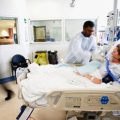
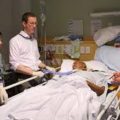
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Will our Loved One with ARDS Benefit from a Lung Transplant in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tara, as part of my 1:1 consulting and advocacy service! Tara’s brother-in-law is with a breathing tube and ventilated in ICU due to ARDS. Tara is asking what would be their next option after ECMO for their loved one with ARDS in the ICU.
What Would Be Our Next Option after ECMO for my Loved One with ARDS in the ICU?
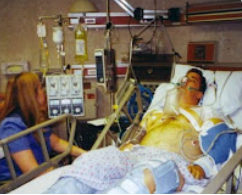
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tara here.”
Patrik: Right. There is reference on the website for lung transplant for children. But not for adults. Having said that, I have worked in ICUs where it was an adult unit, but we actually did also pediatric lung transplants for ECMO. It can go both ways. ECMO is a specialty in and of itself, whether it’s for adults or for children.
Sandy: Right.
Patrik: It’s a specialty in and of itself. And as I said, often, the centers don’t necessarily discriminate between adults and children.
Sandy: Okay.
Patrik: I hope that’s shedding some light on the situation. I tell you what, I’m pretty things sort of, once you have a call with the doctors, or once we have a call with the doctor. Depending on the CT scan result.
Sandy: Yeah.
Patrik: If the CT scan result is talking about fibrosis, they will probably be very pushy for end of life. You got to be prepared for that.
Sandy: Okay.
Patrik: And when I say prepared, I’m not saying that you should be prepared for end of life.
Sandy: Right.
Patrik: What I am saying is we need to be prepared for the discussions around it. And what I mean by that is…
Sandy: Right.
RECOMMENDED:
Patrik: … Challenging them on what I mean mentioned earlier…
Sandy: Right.
Patrik: … On a policy level in terms of, well, you can’t just withdraw life support without medical power of attorney consent.
Sandy: Okay.
Patrik: Does your husband have a living will?
Sandy: No.
Patrik: Okay. Because well, your husband is probably too young for that, but mainly elderly people, some elderly people have a living will where they say, “Look, if I ever go into ICU on a ventilator, I want everything done. I don’t want everything done”. But if that’s not the case…
Sandy: Right.
Patrik: Then if that is not the case…
Sandy: Yeah.
Patrik: … Then you as the medical power of attorney needs to have that say what, what you want on his behalf.
Sandy: Right.
Patrik: But unless there is a formal CT scan result at the end of the day, it’s all speculation.
Sandy: Yeah. What are you thinking now? Think it would be good to have a call tomorrow after they get the…
Suggested links:
Patrik: Oh, you tell me when you want to… Yes. I think the CT scan result is important as part of the discussions. Do you have access to medical records?
Sandy: I don’t know. Would it be from them?
Patrik: Look, most hospitals nowadays, if you want access to medical records, they just point you to a website and they give you a password and the login.
Sandy: Right.
Patrik: When I’m on their website at the moment, I can’t see that link. Normally, on their website, there would be a link to what’s called my chart or there’s…
Sandy: They said that the other day that he directly sign up for your online medical record using this link.
Patrik: Right. Look, the more information you have and the more information we can access besides talking to the doctors and the nurses directly the better it is because again…
Tara: Oh, so you could actually see that from his chart is what you’re saying.
Patrik: That’s what I’m saying. And you can see too…
Tara: Right.
Patrik: … If you…
Tara: Yeah.
Patrik: … especially blood results, often you can see ventilator settings. The more you can see, the more you can question.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Tara: Okay. So can you sign up for that Sandy so you can see everything?
Sandy: I’m doing it right now.
Patrik: Right.
Tara: Maybe you could find out tomorrow how to access that.
Patrik: Yeah.
Tara: Patrik, what would you advise as far as the whole lung transplant avenue? Is that…?
Patrik: Yeah. Once there is a formal diagnosis of lung fibrosis, it’s probably only then when you can pursue it. Patients with ARDS or acute respiratory distress syndrome generally speaking do not end up with a lung transplant.
Tara: Sure.
Patrik: The whole…
Tara: Because they can recover, you’re saying, if it’s not…
Patrik: That’s right.
Tara: Okay. Well, we’ll wait until we get that tomorrow. And then we can have another discussion.
Patrik: Yeah. But in terms of, what I’m worried about she was also talking about the flows are really high. Basically what that means, just to put that in perspective, we talked about that oxygen levels are low. We talked about that he’s on maximum support and she was talking about that the flows for the ECMO are sort of almost maxed out from what I understood.
Tara: Right.
Patrik: What that means is to keep the body supplied with oxygen, they have to increase the flow, which means they’re increasing the flow through the ECMO machine to maximize…
Tara: Yeah. I see.
Patrik: … Oxygen input. Which then might trigger the bleed as well, because there’s more pressure across the board.
Tara: Yeah. That makes sense.
Patrik: Right. There’s certainly many risk factors here but then again, I think the next steps really hinge on that CT scan.
Tara: Yes.
Patrik: And what it also hinges on is, can they maintain his oxygenation by doing what they’re doing without him deteriorating further.
Tara: Right. One thing, do you think it was normal or strange or that they have not given him any steroids or treatment for his lungs since he’s been there. Or is that…
Patrik: It sounds to me…
Tara: I thought that was a little odd.
Patrik: Look. Normally what happens is with the Remdesivir and with the steroids, they’re giving the cause of it. What that means is it’s time limited.
Tara: Oh, okay.
Patrik: It’s time limited. And then they reassess, is it working? Is it not working? If it doesn’t work, usually there’s then other treatment options, one of those options is ECMO, but then there’s other options such as…
Tara: Okay.
Recommended:
Patrik: … And I didn’t ask that such as nebulizer, nitric oxide, there’s other options too.
Tara: Yeah. I thought they were giving him some sort of breathing treatment or something. Did they tell you Sandy? What did they say?
Sandy: They told me that when I asked about the hydrogen peroxide thing. That he was on three different breathing treatments. She never told me what they were and I’ve never heard about them, but that’s just what she told me.
Tara: Yeah. I don’t know. Because yeah, Sandy had asked them about… We had heard about some. A doctor friend had told us about some. She’s more of a natural type doctor, but about hydrogen peroxide breathing treatment, like nebulizing, hydrogen peroxide for long, either pneumonia or fibrosis as well.
Sandy: That was absolutely not an option because it’s not FDA approved or something like that.
Tara: Oh, I see.
Sandy: I don’t know why they are willing to.
Patrik: Say that…
Sandy: But they won’t let me…
Patrik: Say that last…
Sandy: They said, I asked about… What’s that?
Patrik: Say that last part again.
Sandy: When I asked about the hydrogen peroxide nebulizing thing, they said, “That was not an option, it was not FDA approved or something”.
Patrik: Right.
Tara: They said they didn’t, they didn’t offer that treatment or something.
Sandy: They acted like it would do absolutely nothing too.
Patrik: Right.
Sandy: And he was on three different treatments.
Patrik: Right. I’ve not heard of it. It doesn’t, to me like its common, but doesn’t mean… I haven’t come across it.
Sandy: I see.
Patrik: But that doesn’t mean it’s not, it’s not viable.
Sandy: Yeah.
Recommended:
Tara: Yeah. I think it’s… I don’t know. It’s maybe more of something more that…
Sandy: They claim..
Tara: Medicine type ..
Sandy: That’s something you maybe could do pre COVID treatment or something like that.
Patrik: Right.
Tara: I see.
Patrik: Right.
Sandy: But that’s just me. Yeah. All the stuff you read about it sounded good, but I basically, it’s kind of widely accepted treatment.
Patrik: Yeah.
Tara: Sandy, where should we go from here? I guess we’ll wait until tomorrow and see what the scan results come back.
Sandy: Okay.
Patrik: Yeah, I think so. I think…
Tara: And…
Patrik: I think, wait until the scan results come back. The other thing that.
Sandy: Okay.
Patrik: I’m very happy if you wanted to later tonight, your time, we can get on another call with the nurse. If you like, it’s up to you, we can definitely do that.
Sandy: Okay.
Recommended:
Patrik: You just let me know.
Tara: When did they say the results were going to come back from the scan?
Sandy: Sometime tomorrow, I thought she said.
Tara: Ok. And Patrik what is your schedule like?
Patrik: You tell me when you need me and I will make myself available.
Tara: Like today, I didn’t want to call you.
Patrik: No, no, you need to…
Tara: Because it was like the middle of the night, you’re fine.
Patrik: If you need to call me, you call me. And if I can’t make myself available right away, I will make myself available. You tell me, you need me at 11 o’clock tonight, your time. And I can’t make it. I probably can make 11:30. You just reach out to me…
Tara: Okay.
Patrik: … And I’ll work around…
Tara: And would you prefer if I just text you, is that the best way and…
Patrik: Text me, but if it is in the middle of the night for me, you call me because a text won’t wake me up, but the call will wake me up.
Tara: Okay.
Patrik: And now if you need me, you need me.
Sandy: Okay. I appreciate that. Thank you very much.
RECOMMENDED:
Patrik: Oh, pleasure. I wish there would’ve been better news for now, but it’s also important dealing with the facts at hand and…
Tara: Right.
Patrik: Yeah. I guess I’m worried that if he deteriorates further, that would be very dangerous.
Tara: Right.
Sandy: Okay.
Tara: Okay. Well we’ll probably touch base once we get the results…
Patrik: Yup.
Tara: … From the scan tomorrow.
Patrik: Yup. And if you need me before, then please shout out.
Tara: Okay. Sounds good.
Sandy: Thank you.
Tara: All right. Thank you so much.
Patrik: Thank you. Thank you. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!