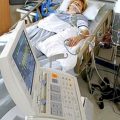
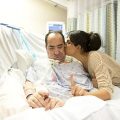
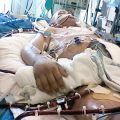
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
How Do I Challenge The ICU Team If They Don’t Want To Resuscitate My Mom?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answerquestions from one of my clients Max, as part of my 1:1 consulting and advocacy service! Max’s mother is critically ill in ICU and Max is asking if ECMO can give his mom a fighting chance to live in ICU.
Will ECMO Give My Mom A Fighting Chance To Live in ICU?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Max here.”
Doctor Al: Yeah, yes. Absolutely. Today, she’s been intubated now for two weeks, and in the time since then, we’ve treated her for hospital-acquired pneumonia, and she’s also developed acute renal failure.
Patrik: Yeah.
Doctor Al: And so given that, she now has multiple organs failing, the lungs and her kidneys, her lungs … We’ve been proning her, which unfortunately has not had the recruitment of lung volume that we were hoping for, and at one point to try to help. And that didn’t quite help, either. Her lungs are extremely stiff. The ventilator setting currently is very high. And you brought up a tracheostomy. At this point, I think she’s not a candidate yet for tracheostomy.
RECOMMENDED:
Patrik: I see. I see. Can you give a few more specifics when you say the ventilator settings are too high? What are we talking about, FIO2, 100%? PEEP greater than 12? What are we talking about?
Doctor Al: Let me pull up her latest FiO2. So she’s on pressure support with an FIO2 between 90 and a hundred percent. From 100 to 90 this afternoon. Pressure is 24 with a rate of 32.
Patrik: I see. I see. Yeah, no. Sure, sure. Yeah. And I would imagine her arterial blood gases would be fairly average, fairly poor?
Doctor Al: Sorry. What’s that?
Patrik: I would then say her arterial blood gases would be fairly average at the best?
Doctor Al: Yeah. Yeah, you could say that. If you’d like her latest numbers, she’s 7.32, PCO2 is 50, HCO3 18, PO2 60% and that’s on the hundred percent.
Patrik: Yeah, sure, sure. No, totally makes sense that you can’t look at a tracheostomy with those settings. In terms of treatment, you’re talking about prone position, lungs are stiff, and lung compliance is down, understand all of that. Is there any sort of alternatives? Would she be a candidate for ECMO? Is ECMO available in your hospital? Have you considered things like nitric oxide, epoprostenol nebulizers? Can you elaborate a little bit more there?
Suggested links:
Doctor Al: Yeah. So ECMO, unfortunately, would not be something that would be available. Multiple organ failure, the high settings she’s requiring on her ventilator.
Patrik: Yeah.
Doctor Al: And in terms of nitric oxide, that’s also something that would be indicated, or that’s not something that would actually profit our patients here in the hospital, at our hospital.
Patrik: Right. So it’s something that is not available in your ICU. Is that what you’re saying?
Doctor Al: Yeah. It’s not a treatment that we have.
Patrik: Right. Okay. But is it like a full blown ARDS picture? Is that what we’re talking about?
Doctor Al: Yeah. Yeah. She does have renal failure and ARDS.
Recommended:
Patrik: Right. Okay. Okay.
Doctor Al: It seems like her repair mechanism of the lungs from the ARDS is abnormal. It’s causing fibrosis.
Patrik: Right, right. Okay. Okay. And other than that, you’re talking about multi organ failure, understand lungs, kidneys. What about the heart? Is the heart struggling, as well?
Doctor Al: No, the heart tends to be okay. She’s only requiring levophed at a low dose, which could be more a result of the sedation that she’s requiring.
Patrik: Right. Okay. Okay. And I understand the situation is pretty concerning, what are your next steps? Is it just sort of a case of sit and wait, or do you have any other suggestions?
Doctor Al: One new treatment that we’re trying, she’s on a course of steroids already. We’re starting a course of solumedrol today, which we hope may help a little bit, but it’s likely that it may not help at all, either. Otherwise continuing pressure support and hoping she improves, the kidneys on the dialysis that is required for the acute renal failure and all other else.
Patrik: No, totally understand. Totally understand. And just again, what I have seen over the years with ARDS pictures, epoprostenol nebulizers, maybe it’s too late for that. Is that something that has happened? Maybe you can just … Again that is what I have seen. I’m not saying that is what you are doing. Is there any alternatives that you can see, or do you think you’ve tried everything within your power to treat the ARDS?
Doctor Al: Yeah, we’ve tried, I would say, everything. We follow the ARDS protocols, low tidal volume ventilation, and COVID. We’re doing everything that’s evidence based that we can do. Trying not to leave any stone unturned to give her the best chance possible.
Patrik: And again, maybe just coming back to one point that I discussed with Max, yesterday was, again, from my experience, I can only talk about my experience, that with ARDS, if proning doesn’t work, ECMO can be an option. Is ECMO available in your unit, or has she moved beyond the point that ECMO is an option? What are your thoughts on that?
Doctor Al: Unfortunately, she’s at this point where she wouldn’t be considered a candidate for ECMO, given her multiple organ failure. Unfortunately, it’s not available.
Patrik: Right. Okay. But you have no concerns neurologically that … I assume is in an induced coma. You mentioned she was paralyzed earlier. But there are no neurological deficits as far as you’re aware at this particular point in time, obviously, besides what’s being induced from a coma?
Doctor Al: She is requiring a lot of sedation. She’s on ketamine and propofol.
Recommended:
Patrik: Right.
Doctor Al: But otherwise, beyond that, there’s nothing abnormal there-
Patrik: Sure.
Doctor Al: … that requires any other neurologic evaluation.
Patrik: Sure. Okay. Okay. Max, is there something that needs to be translated here?
Max: No. No.
Patrik: Right. Okay. I don’t have any other questions at the moment. I don’t know, Max, if you or your family wants to ask other questions?
Max: No. No. We’re good. We’re totally good on everything, on the information. Thank you so much, doctor.
Doctor Al: And again, we’ll continue to try to let you know how she’s doing. Happy to answer any questions you have. I’m glad that you have someone with you to help you-
Max: Yeah.
Doctor Al: … navigate this, as well.
Max: Yeah. Thank you so much for that.
Doctor Al: Well, all right. Have a great rest of your day, and we’ll call you next time.
Max: No, that’s good. Thank you, doctor. Have a great day.
Patrik: Thank you for your time.
Max: Bye-bye.
Doctor Al: Sure.
Recommended:
Patrik: Bye. Are you there, Max?
Max: Yes. Yes. I’m here.
Patrik: Can you talk?
Max: Yeah. I’m right here.
Patrik: Right. Right. I don’t know whether you sent the message that I sent you. Did you bring up earlier, before I got on the call, did you bring up the CPR issue? I wasn’t sure. I wanted to bring it up, but I wasn’t sure whether I would overstep my boundaries. Did you-
Max: I haven’t. No. That was actually the first call that we’ve gotten with the doctor, but he did say, when he mentioned that to me, he mentioned that, that would be until her heart stops, and they don’t see it happening anytime soon, but it is a possibility and they just wanted to prepare us for that moment. So if that moment does come, we’re still discussing if we would like that option for her to get the CPR, just because it is very traumatic for her body, and we don’t want her to live a life where she can’t be how she’s been in her life so far. Because she’s always been a very strong woman. She probably wouldn’t want to live if she can’t live the way she’s used to.
Max: So we’re still trying to see our options in that area, for sure. But hopefully, hopefully we don’t get to that point. Hopefully her body gets better. But, this is my dad. He just walked in. He had to walk out for a little, but this is my dad.
Patrik: Hello.
Patrik: My name is Patrik.
Daddy: Hello Patrik.
Max: Oh My dad is asking, what possibilities do you see, if any?
Patrik: I don’t quite … You would have heard me saying, Max, when I asked about ECMO. I don’t believe that, that she’s not a candidate for ECMO. It’s been two weeks now, and the longer they wait, yes, the less likely it is that she’s a candidate. Do you remember, I did ask what’s her heart doing? She said her heart is strong, which is a good sign. So it’s really, we’re talking about the lungs and the kidneys, right? And did you say that prior to this hospital admission … The kidneys weren’t an issue before the hospital admission, were they?
Max: No, they weren’t.
Patrik: Oh. They weren’t? Okay. I asked on the call about nitric oxide. Did you hear that? Yeah. So when someone has what’s called lung failure, what I’ve seen is nitric oxide, prone position, you heard me mentioned the epoprostenol. He sort of ignored that, which maybe they don’t do it in that particular hospital, but again, it’s certainly something that I’ve seen over the years. And if all that fails, they should look for ECMO. I don’t buy that, after two weeks of this, she’s not a candidate for ECMO.
Patrik: From my perspective, it is the last option. The other option that I should’ve asked, and I forgot about it, to be honest with you, but it’s probably too early for that, the other option is a lung transplant. But before someone has a lung transplant, they usually do go on ECMO. You wouldn’t go from proning to lung transplant. You would go from proning, to ECMO, and then to lung transplant.
Recommended:
Patrik: Your mom at 52 is a candidate for a lung transplant. Usually the cut off for transplants are around 60, 65, so your mom in my experience is a candidate for a lung transplant. But before she gets that, she would have to go on ECMO. The challenge at the moment that I can see is all ECMO beds would be in huge demand. They’re in huge demand outside of COVID, but at the moment, there wouldn’t be many ECMO beds. But I still believe if the lungs aren’t improving, that’s probably the only option that I can see.
Max: All right. Perfect. Well, thank you so much, Patrik. You’re really a lot of help, and we appreciate it.
RECOMMENDED:
Patrik: Thank you. Please get in touch with me when you want to talk again.
Max: Sounds good. Thank you so much, Patrik.
Patrik: Thank you. Take care.
Max: Bye-bye.
Patrik: Bye. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!