Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode was
How to get your loved one into Neurology rehab after a stroke and Intensive Care!
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to continue answering the next questions regarding James’ and Christine’s Dad in ICU who’s had a haemorrhagic stroke.
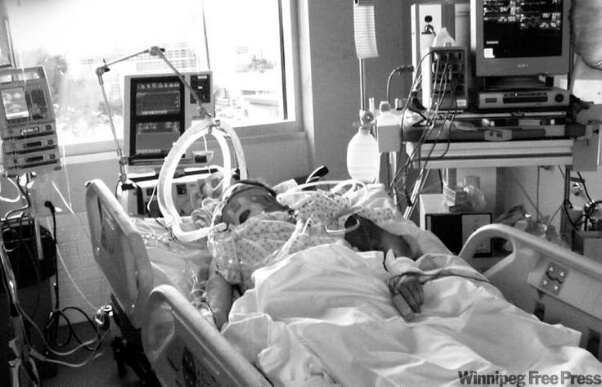
James’ and Christine’s Dad had a brain decompression where they evacuated a large bleed from his brain after the haemorrhagic stroke. And their Dad also underwent a craniectomy (removal of skull) to decrease the brain pressures after the bleed.
James’ and his sister Christine were getting their Dad in one of the best hospitals in the USA, the Cleveland clinic in Ohio.
In the meantime, their Dad was getting a tracheostomy because he couldn’t be weaned off the ventilator and the breathing tube. He also had a PEG tube for feeding inserted.
He also had ongoing seizures due to the stroke and his anti-seizure medications needed to be optimized so he could “wake up” and progress to Neurology Rehabilitation.
Since last week’s 1:1 consulting and advocacy session, James’ and Christine’s Dad has been off the ventilator and has been moved from Intensive Care to a step down unit. Their Dad still has the tracheostomy in place but is off ventilation and breathing by himself.
He’s still having occasional seizures and the doctors and nurses are still trying to optimize the seizure medications.
In today’s episode of “YOUR QUESTIONS ANSWERED”, I answer a series of questions from James and his sister Christine again that are excerpts from various 1:1 phone/email consulting and advocacy session with me and the topic this week as part of this series of 1:1 consulting and advocacy session with me and the topic this week is
How Physical Therapy/Physiotherapy will help your loved one to get off the ventilator and tracheostomy!
You can also read or watch previous episodes of 1:1 consulting and advocacy with James and his sister Christine here
Hi Patrik,
My Dad’s making progress and he’s now having time off the ventilator during the day.
What exercises should the Physiotherapist doing with my Dad while they are weaning him off the ventilator?
Do you have any videos?
Thanks
James
Hi James,
Unfortunately, I have no videos of exercises.
For now the Physiotherapist/Physical therapist should be doing the following
- Get your Dad out of bed twice a day, once in the morning and once in the afternoon, with a break around lunchtime for a rest
- Sitting him on the edge of the bed and see if he can maintain strength in his upper body
- Sitting him out of bed if he can in a recliner chair
- Doing breathing exercises with the goal to strengthen respiratory/breathing muscles
- Coughing exercises, again the Physiotherapist should be doing that if your Dad can cooperate? If he can’t cooperate with coughing exercises they may be using a device called “cough assist” to again strengthen respiratory/breathing muscles and also clear his cough
- Coughing will be essential to eventually also have the tracheostomy removed after he can stay off the ventilator
- They should also continue to move arms, legs to maintain movement, prevent contractions and build up muscle tone. You can move his arms and legs too, any movement and stimulation will be good, as long as he can stay seizure free
- Potentially try and stand up with the help of 1,2 or 3 people depending how and if he can manage
- March on the spot if he can
I hope this makes sense, any questions please let me know.
Kind Regards
Patrik
RECOMMENDED:
Hi Patrik,
Thanks Patrik.
We are really perplexed on what to do with him, where to move him etc.
We are glad he is making steady progress, the ICU is not doing any of these things for him that you described.
At best they put him in a chair once/day and that’s it.
Seems as though step down or LTAC is a bad choice.
What are your thoughts?
James
Hi James,
As I have said many times before, any ICU is much better equipped/skilled to wean a Patient off the ventilator and the tracheostomy than any other area, let alone LTAC.
The only other place that can wean a Patient off the ventilator is INTENSIVE CARE AT HOME services.
It’s very disappointing to hear that they are not doing any of the things that I mentioned, given you are in one of the best hospitals in the US.
It sounds to me like they are in the very early stages of weaning him and given that they probably started weaning him on a weekend, I hope this will gain more speed starting Monday with more resources/staff being available.
I do believe there is a tendency in the US to use a tracheostomy as an excuse to move Patients on to LTAC rather than taking measured steps to wean Patients off the ventilator whilst they are still in ICU.
Bare in mind that in ICU you have the full expertise of Critical Care/Intensive Care doctors, Intensive Care nurses, Respiratory therapists, Physical therapists etc…
Without that level of expertise that is required to wean somebody off the ventilator, LTAC has the potential to set your Dad back.
We get far too many enquiries in regards to families wanting their loved ones out of LTAC because they think it’s disastrous and not what they expected.
Families often think that LTAC’s don’t wean aggressive enough and they often think they deliberately keep Patients on ventilation and tracheostomy to keep their beds occupied. I do believe there are some shocking practices out there.
The reality is that step down as well as LTAC (long-term acute care) won’t provide the same level of care, skills and expertise than ICU. If he was well enough then step down would be good, but it doesn’t sound to me like he’s ready yet.
Have they given you time lines for moving him?
Kind Regards
Patrik
Hi Patrik,
I had the opportunity to tour the LTAC’s today in Cleveland. I was not impressed. In fact, I was getting even more worried for my dad. We are going to ask Cleveland Clinic if my dad can stay in the ICU but they may say we need to leave due to insurance etc.
Do you know what we can say or the reasons to justify for keeping my dad in the ICU as long as possible and then going to the Neuro step down in the hospital? We toured that floor today at the hospital and it was far better than a LTAC.
Thank you,
James
Hi James,
I have spoken to your sister in regards to this issue.
We have been speaking about how to potentially avoiding LTAC and keeping him in hospital/ICU for as long as possible so that they can focus on weaning him off the ventilator and the tracheostomy.
Once that’s been achieved then next steps could be Neurology rehabilitation.
It’s good that there are no timelines yet, once they start introducing timelines around when to leave hospitals you may have to speak to insurances to find out about what they are prepared to fund.
Kind Regards
Patrik
Recommended:
Hi Patrik,
I think I may have little good news.
My father has been up in a chair breathing with the tracheostomy collar most of yesterday and today. He was in the chair for 5 hours and on the tracheostyomy collar for 10-11 hrs total.
Speech therapist came in today put in a speaking valve. They deflated the tracheostomy cuff and discussed using ice chips with dye tomorrow.
Physical Therapist seems to really get him moving today around 12:30 especially when they sat him up straight in the chair. By the end of the day he was actually fighting with my sister to try to take the helmet off his head. I think it was too hot.
It is not safe to even take the mittens off.
They bumped up his dose of Keppra today by 250 mgs because he has a mild seizure early Monday morning.
Wondering if that could be from the Tracheostomy collar ???
Would be nice to hear my father speak a few words at this point !
Please email back with your thoughts and guidance on the above!
Thank you
James
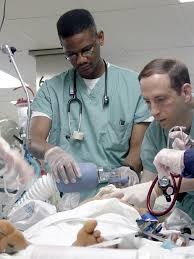
Hi James,
That’s fantastic news and lots of progress!
Seizure is unlikely from tracheostomy collar but it can’t be ruled out either.
Seizures are probably more of a combination from stimulation through mobilisation. At this stage keeping him seizure free is very important to not jeopardise any recovery, hence if they think increasing Keppra is keeping him seizure free then I would support the increase in Keppra.
It’s very encouraging to hear the speech therapist is giving him ice chips. If tracheostomy cuff comes down he might be closer to speaking but don’t be discouraged if he doesn’t talk straight away, one step at the time. Just by what you are describing, it sounds like he’s made a lot of progress just within a few days.
Talk soon
Kind Regards
Patrik
Hi Patrik,
My father had a very interesting day.
They said his blood pressure was low this morning and his white blood cell count is a little over 11 so for some reason they put an IV in his neck to deliver antibiotics in anticipation of an infection.
I don’t know why or how but he became irate. He kept trying to bite his mitt and take it off with his teeth. It was moving his lips and seem like he was trying to yell at everybody.
They did put an arterial line in today.
He seems to be breathing with no problem on the collar.
We got a few words out of him with the speaking tube however he is still not responding to commands but is very active nonetheless. Keppra is at 3500 and Dilantin is at 300.
I have been fighting tooth and nail to keep them in this hospital I’m not moving to the LTAC it’s been kind of ridiculous.
Please email me back with your thoughts on all of the above.
I feel like my father is aware and can understand but is just not able to get the words out. Sometimes the drifts in and out.
The doctors mentioned that he may be depressed from the brain injury and suggested Zoloft (Sertraline).
Many thanks
James
Hi James,
If his blood pressure is low, this could be a sign of infection indeed, White cell count (WCC) 11 is slightly elevated (normal range is 4.3-10.8) and it may well be the beginning of an infection, but I think it might be slightly premature to treat with Antibiotics (AB’s) and putting in an IV, unless they have done more testing and they have already found the source of the infection?
Also, do you know if your Dad has a temperature?
Have they done any other screening for the infection, I.e. taken blood cultures, done a chest x-ray, have they done swaps from catheter, urine or any other IV’s and/or PEG site? Those could all be potential sources of infection.
Recommended:
It’s great to hear your Dad is breathing fine on the tracheostomy collar, has he been back on the ventilator at all in the last 24-48 hours?
Also good to hear your Dad is trying to mouth words or even yell, even though that could be a sign of frustration indeed and it could be a sign of depression, but I come to that in a moment.
Are you also saying his Dad has mittens on his hands to stop him pulling things?
Also if his blood pressure is low, have they started him back on inotropes/vasopressors such as Norepinephrine and/or Epinephrine?
On the one hand I don’t like they put back in arterial line, however as long as he has an arterial line he won’t be going to LTAC. The arterial line to me is a sign they most likely have started him back on inotropes/vasopressors such as Norepinephrine and/or Epinephrine and you may want to find out.
If you think your Dad is aware of what’s going on and can’t talk, it could be that the speech area of the brain is affected from the stroke, a question you may ask the Neurologist.
Keppra dose still high but if it’s needed to keep him seizure free, so be it for now.
Your Dad is on a long road to recovery and it looks like he will get out of ICU alive. That was and still is your first goal, even though there are setbacks with a potential infection. Being off the ventilator is a very good sign and continue to avoid the LTAC if you can.
Arterial line and potentially inotropes/vasopressors means no LTAC for now, being off the ventilator also diminishes the likelihood of LTAC.
Depression might be a reality for your Dad, if you think he’s depressed too, they may start him on some antidepressants, we should probably discuss in more detail over the phone.
Kind Regards
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!