Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intenmailto:ive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How to Fight for My Dad’s Life Whilst the ICU Team is Forcing to Withdrawal of Treatment?
You can check out last week’s question by clicking on the link here.
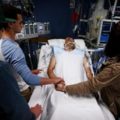
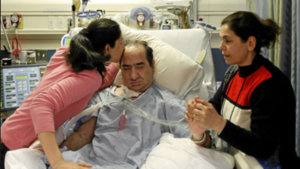
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ashanti, as part of my 1:1 consulting and advocacy. Ashanti’s dad has been readmitted in ICU and Ashanti is asking why are they pushing her to agree on palliative care for her father.
My Dad is Admitted Again in ICU. Why Are they Pushing Me to Agree on Palliative Care for Him So Soon?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Ashanti here.”
Hi Patrik,
Now here today I have been informed that the hospital doctor had made a referral to Palliative Care. I have a meeting coming Monday at 1 PM. I am insisting as always on continuing with all of his curative care. I am worried that I would be forced into something for my father’s care. I plan to stay strong and insist on his curative care for his current condition.
Please advise as to what would be the best course of action in this situation. Hospital people are always pessimistic with respect to the prognosis for my father.
In my assessment of my father’s medical condition. He needs all of the curative care with proper wound care for his stomach area, back, and heel. He has to move from nasal feeding to PEG feeding once the wound heals.
Based on my father’s condition, what would you suggest for his ongoing recovery and care?
Is palliative care not advisable? I want him to continue all the curative care he is getting right now and whatever is needed in the future as well.
Awaiting your response.
Best Regards
Ashanti
RECOMMENDED:
Hi Ashanti,
Thank you, Ashanti.
We need to put ourselves in your dad’s situation. We need to know what does your dad want anyways?
No one can ever predict what will happen next.
Also, you didn’t agree to palliative care while he had a tracheostomy, why would you agree to end of life care now?
Kind regards
Patrik
Hi Patrik,
Thanks for your email. My father and I want to get well however long it takes and get better. Does palliative care mean end-of-life care? Is that not hospice care? Please clarify. I would stay strong on his continuing curative care until he is back on his feeding tube through PEG tube. Other wounds on his tailbone area and bottom are healed as much as possible. One of the hospital doctors had mentioned that they would allow the GI (gastrointestinal) tube area wound to heal before attempting to fix it. This could take weeks I am not in a rush it’s the hospital authorities who are always rushing for discharge. Your comments would be appreciated.
His kidney function seems to be okay but due to high potassium they have changed to a different formula called Nephro 1.8 and he is having very loose stools. Also, the wound on his stomach (GI tube area) though small looks reddish, and they are dressing it up but seems to get wet very often not sure as to what is causing it. They mentioned they have left suction for a long time due to his nasal feeding. Is it something of concern?
Best Regards
Ashanti
Hi Ashanti,
Addressing your question here regarding palliative care. You can look at this link below that will give you good information.
Hope this article helps.
Thank you.
Kind regards,
Patrik
Hi Patrik,
Thanks, Patrik, for your email advice, and input. Thank you also for the article about the difference between palliative care and hospice.
Yesterday I had a meeting with one of the nurse practitioners who is in Palliative Care. I stayed on my course of continuing with his curative care. As on expected lines he sounded very pessimistic stating that doctors were giving a poor prognosis for him to get better. Aggressive medical interventions are not advisable for him. I wanted them to continue with whatever curative care he is receiving. They are trying to coerce me into agreeing to palliative care.
His medical condition as I discussed and observed.
- Vital parameters are stable. His blood pressure is under control; his blood glucose has been under 150 and he doesn’t mostly require any Insulin. Urine analysis for kidney function seems to be okay considering his previous CKD (chronic kidney disease). They are giving some Imodium to address diarrhea.
- PEG tube area secretions are more, and they have attached a bag to drain out better. This is making them change dressing less often. How long it would take the secretions to stop considerably and the wound to heal? Just an estimate. This gastric secretion seems to be more for the last 3-4 days. Not sure as to what is causing it?
- He developed some form of dry gangrene on the feet and his skin looks blackish. This is being dressed every day. I first noticed it 2-3 weeks back. There is no deep penetration of gangrene which appears to be more superficial. They have confirmed that there is no infection of the bone. But not sure how long it would heal and the blood culture markers to come down. As they are treating him with 2 types of antibiotics through IV for his infection as per his blood culture. Do they perform some kind of debridement? Any input about dry gangrene?
I tried to see pictures of his wounds that were taken recently. They could show only a few of them. Points 2 and 3 are now the areas of concern with respect to his health condition.
Awaiting your response.
Best Regards
Ashanti
Suggested Links:
Hi Ashanti,
Thank you for your response and for your updates.
Again, they will always be pessimistic into your dad’s situation, but you can always tell them to continue treatment as seen as appropriate and necessary.
It’s good to know that his vital signs are stable. Addressing his diarrhea with Imodium is okay as well, but I think they need to look at what’s really causing diarrhea.
I think he needs to have a GI (gastrointestinal) consult to assess him and further give appropriate advice as to his current issue with gastric secretions. This is something that needs immediate attention, especially lasting for days already. The thing is, while your dad is having more gastric secretions, they need to carefully monitor his serum electrolytes (potassium, magnesium, sodium, or calcium levels) as this may cause an electrolyte imbalance that is most often caused by a loss of bodily fluids through a prolonged fluid loss like in the case of your dad. This can potentially cause muscle spasm, weakness, twitching, convulsion, and further irregular heart rhythm.
You mentioned that your dad developed dry gangrene and this needs prompt management and care. Anyone with symptoms of gangrene needs immediate medical attention, to reduce the risk of serious complications.
Points to note regarding dry gangrene:
All forms of gangrene happen because of a loss of blood supply to a certain area. This deprives tissue of oxygen and nutrients, causing the tissue to die.
It may result from:
- Vascular problems: Most commonly due to the poor health of arteries and veins in the legs and toes. This usually develops over time due to conditions such as diabetes, peripheral arterial disease, and high blood pressure.
- Severe burns, scalds, and cold: Heat, chemical agents, and extreme cold, including frostbite, can all lead to dry gangrene. Wet gangrene may develop later.
- Raynaud’s disease: There is impaired circulation to the ends of fingers and toes, especially in cold weather. Raynaud’s is implicated in some cases of gangrene.
- Diabetes: Imbalanced blood sugar levels can damage blood vessels and nerves, reducing the oxygen supply to extremities.
If gangrene is suspected, further diagnostic tests will be used to determine the type and extent of the necrosis, and to detect or rule out gas gangrene.
Tests can include:
- an X-ray to reveal gas bubbles in muscle tissue
- MRI (Magnetic Resonance Imaging) and CT (Computerized Tomography) scans to determine the extent of muscle involvement
Tests of blood, tissue, and any discharge may be carried out to identify any bacterial infection.
Surgery may be necessary to explore the extent of the necrosis and to gain tissue samples.
Surgical removal of dead tissue or debridement may also be part of the treatment.
Treatment may involve the following emergency measures:
- intravenous antibiotics
- surgical removal of dead tissue, including amputation of an extremity or a limb to halt the wider spread
Reconstructive surgery may be possible, including skin grafting and other techniques.
Hope this helps.
Thank you.
Kind regards,
Patrik
Recommended:
Hello Patrik,
Thank you for your last email, and it’s been a while since I contacted you with regards to my father’s medical condition.
Yesterday my father suffered cardiac arrest around noon at the long-term nursing facility and seems to have stopped breathing. Emergency paramedics arrived and revived him through CPR (cardiopulmonary resuscitation) and got his pulse back after 45 minutes. He was taken to a nearby hospital Emergency Room.
He is currently intubated and seems to be unconscious and on ventilator support. Please find attached his ventilator settings and vital parameters as of 9 PM last night. He is being given Vasopressor – Norepinephrine and is being titrated down. His vital parameters as per the nurse and physician are critically stable and under monitoring care.
Yesterday evening around 6:30 PM they have started Hypothermia Protocol treatment for him and continue for 24-48 hours.
He is in some kind of cardiogenic shock and his kidney function seems to be badly affected. They have taken multiple blood works and continue to do the same. He is not on any sedatives as of last night. He is on IV fluid. Some antibiotics had been given as well.
Some Positive things:
His ventilator oxygen support seems to be brought down to 60% as of late last night.
His blood pressure also seems to be under control after giving him vasopressor and being titrated down.
Areas of concern:
Since he had to be revived for about 45 mins before getting his pulse back. Not sure about his brain functioning. Neurologist had been consulted. He would be doing some electroencephalograph to check his brain functioning. He seems to be in some kind of unconscious/coma state.
Kidney function seems to be badly affected. His lactate levels are high, urine output is low. He had a bowel movement last night.
Doctors have given a poor prognosis and only know about his condition as to how he progresses in 24 to 48 hours.
With regards to the hypothermia protocol procedure, his body temperature is being maintained at about 32-33 C from last night and will continue for about 18-24 hours before warming up. My concern is that they had started only after 6-7 hours of the cardiac event. Have they waited too long to intervene and apply the procedure? How effective would it be in helping his recovery?
RT (respiratory therapist) is monitoring his condition and caring for him in the ICU. They might start him on specific antibiotics for his UTI (urinary tract infection) based on blood culture. They also mentioned that they might need dialysis for some time for his kidney functioning. He had CKD (chronic kidney disease) and recovered well a month back after intervention with Potassium and Albumin through IV.
As per the nurse practitioner, the cardiologist and nephrologists would come in today and do their further assessment and intervention.
They are going to rewarm him slowly once the cooling phase has been completed.
How would his recovery be from this critical situation? What are some of the key things that need to be taken care of going forward?
What more can they do and continue in his recovery?
It’s going to be a long and slow path to his recovery after this setback in his medical condition. Anxious to know your input at the earliest for his recovery.
Thanks & Best Regards
Ashanti
RECOMMENDED:
Hello Ashanti,
How are you, Ashanti? We have read your email, and we want to thank you for reaching out. We are very sorry to hear about what happened to your father. It’s been a while since we heard about him and his medical condition.
It is good to know that his blood pressure is stable now while on vasopressors. Regarding your areas of concern, I hope you’ll find this input helpful:
- Neurologist consulted – requesting for EEG to check brain function. It is good to proceed with your dad’s EEG given that he was revived 45 minutes after the cardiac arrest. Any alteration in his brain function needs to be checked.
- Seems to be in some kind of coma state. Most patients who are successfully resuscitated from cardiac arrest do not regain consciousness immediately after the return of spontaneous circulation and may remain in a coma for hours or weeks, or even be in a persistent vegetative state. This coma state needs to be observed and monitored further.
- Lactate levels are high. How high is your dad’s lactate level? This needs to be monitored too, a follow up lactate level check must be done. It usually increases post-cardiac arrest. If your dad’s lactic acid level is high, it could be caused by a number of things. Most often, it’s because he may have a condition that makes it hard for him to breathe in enough oxygen. Some of these conditions could include sepsis, heart attack, congestive heart failure, or metabolism problems like kidney or liver disease.
- Urine output is low. Your dad’s urine output must be monitored closely. The nurse will have to check/ collect his hourly urine output to have an accurate record of his fluid balance. Your dad needs to be evaluated by a kidney specialist / Nephrologist.
- Blood culture? UTI? What is the result of his blood culture? Was his urine tested too for culture studies? The result will guide the doctors on what antibiotic needs to be started to fight the bugs/infection.
- Let us know what the cardiologist and nephrologist will advise to manage your dad’s condition. They might request for further tests so they can provide the best management for his condition. The nephrologist will be giving his input also if your dad is considered a candidate to start dialysis.
- Hypothermia protocol procedure – The therapeutic hypothermia procedure is used to cool your dad’s body to a temperature that is lower than normal. The hypothermia temperature of your dad will be maintained for 24 hours starting from the time of the initial therapy. This procedure is actually done after a cardiac arrest of patients that happened outside of a healthcare setting. The Therapeutic Hypothermia Protocol for cardiac arrest is initiated less than 8 hours from return of spontaneous circulation. Your dad will be cooled in the hospital after his breathing and heartbeat start again. This procedure may help your dad survive and reduce his risk of developing brain swelling, blood clots, and seizures after cardiac arrest.
- Currently, we will need to wait for the results of his laboratory tests, culture studies, and also the advice coming from his cardiologist and nephrologist. For his recovery, considering his past medical condition/ concern, if permissible, your dad may be placed in a special type of mattress as a preventive measure for pressure sores.
Ashanti, we would appreciate it if you can share with us the results of your father’s laboratory test results, imaging studies, vent settings, arterial blood gas results, list of medications and other pertinent documentation during his admission so we can guide and assist you further.
If you have any concerns, please feel free to send us a message any time. We’re here to help.
Kind Regards,
Patrik
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!