Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Can I Make Sure That My Dad with COVID is Well-Managed in ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ronald, as part of my 1:1 consulting and advocacy service! Ronald’s dad is with a tracheostomy and on a ventilator. Ronald asks about the survival chance of his dad with kidney failure and on a ventilator in ICU.
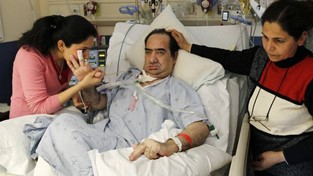
What is the Survival Chance of My Dad with Kidney Failure & on a Ventilator in ICU?
Patrik: Hi Ronald, how can I help you?
Ronald: Yes, we spoke the other day. My father is right now in the hospital. He was sent to an LTAC, and then he’s back in the hospital now. They sent him back, because they said he was in renal failure and I chose not to get dialysis.
Patrik: You chose not to?
Ronald: Yeah, and so… Oh, go ahead.
Patrik: Any particular reason why you denied dialysis?
Ronald: Because the two previous visits that I went to visit him… Once he was… He’s on a PEG as well, and the formula that they were giving him, I don’t remember the name of it, but it said, “For dialysis patients.” And so, I asked about it and then there was a nurse there and she said, “Well, let me check.” “I think that’s got a port that they would have on him.” And she said, “No, he doesn’t have a port.” I said, “Are you sure?” And I was like, well, “Why would you think that?” And she said, “Maybe it was for the person next to him.” She did see the dialysis machine in his room or whatever.
RECOMMENDED:
Ronald: After that I went one day, and his feeding tube was just dripping. There was like a little puddle on the floor, so I brought it to the nurses’ attention and eventually they said, “Oh, well, maybe they forgot to put it back in after they changed him.” I was like, “Okay, whatever.” The next day I went, and the feeding tube was capped off. There was a cap on the end, so he wasn’t getting any nutrition or whatever. When I asked them about that, they said, “Oh, he pulled it out, and we have to basically do the surgery over to put it back in.”
Ronald: It was pretty much the middle of the day, and they said they were going to do that the next day. It was almost like… I ask every day, “How are things going? Anything new? The labs.” No one ever said anything about the kidneys, ever, the whole time he was there. It was the same day that it was time for him to be recertified when they said, “Oh, he’s in renal failure. He needs dialysis.”
Patrik: Okay. How many days ago was that?
Ronald: I think it was two weeks ago.
Patrik: Are you suggesting he’s been in renal failure since around that time? He’s now in ICU, and how are they treating the kidney failure?
Ronald: He’s not in an ICU. He’s in what they call, “A Step Down.”
Patrik: Okay. The Step-Down ICU?
Ronald: They just call it the Step Down. It’s not ICU.
Patrik: He’s on a ventilator with a tracheostomy?
Ronald: Yes.
Patrik: It would be Step-Down ICU or like the ventilation Step-Down unit, most likely. But coming back, why did he go back into… So, he was in LTACH, he went back to that Step-Down unit and that was for kidney failure?
Ronald: That’s what they said, but if you look at… The reason they sent him was because they said he was in renal failure, and I didn’t want the dialysis, so that’s the reason I sent him there.
Patrik: So, how are they treating the kidney failure?
Ronald: Okay. At first… If you go into the records and you look at the medical records, when they admitted him, they wrote on there that he is not in renal failure.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: Okay. Are you able to visit your dad?
Ronald: Yes.
Patrik: Okay. When you go in there, are you talking to the doctors or to the nurses? Are you talking to them?
Ronald: I talk to a doctor. When he first went there, they say he was not producing any urine at all, and when I went into his room there was urine in the collection thing. And so, I was talking to the doctor, and I was just asking for an update, and she said that he’s not producing any urine. I looked at her strangely, so then she asked the nurse to go check. He went to go check, and the nurse came back and told her that there was urine in there.
Patrik: Okay. For someone to make sufficient urine, 30 to 40 milliliters an hour at a minimum. If there’s a little bit of urine in there in a 24-hour period… Just by what you’re describing, without knowing all the details, I’m concerned just with everything that you’re describing. I’m very concerned that your dad is in kidney failure and potentially not getting the right treatment. If someone is on a ventilator, you might be wondering, “What does kidney failure have to do with someone being on a ventilator?” It has a lot to do with it. Let me explain.
Patrik: If somebody is in kidney failure, fluids build up on the lungs, because fluid is accumulating. You can’t get someone off the ventilator if they are kidney failure and you’re not treating kidney failure appropriately. But, dialysis is a procedure and has its risks. It often is temporary, it often is temporary. And if it helps you to get your dad out of kidney failure, I believe it is something that you might want to consider.
Ronald: I have.
Patrik: Right, right. What are they telling you are the next steps?
Ronald: Now, they’re saying that he’s ready to go back to LTACH.
Patrik: So they treat it, the kidney failure?
Ronald: No.
Patrik: Is he still in kidney failure?
Ronald: They said it’s not a huge concern right now, but if I was to change my mind then…
Patrik: Do you know what led him into kidney failure?
Ronald: No.
Patrik: Right, okay. What is-
Ronald: Okay, go ahead.
Patrik: What is your biggest challenge at the moment?
Ronald: I’m concerned about sending him to LTACH. It just seems very strange these events that have happened. It seems like they’re trying to tell me that I only have certain options, and I don’t necessarily believe that’s true. So, my biggest concern is the dialysis, of course, and also the LTACH. I just don’t feel like that’s the best thing, but I’m warming up to the idea.
Recommended:
Patrik: And you are the main- You’re warming up to the idea of?
Ronald: Of the dialysis and the LTACH of being the proper thing to do.
Patrik: Okay. Could they do dialysis at the LTACH?
Ronald: They can.
Patrik: They can? Why did they send him back to Step-Down ICU if they were able to do dialysis? Do you know?
Ronald: Why did they send him back to?
Patrik: To the Step Down if they were… He went back to the Step Down from what I understand because of kidney failure?
Ronald: Yes.
Patrik: Yes. And you are telling me that LTACH would have been in a position to do dialysis?
Ronald: Yes.
Patrik: So why, if they had all the treatment available to treat kidney failure, why did they still send him back to the Step-Down ICU?
Ronald: Because I refused the dialysis. That’s from what I know.
Patrik: I see, I see, I see, I see. Okay, and now they’re telling you kidney failure is all dealt with, and he’s ready to go back to LTACH?
Ronald: Yes.
Patrik: Right, how do you-
Ronald: Oh, go ahead.
Patrik: How do you feel about it? Do you think everything has been done?
Ronald: I really don’t know what else to do to maybe… They said right now, all they’re doing is waiting to see if his kidney heals or jumps back, or whatever.
Patrik: Do you know what urea, creatinine, and BUN are?
Ronald: Do I know what they are? You mean, do you want me to give you the numbers?
Patrik: That would be great, if you could. Either-
Ronald: Take me a second to log into his account, if that’s okay.
Patrik: That would be great, that would be great.
Ronald: Right now the BUN is… Well, the last time it was 157, creatinine 4.67, and GFR 11.
Patrik: Okay. Do you have…? Okay, just give me a second, please. So, BUN seems to be high. Is your dad awake?
Ronald: Is he what?
Patrik: Is he awake?
Ronald: Sometimes.
Patrik: But not all the time?
Ronald: Correct.
Patrik: If you ask your dad to squeeze your hands, is he doing that?
Ronald: He was at a point, but now he… If you asked to hold his hand, he’ll push your hand away.
Patrik: Right, he’s doing that or he’s not?
Ronald: He is.
Suggested links:
Patrik: Okay. Good, good, good, good.
Ronald: Before he would hold your hand, but now he-
Patrik: Okay. It looks like creatinine, if anything, is a little bit on the lower side. Do you know if he’s producing urine, and if he’s producing urine, do you know how much in a 24-hour period?
Ronald: Yes. When I go there at the end of the day, it’s at the top. I think there’s like 400, I don’t know what the unit of measures is, but like 400.
Patrik: 400 milliliters in a day?
Ronald: Yeah.
Patrik: So, that’s about… Just let me get my calculator out. Just give me a second. 400 divided by 24. That’s 16 milliliters, now that’s not enough, that’s not enough. Do you know if he’s on a fluid restriction?
Ronald: He was, but I think they lifted that.
Patrik: Okay, do you know what that fluid restriction is?
Ronald: I don’t. Let me… Do you know what it would be called?
Patrik: Just the fluid restriction, just the fluid restriction. Would be often 1500 milliliters a day, but it could be less even.
Ronald: I don’t know where they would put the…
Patrik: Ask them. Have you asked them?
Ronald: No. If he was on… No.
Patrik: The 16 milliliters an hour could be a result of his kidneys failing, or it could be a result of him being on a fluid restriction. What’s your father’s weight, roughly?
Ronald: When he first went in, he was like 133, but now, when he went back to the hospital, he was like 190.
Patrik: Okay, now that’s a normal weight, because if people really tiny, it sort of impacts on urine output. Bigger person should have a bigger urine output, a smaller person will have a smaller urine output as a rule of thumb. That’s just as a rule of thumb. ICU is trying to more or less kick you out, or kick your father out, is that what you’re trying to say?
Suggested links:
Ronald: No, not really, but they’re encouraging us.
Patrik: Encouraging.
Ronald: It really feels like they want us to move on. Let’s see. I’ll copy this and send it to you. You might be able to look through this a lot faster than me.
Patrik: Do you have access to all of the medical records?
Ronald: From the hospital, but not from the… Yes.
Patrik: Yes, okay. Does it make sense to you?
Ronald: No.
RECOMMENDED:
Patrik: Right, okay. How long was he at the LTACH before? Give me a few more timelines. How long was he at the LTACH before he went back to the Step Down?
Ronald: Like around a month.
Patrik: One month?
Ronald: Yes.
Patrik: And before then, how long was he in ICU, before then?
Ronald: I want to say… Let me look.
Patrik: Just approximately, I don’t need to… Just approximately, a month, two months? Just tell me some timelines.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!







