Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Why Is The ICU Team Not Considering A Neurologist In My Dad’s Treatment?
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Anna as part of my 1:1 consulting and advocacy service! Anna wants to fully understand the course of treatment of her dad in ICU but she’s having difficulty requesting medical records from the ICU team due to matters of kinship.
I Want To Request For My Dad’s Medical Records In ICU But Do I Have A Right As His Daughter?
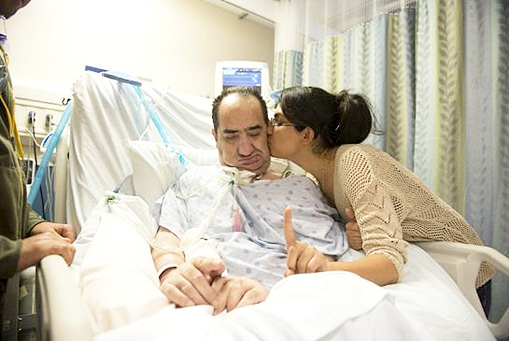
“You can also check out previous 1:1 consulting and advocacy sessions with me and Anna here.”
Patrik: As long as that’s the case, somebody needs to sit down with him and needs to ask him. He will have lighter moments of course, then on some days, than he will have on others. You would have probably seen that already.
Anna: Yeah.
Patrik: Right. That needs to be your line of argument around the brain being intact. At least on some days.
Anna: Yeah, yeah.
Patrik: In terms of them going off that logical, but also emotional argument, it’s also around what it then comes down to hospital policy, that they need to certain follow procedures if they do want to remove treatment against next of kin or medical power of attorney’s wishes. Here is the other thing and I don’t think I’ve answered that question yet. You mentioned in your first email, is it taking longer for patients to come out of an induced coma when they’re older? Definitely yes.
Patrik: Let’s just say, if your Dad was in his 30’s or in his 40’s, there’s a higher chance he would have woken up more by now. It’s not guaranteed of course, but you can generally speaking, say that somebody about the age of 65 in a prolonged induced coma takes a lot longer to wake up. Did you get chance, I sent you an interview that I did with a gentleman. I know it’s a fairly lengthy interview.
Anna: Yes, I listened to it. Yes, it’s very interesting.
RECOMMENDED:
Patrik: Right. This man is unbelievable. With a situation like, if you listen to that, there’s no reason why your dad can’t be in a similar situation. There’s no reason. This man is still alive. The interview’s about two years old. This man is still going strong.
Anna: Yeah. Yeah, it’s an incredible story. Absolutely. One of the things I wanted to ask you Patrik, I know our time’s almost up, is obviously, as you know, the consultant, is it the same consultant yesterday that refused to give us the CT scan report?
Patrik: Yeah.
Anna: I will ask my step mom who is my dad’s registered next of kin on his note, to ask for another, I’ll ask her to ask for a copy. From what you’re saying, there is no reason why they shouldn’t give us a copy of the CT.
Patrik: You have every right, or the next of kin has every right to access medical records. Every right.
Anna: Patrik, do I have a right? Do I have a right as his daughter?
Patrik: Not necessarily, but the next of kin definitely has the right. I think what you might have to establish is, you really need to establish who’s next of kin. The reason you as a daughter may not necessarily have the rights to request the medical records, is in theory, you could be estranged from your dad. I know that’s not the case, but in theory, you might come in. You could be estranged, whatever the case may be. Then you would have no right for that. I guess in your situation, the next of kin needs to request that.
Anna: Okay. I know you said this in your email last night you suggest to ask them to access all of his records from the beginning of his ICU stay?
Patrik: I think you could. You could. The question is, what are you going to do with them for now? I think the CT’s probably way more important at the moment. Get a report there. That’s probably way more important, then also, probably get an idea of what medications he’s on at the moment. Another, what could happen is, I doubt that he’s on anything that’s still keeping him sedated, but at the end of the day, you never know.
Patrik: You would hope he’s off any sedation at the moment, but I wouldn’t rule it 100% out. For example, a lot of patients in ICU, what happens is when patients have been in prolonged induced comas, they have a disturbed day and night rhythm.
RECOMMENDATIONS:
Anna: Yeah, which is what he’s got.
Patrik: Yeah. I’ll tell you what might happen, because he’s got a disturbed day and night rhythm, there is as chance that if they want to keep him asleep at night, that they’re giving him something to help him sleep. They may do that.
Anna: Yup.
Patrik: Right, right. Again, if it’s not a natural product, and it probably isn’t, it may stop him from waking up.
Anna: Okay.
Patrik: The devil’s in the detail in a situation like that.
Anna: Yes, of course. Absolutely.
Patrik: Find out what medications he’s on, and get that CT report, and keep asking for a neurologist. Don’t let them get away with their one size fits all. I don’t know when you said 15 beds in there. I don’t know whether you’ve made much contact in this period of time with other families, potentially, have you?
Suggested article:
Anna: To be honest, because dad’s been in almost six, seven weeks now, I mean I have to say most of the families here that I saw at the beginning. Either their relative didn’t make it, or they were transferred to ACU, or another ward. We’ve not kept in touch with them.
Patrik: No.
Anna: No, but obviously quickly in the beginning, I would say in the first month we saw other families who were in similar positions, really their relative, of our dad. Some made it, and some didn’t, but obviously it was helpful seeing other families, and learning that they had discussed the same things. Mom’s on a mechanical ventilator but they can’t seem to get her off of it, et cetera, et cetera. It was similar stories in terms of challenges faced, and by patients, and critically ill, but as I say, most of them it’s just that didn’t make it, or were transferred. There isn’t really anyone there now that we know.
Patrik: Okay, yeah. No, no. The reason I’m asking is simply, if you feel like there are a lot of patients dying in there, it says something about the place. The reality, 90% of ICU patients survive. You really need to put the doom and gloom in perspective. 90% of ICU patients survive. Why should your dad not be within those 90%?
Anna: Yeah. Absolutely.
Patrik: Now, when I say that 90% of patients in ICU survive, it’s not talking about quality of life.
Recommended:
Anna: No, of course.
Patrik: We’re just talking about patients leaving ICU alive. We’re also not talking about how many patients of them do then leave hospital. We’re not talking about any of that, but the reality is, 90% of ICU patients survive. Why not your dad?
Anna: Yeah, absolutely.
Patrik: At this point in time, he’s proven to everyone, that he’s a fighter. Beyond a shadow of a doubt.
Anna: I know, and I think it’s probably one of the things might have forgotten to convey, too. In some respects they’ve not really treated, or had a case like my Dad’s before. I don’t think that they’ve really ever seen someone of his age, who’s gone through all of the challenges he’s had, and survived. I think it’s a massive puzzle from the beginning, and I think they still find him a puzzle. Obviously when we said, can we just give him more time because we know him, they’d said, okay.
Patrik: Exactly.
Anna: They said, one of the consultants said to my sister, he’s an ICU textbook of how patients follow a path. She said, “Your dad just isn’t doing any of it, and we can’t really work him out.” They said he’ll never breathe on his own. He’ll never come off the ventilator. That was presented to us presumably as a reason to restore treatment. They said, if we remove the oxygen, tracheostomy, they said, if we remove the breathing tube, he would die within minutes. Then fast forward to weeks after that, and then actually they were able to get him off the ventilator. For an hour a day and I think the most was about 12 hours, and then they put him back on overnight.
Anna: I think we tried to trust them, but they keep using example of their, you felt he would never be able to breathe on his own again, based on the picture of his lungs, based on how he’s presenting, but actually he has done it. Don’t you think that that’s actually a massive aspect to determining his future care? They just say well, yeah, but it’s only a reason, and he’s got another chest infection, so now he’s back to step one again. And as they say, every step that he did pass there’s another one that he has to regain. I think, as you say, they necessarily have to deal in the negatives, because that’s what they’re faced with on a typical basis, day to day. We continue to try to take it on a positive side, in terms of he’s off the dialysis, it could be worse. He survived the cardiac arrests. You never said he’d get off the ventilator. He actually has.
Anna: There’s much more to do. We have tried to put forward the positives all the time, and I think there is something to do for dad within the bigger picture of the treatment that still knocks me out.
Patrik: Absolutely. You see, the reality is, they’ve been negative from the start. Your dad has proven them wrong. No ICU will tell you oh I’m definitely going to save your dad. We’re definitely going to save. No ICU will say that. No matter the issue, why people come into ICU, nobody will tell you, oh yeah, we’re definitely going to save your mom, your dad, whoever the person might be. The language is never going to change.
Anna: No, of course.
Patrik: Right. From that perspective, that’s another line of argument for you. You can say look, your prognosis has never changed, but what we actually observe with our dad, is very different to the prognosis that you’ve given us from the start.
RECOMMENDATIONS:
Anna: Yeah.
Patrik: It’s like with anything in life. You’re not watching for somebody’s words. You’re watching somebody’s actions. The words they’ve been speaking for making weeks now, has been negative. However, your dad has made, has not only survived seven cardiac arrests, he’s now at the point where they’re still doing all the right things. I really like that they’re getting him out of bed every day. I think that’s critical. That’s really critical, and you need to make sure they keep doing that.
Anna: Yeah.
Patrik: From my perspective, very few patients have I seen, when you start mobilizing someone, I have seen very few patients who then die or who when treatment gets stop, don’t get me wrong, I have seen the odd case, but that would have been caused by a major deterioration. There hasn’t been a major deterioration since the last cardiac arrest. There hasn’t been a major deterioration. It’s only been up, hasn’t it?
Anna: It has, yeah. Generally speaking.
Patrik: Right. How are you going to sell to a patient that’s potentially waking up more and more, and that’s slowly improving? Yes, slowly, but he’s improving. How are you going to tell someone oh, by the way, we’re going to stop treatment tomorrow? That, in my mind is euthanasia, or even murder.
Anna: I know. Yeah, and obviously that’s, of course as the family, we are his advocates. We have to ask the questions.
Patrik: Absolutely.
Anna: We have to fight for him, because otherwise if we don’t, then decisions will be made for him, based on a person in an ICU bed that isn’t the person to them is effectively…
Patrik: A number.
Anna: A number, yeah, exactly. Okay. Basically, I need to request again my stepmom for kinship, I need to literally request again for a neurologist to come in based on what our dad would have wanted.
Patrik: Absolutely.
Anna: We’ll find out what medication he’s on, and I’ll get back to you.
Patrik: Please, and also send me a picture of the ventilator.
Anna: Oh, yes of course. Yeah, we will. My brother will try and do that today.
Patrik: Please. Also, that’s another last thing that I really want to mention. I think I mentioned it in the email. Yes, you are experiencing resistance at the moment, but don’t give up. It will get easier. Once they know you’re not giving up, it will get easier.
Anna: Yeah.
Patrik: At the moment, they’re treating you like the other 99% of families who don’t question. Once they know you’re not giving up, you will see the changes in them. Don’t give up just because it’s hard at the moment. It will get easier.
Anna: Yeah, absolutely. You’re right. Once they become aware that we will just continue to ask more questions they will get into it.
Patrik: Get comfortable asking them questions. Just get comfortable and don’t worry about their response. Doesn’t really matter what they think, or what anybody thinks. This is what I refer to as a once in a lifetime situation.
Anna: Yeah. That’s really, that’s very true. Yeah, absolutely. As you say, it’s once in a lifetime, and I don’t think we would ever want to look back and regret that we didn’t ask that one question.
RECOMMENDATIONS:
Patrik: That’s right. Yeah, I hope that was helpful.
Anna: Oh, very helpful Patrik, as ever.
Patrik: I will send you the recording of the call. Please send me the ventilation picture, and the medications, and I will comment on that and if you need more help, you know where I am. I’m very happy to look the ventilation and at the medication and make some comments there. I think there’s a very good chance your dad is fairly close to coming off the ventilator hopefully, because that would be another line of argument for you. If he’s close of coming off the ventilator, if he’s on minimum support already, that’s another sign that he’s slowly improving.
Anna: Yeah, absolutely. Okay. Yes. We will do that and I’ll get that to you. Many thanks again Patrik.
Patrik: You’re very welcome. I hope it’s continuing to improve, and stay positive. No matter the outcome, it’s going to help you staying positive. It’s easier said than done, I know, but no matter the outcome, it will help you staying positive.
Anna: Absolutely, yeah.
Patrik: Absolutely.
RECOMMENDED:
Anna: Thank you.
Patrik: You’re very welcome. Have a good day.
Anna: Thank you. Thanks so much. Take care.
Patrik: Thank you so much. Bye, bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!