Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
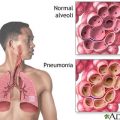
Will My Dad in ICU Benefit More From A Tracheostomy Instead of A Breathing Tube?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Irene, as part of my 1:1 consulting and advocacy service! Irene’s dad is in ICU on a ventilator and shows good improvement. Irene is asking why the ICU team is pessimistic about his dad’s prognosis.
My Dad’s Condition in ICU Improves But Why is the ICU Team Pessimistic About His Prognosis?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Irene here.”
Irene: Yeah. So, but you can get the settings from the nurse. She just has to look harder, she just has to look harder because it’s not her specialty.
Patrik: I don’t get that. Yeah, sure. I don’t get how an ICU nurse doesn’t want to know about ventilation, but yeah. I’m not going there.
Irene: Yeah, I know.
Patrik: Okay. Okay, Irene, look, you’re happy with that. I’ll call you tomorrow at noon, 12 o’clock your time.
Irene: Okay.
Patrik: Okay. Thank you so much. And we’ll talk tomorrow.
Irene: Yes Sir.
Patrik: Thanks Irene. Bye. Bye.
RECOMMENDED:
Patrik: Hi, Irene, how are you?
Irene: Good, Patrik. How are you doing? Nice to see you.
Patrik: Can you hear me? Can you see me?
Irene: Yes, I can see you.
Patrik: How are you doing?
Irene: Pretty busy, trying to figure things out. I’ve been getting updates and stuff today from the hospital and that kind of thing you know.
Patrik: Yep. And are you contented?-
Irene: Made some contact…
Patrik: Right. Are you contented with what you’re hearing?
Irene: Well, not so much from the nurses that work with my dad. They’re on the pessimistic side. You know, they’re not very optimistic about my dad’s prognosis. They say one thing, what they heard from the neurologist. And I tell them, “That’s not what I heard from the neurologist,” and you know, that kind of thing. And then they kind of get on me a little bit. “Oh, you know, that they were trying to get you to agree to take care of your dad in this sort of way. And you were not available the other day and what happened there?” So they’re trying to, you know, make me look like I’m not deciding the right things at the right time, kind of thing.
Recommended:
Patrik: Right. I’m just reading through your email. I mean, if there’s no brain damage, there shouldn’t be an issue in the extubation of your dad if he can breathe. The question is, so last time when you showed me the Zoom video, when we saw your father on Zoom, would you say that things have improved?
Irene: Yes. And when you saw him, he was more sleeping. We didn’t see him when I actually was asking questions of the nurse, how my father’s body felt. If it felt limp or if there’s some muscle tone, when they moved him, when they lifted him and arranged him in the bed, did he move his arms and legs? And the nurses say, “Yes he does.” But he’s still not quite there on all of it. So he lifted up one of his arms like this and the arm just kind of went down like that, but it didn’t drop down a lot. It just kind of went down. Like, my dad kind of controlled it a little bit. And then after he did that, my father woke up and was watching the nurse and watching me. And the nurse moved the other side of the bed.
Irene: My father turned his head a little bit, followed the nurse with their eyes. And then I was on this side talking on the… They have these little laptops that they have there and they’re portable. And they brought it right next to him, flat on this side of my dad and the bed’s right here. And the nurse’s over here talking across my dad’s face and across his body to me. And I’m talking back across, and my dad’s just kind of turning, looking at me with his eyes. Turning, looking at the nurse with his eyes, turning, and looking at me.
Irene: So I think he recognized me. He recognized me and he spent some time… His eyes were pretty much open all the way. I’d say about almost seven eighths of the way, maybe three fourths of the way open, a little bit more. And he was kind of watching me talking, and I was waving and doing things like that. Today was a little different. He was more sleepy, but I was in there for quite some time, for a couple hours. And every now and then I’d say, “Hi, dad, how are you doing?” And I kind of whistled, or give him a little high hoots and noises. And he would open his eyes, kind of looked at me a little bit, and then kind of doze off back to sleep. Half an hour later, I do the same thing. And there was time when he opened his eyes completely as I was talking, and then turned his face towards the screen again. Just a little bit today, not as much as yesterday. Yesterday, they did a lot more physiotherapy, today they didn’t do any physiotherapy…
Patrik: Oh, good. Good. Irene, you say in your email, he’s close to extubation. Can you quantify that? Or qualify that.
Irene: Well, based on the neurologic assessment mainly, and also the fact that they were saying that he’s breathing on his own. But today I got a different report from the nurse saying he’s not breathing on his own. And I said, “Well all the reports I have are saying that he initiates his breath and he breathes, but breathes shallow.” So I quantify it by on his neurologic, there’s a medicine called Zolpidem.
Irene: It’s a medicine that you can wake people up with that are, you know, hypoxic brain injury. I was going to ask them, Ambien is another name. You know, for people who wake up from sleeping. And I guess that there’s been quite a bit of studies about waking people up on this medicine or, there’s some good results. And the other thing I quantify it by is, a neuro doctor also said, again, that the MRI that he ran on last week, he just ran an MRI, like, 24 hours ago. The MRI that was ran was a better MRI because my dad didn’t have any artifacts. He wasn’t moving. It was a very good MRI and it showed no difference from pre-hospitalization MRIs or the other previous MRIs on his brain. So it didn’t show any brain injury or damage on the brain MRI.
Irene: So that’s from a neurologic standpoint. But he still prefaced it by saying, “Well, that still doesn’t mean that he hasn’t gotten any hypoxic brain injury. You know, we don’t really know, but it’s a negative finding. The brain MRI is negative.” So, and I always told these doctors, I said, “You’re not going to find anything on my dad’s CT or MRI of the brain.” They always worry that they’re going to find something and they never do, because he’s just more sleepy and somnolent and quiet. And they think something mentally is off. So they’ll buy a brain MRI and find nothing.
Patrik: Yeah. And just because the brain MRI is negative, he still needs to show signs of waking up. He still needs to breathe by himself. So there are many boxes that need to be ticked before he can be extubated. I would almost argue the brain MRI being negative is probably last on the list, because if he was obeying commands, and I know that’s the language barrier, I get that. But if someone can get him to obey simple commands, like squeezing fingers, raising up his hand or whatever it is, right? That would show that the brain is intact. That would eliminate the need of an MRI scan. However, a negative MRI scan increases the chance that he will wake up.
Irene: Yes, yes.
Suggested links:
Patrik: Right? What do you expect for the coming meetings?
Irene: Well, we’re having a brand new set of doctors. And one of the doctors that’s going to be there is his neurologist that he normally sees before the hospital. So he knows him. So he’s going to be his neurologist and I’ve had pretty good relations with him. And we get a lot of things accomplished with my father and he follows my dad in and out of hospital. So that’s a good sign that we have him. But I think what I’m trying to get out of the meeting is, if in fact he has some kind of neurologic issue with the brain and we need to work on healing the brain. Like, if they have inconclusive images, then we need to do things like a PET scan and SPECT scan. We need to do these other scans.
Irene: Because the MRI, CT is not a catch-all. And also try some medications out on him and try to wake him up. Why not? Why not give him Ambien? You know, it says it works with hypoxic brain injury, and people can wake up pretty abruptly from that. Why not give him a full chance to cure the underlying issue that he has right now, which is he’s not really responsive too well. But if we just keep going forward, leaving the brain unattended to, that’s not going to help him down the road anyway. If he leaves the hospital, who’s going to tend to that? So I think we need to focus on if that’s number one priority… And the nurse said that. He went and he showed me the whole body and the breathing.
Irene: He says, “We have nothing here wrong with the breathing. We have nothing wrong here with the heart. We have nothing wrong here with any other parts of the body,” except maybe he does have a blood test that came up showing that his brain is releasing a high level of peptides right now, which usually symbolizes a problem with heart failure. But that number apparently, it’s the BNP number. That number apparently trends down just like the Troponin has been trending down. Well, maybe it will trend down. The brain releases that peptide chemical, the brain naturopathic peptides. So with that said, yeah, I think we need to cure the underlying problem the best we can. To give him a chance to wake up, to get him a chance to wean. But if we just go into tracheostomy and then, they’re going to put him on a different floor. And it’s not the ICU, which will give him a better sleep pattern, it’s going to have dark hours, light hours. And that’s where all the trache patients are in the hospital. And they’re going to monitor him away from the busy unfriendly area that ICUs really are. All the bells and whistles.
Recommended:
Patrik: Yeah, I agree.
Irene: So that’s a positive thing. But at the same token, we have a cardiac doctor who I spoke to finally. He’s also my dad’s clinical cardiologist, he was on his team this last week. I’m not sure if he’s going to be on the team next week, but my dad has two cardiologists. He has this one that he’s seen a couple of times. The other one was a female doctor. And those two cardiac doctors are going to talk. But the one that spoke to me recently said, you know what? I’m thinking about doing a pacemaker to your dad, but now I’m not so much thinking that he needs it, because his heart functions pretty well. And I’m also thinking that the issue that happened to the heart was not a primary heart attack with the heart being bad. It was the lung spilling up and putting stress on the heart, because it wasn’t getting enough oxygen. And you know, the relationship between the lungs and the heart failed.
Irene: So the body turned blue, it went hypoxic and the heart wasn’t getting enough oxygen and Troponin leaked and went really high. And the heart stopped for, went on arrest for a while and he had very low or no pulse for a while. So that’s basically how it was explained. It wasn’t a primary heart attack. So with that said, he said, “You know, I’m not sure if we’re going to do a pacemaker, but one of the reasons why I don’t want to do anything right now is I don’t want to aggravate or insult his body with another invasive procedure that’s going to sedate him and have him at his age, come out of sedation. And it’s just going to put his brain function backwards in time to recover even further.”
Recommended:
Irene: So in that day when, they were talking about… And I didn’t get a chance to tell him about the things that the ICU wants to do, but what they want to do, these two invasive procedures, like cutting a hole in the throat and putting in the trache, and putting in G -tube in the stomach. Those are both going to require some sedation. So his brain activity, once again, a few steps backwards before we start moving forward. If we move forward at all, to come out of that scenario. So the doctor really wants to avoid sedation, but now they’re pushing on to do the trache.
Irene: So my thought is one, let’s try to heal the brain. Let’s try to get the brain awake the most that we can and see if he could come out of his stupor and out of his twilight of being comatose or getting better. Because he is awake, he is responsive. You know, he’s been very responsive the last two days with me. And we made inroads that dad is waking up now. Now we go a step back and we sedate him, he’s going to go back into a comatose situation, and once again have to come out and heal all these invasive procedures. And then at that point, might be even pressured to remove him off the trache floor and into another facility long-term. Which make their decision to move him out of the hospital easier, if his brain is even less responsive or less awake down the road, after these procedures. So that’s the other concern I have too.
Patrik: Right. I see. And let me ask you this. Do you know if he has… How long has he been off sedation for, do you know?
Irene: About a week or so now? I don’t know the exact day. I think it was day six or so. They were starting to wean him off of a sedation and they were trying to not have any of it on him. Let his brain, and then, he finally woke up on day 13, day 14. It took him, I’d say, 12 to 13 days just to wake up from sedation.
Recommended:
Patrik: Absolutely.
Irene: So if we sedate him again, we’re going to be taking another two weeks backwards before he wakes up again.
Patrik: Look, if they do a trache and the PEG it’ll be short term. Yes, he needs sedation, but it’ll be minimal and it’ll be quick. So it won’t be as much as being in a prolonged induced coma. But wherever you can avoid it, avoid it. But I tell you the missing links for me. The missing links for me is I still don’t know what ventilation setting he’s on today or yesterday, and the missing link to me is someone needs to talk him in such a way that he would understand. Like, ask him what he needs to do once that tube comes out. Somebody needs to talk him through. He needs to breathe. He needs to cough, because that is something that I believe would be very advantageous.
Irene: Yeah. But he’s way too sleepy now to do that. That’s the problem.
Patrik: Yeah. So at the time, if he’s not waking up, time is working against him.
Irene: Yeah.
Patrik: Do you have access to the medical records? Don’t you?
Irene: No, not yet. I don’t.
Patrik: Oh, okay. All right.
RECOMMENDED:
Irene: It’ll take a month for them to mail it to me and the hospital still hasn’t, I still don’t know what the records… Matter of fact, the cardiac doctor who is making rounds, he had questions about the heart attacks. It’s unclear to him what happened when and how it happened. He knows it happened when he was first on that floor, but it’s not clear how much did he vomit and aspirate, or was this the purely an oxygen starvation problem at the beginning. And then there was another one when he was in the ICU. And apparently there was another one when they intubated him as well. So it’s unclear, there’s like three of them. It’s not clear, it’s unclear. And then there’s also another story. Something happened when they were trying to take him down to the MRI room.
Irene: Something happened with the heart. So I know there’s at least three, but I haven’t seen the record. But when I complained to the insurance company… So one nice thing about me complaining to them about a hospital trying to push for a relative, a loved one out too soon, early discharge, you don’t think they’re ready to be discharged, you can complain. And it’s a real quick process. Within 24, 48 hours, you get the response. And what happens during that 24, 48 hours is they get a doctor. The government does, to get all the medical records electronically over to the government. And the government has a doctor that reviews the whole record and then contacts the hospital and asks them, why are you trying to send a patient out? He’s still on life support.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!