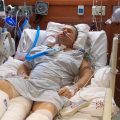
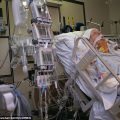
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Is It Legal for the ICU Team To Decide Not To Resuscitate My Mom Without Our Consent?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Max, as part of my 1:1 consulting and advocacy service! Max’s mother is in ICU with a breathing tube and Max is asking how he can challenge the ICU team if they don’t want to resuscitate her mom.
How Do I Challenge the ICU Team if They Don’t Want to Resuscitate My Mom?
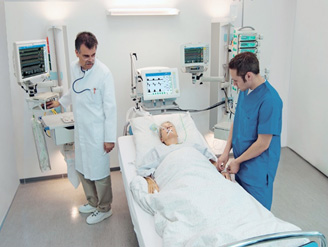
Max: They’re saying that they’re just going to keep doing the dialysis on her and hope that her kidneys get better. And because she choked on her nutrition I believed in the morning, her lungs got another hit and so the lungs are damaged and scarred. And so they’re going to hope that it gets better. But there are no other steps that they’re probably taking.
Patrik: All right. I’m hearing this at the moment all the time with COVID in particular, that the lungs are scarred, hearing it every day. Do you know how much oxygen she is on?
Max: Yeah. Yesterday, it was the first good news that we got from the doctors from the whole situation, is that she was on 60, and so she was breathing a little better. But because of her gagging on her nutrition in the morning today, she went back to getting on 100%.
Patrik: So she aspirated? Do you know what I mean?
Max: Yeah. That’s what they said.
RECOMMENDED:
Patrik: That’s definitely a step back, yeah. All right. Look, moving forward, it’s now… Which day was she intubated?
Max: She was intubated two weeks ago.
Patrik: So 14th day marks that a tracheostomy should be the next step especially if she can’t come off the ventilator. If she’s on 60% to 100% of oxygen, there’s no way she can come off the ventilator. So a tracheostomy would be the next step. However, at the moment with COVID, all tracheostomies are getting delayed. The reason for that is a risk for staff infection and instability of patients. So 60 to a 100% of oxygen, it’s almost too high. The risk is too high to do a tracheostomy. Not say it’s impossible, but the risk of staff getting infected plus your mom being very unstable probably will delay a tracheostomy. And also before they do a tracheostomy there are other ventilator settings they need to consider. Do you know if she’s on any vasopressors or inotropes, do you know what I mean by that?
Max: I don’t. Actually don’t.
Patrik: Okay. All right. The reason I’m asking you this, I’m trying to find out, yes, you’ve put a lot of information in there and that’s good, but when someone is in a situation like your mom, I as the clinician want to know the 30 other things that are happening. And I’m not exaggerating when I’m saying the 30 other things. There are 30 other things happening. The devil is absolutely in the detail. I would like to know blood results, chest x-ray results. I would like to know what medications she’s on. I would like to know arterial blood gases, which basically gives everyone a reading of oxygenation in the blood, which will tell everyone how effective is ventilation. Is her body getting enough oxygen?
Recommended:
Patrik: Issues such as now that she’s dialyzed, I would like to know the kidney markers, kidney blood results. The devil is absolutely in the detail in a situation like that, and that’s where I believe I can definitely help you as a next step. If you and I were to get on a call with the doctors, we can definitely ask all the questions that I believe you are not able to ask because you just haven’t worked in the environment. And I believe it’ll… Especially with issues such as, you’ve got the issue they want to not resuscitate her and they haven’t told you half of the things that are happening. Right?
Max: Yes.
Patrik: That is a massive concern to me that when they hand over to the doctors or to the nurses, they are giving the doctors and the other nurses the full overview, whereas they’re giving you only half of the information to you and all they tell you is, “Oh, well, we wouldn’t resuscitate her if her heart was to stop.” Your mom is 52.
Max: I know. Yeah.
Patrik: But we would be having the same conversation even if your mom was 89. We would be having the same conversation. If your mom wants to live, well, she wants to live. If you as a family want her to live, we would have the very same conversation irrespective of age.
Max: Yeah. I believe so too.
Patrik: You know?
Max: Yeah I got you.
Patrik: So I do not want to be negative. As long as there’s life, there’s hope. How do you get updates?
Recommended:
Max: Phone calls. The doctors call us every day around like 3:00, 4:00, 5:00 P.M. And then today was the first day that I asked them to call me twice, one said they’ll, which is when they told me about the gag and about the aspiration. And then they called me again to give me more of an update see if… Another doctor called, another more experienced doctor called in the beginning said, but yeah. So we’re going to be calling him. We call the nurse to talk with my mom and then the doctor calls us to give us updates.
Patrik: Okay. Right. And if you don’t pick up, can you call them back and they will talk to you then, or is it a case of if you miss then bad luck?
Max: Well, we actually haven’t missed a call so we don’t know. But we’re consistently picking up and we’re just keen watching the phone and all of that, yeah. Each phone call that comes in we’re like, “Oh, my gosh.”
Patrik: Yeah, got to answer. All right, look, here is where I think I can help you. I mean, you know what to do to challenge the not giving her CPR. And they will probably make life difficult for you, they may. But again they will probably reiterate with you that they can make that medical decision. Because that’s what they do with most people, they try to intimidate them. So just because you will challenge that doesn’t mean they’re going to give in straight away. My advice is to be persistent. And if you ask for their hospital policy about CPR and they’re not giving, emailing it to you or whatever, well, your question needs to be, “What do you have to hide?”
Suggested links:
Max: Okay.
Patrik: Why is there no transparency about that? How big is this ICU? Do you know how big the ICU is?
Max: Because it’s a general hospital, so it’s pretty big.
Patrik: Pretty big. Okay. The reason I’m asking is, I’m glad to hear that it’s a big ICU, I would argue that the bigger the ICU, the more expertise they have.
Max: I agree.
Patrik: Okay. There’s also a higher chance that if it is a big ICU, that they might have ECMO available. When I hear clients.
Max: Yeah, I’ll sort that tomorrow.
Patrik: I think you should. Definitely. The smaller the ICU, I’d say the worse, because there’s less resources, less expertise. So bigger ICU I argue is generally speaking better.
Max: Okay. Hopefully.
Patrik: Hopefully?
Max: Yeah.
Recommended:
Patrik: So, yeah. Look, that’s where I think I can leave you with. What I can do as a next step Max, is I can send you an email just with some consulting options. If you would like that I can definitely get on a call with you to the doctors, ask the questions that you are not able to ask simply because you haven’t worked in the environment, and that’s where I can help you with.
Max: Definitely. Thank you so much.
Patrik: Oh, pleasure.
Max: Thank you.
Patrik: It’s horrible.
Max: Thank you for getting on this call with me and taking the time to do this. It does mean a lot to us.
Patrik: It’s pleasure. I can tell you what’s happening at the moment, it’s terrible. Unfortunately, there are so many families in a similar situation than you are. It’s just… I mean, we’re busy all year round but the COVID certainly has put an extra layer of complexity to everything.
Max: Yeah. I’m sure. It’s crazy how 10 months went by and we were good and healthy and then out of nowhere it just all hit, right?
Patrik: Yeah.
Max: Just going with emotions and praying and hoping that her body is doing everything.
Patrik: Yeah. Definitely do that, pray and hope. At the same time I do believe that more clinical information will help you to keep advocating for your mom. Because again, I do believe that they’re only telling you a half of the story.
Max: Yeah. I believe so too. And I’m so glad that I found your YouTube channel because it was very informative too and I was like, “Yeah, now he knows exactly what he’s talking about and I need help.”
Patrik: Sure.
Max: Because I’ve been doing this all by myself and it’s been really difficult.
Patrik: And you don’t have any health professionals in your family or…
Max: No. I have a friend who… She’s going to nursing school. She’s also going through it, learning.
Patrik: Yeah. Okay. All right Max, what I’ll do is, look out for an email, I’ll send you an email in the next 10 minutes or so, and then you can go from there. Please note that if you do want to engage my service, I do work on a first come first serve basis.
Max: Okay.
Patrik: That’s all.
Max: All right. We’ll definitely keep you in the loop as well.
Patrik: Yeah, sure.
Max: Thanks so much. Thank you.
Patrik: Pleasure. And go and get some sleep, it’s late.
Max: Yeah, you too.
Patrik: Okay. Thank you so much. Have a good night.
Max: Yes. Bye.
Patrik: Thank you. Bye.

Max: Hi Patrik, we’ll be in a call with the doctors.
Patrik: Alright.
Patrik: Ask questions straight away. What do you want me to do?
Max: I’ll just listen.
Patrik: Okay. Okay. Thank you.
Max: Yeah.
Doctor Al: We hope she improves. We really do. But I just wanted to let you know to prepare for the possibility that she may get even sicker. We can do to stop that with multiple organs failing.
Doctor Al: We are doing everything we can to give coronavirus a chance to retreat.
Max: Okay. Hi, doctor. I am the son of your patient, and I have a family friend who was able to come by and give us a couple of advice, and he’s on the call right now, as well, and I think he may have a couple of questions, as well. His name is Patrik.
Patrik: Good afternoon, doctor. How are you?
Doctor Al: I’m good. How are you?
Patrik: Very good. Thank you. Can you hear me okay?
Doctor Al: Yeah. Yes.
Patrik: No, that’s wonderful. That’s wonderful. Look, I am helping the family with this obviously significant issue to deal with. I am a critical care nurse by background, and maybe if you can highlight the main issues. Max has given me a good update, but I guess he’s not clinical. Maybe just to give me a bit of an overview from head to toe. I guess she’s in an induced coma. She’s being proned, from what I understand. The lungs are scarred, from what I understand, and I guess you are fearing for her life, and I do understand you’re doing everything that you can. Maybe just for my own understanding, what … She’s on a ventilator. Is she on vasopressors? She’s in an induced coma? Have you considered things like doing a tracheostomy as a next step? Can you shed a little bit more light on those issues?
Recommended:
Doctor Al: Yeah, yes. Absolutely. Today, she’s been intubated now for two weeks, and in the time since then, we’ve treated her for hospital-acquired pneumonia, and she’s also developed acute renal failure.
Patrik: Yeah.
RECOMMENDED:
Doctor Al: And so given that, she now has multiple organs failing, the lungs and her kidneys, her lungs … We’ve been proning her, which unfortunately has not had the recruitment of lung volume that we were hoping for, and at one point to try to help. And that didn’t quite help, either. Her lungs are extremely stiff. The key to the ventilator going is very high. And you brought up a tracheostomy. At this point, her ventilator settings are too high. And as we do any type of tracheostomy, it is not where she needs to be.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!