Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
This is another episode of “YOUR QUESTIONS ANSWERED”. And in today’s episode, I want to answer a question from one of our readers, Harold.
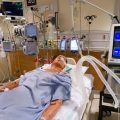
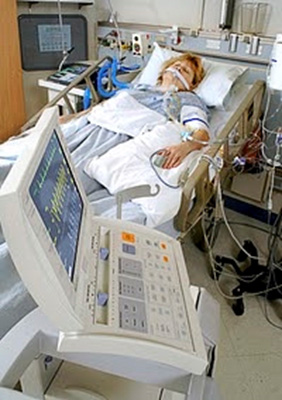
Harold has his mother in the intensive care unit after cardiac arrest. He is asking, does she have brain damage, and can she survive?
My Mom is In ICU After Cardiac Arrest. Does She Have Brain Damage, And Can She Survive?
So Harold writes in,
How are you doing Patrik? I just discovered your YouTube videos last Saturday. My mother suffered a cardiac arrest on Wednesday. I was at work. My father and brother found her. My brother and her had just had a conversation with her. He went to the bathroom. My dad was in the kitchen and heard my mother make a loud sound. My dad said he can’t describe the sound my mother made, but we’ll never forget it. They tried to wake my mother up. She wouldn’t respond. They called 911 they came after several minutes.
My mother already had a weak heart. She has been in ICU since Wednesday. They are telling us that since she went minutes without oxygen to her brain that her brain is damaged and won’t respond. They have presented us with the doom and gloom scenario and the negativity as you say. They want us to “make a decision” or “make decisions”. I had my doubts, so I started to do some research today and starting watching all of your YouTube videos and read your site. I am extremely optimistic after your information. All I want to know, is there anything else you can tell me about the brain damage and the outlook without the doom and gloom? Thank you for your time.
From Harold.
RECOMMENDED:
Hi Harold,
Thank you so much for writing in and thank you so much for being a client and I’m very pleased to hear that you found my videos and our website intensivecarehotline.com useful. So as you may have heard me say before, the biggest challenge for families in intensive care is that you simply don’t know what you don’t know and that you don’t know what questions you need to ask and that you don’t know how to manage the doctors and the nurses without knowing that you will be pretty much fighting a losing battle in such a high stakes life or death decision. Because as you’ve already correctly alluded to, you are presented with the doom and gloom and the negativity and the intensive care team will most likely try and push towards withdrawing life support and try and push towards an end of life situation, which you certainly don’t want for your mother.
And I’ve seen this over and over again that if you’re not arming yourself with the right information, again, you’ll be fighting a losing battle. If you don’t know how to manage doctors and nurses, you’ll be fighting a losing battle. And you don’t know what to do next and you don’t have a strategy.
So what’s important to know in a situation like that Harold is really, there are so many things happening simultaneously when somebody had a cardiac arrest outside of the hospital and is now in intensive care ventilated with a breathing tube or endotracheal tube in their mouth, in an induced coma, on sedation, most likely on Inotropes and other mechanisms of life support. But I’ll break it all down for you in a moment so you understand what’s happening. And I’ll also come to your main question, which is the future outlook, but we can’t really look at the future outlook unless you understand what’s happening at the moment and what your options are.
RECOMMENDED:
And you know another word of warning here that the ICU team won’t present you with options because the only option they present to you is the “doom and gloom and the negativity”. Because they simply want to save money. They want to empty the bed. They only want to basically move towards the end of life as quickly as possible so they can free up the bed, limit their investment, get the next patient in and earn money again.
But they often don’t make the emotional as well as the financial investment to help critically ill patients like that because they see it as pointless. But I know from experience it’s not pointless. And that’s obviously why you’re writing in because you don’t see it as pointless either. So let’s break this down for you Harold so you understand what you’re dealing with.
RECOMMENDED:
So when your mother had out of hospital cardiac arrest and it’s unknown how long cardiac circulation has ceased, which means, you know, if the brain doesn’t get oxygen to the brain for more than three minutes, there is the risk for irreversible brain damage. And that is probably what the intensive care team is referring to. That the “downtime” for your mom and the downtime means the number of minutes your mother’s brain didn’t have sufficient oxygen supply. So you know, if it’s longer than three minutes, then the risk or the likelihood of brain damage or permanent and irreversible brain damage is definitely there.
But again, it sounds to me like there is no evidence for that at the moment. And it’s hard to say how long was the downtime. It’s also hard to say how effective was the CPR or cardiac compressions. You haven’t actually alluded to that, you know, how long it took to recommence or to commence CPR. How effective it was? Must’ve been effective because otherwise, your mom wouldn’t be here. So the evidence of how long the “downtime” was, can come from a CT or MRI scan in order to determine the brain damage.
So my first question to you is, has the CT or MRI scan of the brain being done to determine the level of brain damage or maybe brain damage could be even ruled out from a CT scan. So again, you know, they can’t give you the doom and gloom talk if there is no clinical evidence. So that’s your first step. Find out whether a CT or MRI scan of the brain has been done. Has it been revealed? What are the neurologists saying about potential brain damage? You know, again, where is the clinical evidence?
So next when somebody has an out of hospital cardiac arrest, standard therapy in this day and age is cooling therapy to protect the brain, protect other vital organs to limit their perfusion again, to give the body a rest. And that is standard therapy usually takes 24 to 48 hours of cooling down to 32-33 degrees Celsius and then slowly warm up the body again. During this period of time, an induced coma need to take place and obviously for anybody after significant cardiac arrest, they will be ventilated. Your mom would have been commenced on ventilation even at home when the ambulance arrived. But in order to tolerate mechanical ventilation and the breathing tube, your mom would have gone into an induced coma early on. And with the cooling therapy hopefully that she has, she would have had to go into an even deeper sedative state and into a deeper induced coma because you know, if you’re cooling somebody’s body, the patients start to shiver. And one way to manage the shivering is again to put people into a deep induced coma. And even that doesn’t prevent them from shivering, then sometimes they need to be paralyzed medically as well.
RECOMMENDED:
So that’s sort of the framework. The other thing you do want to find out is with the cardiac arrest, your mom might have had an angiogram or an angioplasty to find out the blockage of the heart that led to the cardiac arrest. Again, find out if your mom had an angiogram or an angioplasty to potentially unblock an arterial blockage to the heart.
Again, you haven’t mentioned any of it. I am already wondering, you know, what has the intensive care team shared with you? Have they been open and transparent with you? For example, if the angiogram hasn’t taken place, number one, why hasn’t it taken place? Is there a cardiologist involved? If it has taken place, why are they not telling you? And again, that’s why it’s so important to remind people that you need to ask the right questions. If you don’t ask the right questions, you don’t know where you stand, you don’t know what to do, you don’t know what questions to ask. You are walking in the dark. And I’m obviously here to help you with that and you know, shed light on your questions and shed light on this situation.
RECOMMENDED:
And other thing that needs to happen after cardiac arrest is obviously an ECG, needs to be done. Electrocardiogram, troponin levels need to be checked. Troponin is a blood test that can indicate how severe a heart attack or cardiac arrest was. A high troponin level suggests a significant heart attack or cardiac arrest. Other blood results that are important are hemoglobin levels, white cell count, liver function, renal function, or kidney function. Because again, if your mother had prolonged hypotension or prolonged low blood pressure, there is the risk for kidney failure to occur as well.
So, you know, the whole situation is a very complex situation and it’s not as simple as, you know, doom-and-gloom and withdrawal treatment. Everybody, organ needs to be looked at. It needs to be looked at in their own way and see, you know, what needs to be done next to get your mother through this situation, get her to survive, and then look at rehabilitation.
RECOMMENDED:
So other things that should have happened in the meantime is, your mom should have had a chest X-Ray, your mom should have had an ultrasound or an echocardiogram of the heart, potentially a TOE, a trans-esophageal echocardiogram. Again to look at the damage that has been done to the heart, how significant is it?
For example, ejection fraction needs to be determined as part of the ultrasound or echocardiogram or trans-esophageal echocardiogram. Ejection fraction gives you an indication of how good or how bad the contractility of the heart is. Because if she already had a weak heart, as you said, you know, it’s really important that the ejection fraction will be determined which you know also means if ejection fraction is low, it would, for example, determine if your mother needs certain, inotropes or vasopressors.
Now she most likely is already on inotropes or vasopressors for sustained low blood pressure after cardiac arrest. She would have been started on norepinephrine or noradrenaline, potentially adrenaline or epinephrine and if her heart is really weak, she would also be on medications such as Dobutamine or milrinone or maybe dopamine. Again, those are inotropes or vasopressors and they are considered life support as mechanical ventilation is considered life support. And with life support being commenced, patients need to be in intensive care.
So then, the next step is with the induced coma and she’s not waking up. Sometimes, it takes a few attempts to wake up. Now let’s just run through two scenarios here. Let’s just say the first scenario is your mom has brain damage, she has brain damage and she’s not waking up, it could be part of the brain damage. If your mom doesn’t have brain damage and she’s not waking up. The situation is probably most likely looking similar to this stage but we don’t know whether there is or there isn’t brain damage.
Waking up after an induced coma can take time and if your mom is waking up and she’s confused, there is no way to determine whether the confusion is part of the induced coma or part of the brain damage that needs to be determined by follow up CT scans by a neurologist, examining your mom and so forth. You know we have written extensively about waking up often after induced coma and patients are often confused after an induced coma anyway and it’s got nothing to do with brain damage. It’s just a side effect and people after days or sometimes weeks they come around and they function normally if they have been confused often after induced coma.
So it’s way too early to determine whether your mom is having permanent and irreversible brain damage because you haven’t spoken about any of the evidence that is needed, which is again CT scan, MRI scan of the brain, and also the opinion of a neurologist.
RECOMMENDED:
Next, let’s just say your mom isn’t waking up and she can’t come off the ventilator so she’s not waking up. She can’t come off the ventilator because she wouldn’t be able to protect her airway. Let’s just say that’s the case. After about 10 to 14 days on the ventilator, your mother would need a tracheostomy if she can’t come off the ventilator because she’s not waking up, she’s not obeying commands, she’s not protecting her airway.
So the next step would be a tracheostomy. If your mom ends up with a tracheostomy, you would buy her all the time to recover in her own time. So that’s important for you to know and understand. A breathing tube is very uncomfortable because it’s in the mouth, whereas the tracheostomy sits on the neck and it’s just so much easier to tolerate and it would give your mother all the time in the world to recover in her own time, go onto a rehab, being weaned off the ventilator, but most importantly, she could then come out of the induced coma because most of the time an induced coma is needed for a breathing tube because it’s so uncomfortable. Whereas a tracheostomy is comfortable and easy to be tolerated.
RECOMMENDED:
Another thing that can happen if there is brain damage and waking up out of sedation, sometimes jerking movements, or seizures can happen. So again that would be unfortunate, but again, I have seen this before and if there is brain damage, the risk for seizures is definitely increased. And again, you’ve got to look out for that. If there are seizures, they will need to start your mother on anti-seizure medications such as Keppra, Phenytoin, and a few others. But again, you’ve got to look at that.
So then looking at the outlook going forward, again Harold, sometimes it can take weeks or months to wake up after an induced coma. It’s got very little to do with brain damage. It’s got everything to do with being critically ill and you know, the body simply needs to recover and the brain, including the brain and that means, waking up can be prolonged, and it often is hard to say whether there is or there isn’t brain damage when patients are confused or not responding, you know, it could be a combination of both.
But time in this situation is the ultimate healer. Also, it also depends on what you or your mother determined. Even before this event, what you would consider as an acceptable quality of life. Let’s just say your mother has brain damage but she still wants to live and you want her to live, you know, then you should advocate for her to live, you know, because that’s your right, that’s what you want. That’s what your family wants, that’s potentially even what she wants.
So, you know, from that perspective, having the intensive care teams say you need to make decisions. Well, I think the only decision you need to make is to wait how your mother recovers and timelines don’t really matter as long as you’re patient and you are prepared to put in the time and the effort it takes to get your mother through this, even if she may not fully recover.
RECOMMENDED:
So, you know, don’t let the intensive care team pressure you because it’s your mother. It’s your decision. It’s not their decision. Their job is to help your mother get through this. So you know, don’t let them pressure you. It’s your decision. Stand your ground and you know, we are here to help you with that. Again, you have rights and we can make sure those rights are being followed on. Again, that’s our job as advocates and consultants for families in intensive care.
So then let’s just say your mother ended up with a tracheostomy and you know, is still not waking up. Then she could go onto rehab if she doesn’t need a tracheostomy, hopefully. And she can leave ICU, she would probably need some, some level of rehab probably in neurology rehab. And again, there is no hard to say at this point in time can she fully recover, can she not fully recover? But nevertheless, it’s worth doing that rehab because you want her to live and she most likely wants to live.
So you’ve got a little bit of a steep climb ahead here. But you know, nothing that certainly I haven’t seen before. Nothing that you know, intensive care teams haven’t seen before. But your biggest challenge now is to keep advocating for your mom because the recovery will take time. And I know agendas of intensive care units, their agenda often is, you know, whenever there’s a significant critical illness with an uncertain outcome, that is the intensive care team’s worst-case scenario because they might look after your mom for an indefinite period with an uncertain outcome and they simply don’t want to invest the resources, the beds, the money, the staff to get through treatment with an uncertain outcome. And that’s the dynamic you need to be aware of and that’s the dynamic you’ll need to mention. You need to manage.
RECOMMENDED:
Also, if asked for a family meeting, the bottom line is they would probably put pressure on you to stop treatment. My advice for any family meeting for families in intensive care is don’t go to a family meeting unless you have two things in place. Number one, a written agenda in writing. And number two, have an advocate there with you like myself, either in person or over the phone. So because I know what they’re going to say in a meeting and you need to be prepared for it. If you’re not prepared for it, they will walk all over you. It’s as simple as that. Because you haven’t seen those situations before. I have been in hundreds of family meetings in intensive care. I know the dynamics, I know what to say. I know when to say it, I know how to say it. So you can actually get the best care and treatment for your mother. So if you’re not prepared for that, the intensive care team will have their agenda being pulled through and you wouldn’t even know that it’s happening until it’s too late.
RECOMMENDED:
So I really hope that helps, Harold. I know we’ve got a phone call lined up soon and we can discuss more of the things that we spoke about in detail, but I know that we can help you buy all the time in the world with your mother in intensive care because we can advocate on a clinical level and we can ensure your mom can have the best care and treatment.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!