Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Do They Manage My Loved One Who is a COVID Patient in ICU?
You can check out last week’s question by clicking on the link here.
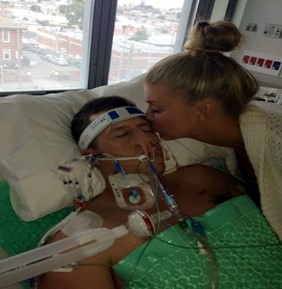
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Kenneth, as part of my 1:1 consulting and advocacy service! Kenneth’s brother has COVID in ICU with a breathing tube & on a ventilator. Kenneth is asking how his brother can get off the ventilator if he’s in an induced coma.
How Can My Brother with COVID in ICU Get Off the Ventilator if He’s in an Induced Coma?
Patrik: How are you?
Kenneth: Good. I’m sorry, I’m having a very bad day. There we go.
Kenneth: Hello.
Patrik: Hello, how are you?
Kenneth: Awful. I don’t want to lie to you, I’m looking a horrible mess, but awful. Yeah, awful, in all honesty.
Kenneth: Honestly, Patrik, I can’t even remember where I’ve been found… I’m sleep-deprived a little bit, so I can’t remember where I found the details, let me just try to do the consultation and see what you think and see if you could… I know that you have a paid hourly. If you think that it would be something that you could provide or would be of assistance of, so that’s what that’s about, and hopefully I can get some sleep sometime in next week.
Patrik: Are you referring to one of your parents, is it your mom or dad that’s in ICU?
RECOMMENDED:
Kenneth: I actually had called my dad, I told him I have a 15-minute consultation, I was like, “Do you want to just listen in?” So I have a brother who has Spina Bifida and he has a host of health issues, a lot of surgeries through the years, the complexities that come with that, he already had… So to sum it up, he’s in the ICU right now, he has tested positive for COVID, which for him, out of all people, you know when you talk about people with immune systems, everything that COVID would exploit, he’s pretty much… Overweight because of the years of steroids, he was already being given oxygen from a past surgery at a hospital here, so he has to have that.
Kenneth: He already had issues with breathing, and I think kidney or liver, just so many complexities over the years, he’s been really blessed to go this long, but just a lot of complexities. And so he’s tested positive, he’s in the ICU… And usually, his previous hospital would be the hospital that would really deal with him, so he lives more in a rural area, where the hospitals are…You know, they’re good, but when you come to more complex, usually his previous hospital is the one that would take over, they usually don’t want to really deal. So he’s down there, he’s in there, and what’s making me even more stressed is that my father, I guess being a parent, he’s like… Because of disability he has, they allow him to be in the room with him. And so of course, I’m kind of concerned about just him getting sick.
Kenneth: The doctors pretty much said… They put him on the ventilator, he’s been sedated, and now is on medically induced coma. And from what I understand… This is kind of partly, why I want my dad on the phone to make sure I’m getting this right to you. And they’re not able to get him off the vent, I think because when he comes off, he can’t tolerate it, and I think they have the highest, not pressure, but they’re up… I don’t know the language.
Recommended:
Patrik: Oxygen levels?
Kenneth: Yeah. Oxygen levels, not the pressure. And even with that, he still kind of struggles with the breathing part of it.
Kenneth: The doctors says he has pneumonia from COVID, COVID pneumonia, so the lungs are completely..
Patrik: Wiped out.
Kenneth: Yeah. And he’s already had that, just problems with it any way.
Kenneth: So the doctor… Just talking about it almost gave me a headache. So the doctor’s been treating him, they kind of had him… It’s hard because he’s there, initially when they put him there, I thought in my mind, “Okay, he’s always said that he didn’t want to live his life on a ventilator.”
Patrik: with a breathing tube.
Kenneth: So I can get that, so the thought was that my dad has fallen through with that, but we’re thinking, “Okay, we understand that the breathing is to…”
Patrik: Difficult?
Kenneth: To give him some time, as it heal him, but give some time to see if he can pull through with the difficulties of his health.
Recommended links:
Patrik: What timelines are we talking about, how many days in ICU?
Kenneth: Good question. So today would make it… what’s today, Tuesday? So Monday, he went to ICU, he went to hospital on during the weekend, I think they moved to the ICU on Monday.
Patrik: So yesterday?
Kenneth: Last, I’m sorry, last.
Patrik: So we’re talking about eight days?
Kenneth: Yeah. So this week would probably be at least seven days on the vent, I believe. Today might be seven or six, but he’s been pretty much… The last Saturday would make it the day that he would be admitted to the hospital, but he didn’t go to the ICU I think until Monday, I can’t remember, so we’re definitely over six days of him on the vent. The sad thing about it is that prior to last week, he went to the hospital, Wednesday or Thursday, and they told him he had severe asthma and maybe some urinary tract infection. I asked my dad, “So what does the asthma have to do with fever and all that?” They never tested him for COVID, and given him complexities, it’s time that was wasted, and I have so much anger with that part.
Kenneth: So he went back home, tried to take whatever they gave him, and he was ambulanced then. My dad flew back in, because he couldn’t take it…But he went to the emergency room. Not last week, the week before last. And let me tell you, for my brother going to the hospital, because of all his years, so his tolerance for pain is… it’s pretty much high. Yeah, very high, very, very high.
Kenneth: So I have anger already that I’m trying to push aside with the hospital about that, because that’s a lot of time wasted.
Patrik: Absolutely. What’s the hospital telling you about the next steps from their perspective?
Suggested links:
Kenneth: So from what they’re telling me is that… not telling me, telling my dad, I talked to the doctor… I’m sorry, I’m not trying to be rude, I was trying to see if he was on the phone to make sure I’m not telling you anything wrong between our 15-minute conversation. My mom doesn’t really understand what’s going on, she’s like, “Is he awake yet?” Because we can’t really see him. My dad is so destroyed…
Kenneth: Dad, I have you on speaker phone, I’m talking to Patrik of Intensive Care Hotline. Did you want to just hear, to make sure I’m not saying anything wrong, hopefully Kiko can’t hear the conversation, but you’re not on speaker phone, aren’t you? No, I have you on speaker phone, I’m on the call. Remember I told you I had a consultation to see if he can be given assistance, and then just helping us think through things.
Dad: Right, but I am on speaker. I think it won’t be a good idea because I am with your brother in the room.
Kenneth: So it’s not a good idea. Okay, all right.
Kenneth: He said, he’s in the room with my brother, he doesn’t want him to hear… Even though they said that he’s-
Patrik: In a coma.
Kenneth: Well, what the doctor is saying is this, his lungs and everything is really that bad, and that right now they can’t get him off the sedation. Because my concern was the cognitive effects, he is on sedatives, he too is on a paralytic, and how long… It’s a timeframe, and so they can’t get him off because when he’s off, I guess he can’t, would you call it tolerate, he’s fighting against the rhythm, pulling the tubes, and I said, “Okay.” So I said, “But if that’s what’s happening…” And then it jumps his vitals everywhere, and then the longer that he goes on there, of course with the COVID and all that, other functions are going to… health problems will come apart. And I was saying that, “What is the plan?” Because I hear that… But if that’s the issue, the longer that we have him on there, I feel like he’s not going to come out, it’s just going to be coma or a real coma or not be able to function, or he’ll not be able to breathe at all on his own. He’s in right now, and he’s not able to be on his own, they try to wean him down and he’s not able to breathe, so they put him back.
Suggested links:
Patrik: Okay, okay. Have they talked about ARDS, have you heard of ARDS?
Kenneth: ARDS, yes. Acute respiratory…
Patrik: Distress syndrome, have they brought that into the mix?
Kenneth: I thought they might’ve said to my dad, because he’s the ones there. My dad got the doctor to come and talk to me yesterday.
Patrik: Let’s narrow this down, what is your biggest frustration at the moment, what stands out to you?
Kenneth: What stands out to me is that, one, I think that the hospital… When someone says that I’m doing all that I can do, right? I believe that. But what if all that you’re… That might be your knowledge and skillset, because initially I said, okay, my mother was like, “Why can’t we send him back to his previous hospital, but his previous hospital might not be able to take her and the longer the time goes on, he gets so much critically worse off.
Recommended links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: Is he in the hospital of your choice?
Kenneth: No, he’s in a nearby hospital where he lives at. And they usually always, bring him to his previous hospital because he’s so complex. And this hospital now where he’s at, only if it’s smaller things.
Patrik: I see. Okay. In the ideal world, what would you like to see happen?
Kenneth: For him to come back, for him to come back. I think the hardest thing is that, three days ago he couldn’t talk, but he would open his eyes with certain people to let you know that he’s there, and as long as they sedate him, or the longer… I know that that’s going to go down, and I know that there’s pain. I hear what they’re saying, we’re trying different mixes and all that, a part of me wants to go… So I asked the guy, I said, “What about the tracheostomy?”
Patrik: The tracheostomy, that was my next question, what about the trache?
Kenneth: Right. So I asked about the trache, I said, from my understanding it’s not, again, it’s not going to take away any health issues, but what would it might do I thought, would take him where he can be up and not like…
Patrik: Yeah, he could be woken up, he wouldn’t need as much sedation as he does at the moment with the trache, however, you mentioned that he’s on maximum amount of oxygen support, which would be a hundred percent, they wouldn’t be able to do a trache on a hundred percent of oxygen, the risk is too high, so his oxygen levels would need to come down. So the other question that I have, are they proning him, do you know what I mean by proning?
Kenneth: Yeah, they tried that and my dad said that they… It seemed to help, but then after a while it was a lateral, it didn’t really work, its so many different complexes.
Patrik: Okay. Do you think that if he was going to the previous hospital, is he known there as a patient?
Kenneth: Yeah.
Patrik: How big is this ICU where he is at the moment, is it a big ICU, is it a smaller ICU?
Kenneth: No, this hospital where he is now is located in a smaller town, so I guess a regular sized hospital, I called his previous hospital and they told me that… Because my dad was like, “They’re not going to take a COVID patient.” They said, “Yeah, we will do a transfer for COVID patient.” But they’re so full on COVID, they have other buildings that they’re moving their COVID patients too. And my dad’s like, he doesn’t want it to be… His doctors from the previous hospital would still be there, but they don’t want to be a factory type, overflow type, he’s assuming.
Patrik: Yeah. Okay. If proning doesn’t work, have you heard of ECMO?
Kenneth: I feel like I’ve read that somewhere, I’m not really familiar with it, but…
Patrik: So look, it sounds to me like, if they tried proning the pneumonia must be pretty severe, maybe he does even have ARDS, it’s something we could find out if proning doesn’t work and he’s still on a hundred percent of oxygen, and he’s not getting better, I would argue the only way for him to potentially improve and also survive is to go on ECMO. Basically what ECMO is, and I would be very surprised if they had it where he is at the moment, they probably would have it there in his previous hospital. ECMO is a bypass machine that basically takes over the function of the lungs for a period of time, to let the lungs rest and heal. I would argue that ECMO therapy has been in very high demand before COVID, COVID had that demand go through the roof, okay? So ECMO beds would be in very high demand and in short supply, but obviously there are a lot of COVID patients on ECMO at the moment, and if you don’t ask, you don’t get. I guess it’s a case of, is the ICU painting a picture to you and your family that your brother’s going to die, but what’s the picture they’re painting?
Suggested links:
Kenneth: Yeah. What I hear is that, they’ve done all that they can do, but they will continue to try different… They fix this, the blood pressure might go up, his oxygen level drops, his sugar level drops, they try that, and this and that, but they said, what we need to start doing, as they told us, is start thinking about when we’re ready, comfort care.
RECOMMENDED:
Patrik: Well when you’re ready, my argument there straight away would be, when the hospital is ready, make a referral to a hospital that has ECMO. So they are operating from what they’ve got available there. And I also argue that the smaller hospitals, smaller ICU, I would argue, doesn’t have all expertise in looking at all options. So I believe they’re operating from a mindset of limited resources, limited expertise, whereas, okay, they’re talking about comfort care, how old is your brother?
Kenneth: 36.
Patrik: Oh my goodness, he’s so young. My argument would be, okay you’re talking about comfort care, what about looking at other treatment options in other hospitals?
Kenneth: I try to ask that, but I think even with his doctor from the previous hospital, they wouldn’t do anything differently than what they’re doing, and I don’t know that could be true, that’s why I became interested with your advocacy and consulting services at Intensive Care Hotline.
Patrik: Absolutely.
Kenneth: I wanted to just see, even through this process, I wanted somebody else, a medical professional where we pay and can give updates and help us. I don’t know what services, whether you’re part of seeing with the doctor to just help… The hardest thing is that, now my dad is in the hospital with my brother and just knowing… Then he’s coughing, I’m like, “Please don’t tell me you have COVID.” And whatever happens to my brother, I want to know that we have done what we can do. I don’t trust the hospital, who doesn’t give somebody a COVID test.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!