Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode was
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to continue answering the next questions regarding James’ and Christine’s Dad in ICU who’s had a haemorrhagic stroke.
James’ and Christine’s Dad had a brain decompression where they evacuated a large bleed from his brain after the haemorrhagic stroke.
James’ and his sister Christine were getting their Dad in one of the best hospitals in the USA, the Cleveland clinic in Ohio.
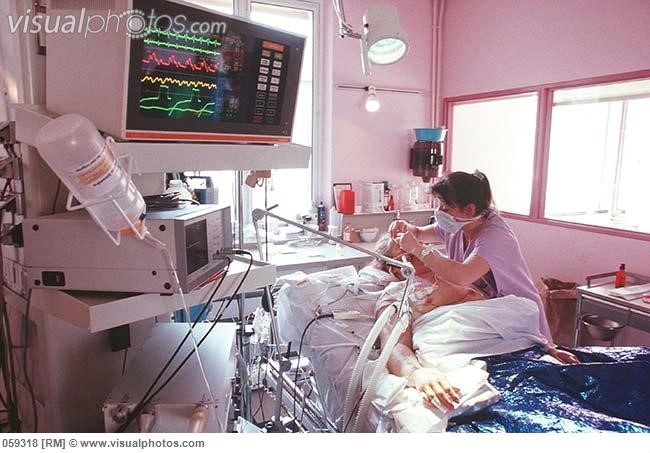
In the meantime, their Dad was getting a tracheostomy because he couldn’t be weaned off the ventilator and the breathing tube.
He also had ongoing seizures due to the stroke and his anti-seizure medications needed to be optimized so he could “wake up” and progress to Neurology Rehabilitation.
In today’s episode of “YOUR QUESTIONS ANSWERED”, I’m talking to James’ sister Christine again who also has questions regarding her Dad’s situation, especially with a view of the Cleveland clinic wanting to move her Dad to an LTAC (long-term acute care) facility.
Christine wants to know what’s the best course of action and I can show her proven strategies how to keep her Dad in a safe Intensive Care environment. You will see in this episode why anybody on a ventilator with tracheostomy should stay in ICU or go home with INTENSIVE CARE AT HOME services, rather than going to LTAC (Long-term acute care) or even worse subacute care.
Today’s consulting and advocacy session is another excerpt from a 1:1 phone and email consulting and advocacy session with me and the topic this week as part of this series of 1:1 consulting and advocacy session with me and my clients James and Christine is
Proven Strategies: How to keep your loved one ventilated with tracheostomy in ICU rather than going to LTAC/subacute care!
Christine: Hello. Hello.
Patrik: Hi Christine, it’s Patrik speaking from intensive care hotline. How are you?
Christine: I’m good. I’m good. Thanks for calling me!
Patrik: Well, I was busy in the last hour, I hope I haven’t woken you up.
Christine: What do you think? Don’t know how this is going to work. I don’t think they’re going to give my Dad an extension to stay in ICU.
Patrik: Have they given you any timelines?
Christine: No not really, as you know I’m very new to this. You know with the LTAC (Long-term acute care facility), we had no idea what it is, but when we first got there last week, we were shocked and then the ICU doctor said if he’s coming off the ventilator in the hospital, he’ll go on to step down in the hospital.
Patrik: Ok
Christine: Time went on and we really didn’t understand all that. And then last week they said to us that, you know, my dad would move to LTAC, the head of the ICU and the Neuro surgeon doctor said this in the beginning! And then they kept repeating all of this again and again, you know, “you have to start thinking about the LTAC for your dad, and eventually a nursing home for him”, which was very upsetting to us.
So we started to look and when I went to the LTAC, I mean they were… I didn’t see a whole lot of active care going on. Now I do feel like it was more like Patients weren’t there to get… I mean I shouldn’t say it, but I didn’t see patients getting better. Like OK, we’ll just put the patient here and hope for the best. So I immediately became very concerned and a couple of days later I went to the ICU doctor and said, I just don’t think my dad is ready yet, LTAC is not a place for him. And so he said, OK, we won’t push you out and we’ll delay it. See where we’re at. The ICU doctors change every four days or so. So now we have a new one and he’s one for seven days. He hasn’t said too much about it and we’re waiting for the neuro surgeon, Dr. king here to come back on Wednesday. But um, we just want to have our story straight as to why we should keep our dad in the ICU and convince the doctor so you know, he doesn’t push us towards an LTAC, again.
Patrik: Do you think the neuro surgeon wants to keep him in ICU?
Christine: I, we don’t know because he has been gone and then he’s been on vacation, he was in a conference and he’ll be back on Wednesday. We don’t know what his thoughts are going to be, you know, he’s going to be the determining factor.
Patrik: Right. Just remind me, which health fund is your Dad with, I’m sure you mentioned Medicare?
Christine: He has Medicare and then his wife says he also has a secondary insurance with blue cross blue shield, which is a PPO (Preferred provider organisation). You asked when you can go wherever you want to go.
Patrik: So, what I’ve learned with other clients. With Medicare patients, the push is often from the insurance to push them out of ICU and unfortunately ICU’s are often supportive of that because they need the beds. I’m, you know, I’m still very supportive of your dad getting weaned off the ventilator in the ICU because I do believe it’s the best place to be weaned off the ventilator!
Related article/video:
Now, they often don’t want to give patients the time because the one and they’ve got the insurance is breathing down their neck, you know, we’re wanting to move them to a cheaper location. And then number two, they often need the ICU bed, so they are willingly sending patients out.
So those are the two sort of pulling forces, if you will, that are working against your dad, but at the same time there’s two things that I’m pleased about. Number one, they haven’t given you any timelines. And number two, um, there is no talk about insurances being in your face at this stage. And also when did they start, when did they start taking him off the ventilator and get him on the tracheostomy collar for the first time?
Christine: That was just today!
Patrik: That’s good.
I’m very positive about that. Um, were you there when they took him off it for the first time?
Christine: I was there within an hour. So my brother had told me they, they did the tracheostomy collar and I went in to see him.
Patrik: And how did you feel like did anything change? What’s your dad like? Was He looking tired, exhausted? Was he struggling to breathe?
Christine: No, not at all… No, they did it again. He looked really good.
Patrik: So that’s, that’s all good. So that’s, that’s the good news. I still believe, you know, they are all talking about LTAC then they’re talking about nursing home. I do believe they’re talking about the wrong things here, you know, the push should be to wean your dad off the tracheostomy and the ventilator if they can and then still get him on to a neurology rehabilitation and not talking about a nursing home. I mean it’s just terrible.
Christine: I know it’s very upsetting
Patrik: And that’s why you need the neurosurgeon almost as one of the advocates, you know.
Christine: And that’s what we’re trying to figure out. You make a good point. And I said that to my brother. I said if we can keep them here at Cleveland Clinic and ICU and get him off the ventilator and the tracheostomy and then they put him in, it’s putting him in the neuro step down to get some strength back. Then we can send him to one of the best neuro rehab programs.
Patrik: Absolutely. Absolutely the right direction to go. Absolutely. I said to James early on, I said, you know what, if he…
Let’s just run it, let’s just run through the worst case scenario. Your Dad can’t come off the ventilator and the tracheostomy and they sent him to LTAC (Long-term acute care). While the LTAC is mainly focusing on weaning patients off a ventilator, but they’re not focusing on neuro rehab, which is what your dad needs. Right, and that’s why. That’s why I’m so adamant about it ,if they can wean your dad off the ventilator at the hospital, well then the LTAC goes out the window because you won’t need that right? Then the next tip is to focus on his recovery for the stroke.
Christine: So this is where we’re a little lost here, is now we get my dad off the ventilator and he’s not ready for the full blown rehab. They call it acute rehab three hours a day. Do you think there’s places, I mean some of these rehabs have the semi acute or whatever they called sub-acute. We have here at Cleveland Clinic, they said to, we only have three hours a day of Rehab. Your Dad’s not ready for it. That’s why I thought, well maybe we should go to the step down here, then try to build them up to the three hours here.
Patrik: Yup, Yup. Absolutely. Absolutely. I mean, you know, leaving the hospital system is not working in your dad’s favour at this stage, you know, and, and l at the end of the day is not, it’s not a hospital, it’s sort of, it’s a facility.
Recommended:
I mean it’s in the name, you know, the other thing that I don’t like about long term acute care is it implies long-term, right? I mean your dad is in a difficult situation and it might take him a while to recover, but the recovery needs to be in the right environment.
Christine: OK. And then my other thought was… I don’t know how you feel. So it’s my brother. I know I’m not an expert with the seizures, but I mean I’m glad to see Dad off the vent and, or getting him in that direction. And this may take a little while, but do you think also before we leave ICU, they may wanna try reducing the Keppra a little bit. Would that be too aggressive at the time?
Patrik: 3000 milligrams of Keppra twice a day. I think that’s what it is, isn’t it?
Christine: 1,500 mg twice a day.
Patrik: So the standard doses that I’ve come across in ICU is mainly 500 mg twice a day, 750 mg, twice a day or 1,000 mg twice a day. Right. But normally it’s 500mg twice a day or on the odd occasion it’s 1,00mg twice a day and that doesn’t include the Dilantin (Phenytoine).
Normally it’s either or. Now in your dad’s situation they’ve had difficulties managing the seizures, which is why they’re probably giving him a high dose of Keppra plus the Dilantin (Phenytoine). So I guess the hospital might look at the situation the following, they think OK, well if we reduce the Keppra and your dad will have seizures, number one, he will stay in ICU longer. And number two, if he does go to an LTAC and he will have seizures again, he will be bouncing back. Right?
Christine: So can you say that again, because they come right back to the lower dose?
Patrik: That’s right. And that, that would be one of the, uh, you know, that might be one of their management strategies. I mean on the one hand, I think it’s very important keeping your dad’s seizure free, but they are probably erring on the side of caution by giving him a fairly large dose and you know, trying to manage it that way. So, you know, the, the other thing, is there a, you mentioned the neurosurgeon is there, a neurologist involved, which is basically the medical side of a neurosurgeon.
So the surgeon is operating on the brain and then you’re, the neurologist is usually managing, you know, managing anything that’s related to the brain that’s non-surgical.
Christine: No, I think he thought he was both. I thought he was doing both.
Patrik: Very rarely happens…maybe on the odd occasion, but that’s not my experience. That’s not my experience. There is.
Most of the time the neurologist is not a neurosurgeon. He might be, but it’s rare that I’ve seen that. Um, but he might be, you never know, but they should be, they should be your advocates around, you know the neuro rehab which should be the focus at the moment. He’s on ventilation because, you know, the sooner he can come off it, the better it is. The long term process should be about the neurology recovery. That would be the long-term goal.
Christine: So, um, we have an epileptic doctor with that Keppra and I said this to my brother too, I said maybe when the neurologist comes back on Wednesday or usually the neurosurgeon came here for he might have ideas about and I don’t know what you think this Keppra and because I think they’re being quite conservative, but you know, I liked the, doing the ventilator now. But once my dad again some strides with the ventilator, I mean it would be nice if they kept the EEG. They don’t have the EEG at the LTAC. OK. So it would be nice that if they did this, if could keep it on. He’s still on, they tried to lower the Keppra a little, you know. So this is all my brother says, I’ll come from what the epileptic doctor said.
They are specialized doctors, just for epilepsy and they are reading the brainwaves, they read everything.
Patrik: So they are even more specialized all they worry about is the seizures?
Christine: That’s all they worry about. Hey. But it was interesting the other day.
I had talked to the head of ICU when I had said, you know, that LTAC is not for my dad and he said, well let’s drop the Keppra to 1,250 mg and then the other epileptic drugs. But no, he kept it to 1,500 mg but we don’t know for, just maybe hit to try and get my strength up or maybe it was because he thought we were going to the LTAC. I don’t know…
Patrik: Have you asked him why he was keeping it at 1,500 mg?
Christine: Um, I, I didn’t ask him and he also said he wanted to keep it there for six months, which I thought was unusual to me to keep it for such a long time at that high level.
Patrik: I remember James mentioning that in an email a while ago, but the reality is your dad would probably be on Keppra and Dilantin for quite some time now. The challenge will be to find the right dose. That will be the challenge because you know at the moment he’s still sort of in the acute phase, meaning that the biggest challenge at the moment is to keep him seizure free, but once they know they can achieve that, that’s the time when they can look at the doses, but it might be a little bit too early to do that.
Recommended:
Christine: I think you’re right. Maybe if and again if he stays in ICU or even a step down here maybe for another week, again, you know, now with the Keppra and the Dilantin for two weeks and seizure free, they might then feel more comfortable lowering the dose and that’s another reason to stay here!
Patrik: I think you mentioned that when you had a look at the LTAC, there’s only one doctor for the whole facility are there. You mentioned that, you know, which is another concern.
Christine: Right, right. I agree. So let me ask you this, do you think my dad will come down on that? Keppra, I know the Dilantin they say is an average dose. I believe at hundred milligrams three times a day. But if we were to get him down on the Keppra and the Dilantin, how could he improve? Would he not be as tired and would he be a little bit more alert?
Patrik: Well, what do you think like in the last few days, is he still opening eyes?
Christine: Yeah, today was extremely alert. Trying to think. Maybe this is from the ventilator off him. His eyes are open a lot. He’s having a lot of facial expression…
Patrik: Is he following your commands and squeezing your hands if you ask him to?
Christine: No, he’s not. So this is where I’m being, where, this is what I think and I don’t know what you’d think if you talk to him and say things to him, his facial expressions. Because I know my dad quite well dictate that he understands, like, I’m pretty sure he’s understanding, however I think he’s very, very tired and cannot do these commands. And so, um, I think it’s either, he’s like, I mean he’s been sitting in the bed for a month now who’s got to be exhausted physically? So, um, I don’t know if he’s not following commands or if he’s just so tired and he doesn’t feel like doing them. I don’t know.
Patrik: So I mean like with anything, you know, the list, but at the same time, you know, I do believe they are conservative in terms of seizure management because they’ve seen that the dose is too low and that he might have seizure. So that’s one train of thought around that. And Your Dad might be following commands. And that’s why Physical therapy is so important which is what I mentioned earlier that they keep moving arms and legs. Yeah, I think it’s, it’s critical.
Christine: Do you think the high dosage of Keppra is causing him not to follow commands?
Patrik: I don’t think so, especially if you feel like, especially if you feel like he can understand and you know, so therefore I don’t think so. I do believe that he’s not following commands, could be a sign of, you know, the brain injury or it could be a sign of weakness, a physical weakness. But that’s, you know, he’s, he’s trying to talk? Is he trying?.
Christine: Yes, he starts moving his mouth a lot.
Patrik: OK, that’s good.
Christine: But, I don’t know. I don’t know if they’re words. I mean, I had seen words come out, like “why”, “know” and “what” I had seen very clearly on his mouth. So I think he would be able to say those words, but I don’t know if he’ll be… he might have a language barrier there. So, I mean they said that the brain, the brain bleed, that’s quite significant, so I don’t know. But, um, based on what they said, they were so bleak. But at the same time, I’m seeing a lot of facial expressions here where he seems to be understanding.
Patrik: That’s interesting, very bleak? Is that what they were saying? A very bleak outlook? Is that what you’re saying?
Recommended:
Christine: Well, the ICU doctor earlier in the week before my dad started to open his eyes a lot more, uh, he said to me that, you know, my dad would require a lot of care for himself long-term. He wouldn’t be able to care for himself. But, you know, this is how I feel.
These are ICU doctors and they don’t follow patients for years and everybody is different and you know, and I don’t mean this in a disrespectful way, the doctors are very competent, but they come in for five minutes, even if they come in and see him, they don’t watch all day.
Recommended:
Everything we see and the responsiveness is enough, you know, the facial expressions. So, um, and I know my dad and he’s left-handed, so, you know, I don’t know if I. At first I was very upset and laughed and then I thought, I don’t know if I believe all that. So, and my feeling is I’m not sticking them in an LTAC and then to a nursing home, I’m giving him a chance to get better.
Patrik: Right. And so that’s what I said to James as well, I can tell you anything that happens in ICU because that’s my area of expertise and when patients do go on to rehab, I have no idea what your dad look like in six months time because it’s not my area of expertise.
And that’s a big downfall for any ICU professional. You know, they try to jump to conclusions. At the end of the day, we have no idea what, what patients lives look like in six months time. Right. And it’s very easy to look at a critically ill patient and be negative. That’s very easy. That’s almost like the default position. Right? But the reality is most patients do survive. We just don’t know what their life looks like down the line. Right. That’s why I believe it’s so important that he doesn’t go to an LTAC (long term acute care) so they can focus purely on his recovery for, for the neurology side of things.
Christine: Right. I agree. Write that down. That’s a good reason that LTAC is not focused on neuro rehab. Therefore LTAC wouldn’t be beneficial.
Patrik: The other thing you may want to find out, maybe more subtle rather than overt is the insurance issue. Whether you know, I mean, it’s good that they haven’t given you a timeline yet, but as soon as they come up with timelines, you may want to look into what the insurance policy says or what your insurance options are because the one insurance might say, you know, you need to go to LTAC because he’s run out of ICU funds, whereas you know, if he’s got another insurance, you might want to look how you can leverage that to keep him in the hospital.
Christine: Yeah. So you think, I don’t want to call the insurance right away because I’m afraid than they might start looking into it. So you’re rising or they give me a timeline then look into insurance. OK,
Patrik: Wait for timeline. OK. Anything I would ask them around timelines to get him off the ventilator. You know, ask them for timelines.
Christine: I know you said to my brother the ventilator might take a year, but I don’t know. Do you think he can possibly come off the ventilator in a week, two weeks from today?
Patrik: Yeah. Too early to say really, you know, it’s the first day off the ventilator. It’s, um, it’s way too early to say where he’s going with ventilation. Some days he might cope well off ventilation and others he may not cope.
Christine: So what’s the normal, how do they, what’s the normal plan to wean somebody off the ventilator? Just how they’re doing it every two hours and he can tolerate that?
Patrik: Yes and then gradually increase with mobilizing him and sitting him out of bed to get his strength back.
Christine: OK. Is that harder for him if he’s sitting in the chair compared to laying down?
Patrik: No. Not at all. And I tell you why!
Number one is to strengthen his breathing muscles, sitting up with strength and his breathing muscles and number two, many patients in ICU on a ventilator end up with pneumonia. Why? That is one of the reasons he’s that he’s immobile in bed and because their lungs basically can never fully expand because there’s too much pressure on the lungs because patients are lying in bed all day long. That’s why they end up with pneumonia. So by getting patients out of bed is the best pneumonia prevention there ever is because the lungs can expand.
Christine: OK. That’s another reason why the LTAC isn’t good. I don’t think they take the patients out of the bed.
Patrik: Something you do want to find out whether they do that or they don’t. I don’t know.
Christine: OK. Hi. I think I’m pretty good. Well I hope we can just stay here and that’s what we’re going to go for. I think right now at this time, keeping him in ICU or going to the step down in this hospital is where we want to be in the mean time.
We’ll find the best rehab around to take them to a neuro rehab and that could be another totally different city. And when we were finding some in Chicago or maybe New Jersey, I mean these are like top notch places. So, um, you know, what to ask when I call these neurology rehab clinics? I mean any advice you could give when I call the neuro Rehab, what I need to ask,
Patrik: Ask about the experience and tell them about your Dad’s situation and see what they say. See whether they can, you know, sort of anchor in what you have to say and whether they can lead the conversation then because if they can lead the conversation and they, they understand your dad’s situation, they can lead the conversation of what to do next. I think those would be the signs to be looking for.
Christine: All right, Patrik. Glad I really appreciate all your thoughts flow.
Patrik: You’re very welcome. Thanks again.
Christine: Have a good night. Thank you.
Patrik: You too.
Christine: OK, bye. Bye.
Watch out for the next consulting session with James in the next episode of “YOUR QUESTIONS ANSWERED”
See you then!
Your friend,
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!