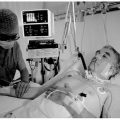
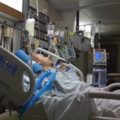
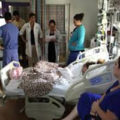
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Mikaela, as part of my 1:1 consulting and advocacy service! Mikaela’s sister is with a tracheostomy in the ICU and is now off the ventilator. Mikaela is asking how she can stay positive amidst negative reports from doctors about her loved one’s condition in the ICU.
How to Stay Positive Amidst Negative Reports From Doctors About my Loved One’s Condition in the ICU?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Mikaela here.”
Dr. Rich: It’s a philosophical thing about what it means to be human, and what it means to be… What brings meaning to your life, what brings quality to your life, and we ask very profound questions about that. And actually, it’s the same experience from 16 years. I’m not sure I’ve still got my head completely around it, but I’ve got a lot of experience of doing it. And it takes families a long time to really understand it. You’ve got to live and breathe it for a while, and you’ve got to see it. And COVID has made it more difficult because of the amount of time you can spend with your loved one. I think you need family time really. So in your loved one’s situation now, when you think about it, and then you think about it the next day and you have a slightly different take on it, and it just takes time to understand it and to get your head around it, really. I just hope that your ideas about what’s right and wrong for her will crystallize, I think, with time. That’s what I think.
Mikaela: That’s all we ask, really.
Dr. Rich: I think we’ll probably be… I’ll give a bit of time, and really..
Mikaela: Understand.
Dr. Rich: Understand and know what the right thing to do is. Of course, it’s already been a bit bleak, it’s a horrible situation.
Mikaela: Well, it’s not really in that sense. You’ve explained it quite clearly and it was good, I’d say.
Dr. Rich: From my point of view, because I must say, I’m a rehab person, but most of what I do is trying to get people’s independence back. And at the moment, I don’t think she’s very likely to have options because of the medical complications along the way. So actually, I can give you a very bleak picture of things, but I’ll tell you what we can do, what we do in this situation, and how we bring some measurements, some actual objective measurements into the situation. At the moment, it’s just trying to really be crystal clear on where we are on that, and what kind of things are changing, and share with you some of the tools that we use. I think I’m going around in circles a bit here.
RECOMMENDED:
Mikaela: No, no.
Dr. Rich: I feel like I’ve also spoken a lot, and I’ve not done much listening, so.
Mikaela: No, no. It’s been quite back and forth, so it’s been okay, I think. You know with the Glasgow coma scale? There are times where it’s been sometimes 7 or 8, as well, from what the nurse has mentioned. As high as 7. Probably never an 8, was it? It was probably a 7 more than that.
Dr. Rich: Yes, Glasgow coma scale for her varies. That’s what I think, so… Yes, but they probably just gave a higher score..
Mikaela: Yeah, it’s probably be a 7 or 8 here and there, perhaps, but it’s not consistent enough. I think that’s the problem, isn’t it?
Dr. Rich: Yes. The Glasgow coma score tool just doesn’t work in this situation, it’s not what it’s designed for. It’s designed for the prognostication in the very early phases of head injury.
Dr. Rich: Like, the next day, she’d be fast asleep and she’d score 3 points lower. That’s all that were measuring.
Mikaela: For you guys, obviously, it’s more long-term, isn’t it?
Rinzzie: Yes, we tend not to use the GCS scale and break it down to the visual, the auditory, tactile, motor function, those kind of things.
Mikaela: Right, okay. Yes. So, it includes things like motor and the state, and stuff like that.
Rinzzie: Yes.
Mikaela: But it’s just more of..
Rinzzie: It’s just more in-depth.
Mikaela: Yes.
Rinzzie: Yes, more in-depth. It looks at all the really intricate details of somebody’s consciousness.
Mikaela: Right, okay. I see.
Dr. Rich: There are a range of tools we can use.
Rinzzie: There are, yes. There’s a range of tools, yes. I think the tool we would choose would depend on what she could tolerate, and what is going to fit best with her. So, some of them are predominantly used in patients who have more traumatic brain injuries. The one we’re using with her at the moment is called the coma recovery scale, and so, that’s… It’s an in-depth assessment which looks at all the different areas. So, for example, if it is true that your sister has a visual impairment that she can’t see, that we’re not just relying on that visual information. We’re not just relying on that as the assessment. It’s really, really common for patients with head injury not to have good vision, so with coma, a lot of the assessments rely on vision, so we’re using things like sound, and touch, and those kind of things. Seeing whether just that gives a different level of response, and we look at all those different levels that I mentioned earlier to see, does she do the things that respond to that level? And that’s done over a period of time to see whether, is there any subtle changes?
Recommended:
Rinzzie: There’s an actual score at the end, so at the moment she’s scoring between a 3 and a 4. The maximum score is 23, but she’s got to do quite a lot to jump to that next stage. On another day, I can talk you through it, and we can go through the kind of things that we’re doing. Not today, but I’ll come back to you again maybe in a little while.
Mikaela: Okay. Yes, that’d be good.
Rinzzie: Yes, and even things like observing you on calls and things like that, I can do that to see whether there is any difference with your sister if you do things to her as part of the assessment?
Mikaela: Okay, yes. yes.
Dr. Rich: Part of the assessment is actually just sitting silently and watching what she does.
Rinzzie: It is, yes.
Dr. Rich: That’s part of it. Because then, you pick out all the stuff that is just automatic behaviors, and then you almost take that away, “Oh, we saw that again when we did this, but she’s doing it without that, as well,” so obviously, we can take that away.
Rinzzie: I do, I do. I’ve spent a lot of time sitting watching her, yes.
Dr. Rich: Spontaneous.
Joseph: The first week when I was coming in, I’d lift her lids up, and speak to her. She did actually respond in the sense. I don’t know, she kept her eyes open. That was the first week, and then, when I didn’t speak to her, and she had her lids open, I just spoke to her because I was really upset, and she actually cried. So, I don’t know whether there was just tears on her eye or she was actually crying.
Rinzzie: Yes, I can’t say for sure, but… What I would say is, our body can do a lot of things automatically. I don’t know if that was a meaningful response or not, but just so you know, the thought which is, without processing something, without being aware, you can do that. You can cry, you can smile, you can scream. Just some of these things… And it’s really… And it… It’s really awful as a family member, because you’re looking for that. You’re looking for that something, and then we say, “Well, actually, that’s just automatic.”
Suggested links:
Dr. Rich: That is something that happened usually. Different people are doing different things. Some behavior that’s just automatic. It wasn’t a response. They certainly can, but it’s really… It’s hard to observe that she is doing that any more. Talking to her, and it’s not when we’re talking to her, or just when we’re… She doesn’t know we’re watching, but we are. And that’s exactly the kind of thing we still want to pick up. Whilst others are discriminatory response towards you that… She’s realized that you’re her dad, and you’re different to us. That has a more personal meaning to her, too, and that really doesn’t process some things. But you need to see her more than once, you need to see some consistency, until you can prove that that’s a definite connection. And so, it’s something to tell us about when you see it, absolutely, because that’s really important, and we might say, “Well, we’ve never seen that.” Or you might say, “Yes, we were just observing.” So, yes, those kind of things, we probably would..
Joseph: It’s just been difficult without the visits, like I said in the past. It’s not helped, really, and I think she was probably… I don’t know, more alert that week, the first week that she was in. And she could recognize my voice, I suppose, the first week.
Mikaela: It’s hard to say, because I think she was on something as well, so I doubt it. But..
Dr. Rich: We can only assess where she is now.
Rinzzie: Yes, and it doesn’t mean you stop talking to her, you still do all the things you do as a family. Because now, that’s what we need to do, that’s your sister.
Dr. Rich: Exactly.
Mikaela: Yes, we’re getting some other family members in the call… We’ve got quite a large family, so she’s quite family-orientated, so she’s quite close knit, so she likes to have these… She always calls them every other day, so we’ll get them in. So, familiar voices, so she can just generally hear. How much she takes in? I don’t know. This is what I keep saying to dad, I’m like, “I don’t know how much of it goes in,” but if we can only hope that something might be happening in there.
Recommended links:
Dr. Rich: In a sense, you’re her family, and what you’re doing is different from what we’re doing, we try and keep things simple, and because if she is able to process anything, the simpler you can make it, the better, and try and reduce as much distractions as you can.
Mikaela: Agree.
Rinzzie: When talking, keep it simple, having breaks. Don’t feel you need to talk all the time in the call.
Joseph: I don’t feel like we’re talking too much today.
Rinzzie: Yes, if you can ask her to open her eyes, maybe just for a few seconds.
Dr. Rich: Yes. Don’t feel you need to tell a lot of things, just knowing, if she is aware of something, then sitting in silence is also one way. So, she is going to process something, and in a sense, she’s more likely to process those things. And actually, if she’s just trying to process that you’re there, actually sitting in silence might be the best way of just processing that you are there.
Dr. Rich: Okay, I think we’re okay with that for now. Are you going to go and visit her, did you say?
Jospeh: Yes.
Mikaela: Yes.
Dr. Rich: Sorry, Patrik, are you still on the call?
Patrik: Yes. I am still on the call.
Patrik: I have listened to all of this, and I think it’s great that everybody’s acknowledging what the family wants despite all the difficulties that a situation like that brings with, inevitably. Maybe just a couple of questions from my end. You mentioned physiotherapy earlier. I missed that part slightly, in terms of, are you mobilizing her? Can she get into a chair at all? Maybe in a recliner chair, or is she just in bed all day?
Recommended:
Dr. Rich: She has been on the bed all day. She’s not at the stage of being able to sit out, but she has been sat up on the edge of the bed with five people supporting her. Her tolerance isn’t there, so her head is very floppy, for instance. Even with a lot of tilt on, she’s not got proper control yet. The goal is, we’re working towards seating, and there’s a process that we go through to get there.
Patrik: Yes, sure. And with the move to the hospital ward, that’s imminent, or..?
Dr. Rich: As soon as there’s a bed that she can be safely managed with, which there isn’t at the moment… Because she’s got the tracheostomy, it’s demanding. So, there’s just a lot of other people with tracheostomies at the moment, and we don’t overload them with tracheostomies, because it’s not safe.
Patrik: Yes, no, absolutely. I see, I see.
Dr. Rich: But that’s the only barrier at the moment.
Patrik: Yes. And you mentioned earlier, obviously, that you want to do a PEG tube depending on the theatre slot available, from what I understand. I guess, with her not moving purposefully, she’s not at risk of pulling out her nasogastric tube at the moment?
Dr. Rich: No, but it can get dislodged during turning.
Patrik: Yes, of course.
Dr. Rich: Also, when I’m doing assessments, it’s a distraction, because it’s in her eye line, and it’s another thing that she can sense.
Patrik: Yes, agreed.
Dr. Rich: So, there are reasons, and they’re just.. you know nasogastric tubes, they’re really good for tiding you over for an acute illness for a few weeks. They’re terrible when kept longer in place..
Patrik: Yes. No, I get that. And just quickly with the tracheostomy, is she on oxygen, or just on a humidifier?
Dr. Rich: She is on a little bit of oxygen, because that’s how we deliver the oxygen to her body, but she’s not oxygen-dependent.
Recommended:
Patrik: She’s not… She’s more or less on room air.
Dr. Rich: She can certainly tolerate being on room air. So, no, she’s not on oxygen.
Patrik: Sure, yes. And how often do you suction her? Every hour, three times a day?
Dr. Rich: Just as she needs it, really. Obviously, the secretion load varies throughout the day and from day-to-day. The nurses and the physiotherapist will just assess that continuously, and they quantify exactly how often that will be, but just as and when she needs it.
Patrik: Right. And she does have an inner cannula?
Dr. Rich: Yes.
Patrik: Right. Okay. That’s great. Okay. I don’t think I have anything else. Oh, maybe just with the catheter. So, she’s got an indwelling catheter. Are you thinking maybe to look at a suprapubic catheter?
Dr. Rich: Possibly, yes.
Patrik: Right, at some stage.
Dr. Rich: It’s down the list of priorities..
Patrik: Yes, of course.
RECOMMENDED:
Dr. Rich: The urethral catheter is not causing any problems. Again, there’s other ways for drainage. That problem has not occurred. If needed be, we’d certainly consider putting a suprapubic in there.
Patrik: Yes. No, I understand it. It’s not a priority, I appreciate that.
Dr. Rich: Yes. So, if urinary management would be more problematic. We may well have done that, but..
Patrik: Yes.
Dr. Rich: Okay.
Patrik: Thank you.
Dr. Rich: You’ll visit your sister, then? Yes, that’s fine. Cheers for that, Patrik. Thanks for joining.
Patrik: Pleasure, pleasure. My pleasure.
Dr. Rich: All right.
Patrik: Thank you.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!