though.
RECOMMENDED:
James: Exactly. Right. So then Neurosurgery said, “Well we’ll try to get someone else in here to evaluate him.”
Patrik: Yes.
James: So I said, “How could we have such a difference in opinion from a Physical Therapist that actually works with him for an hour, versus somebody just evaluating him for five minutes?” You know? You have a disconnect there.
Patrik: Absolutely. Absolutely. Look, there’s a number of things. Number one you would be surprised how many people just go with whatever’s been suggested. You would be surprised. You know? How many people don’t do any research or don’t question. So I think they don’t like being questioned. We know all of that. But that’s besides the point.
So it’s good that, I still do believe, it’s good that the LTAC is off the table. It’s not good that they’re talking about nursing homes. I still do believe that the neurology rehab is the right way forward because we’re still talking about single organ failure. You know? His heart is fine, his lungs are fine, his kidneys are fine, his liver is fine. You know? The only organ that’s partly failing is the brain. Right? So from that perspective, the only way forward to deal with that single organ is a neurology rehab. Have you or your sister spoken with the, you’ve spoken to Neurosurgery, have you spoken to a Neurology as well?
James: Yeah, well they’re neuro ICU doctor says that he’s a neurologist and he’s a epilepsy doctor, and he’s an ICU doctor.
Patrik: Okay.
James: So I’ve never actually spoken to an actual Neurologist, Neurologist.
Patrik: Might be worthwhile to see whether you can hunt down just a Neurologist in there. You know? Just to get his view. Yes, Neurosurgery, they would be supportive of neurology rehab, but it would also be good to talk to a Neurologist. If you’re saying you don’t feel like they want to send him out quickly, it might buy you a little bit of time. Do you know whether it’s an insurance issue as well?
James: Yeah, I think that’s part of the problem. There’s always insurance involved. And yes, that’s definitely part of the problem. Which I don’t think they’re gonna come out and say that.
Patrik: No, no, no. Of course not. Have you or your sister spoken to the insurance?
James: Not directly, no.
Patrik: Okay. Okay. But you’re not there at the moment obviously?
James: No. You know what, I got a little sick so I came home.
Patrik: Yeah.
Recommended:
James: I’ve been sitting in there in that ICU forever and I picked up some stomach bug or something.
Patrik: Yeah, absolutely. I mean that, ICUs just a terrible environment.
James: Yeah.
Patrik: Okay. Is your sister there at the moment?
James: No, she just left as a matter of fact, to come home. But his wife is still there.
Patrik: Mm-hmm (affirmative). Mm-hmm (affirmative). Okay, the other thing with, you’re talking about the Cranioplasty . Look, I, look to be honest with you I have no opinion on that. And the reason I have no opinion on that is simply, when patients leave ICU, they don’t come back for the Cranioplasty . They have the Cranioplasty at some point, but it usually doesn’t require ICU. Okay? So therefore I couldn’t tell you when patients have the Cranioplasty. I don’t know whether that’s six months down the track, whether it’s two weeks down the track, I really have no idea.
James: Uh-huh.
Patrik: Right? So I couldn’t guide you with a Cranioplasty because I simply don’t know what they’re doing once patients leave ICU.
James: Okay.
Patrik: So that is outside of my expertise. So, yeah, I think talking to Neurology might help. And see whether you can still try and move it to a acute rehab if you can. Do you know if there’s an acute rehab in the area?
James: There is, yeah.
Patrik: Right.
James: So the thing with the Cleveland Clinic, I mean they’re the second best hospital in the United States.
Patrik: Yes.
James: And they don’t have a neurological rehab.
Patrik: Right.
James: They have a general rehab.
Patrik: Mm-hmm (affirmative).
James: So I think part of the reason why they’re trying to get us out is because they don’t think that their rehab is really that good.
Patrik: Mm-hmm (affirmative).
James: Or it might not be the right place for him. But they did say that there was a place in the same city there, in Cleveland, that’s supposed to be pretty good for neurology rehab. But it’s like a State hospital. You know? Like a public hospital.
Patrik: Yeah, yeah, yeah, yeah, yeah. Mm-hmm (affirmative). Have you made any inquiries about their level of quality? You know? Do you know anything about it?
James: No, I don’t. But if you Google the top five neurology rehab centres in the United States, Chicago is the first one.
Patrik: Okay.
Recommended:
James: That’s supposed to be the best one. It’s sort of like an entire skyscraper full of neurology rehabilitation.
Patrik: Okay. Would you consider going to Chicago if you feel like that’s the right thing? Would you consider that?
James: Yeah, absolutely. But the problem again is insurance. So Chicago’s only gonna do what the doctor says he can do at the Cleveland Clinic.
Patrik: Right. Yeah, yeah, yeah.
James: So he doesn’t really have more than, it doesn’t sound like he has more than two weeks, maybe three weeks tops in Chicago. And then they have to move, as an inpatient rehab, and then they have to move you as an outpatient.
Patrik: Mm-hmm (affirmative). Yeah, yeah, yeah.
James: And then you have to go, basically get a hotel room or something. And he’s not well enough for that yet.
Patrik: No, no, no. It doesn’t sound like it. Tricky.
James: I don’t really know where to bring him.
Patrik: Yup.
James: You know, I could bring him home for a while, he has some friends that are doctors that will take him into hospitals and do their best to rehabilitate him. But you know, I just, I don’t wanna, again, I don’t know if it’s an issue of time, or if it’s an issue of getting him to the right rehabilitation centre to make him progress.
Patrik: Yeah.
Recommended:
James: Which one is it? What’s the answer? Come back here and buy ourselves some time? Or just to get him right to a good place?
Patrik: Yeah, absolutely. Absolutely. In terms of progress, is your dad for example, he’s getting out of bed every day, that’s a given.
James: I don’t think he was yesterday, but today he did. They brought him up to the rooftop and got him some daylight and some sun.
Patrik: Okay. Do you know whether they tried to stand him up yet? Do you know whether he’s been standing up at all?
James: No. I don’t think so, no.
Patrik: Okay.
James: They added that third seizure medication.
Patrik: Yes.
James: With those seizure medications, it makes him really drowsy for the first couple days and I think he still has to kind of adjust.
Patrik: Yeah. Yeah.
James: They were actually talking about raising the dose. I don’t think the seizure team there is doing that great of a job.
Patrik: Yeah. Look, seizures, anything related to the brain is difficult to control. I still believe the Keppra is a very high dose. But I mean, given that he had another seizure earlier in the week, somethings not working.
James: Well I have a friend who’s a Neurosurgeon and he was saying that it’s pretty uncommon for him to continue to have these seizures seven weeks after the stroke.
Patrik: Right.
James: And he was saying that the Cranioplasty needs to be done. Because he was saying that if you, there’s some term, but basically that skin flap there starts to sink into the head and into the brain, and it causes a neurological deficit.
Patrik: Right. Right.
James: A lot of people start to bounce back faster when they-
Patrik: There you go.
James: When they put their skull back on.
Patrik: There you go, and that’s knowledge I don’t have, because my area of expertise is intensive care. You know? I’m glad you’ve got that because that’s a good guide for you to know that he should have the Cranioplasty sooner than later.
James: Right. But the doctor here said he wasn’t ready for the Cranioplasty cause there’s still some inflammation there.
Patrik: Right. Have they done a recent, or a follow-up, CT or MRI of the brain?
James: No. It’s another problem … Hold on a second Patrik. I just get my sister into the call, she was a little delayed but is just trying to dial in…
Patrik: Great, that’ll great!
In next week’s 1:1 consulting and advocacy session we continue the discussion between James, Christine and myself to get James’ and Christine’s Dad into Neurology rehabilitation and we continue to find proven strategies that work to get their Dad best care and treatment! Look out for the next episode of “YOUR QUESTIONS ANSWERED” and I’ll talk to you then.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!