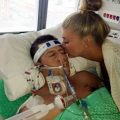
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Family Meetings in Intensive Care, Avoiding the Pitfalls and How to Be in Control! Live stream!
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Eric, as part of my 1:1 consulting and advocacy service! Eric’s dad is with a breathing tube and is on a ventilator. Eric is asking how prone positioning can help his dad with pneumonia recover in the ICU.
How Does Prone Positioning Help my Dad with Pneumonia Recover in the ICU?
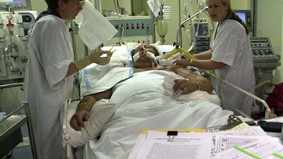
Nurse: Hello.
Eric: Oh, hello. It’s Eric, and I’m Mr. Corr’s son. He has pneumonia and he’s on a ventilator. Would we have time to have a little chat with you or with one of the nurses? And we’ve got a friend to the family, and he’s on the telephone as well, with me. His name is Patrik and he’s really supporting me, because he’s a critical care nurse. So he’s right here, just helping me out with all the jargon and stuff. Would there be time to speak to anybody, or would we need to call later?
Nurse: It’s okay but I am not the nurse for your dad so I cannot tell you much about your dad’s current condition right now.
Eric: Yeah, that’s not a problem.
Nurse: Okay. I’ll just get the nurse who’s taking care of your dad.
Eric: Oh, thank you.
Patrik: I could barely hear what he was saying, so I hope the line with that other nurse will be better.
Eric: Yeah. What he was saying: they can’t really tell us too much.
RECOMMENDED:
Patrik: Oh, look. I wouldn’t be too worried about it for now. Let’s just get this nurse on the phone, and I hope I can get some information from the nurse. Let’s just try that.
Eric: Yeah.
Patrik: And if the nurse is experienced and cooperative, of course, I’m sure we’ll get some answers. So let’s not try and over-complicate, and let’s not worry about what this other nurse just said now. Let’s just get the bedside nurse on the phone, and let’s see whether they are experienced and cooperative.
Eric: Yes. Thank you.
Patrik: And when was the last time you have seen him?
Eric: It was yesterday. It was about 8:00 at night, and we said night-night to him. And he was in prone position. But they’ve turned him up this morning, apparently.
Patrik: So he was in a prone position, was he?
Eric: Yes.
Patrik: For the first time?
Eric: I think they tried before, but I think they struggled. And so, yeah.
Patrik: Right. Just to remind me, how many days has he been in ICU, now, for?
Eric: 14 days.
Patrik: 14 days. And yesterday you think was the first day they were, or the second time they were proning?
Eric: Yeah. I think.
Patrik: Yeah.
Eric: And so I remember the nurses are telling me a few days ago they tried to prone him, and they couldn’t do it, and he struggled.
Patrik: Yeah. It can be very uncomfortable. Can be very uncomfortable.
Eric: Yeah. Because he has that feeding tube in. And so I think that doesn’t help enough to prone him appropriately.
Patrik: Yeah, absolutely. And also, when they prone, they put people not only on their tummy, they also put them head-down.
Recommended:
Eric: Yeah.
Nurse: Hello.
Eric: Oh here’s the nurse. Oh. Hello.
Nurse: Hello.
Eric: Yeah. I was just wondering how Dad was doing. My friend’s on the phone as well. He’s supporting me. He’s a friend of the family.
Nurse: Okay.
Eric: And he’s a critical care nurse, so he’s quite good at helping me with the jargon and stuff.
Nurse: Okay, yeah. No problem.
Eric: But please can you tell me how he’s getting on today?
Nurse: Oh, it was the same typical day for him.
Eric: Yes.
Nurse: Yes, because he is still on a ventilator and we have tried proning him within the day so that his oxygenation may improve, but we have to put him back up because he cannot tolerate it.
Eric: Yeah.
Nurse: And then he requires a lot of oxygen because his oxygen saturation decreased after that.
Patrik: When you’re… Hi. Sorry. My name is Patrik. How are you?
Nurse: Hi. I’m all right, thanks.
Patrik: When you’re saying he’s on a lot of oxygen, what are we talking about? 100%?
Nurse: We’re on 90% at the moment.
Patrik: 90%. And is he proned now?
Nurse: Not at the moment, no. As I was saying, he was being proned then was put back at 9:00 this morning.
Patrik: Right. And his blood gases are poor? Or…
Nurse: There’s issues with his blood gases but we are doing something about it.
Patrik: Okay. That’s great. And is he needing any vasopressors? Any inotropes?
Nurse: He is, yeah. So he’s on a couple of different ones. But we’re just giving him adrenaline at the moment.
Patrik: Right, I see. And the kidneys are working?
Suggested links:
Nurse: I’ve not looked through the lab results myself. Hang on, let me just check. Seeing through his labs, there seems to be no problem with his kidneys and he is passing a good amount of urine as of this moment.
Patrik: Right. Okay. And so you’re not giving any Lasix at the moment, to offload fluids.
Nurse: No. We’re not.
Patrik: Oh, that’s great. And he’s absorbing feeds?
Nurse: He is, yes.
Patrik: That’s great.
Nurse: Yup
Patrik: That’s great. And the other blood results, pathology is fine? Or, white cell counts would probably be very high?
Nurse: Oh, yeah. Yeah. I believe it’s okay. But I couldn’t tell, really. I haven’t had the chance to check the other blood works.
Patrik: Sure. Sure.
Nurse: And so, yep.
Patrik: And is he having a temperature?
Nurse: Nope, it’s about 97.5F.
Patrik: Right. Okay. So it’s predominantly the lungs that are not working at the moment, then?
Nurse: Yeah. It is. That was his main issue.
Patrik: Right. And is there any plan to prone again, or?
Nurse: Not at the moment, no.
Patrik: Right.
Nurse: That’s not the priority for now I believe.
Patrik: Right. And he’s on antibiotics for the infection?
Nurse: He is, yes.
Patrik: Right, I see. He hasn’t been diagnosed with ARDS. Just the pneumonia? Or has he been diagnosed with ARDS?
Suggested links:
Nurse: I believe it’s just the pneumonia. Yeah, just the pneumonia.
Patrik: Right, okay. Hopefully the FiO2 (fraction of inspired oxygen) can come down at some point.
Nurse: Yeah. That’s what we target too. We’re trying to wean the FiO2 down if possible.
Patrik: Yep, sure. And does he have a lot of secretions on his chest?
Nurse: Nope. He does not have too much of the secretions as of the moment. But there are times he will have increased secretions that we really need to suction him every now and then.
Patrik: Right. And is he heavily sedated, or just lightly sedated?
Nurse: He is. Yeah, he’s heavily sedated.
Patrik: Right. Like you’re giving midazolam or propofol?
Nurse: We’re giving him the fentanyl.
Patrik: Right. And then propofol or midazolam? Or…
Nurse: Yes, yeah.
Patrik: Right, okay. Fair enough. But he’s not paralyzed.
Nurse: No, he does not need to be paralyzed and he is comfortable as well while on his current sedations this time.
Patrik: Right. And if you’re not paralyzing him, will he breathe against the ventilator?
Suggested links:
Nurse: Yeah. I think there are episodes wherein he will do that.
Patrik: Right.
Patrik: Okay. Well, thank you so much for all the information and for taking care of him.
Nurse: Oh, you’re very welcome.
Patrik: Thank you so much.
Eric: Yeah, thank you, yeah. You’re working really hard.
Nurse: Thank you.
Patrik: Thank you. Really appreciate it. Eric, I don’t have any other questions. If you…
Eric: Yeah.
Patrik: I don’t know whether you wanted to ask anything else?
Eric: Do you know when… I think the consultant wanted to do a CT scan. Did he manage to get one done for him? Because I know, when he was awake, it was really hard to do.
Nurse: I have not been informed of a CT scan, but I can check if there is one.
Eric: Yeah.
Nurse: But, there’s no significant findings in the CT scan. But obviously that can change. We still need to have the official result coming from the doctors.
Eric: Yeah. Oh, that’s understandable, yeah. Thank you.
Nurse: Oh, you’re welcome. They might want to leave him here in the ICU for a couple more days, just to kind of see how he does. And if the oxygen still looks a bit low, they can defer / delay transfers until he is stable enough for transfer, and that kind of thing.
Eric: Yeah.
Suggested links:
Nurse: All right.
Eric: Yeah. Well, thank you. Thanks a lot.
Nurse: Oh, you’re welcome. Yeah, we’re here all night, all day, so just ring me if you’ve got any problems, any concerns, or you’ve just got a question for the nurses that are in. All right.
Eric: Oh, thank you.
Nurse: Yeah.
RECOMMENDED:
Eric: Do you think they’ll let us come and see him again soon?
Nurse: I’m really not so sure about that. I think at the moment, from what I’ve heard, it’s still not possible.
Eric: Okay. Would you tell my dad night-night? Would you tell him night-night?
Nurse: Oh, okay. I will do that. What was your name, honey? I forgot to ask it.
Eric: Eric. It’s his son.
Nurse: Oh, yeah.
Eric: And so I’m next of kin. Yeah.
Nurse: Yeah. Yeah. I’ll let him know that you phoned in your nurse, and that you phoned good night.
Eric: Yeah. Oh, thank you for your time.
Nurse: You’re very welcome.
Patrik: Thank you so much.
Nurse: Okay.
Patrik: Have a good shift. Thank you so much. Bye. Bye.
Nurse: Bye. Good night. Have a good night.
Eric: Yeah. Will do. Bye.
Nurse: Thanks. And goodbye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!