Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Husband is in a Coma in ICU. Can the Neurologist Best Help Him Improve His Condition?
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Paul as part of my 1:1 consulting and advocacy service! Paul’s dad has COVID in ICU with Tracheostomy. Paul is asking if it will be safe for his dad to go out of ICU quickly after decannulation?
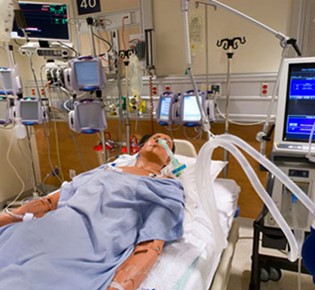
My Dad has COVID in ICU with Tracheostomy. Is it Safe to Get Him Out of ICU Quickly After Decannulation?
Paul: Here, let me turn my phone off real fast.
Patrik: Sure. I’ve done the same. I’ve put it on silent.
RECOMMENDED:
Paul: Okay, great. That should do it. Let me tell you, is it okay if I just start to tell you about my father.
Patrik: Please. Yeah.
Paul: Okay. My dad came down with COVID symptoms. My dad is 79 years old. He was a very active man. He’s not obese. Had no health problems prior to this. He was a smoker for about 20 years. I guess there was some COPD from what the hospital says, but it had never really presented itself. I’m in San Francisco. He lives in Sacramento, but he keeps a vacation condo in New York. So, just a week before he left for New York, because he’s in San Francisco now where I believe he caught COVID. I think he caught it enroute. I was moving furniture and stuff with him, so he’s in really good shape. He’s very trim.
Paul: So, he first came down with COVID symptoms on the fourth. He had difficulty breathing, and his saturation was at about 86, 87, because I gave him an oximeter, because I was worried about and traveling during COVID. So, on the evening of June 6th, he went to the hospital here, St. Seliana in San Francisco. They admitted him. They did a COVID test and admitted him. So, he was put in a COVID section. He was going to be released on the 13th initially without oxygen. So, he was doing real well. I was opposed to that because I was like, “He’s going to be self-isolated. He’s going to need oxygen. You should at least give him some supplemental oxygen in case he needs it.” I’m like, “At least walk him around a little bit so you could see what his stats are.”
Paul: They agreed to discharge him with oxygen. They ordered oxygen. Then approximately about three days later, he started to really go downhill, which is about 10 days from the admission. He was admitted to the ICU. He was desaturating. He needed increasing amounts of oxygen. They put him in the ICU, I think, on an Optiflow mask. He was on that for about three days, but he continued to decline. On June 18th he was intubated. He was pretty stable when he was intubated. I think that there was an accident at the ICU, because they told me that a respiratory therapist had accidentally pulled out his breathing tube, and they re-intubated him. Then later on, they said that it was a self-extubation, which caused me a big concern, because I’m like he was not self-extubated. The ICU nurse told me that it was an accident that was caused by the respiratory therapist. The physical therapist when they were doing some PT.
Patrik: You could find that out by requesting access to the medical records, whether it was self-extubation, or whether it was an accident by the physical therapist.
Paul: In the medical records, it existed as according to the caseworker, it says self-extubated in the medical records, but I remember the nurse told me. You know what I understand accidents happen. Sadly, I’m just afraid that set him back, because he was, at that point, around 92, 93 saturation. I think he was on 10 PEEP of pressure and was about 60%. I mean he was receiving 60% FiO2. After he was re-intubated, he was at 90% FiO2, and up to 12 PEEP. Anyways, he recovered from that. He was pretty stable, and his condition really wasn’t getting better. Maybe it was getting a little bit worse, because then they gave him Remdesivir, the COVID medicine. He was receiving Methylprednisolone via drip and he was also receiving another one. He got that, the last one.
Paul: Those are the new medication that are approved by the FDA here for COVID. They treated the COVID real well, I think. They were going through all protocols. He’s stabilized and he’s been stabilized for quite a while now.
Patrik: Does he have a tracheostomy? Is he still on the ventilator?
Paul: No, he’s had a tracheostomy on July 5th. He was intubated on June 18th. He’s been tracheostomy ever since. He still is on a tracheostomy. He has been testing consistently positive for COVID since that time. Frankly I don’t think they want to transfer him to long-term acute care. That’s why initially had contacted you. Initially, I was really against it, because I felt that he was still COVID positive, but even though he’s still testing positive. He just got a test back today it was positive. The test before that was rejected. The test before that was positive. The test before that was rejected, and the test before that was negative.
Paul: When I say rejected it was considered non-viable. Either way he’s still testing positive. He has been off the ventilator and on Optiflow on the cuff pretty consistently since 6 AM yesterday.
Patrik: Okay. So, it’s the longest time he’s been off the ventilator.
Paul: Yeah, and has a Passy-Muir.
Patrik: Passy-Muir.
Paul: So, he can speak. So, I’ve been speaking to him regularly.
Patrik: Great.
RECOMMENDED:
Paul: He has a strong voice. He’s able to walk a little bit. Actually, they had to move room because they had to do some maintenance on one of the rooms in the hospital. He walked about 150 feet today, and he walked about 150 feet yesterday.
Patrik: That’s great.
Paul: Yeah, he’s improving. He’s currently on 60% oxygen with 40 liters of pressure through the cuff. He has significant secretions. That’s causing some problems because, it clogs the tracheostomy. Before that they were putting him on CPAP mode at night and doing the Optiflow in the day, but they just moved him, 24 hour Optiflow now.
Patrik: That’s great.
Paul: He was on CPAP mode on the ventilator. Last time he was a 50% FiO2 with 5 PEEP per pressure. He’s getting better. He’s recovering. He doesn’t have any fever. He’s not on any type of medications other than Lexapro for depression Pepcid. He has an NG tube as well. He’s had an NG tube pretty consistently, because no surgeon will do a PEG while he tests COVID positive. They can’t find a surgeon to do it.
Patrik: Would you like a PEG? Would he like a PEG?
Paul: I don’t know. I would like whatever is in his best interest.
Patrik: I think you’re pretty safe with a nasogastric tube.
Paul: Okay, so that’s not an issue.
Patrik: I think you’re pretty safe.
Paul: My main concern here is that I don’t really feel that they’re working towards decannulation. It’s an ICU, so they want to keep him medically stable for transfer over to the LTAC where he’s no longer really a problem. He’s not getting regular therapy sessions. He sees a speech therapist maybe twice a week, a physical therapist twice a week. I don’t think he’s seen an occupational therapist. He only sees a doctor about once a week, an actual physician.
Patrik: In ICU?
Paul: Yes, and it’s pretty terrible. The nurses are pretty good and competent. I like the nurses generally speaking, but when I asked them what’s the plan. They say, “Oh, well the plan is to transfer them over to this other facility.” I mean, I pretty much understand they’re trying to. They don’t want to move him. At this point he seems like he’s in pretty good shape to decannulate. I don’t really know. I’ve had no experience with any of this.
Paul: No, my dad said the last time he saw the actual physician was about a week ago. I’ve only spoken to the physicians, and I’ve left constant messages maybe six times since June, since he was admitted to the ICU. They don’t contact me. I leave messages. I have no idea what the plan is.
Patrik: That’s terrible. You can’t visit. No visitors.
Paul: Yeah, it’s no visitors.
Patrik: FaceTime?
Paul: I can FaceTime him yeah.
Patrik: Okay.
Paul: Go ahead. I’m sorry.
Patrik: You can FaceTime the nurses, but not the doctors.
Paul: I can’t FaceTime the nurses, but I can speak to them on the phone. I mean, when they’re in my dad’s room. The nurses are very communicative. They do call me back, or they answer the phone. I mean, occasionally they don’t call me back, then I just call back and then they pick up. They’re super busy.
Paul: I actually called the physician. They won’t give me an email address, or an extension for the physician. I actually called the respiratory therapy department of the hospital, I explained it to the nurse, asked to leave a message to the pulmonologist. The pulmonologist I got the afterhours answering service. I explained it. I just said I want to leave a message to the answering service, but she felt bad given that my dad was a COVID case. She actually called the physician. He wouldn’t take a message. He specifically said for me to ask the nurses. He wouldn’t even take my phone number. It was honestly really horrible.
Paul: As much as I was hesitant to have him go to the LTAC, I think he would be getting better care there than he does at the ICU.
Patrik: Yeah.
Paul: They told me today that they were going to do a radiology, take him to the radiology department to put some Blue Dye in to test swallow function, but they didn’t want to do it, because there was no way that they could transport him with the oxygen. They scheduled it for next week.
Patrik: Okay, but on that note, now that you’re telling me they’re doing the Blue Dye Test, that is definitely a step towards the decannulation.
Paul: It is, okay.
Patrik: It is a step. That’s good. That is a good sign.
Patrik: Can I just quickly sum up what I’m hearing from you so far?
Paul: Yes.
Patrik: I do believe that if your dad can stay off the ventilator for the next 48 to 72 hours, and his secretions, or he can clear his airway, he can clear his own secretions, and the speech therapy assessment, and the Blue Dye Test is positive, I would say he can be decannulated. Now the question for me is if they can decannulate him, would he need to go to LTAC? I would say, no he doesn’t need to. The question is, how quickly can they move him towards decannulation that’s the question. If they’re doing the Blue Dye Test, that’s one of the tests that needs to happen. Have you spoken to speech therapy? Do you have any access to them?
RECOMMENDED:
Paul: I think so. Yeah, I’ve spoken to them a couple of times when he was in the room, because when they put the Passy-Muir valve in, I talked to them, because my dad called me right away and they were there. He’s been having that in about 16 hours a day. They take it out when he goes to sleep at night.
Patrik: Great.
Paul: His voice is strong. The secretions are an issue when he goes to sleep. Tonight was the first night that he was on Optiflow overnight, or last night I should say. The nurse had to come in twice and clear secretions from the actual valve, but he’s able to clear secretions with the suction in his mouth.
Patrik: So, you’re saying the nurse needed to suction twice overnight?
Paul: Yes.
Patrik: So, if you were telling me she needed to suction twice an hour, then I would say to you I would be concerned about decannulation. If he needed suction from the nurse twice overnight, I think he’s heading in the right direction.
Paul: Okay. I think it maybe because he’s lying prone. So, I suggested maybe he lays up a little bit in a recliner, because he says he doesn’t have the issue in the daytime, and I’m like, “Well, you’re clearing your secretions with the suction in the day, they accumulate overnight, and this is the first night, so.
Patrik: Exactly. So, this is the first night. He needs suction twice. If it was the first night and he needed suction 10 times, I’d say, “Okay, well it’s the first night.” Given that it’s the first night, I think that sounds very encouraging, Paul, it sounds very encouraging to me.
Patrik: I’ll tell you what my biggest concern is from everything that you’ve shared so far is that he’s still on 40% of oxygen. That’s probably my biggest concern.
Paul: 60%.
Patrik: 60%?
Paul: 40 liters.
Patrik: Yeah, that’s probably my biggest concern.
Paul: Okay. He is saturating last night. He was at 99%.
Patrik: On 60%.
Paul: Yeah, and I said that they should lower it. Well, I didn’t say it, but I asked, “Do you think maybe it might be lowered?” They said, “Well, we just want to give his lungs the ability to rest.” He was at 50% when he was, two nights ago, on the ventilator when he is in CPAP mode.
Patrik: Okay. Paul, do you know if they’re checking regular arterial blood gases? Do you know what I mean by that?
Paul: I do. They’re taking it three times or twice a week. Two or three times a week.
Patrik: So, do you know if they’ve done one since he’s come off the ventilator?
Paul: I don’t know, no.
Patrik: I guess that will be the crux really. It’s great that he’s saturating 99%, but he CO2 might be high, especially if it’s got an underlying history of COPD. I think the next step really is for them to do an arterial blood gas to check the CO2 in particular, especially since he’s now lost the PEEP. He’s had a PEEP of 5 on the CPAP. When people lose the PEEP, they can also increase their CO2. That’s really sort of the point where people either, it’s the make or break point really. It’s either they can manage their CO2 or they can’t. Even if they can’t, it’s not the end of the world. They might need a little bit more PEEP for a few more days, but also they might need physical therapy.
Patrik: The other concern is he’s only got physical therapy twice a week you said. I mean, he’s walking, that’s great.
Paul: The nurse gets him up, and walks him to the. He sits in the chair, and they walk him around a little bit. So, he gets a little bit of exercise every night, going from the bed to the chair. I mean, I’ll tell you how bad it is though, Patrik. I actually had to buy my dad weights at the sporting goods store, because he didn’t have any. They wouldn’t give him a squeeze ball. So, I got some one pound weights and a squeeze ball. I think that nobody really. They don’t want to be doing physical therapy in the ICU. Plus, because he’s COVID positive. They don’t want to.
Patrik: Sorry, I didn’t hear the last part, Paul.
Paul: I think that physical therapy doesn’t want to work with him very much, because of his COVID status.
Patrik: Sure, but I mean he’s gone a long way. Let me ask you something else Paul, do you know whether he had ARDS? Do you know what I mean by ARDS, A-R-D-S?
RECOMMENDED:
Paul: He did. He was, yeah. I heard in one of the reports that he had respiratory failure, and then another time they referred to ARDS.
Patrik: I mean, that sounds amazing in terms of recovery. He’s been struck by what other COVID patients have been struck with, and as the mortality rate for COVID is pretty high. I mean, just by what you’re sharing he’s done incredibly well. He’s done incredibly well. If he is now managing the Passy-Muir of 16 hours a day, that’s incredible. That’s incredible. I would say everything that you’ve shared is very encouraging, given where he started, very encouraging. We have so many inquiries at the moment, especially with the COVID and quite frankly we have a lot of inquiries when patients have ARDS and a lot of them don’t make it.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!