Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode was
How to get into Neurology rehabilitation from ICU after a stroke and avoid a nursing home!
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to continue answering the next questions regarding James’ and Christine’s Dad in ICU who’s had a haemorrhagic stroke.
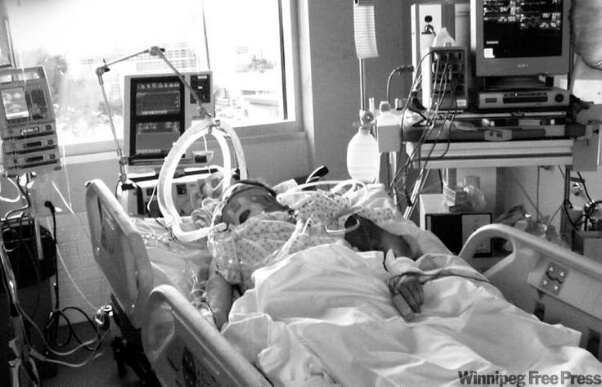
James’ and Christine’s Dad had a brain decompression where they evacuated a large bleed from his brain after the haemorrhagic stroke And their Dad also underwent a craniectomy (removal of skull) to decrease the brain pressures after the bleed.
James’ and his sister Christine were getting their Dad in one of the best hospitals in the USA, the Cleveland clinic in Ohio.
In the meantime, their Dad was getting a tracheostomy because he couldn’t be weaned off the ventilator and the breathing tube. He also had a PEG tube for feeding inserted.
He also had ongoing seizures due to the stroke and his anti-seizure medications needed to be optimized so he could “wake up” and progress to Neurology Rehabilitation.
Since last week’s 1:1 consulting and advocacy session, James’ and Christine’s Dad has been off the ventilator and has been moved from Intensive Care to a step down unit. Their Dad still has the tracheostomy in place but is off ventilation and breathing by himself.
He’s still having occasional seizures and the doctors and nurses are still trying to optimize the seizure medications.
In today’s episode of “YOUR QUESTIONS ANSWERED”, I answer a series of questions from James and his sister Christine again that are excerpts from various 1:1 phone/email consulting and advocacy session with me and the topic this week as part of this series of 1:1 consulting and advocacy session with me and the topic this week is
How to get your loved one into Neurology rehab after a stroke and Intensive Care!
You can also read or watch previous episodes of 1:1 consulting and advocacy with James and his sister Christine here
Patrik: Sure.
Christine: Go ahead.
James: Patrik?
Patrik: Yes.
James: I have my sister Christine on the phone.
Patrik: Right. Great.
Christine: Hi Patrik.
Patrik: Hi Christine. How are you?
Christine: I’m good. I’m good. How are you doing?
Patrik: Very well. Very well. Thank you.
Christine: Good.
Patrik: So with the email that James sent a bit earlier, and I know he’s copied you in. From my perspective I, or, sorry, lets not get ahead. So I understand LTAC is now off the table again?
Christine: Yeah, it’s back on. Did James update you on the status on my dad now? He’s off the ventilator. He’s in step down.
Patrik: Yup. Yup.
Christine: He’s got the tracheostomy still but he’s off the ventilator. I didn’t see the email.
Patrik: Oh I see. Yeah, okay. Okay.
Christine: So we’re trying to think of our options here.
Patrik: Yeah. I mean it’s very concerning that they bring up a nursing home as an option. That is certainly concerning. I still believe that neurology rehab is the right way forward.
Christine: Okay.
Patrik: You know, I mean, a nursing home is just, that’s definitely not the right environment. There’s no doubt about that. It could be-
Christine: Right.
Patrik: It could be an insurance issue, that if your dad was to go to neurology rehab the insurance may not necessarily wanna pay. Right?
Christine: Right.
Patrik: So that’s something you may wanna find out. But I do believe that if the doctors at Cleveland General say he needs to go onto neuro rehab, then the insurance should support that. It’s a matter of getting that statement from the hospital or from the doctors. In terms of the Cranioplasty , now that I’ve spoken to this with James just a moment ago, it sounds to me like he really needs the Cranioplasty sooner than later. And maybe that is something he needs before he’s going on to neurology rehab.
Christine: Do you think, we got two opinions here on what should go back on his head. His original skull, cause it fits better? Or should we get one made? I mean?
Patrik: I don’t know. That’s really, I really don’t. I was just saying to James earlier, that when patients have their Cranioplasty back, they don’t come back to ICU. So I have, very rarely have I seen patients coming back to ICU with a Cranioplasty, so therefore I don’t know.
Christine: Right.
Patrik: I simply don’t know.
Christine: Right. Okay.
Patrik: So how, let’s just say in the last week, would it be fair to say that in the last week he hasn’t made a lot of progress but he’s, I mean he’s out of ICU now obviously. Which is good. But he hasn’t made a lot of progress? Would that be fair to say?
Christine: Well its kind of frustrating because he had this seizure Monday morning, this past Monday. It’s a small seizure. And then they added a third seizure medicine. James do you know the name of it again?
Patrik: Yeah. We’ve got it here.
James: No.
Patrik: It’s Zonisamide, Zonisamide.
Christine: So he’s on Keppra for 35 hundred. He’s on Dilantin and then he’s on this other one.
Patrik: Yeah.
Christine: I think he’s gone. I think he’s just not with us, you know?
Patrik: Yeah, yeah, yeah, yeah.
Christine: He’s just tired inside. And then they added that Seroquel (Quetiapine) at night.
Patrik: Oh.
Christine: 12.5 milligrammes.
Patrik: Oh, how much?
Christine: 12.5 milligrammes.
Patrik: Seroquel? Right. Okay.
Christine: They added this week, Seroquel 12.5, and then that Zonisamide or whatever.
Patrik: Yeah.
Christine: Seizure medicine is the third one. And then my dad’s wife had a psychiatrist come and say he wasn’t cognitive. I’m like, “Of course he’s not cognitive.” You know?
Patrik: Why? Why is he getting the Seroquel (Quetiapine)? Do you know?
Christine: Because they said he was wide awake.
Patrik: At night?
Christine: I don’t know what was going on, but… Yeah. But it was only, honestly it was, we had a new nurse Monday and Tuesday. And all of a sudden all these things changed. Like he was wide awake, he didn’t sleep, so they put him on Seroquel 12.5 mg, now he’s sleeping. Nobody had ever said he wasn’t sleeping before.
Patrik: Mm-hmm (affirmative).
Christine: And then they put him on this third seizure medicine. So I mean he’s like, last weekend my kids came here, he was completely cognitive. I mean, patting my son on the back, his best friend came.
Patrik: Right.
Recommended:
Christine: Very much with it. Talked to me about things, like tried, his expressive language is gone. But he was, these two medicines they added along with everything else, just put him in a real … He’s a little bit more alert today. I don’t know if it takes time for them to balance out, or he’s gonna be like this permanently while he’s on this medicine until they titrate it.
Patrik: Mm-hmm (affirmative).
Christine: So.
Patrik: Yeah. The Seroquel, okay, let’s say a few things. I’m not surprised he wasn’t sleeping at night. I’m not surprised by that at all. Because many weeks in hospital, or in ICU in particular, patients end up with a disturbed day and night rhythm. So I’m not surprised by that.
Furthermore, after many weeks in ICU in a coma, there is also the chance of what’s called ICU Psychosis or ICU delirium. The issue with this is that your Dad is difficult to assess because he’s non-verbal.
Christine: Right.
Patrik: And the Seroquel is sort of, one of the drugs of choice to manage that. But it’s not, it helps patients sleep, but on the other hand they may be too sleepy all of a sudden. You know? Because it has side effects and it’s a fairly strong medication, right? So on the one hand he needs to sleep at night. On the other hand you want him awake during the day. You know?
And the more, anything that’s related to the brain like with the seizure medications as well as the Seroquel (Quetiapine), you’re saying he was awake last week when your kids were there and the best friend was there, and now all of a sudden he’s drifting off again. It makes you wonder whether it’s the drugs that he’s getting now, or whether it’s just his cognition going back. Which is a possibility too, with a stroke.
Christine: I gotta tell you Patrik, he was really sharp last weekend. I just don’t think the strokes going back. I think he’s loaded up. I got a list of all these medicines.
Patrik: Yeah, yeah, yeah, yeah.
Christine: You know, and it aggravates me because I just spoke to the seizure team, and what they did is, and I don’t know what you’d say. But Monday he had the seizure in the morning, and then he’s had three seizures before that. So he had a seizure on August 29th.
Patrik: Yup.
Christine: Then he had one two weeks later on September 12th. And then he had one a week later, this past Monday. So I said, then they took the EEG off today and I said, “Why did you take it off? He was going a week between these two seizures, why wouldn’t we at least wait a week to take it off and make sure he’s seizure free for a full week?”
Patrik: Yeah, yeah, yeah, yeah.
Christine: And you know, I really felt like I was pushing it and then putting them … You know, he was good. The doctor was good. He said, “I don’t really see a reason.” And he said, “It was such a small seizure.” And then I said, “Well why did you add the third medicine?”
Patrik: Yes.
Christine: I try not to be like that. You know? I’m just questioning what’s going on here.
Patrik: Yeah, exactly.
Christine: He said, “Well we did it.” And I said, “Well now he’s out of it and you’ve not, and now they’re not approving him for acute rehab but for a skilled nursing home.” You know?
Patrik: Yeah.
Christine: So I don’t know. I’m starting to think, I don’t know if John told you this, but we know a doctor in Buffalo. He can do a hospital to hospital transfer. And they can manage his seizure medicines and maybe get my dad stronger, and start some rehab. I mean it’s not the best hospital in the world, but it is nice, and we know the doctor who knew my dad before this pretty well.
Patrik: Yeah.
Christine: And maybe they can strengthen him to get my dad more cognitive because, to go to a neurology rehab, you know what I mean?
Patrik: Absolutely.
Christine: Like sending him off to Chicago, now I’m starting to think, “How am I gonna send my dad off to Chicago to neurology rehab when he’s out of it?” You know?
Patrik: Yeah, yeah, yeah.
Christine: And he was fine four days ago, and then you’re gonna stick him in a skilled nursing home. I’m afraid he’s gonna get stuck there.
Patrik: Absolutely. And I mean the skilled nursing home just sounds horrible to me. I mean, and I think if you can get him closer to home, I do believe that the family support is just as important as the environment. But you know, you’re absolutely right. You could send him to Chicago to the best neurology rehab in the United States, but that’ll be difficult for you to be there probably. You know? And you’re thinking around bringing him closer to home might be the right approach.
Christine: Why can’t we, I mean, our goal is to bring him to Chicago. But there’s this in between phase.
Patrik: Okay.
Christine: So I mean, are we losing time by not getting him to Chicago? Like if we bring him home for a couple weeks, and get him cognitive, and get these seizure medicines straight, and keep him in the hospital with this doctor. And then now my dad’s like, we’ve titrated some of the seizure medicine, now he’s pretty cognitive. And at that point we say “Okay, let’s go into three hour rehab in Chicago, you’re good.” You know what I’m saying? Are we losing time on this whole thing by not going immediately into rehab up in Buffalo?
Patrik: Yeah, yeah, yeah. Look I do believe that the sooner he can go onto neural rehab the better it is. That’s one thing. But there are those intermediate steps and one of those intermediate steps, even maybe before bringing him to Buffalo, is the Cranioplasty. Right? So whilst he’s in the hospital in Cleveland, maybe that’s something they need to look at. And I mean it sounds-
Christine: They don’t want to do that for eight weeks from the time, so that would be like the beginning of October. And they’re trying to push us out of here. And then not only that, my dad’s skull, or whatever, his part, is in Buffalo.
Patrik: Yeah. Yeah.
Christine: So.
Patrik: Yeah, I think it’ll be important to have a plan with the Cranioplasty. He can go to neurology rehab. I’m very certain he can go to neurology rehab without having the Cranioplasty back. But you don’t wanna go to neural rehab without the Cranioplasty and then interrupt that probably. You know? You would wanna have the neurology rehab and then potentially after that, have the Cranioplasty. Or do it beforehand.
Christine: Okay.
Patrik: That’s what I think. Because you don’t wanna have, once he’s at neurology rehab, you don’t wanna interrupt that with another surgery, necessarily.
Christine: Mm-hmm (affirmative). Mm-hmm (affirmative). Yeah. I don’t know. I’m gonna have to talk to John. I’m starting to think it’s not a bad thing to come home for a little bit.
Patrik: Yup.
Christine: As long as it’s not skilled nursing.
Patrik: Yes.
Christine: If we could do that hospital to hospital transfer.
Patrik: Yup.
Christine: And have someone put that, this doctor will give us the referral to RSP.
Patrik: Yes, yes. I think that’s what-
Christine: You know? We know him.
Patrik: Yup.
Christine: So you know, and then just kind of regroup there. This is family. I mean how can he go there on three seizure medicines? I mean we don’t know. Do you know what I’m saying?
Patrik: Yup.
Recommended:
Christine: It’s like, I mean is he gonna get the most out of it anyway, even when he’s on all this medicine?
Patrik: That’s right. That’s right. I think bringing him home might not be a bad idea.
Christine: See, but we can always bring him, there’s no LTAC’s in Buffalo. So if we can’t get the hospital to hospital transfer, then we’re back at a nursing home in Buffalo, which is a disaster.
Patrik: Mm-hmm (affirmative).
Christine: So, you know. And then they tell you, “Well a hospital has infections. It’s not the best place for people.” But he’d have his own room there. You know what I mean?
Patrik: Yup. Do you know if there are any neurology rehabilitation hospitals in Buffalo or in the area?
James: Yeah, there’s a couple.
Patrik: Okay.
Christine: Yeah, there’s that EC. Yeah. I mean, they’re not as expensive as Chicago. James there’s ECMC, I mean-
James: Right.
Christine: Actually I’m thinking-
James: There not state-of-the-art facilities.
Christine: Right.
James: Mm-hmm (affirmative).
Christine: Buffalo is just a small town.
Patrik: I know Buffalo. I’ve been to Buffalo.
Christine: Okay.
Patrik: 20 years ago. I know Buffalo.
Christine: Oh, okay.
James: Mm.
Patrik: I’ve been to Toronto, and that’s when I went into Buffalo as well at the time.
James: Mm.
Patrik: Okay. So, okay. I think they gotta get the seizure medication straight. Whether they do that at Cleveland or whether they do that somewhere else, I think that’s imperative. Have them try and get some plan about the Cranioplasty. And then try and get him into neurology rehab. That would be my advice for now. I can’t tell you where you should be doing that, whether you should be sending him to Chicago, whether you should be taking him home. But maybe taking him home to be in a familiar environment, that familiarity in an event like that, I think that’s important too.
Christine: Yeah, well I kinda feel like if we brought him home and we get the seizure medicines down, and he’s around his family, he might become a lot more cognitive.
Patrik: Yes. Yes. If he was-
Christine: And … I’m sorry, go ahead.
Patrik: If he was to go to Chicago, you couldn’t be there all the time.
Christine: Well his wife could be, but I mean, I think my brother and I both feel at least one of us should always be around, to kind of, it’s a lot on one person, and there’s a lot of decisions, critical decisions actually, I think.
Patrik: Absolutely.
Christine: Not that we’d tell her what to do, but I think our input as his children helps. You know?
Patrik: Oh, totally. Totally.
Christine: So that’s what kind of concerns me while we’re on the phone here, is I haven’t told my brother that, but my brothers not gonna be able to be in Chicago a lot, and neither am I. It’s a little bit further for us than Cleveland, and we’re not always gonna be able to be there. So I’d rather have him go tot Chicago when he’s a lot more cognitive.
Patrik: Mm-hmm (affirmative).
Christine: You know? So I don’t know. I gotta talk to my brother about that. You know, it’s kind of this balancing act where we can’t put him in the best neuro right off the bat because he’s not cognitive and he’s on this medicine.
Patrik: Mm.
Christine: You know? So. But now the other thing with the Cranioplasty, is that like, we have one doctor the one, we have two choices on where to bring him. Between two doctors. The one doctor, they’re both neurosurgeons, but the one does more back surgery, but he says he can do the Cranioplasty no problem. I mean is that a simple thing or do you really need a very expert neurosurgeon?
Patrik: As I said, I don’t know to be honest. Because-
Christine: Okay.
Patrik: When patients leave intensive care they don’t have the Cranioplasty done. They leave without the Cranioplasty right?
Christine: Mm-hmm (affirmative).
Patrik: And when they have the Cranioplasty they don’t come back into intensive care most of the time. So I haven’t really seen it. I have no experience around that, if that makes sense.
Christine: Right. Right. You know John, the more I think about it, if we went with the Landi to Kenmore, the excuse would be that his skull is at Buffalo General, so we don’t want to risk anything with bringing the skull to Kenmore Mercy.
James: Right.
Christine: You know? That would be a way to get around it.
In next week’s 1:1 consulting and advocacy session we continue the discussion between James, Christine and myself to get James’ and Christine’s Dad into Neurology rehabilitation and we continue to find proven strategies that work to get their Dad best care and treatment! Look out for the next episode of “YOUR QUESTIONS ANSWERED” and I’ll talk to you then.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!