Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
What Would Be Our Next Option after ECMO for my Loved One with ARDS in the ICU?
You can check out last week’s question by clicking on the link here.
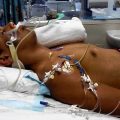
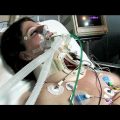
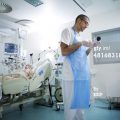
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tara, as part of my 1:1 consulting and advocacy service! Tara’s brother-in-law is with a breathing tube and ventilated in ICU due to ARDS. Tara is asking why the ICU team is negative about their loved one’s progress in weaning off ECMO in the ICU.
Why is the ICU Team Being Negative About my Loved One’s Weaning off ECMO in the ICU?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tara here.”
Tara: This is Tara.
Patrik: Hi, Tara. It’s Patrik from here from Intensive Care Hotline. How are you?
Tara: Good, how are you doing?
Patrik: I’m very well, thank you. How can I help you?
Tara: Well, it’s been a couple weeks since we spoke.
Patrik: Yes.
Tara: The week after we spoke… First of all, I want to thank you for reassuring us that they can’t just pull the plug on the machines as they were acting like. That alone was reassuring. The doctor that we had that week was something else. Oh my. She was just extremely rude, disrespectful, I would say, negative, basically told my sister that they could… I think I told you that that they could just, she had signed something, and they could unplug him whenever they wanted. She told her at one point, I think it was towards the end of that week, that she didn’t think he was going to make it through the night, that his organs were failing and he would be dying within a few days, is what she had told her.
RECOMMENDED:
Tara: Anyway, we got through that week. Thankfully, she left and another doctor came in. The new doctor was, she was nicer. She said, “I’m not going to sugarcoat things, but we’re going to do everything we can for him.” One of our questions is, well, first of all, so what happened last week, they were trying… I don’t even know what they did, but they did some sort of new breathing treatment, a couple different ones, actually. One on the ventilator and some kind of nebulizer or something.
Patrik: Yep.
Tara: Then, on that weekend… pretty much, his oxygen levels were pretty low. I guess I was thinking that the ECMO was able to keep your oxygen levels up, but apparently that’s not the case, because his oxygen levels were low 80s.
Patrik: Right.
Recommended:
Tara: Maybe 85. They were getting concerned. Then the next day, I’m just going to call it miraculous because that’s how we felt about it. That morning, all of a sudden, his oxygen levels went up to 95 and his… I guess they measure, it’s called I guess tidal waves. What they said was the tidal wave, the whole time, the weeks he’s been in there, hasn’t been above 70. That day, they went up to the 200s and they said they could tell he was starting to use his lungs.
Patrik: Yep. Yeah, I’m following there. Yep. I’m following. It makes sense, yeah.
Tara: Okay. And then through the weekend, he continued to get a little better. His lungs were… well, yesterday, it went up to 400, the tidal, whatever they call it. Tidal-
Patrik: Tidal volume, yep. Yep, that makes sense.
Tara: Tidal wave was up to 400. Yeah. Yep, today was… he got off that high today. It was the 300s again, but anyway, now they’re I guess talking about possibly, there’s hope to wean him off the ECMO or they’re going to start a little bit at a time.
Patrik: Yeah.
Tara: One of our questions was, and I don’t know if this is even a question to ask you, but it’s been very frustrating with the doctors changing every few days, several days.
Patrik: Yes, I can imagine.
Tara: Is there a way to either request a certain doctor or not have a certain doctor or not have a certain doctor?
Patrik: Yes and no. Let me ask you a few questions. How big is this ICU? How many beds?
Tara: Well, that is a good question. I do not know. I wonder if my sister would know.
Patrik: Okay. Just give me a second. Okay, let’s just say it’s a 10, 15 bed ICU, it’ll be difficult for you to request a different doctor. If it’s more than 15 beds, let’s just say it’s 30+, there would be more than one specialist on duty, which means, yes, you should..
Tara: I see.
Patrik: … be able to request.
Tara: Okay.
Patrik: Right?
Tara: Yeah, I don’t know how that works, if they just have shifts.
Patrik: Pretty much.
Tara: Because one doctor will be there for a week and then the next he gets another one, and then the next he gets another one.
Patrik: Pretty much.
Tara: Okay.
Patrik: And they are working long hours when they are on duty, so that’s why you will only see them doing a few days. Different ICUs have different rosters, but usually, from my experience, it’s usually seven days on, seven days off or seven days on, seven nights off, something like that.
Tara: Sure.
Recommended:
Patrik: But it’s not… that’s why it really depends on the size of the place.
Tara: I see.
Patrik: I can’t-
Tara: Well, there’s a different one, now, a third one this week, but the difference between the doctor last week and the week before was just unbelievable.
Patrik: I’ll bet.
Tara: I don’t know for certain that she was the reason that the new treatment started, but it happened at the same time, so kind of made me think she may have been the reason. But yeah, that’s been one of our things is I don’t know how that works.
Patrik: Yeah. What’s your main concern with the doctor? Is it just the attitude?
Tara: Well, the first one was the attitude, and I guess we didn’t feel like she was really even treating him. You know what I mean? The other doctor was like, “We’re going to do everything we can.” She basically just had given up and said, “You need to give up.”
Patrik: Right.
Tara: I mean, she also said things that weren’t true in my opinion. I don’t know why she said his organs were failing when they weren’t, and then she told my sister the thing about fibrosis, which you probably remember when you asked the nurse, “Has he been diagnosed with that?” The nurse was like, “Well, no, it’s not in the file,” so I don’t know if she just said that for… I don’t know, it was just strange.
Tara: But the other question we had as far as… now, do you know how that works with the ECMO, weaning it? Do they have to be at a certain..?
Patrik: Yes.
Tara: I don’t know the tidal volume. I don’t know what they have to be at in order to..
Patrik: Yeah, so I’ll tell you what my interpretation of the information that you’ve given me is. I’ll tell you my interpretation.
Tara: Okay.
Patrik: So, he probably would have been in an induced coma for quite some time while he was on ECMO, and they might have lowered his sedation to get him out of..
Tara: They did lower his sedation.
Patrik: Right. And that’s when he..
Tara: They did. They lowered him a little last week.
Patrik: That’s when he would have started breathing. So prior to that, he was probably in a deep coma to let the lungs heal, and then they would have done chest x-rays and they would have done blood gases and they would have done all sorts of tests. They would have seen that the lungs are probably improving. That would have been the sign for them to lower sedation and then see whether he can start breathing. And it sounds to me like he did start breathing.
Tara: Yes.
Patrik: Right?
Tara: Well, when I say they lowered sedation, I think pretty much all week last week, it was a little bit lower.
Patrik: Okay, great.
Tara: They also put him on a different sedative, which he had been on ketamine I think for a while.
Suggested links:
Patrik: Yeah.
Tara: I don’t know if this is why, but his blood pressure was really high and they claimed they did want to lower the sedation, because it made his blood pressure go up. But the doctor, the negative doctor, she had told her that the reason his blood pressure went down was because his heart was struggling or whatever, but it happened the same time where that they switched him off of ketamine, so I kind of thought maybe that had something to do with it, too, all of a sudden, because I know ketamine does raise your blood pressure.
Tara: But anyway, whatever the case, they did let him start waking up last week more, and this week he seemed… even though he’s still semi-sedated, just way more I guess alert or aware.
Patrik: Why? That’s good.
Tara: Last week, he actually tried to get up out of the bed.
Patrik: Oh, really?
Tara: Yeah.
Patrik: That’s good.
Tara: Well, yeah. This is when they had him really sedated, too. I told my sister that to me, that’s a good sign when they’re fighting like that because he had been sedated for… I mean he’s been in there for..
Patrik: Absolutely.
Tara: He’s been on a ventilator for six weeks, and last week, she said he… she talks real positive to him. My sister, she’s a very positive person, which I guess in the situation, you either remain positive or you fall apart.
Recommended:
Patrik: Agreed. Agreed.
Tara: But she was just talking very positive to him, and she said he literally tried to… his hands are tied, but she said he fought like crazy and she could tell he was trying. She said he squeezed her hand really hard and tried to get up out of the bed. The nurse quickly sedated him. She was kind of freaking out a little bit, because he’s on the ECMO and didn’t want him to move too much, but she said, “What do you want to do? Do you want to write?” He shook his head no and my sister was like, “You want to get up and run out of here.” He shook his head yes. She said, “I knew what he was trying to do.” But anyway, so I thought that was a good sign. This is before his lungs started working more that he did this.
Tara: This week, she said just more alert-acting and stuff, which I don’t know if that’s… I guess maybe they are lowering sedation more. I don’t know. But anyway, what you were saying, sorry I interrupted, what you were saying about the weaning process.
Patrik: Yes, so they would have lowered sedation. They would have seen him starting to breathe.
Tara: Okay.
Patrik: And if his breathing is adequate, they would start weaning ECMO.
Tara: Okay. Do they basically just… because she said something about today, they turned it off for like, I don’t know what that means, turn it off. If they turned the oxygenator off or what, but for like 15 minutes, and then just to see how he’s doing, then put it back on.
Patrik: I think they would have turned off the sweep gas flow, probably. It’s probably very technical, what I’m saying now, but they would have reduced some of the oxygen and they probably would have reduced the sweep gas flow. You’re reducing the oxygen to regulate the oxygen in the body and you are regulating the sweep gas flow to regulate the carbon dioxide in the body.
Tara: I see. So just to see how the body basically reacts to it or whatever?
Patrik: Well, yes. So, what they would do is this. What they wanted to achieve by doing that is this. They would want to see, if we’re reducing oxygen support on ECMO and if we are reducing the sweep gas flow, is the then triggering some breaths from the machine?
Tara: Oh, okay.
Patrik: Is the ventilation support enough to wean off ECMO?
Recommended:
Tara: I see. Okay.
Patrik: Basically what ECMO is doing, is ECMO is a replacement of the lungs, 100%.
Tara: So they can’t completely get your oxygen levels tied… do they need to be, though? Because that’s one thing we were confused about last week was why they were so low even on the ECMO.
Patrik: Yes. I believe… I’ll tell you what my interpretation of that is. If the oxygen levels are low, even on ECMO, the doctor might have been right when the doctor said his organs are shutting down and they might have shut down temporarily, because no amount of ECMO support can support organs that are shutting down.
Tara: I see.
Patrik: That’s what I’m hearing here. And for whatever reason, it looks like he turned the situation around, which is great.
Tara: Yeah. He definitely… something happened between midnight Friday night and Saturday morning when she got there. Everything just jumped up. The oxygen went up and the tidal volumes went up. So anyway, they’ll just basically, I suppose, just see how he does until they can… that’s how they wean him off, they just keep trying to turn it down or whatever.
Patrik: Exactly. Basically, I’ll tell you what needs to happen. When they wean off ECMO support, a number of things need to happen. They need to lower sedation. They need him to do more work with a ventilator. Or, if he can’t do more work with a ventilator, they need to change his ventilation settings so that he’s adequately ventilated so that they can-
Tara: Would that mean they would turn the ventilator up, then? Because he’s been very low this whole time.
Patrik: Yeah. No surprises there. Yes, they would have to increase support, because as good as ECMO is, ECMO is time-limited.
Tara: Yeah.
Patrik: There’s too many risks that come with long-term ECMO.
Suggested links:
Tara: Right, okay.
Patrik: How long has he been on ECMO now?
Tara: He’s been on it… no, he’s been on it for almost a month.
Patrik: A month? That’s a very, very long time. Very long time. They would want to move with that fairly swiftly, I would think.
Tara: Okay.
Patrik: And yes, they would need to see that the ventilator can take over the supply of oxygen. In the ideal world, he would do most of the work on the ventilator. And if that can’t be achieved, they would use ventilator settings where the ventilator is doing all the work, but they would have the ultimate goal at the moment to remove him from ECMO as quickly as possible.
Tara: I see. Now, the ventilator, what does that… can you explain a little bit what that means? When he’s at, say, 300 or 400, what is a good number?
Patrik: Yes, I’ll tell you what a good number is. What’s his weight, do you know?
Tara: I think he’s about, I thought she said like 300.
Patrik: 300? Just give me a second.
RECOMMENDED:
Patrik: Yeah, so let’s just say… so that’s 300 pounds, is it?
Tara: Yes.
Patrik: Yeah. So that’s around 136 kilos. I’m just looking at my calculator here. The research suggests 7 to 10 mils per kilo. If he’s 136 kilo, you could say per breath, he should be breathing at least 1,000 mils. Now-
Tara: So when they’re saying 300, that’s mls?
Patrik: That’s not enough. It’s not enough. It’s not enough.
Tara: But I’m saying, when they’re saying 300, that’s considered mls? Is that-
Patrik: Yeah, mls. 300 mls. Yeah. It’s not enough.
Tara: Okay. All right.
Patrik: Probably not even a third he should be breathing. Just remind me, Tara, does he have a tracheostomy?
Tara: No. That was our other question, because they had told her, originally, the doctor had said they were going to do that, and then they just decided they’re not going to do it, because they said it would not change his outcome is what they said that we said they were being negative. Now, what they’re saying is they’re saying they don’t want to do it because it’s too dangerous to do it while he’s on the ECMO.
Patrik: Agreed.
Tara: But they want to possibly do it… you’re possibly doing it as soon as they get him off the ECMO. That was the other thing we were wondering about, because I don’t know… sounds awful to do another procedure at this point, but I mean, at what point… because she said at first, it seemed like those tubes really bothered him down his throat, and now he’s actually had… he’s been on the ventilator with those tubes for six weeks now, and the weird thing is, it doesn’t seem to affect him anymore, as far as he’s not acting irritated. Is there a danger to having them long? I mean, I know they already put it on six weeks.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!