Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
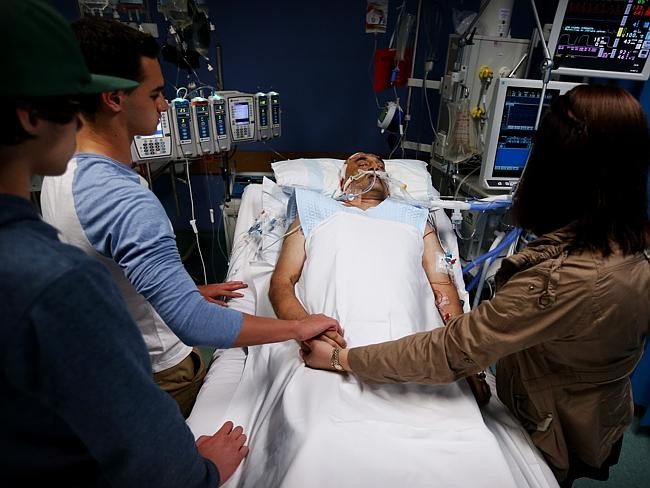
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the questions from one of my clients Peter, as part of my 1:1 consulting and advocacy service, asking why the ICU team has not informed him early that his Dad in the ICU is having end stage renal disease.
My Dad in ICU is having end- stage renal disease! Why has the ICU team not informed me earlier?
Hi Patrik,
Dads making some progress: kidneys working again …2-3 liters a day now with Lasix drip and Hydrochlorothiazide drip/dose to remove excess fluid.
Why does Dad need such a large dose for his kidneys?
Generally speaking, how does one transition from IV drip Lasix ~20 mg an hour to pill form after discharge?
However, creatinine 3.1 to 3.7
…I am praying that it won’t go higher anymore.
Dad breathing on his own and awake sitting up on chair bed -but on vent- as a precaution until lungs clear.
BP normal/stable now without meds.
Back on feeding pump.
Doctors aren’t sure if dad has a lung infection or not …sputum culture negative …they stopped antibiotics.
So several concerns continue.
Peter
Recommended:
Hi Peter,
That’s great news!
So, he’s getting 20mg/hour IV Lasix and he’s getting rid of around 2-3 litres of fluids per day! That’s great news, especially if he can escape the dialysis machine because of that!
Given that they’ve started to sit him up in bed with the breathing, they’re very proactive in trying to get him off the ventilator hopefully soon! Not every ICU is that pro-active, that’s great Peter!
20 mg/hour Lasix is a fairly high dose but, in some instances, I have seen up to 80mg/hour! The goal should definitely be to reduce the Lasix as quickly as possible and let the kidneys do their own work again.
In order to do that Creatinine also needs to come down in order for the kidneys to kick back in again. Creatinine of 3.1-3.7 suggests moderately damaged kidneys. 0.6-1.2 are normal Creatinine levels.
High doses of IV Lasix can certainly damage the kidneys and therefore it should only ever be a temporary therapy and never long-term.
Again, as discussed, this week the kidneys is probably the most “forgiving” organ out of all of the major organs such as the heart, lungs, liver, brain and kidneys.
Given time, kidneys often do recover but they need to be monitored by regularly checking fluid intake, urine output and obviously by checking Urea and Creatinine regularly.
Your Dad’s certainly not out of the woods yet, however given that they are “drying him out” so to speak by draining 2-3 litres/day, given that he’s now more awake, given that he’s now breathing on his own and sitting up in bed that’s all very encouraging!
Recommended articles:
Sometimes, when people are severely fluid overloaded and you “dry them out” the lungs often see an immediate effect, which is what I think happened to your dad!
Furthermore, with being so fluid overloaded it didn’t surprise me that when they were lying him down on the ward that he desaturated and ended up in ICU intubated.
Now you can see the opposite effect when starting to make lots of urine in a short period of time!
It might have also helped if they have done a bronchoscopy and suction out any excess secretions.
It probably also helped having him “only” on Propofol instead of Midazolam (Versed) for sedation because Propofol is short acting and Midazolam (Versed) is a long-acting sedative. Therefore, once they stop or reduce the Propofol your Dad should “wake up” relatively quickly. You don’t see that with Midazolam (Versed), because once patients in ICU are on Midazolam (Versed) it takes them a lot longer to “wake up”. Therefore Midazolam (Versed) is for longer-term induced comas.
Related links:
Keep an eye that if they do re-sedate him that they stick with the Propofol.
Given that he’s more awake and breathing on his own it’s probably also a sign that his infection is clear if the samples came back negative.
Also, the combination of fluid overload and an infection in the lungs is a recipe for needing ventilation. Now that everything seems to clear up your Dad’s improving!
Again, normal blood pressure is usually also a sign that there’s no infection. Keep in mind that with draining so much fluid now your dad might become hypotensive (low blood pressure) because of being fluid depleted. They need to keep an eye on that.
Concerns continue for sure as long as he’s in ICU on a ventilator, however when we last spoke, I was very worried about your Dad, because at his age and in such a fragile state you never know.
It sounds like he’s making progress for now.
If he’s breathing on his own and his ABG’s (blood gases), his oxygen saturation, if his chest x-rays are clear, if he can cough and if he can obey commands he should be able to come off the ventilator soon!
Related information:
Keep up the good work Peter, let me know what you need and look after yourself too!
Don’t forget the most important person in all of this and that’s you!
Kind Regards,
Patrik
Hi Patrik,
Dad still on vent until remaining fluid removed from lungs. Dad slept all day yesterday but occasionally opened his eyes today.
RN told me Lasix is being reduced after much water weight removed and lungs clearing and creatinine slowing to 3.8.
MDs want to do MRI (to rule out brain trouble) while on vent and lying flat in bed.
Pro and con regarding whether or not to do MRI…. which will help with diagnosis yet no treatment offered…. which is concerning.
I am concerned about Dad’s sleepiness as well.
Have you seen MDs use any alertness drugs or treatments like Provigil with any success?
Peter
Hi Peter,
When you say your Dad was asleep all day, do you know if he’s still on any sedation such as Propofol or Midazolam (Versed)?
Also, do you know if he’s getting any pain killers such as Morphine or Fentanyl?
If he’s opening eyes, is he making eye contact and/or recognizing you?
Do you think brain trouble needs to be ruled out by an MRI? I.e. is he moving his arms and legs on purpose? Are his pupils equal and reactive to light?
I’m concerned about your Dad’s sleepiness if
- a) he’s off all sedatives and opiates/pain killers
- b) they suspect there has been a neurological event such as another stroke
I have not seen the use of Propofol in ICU, what I have seen is the use of Naloxone for Morphine/Fentanyl overdose and/or Flumazenil for Midazolam (Versed) overdose.
Recommended information:
Therefore, in order to determine why your Dad is still sleepy, we need to look at how much sedation he’s still on or if he’s off it, how much he’s had in recent days. Once we’ve established that then we may be able to determine if a CT or MRI of the brain is feasible.
Also, do you know how well he’s breathing?
I can be available for a Skype call pretty much anytime, but very happy to talk via email if you prefer that.
Kind Regards
Patrik
END OF EMAIL
Peter has been an ongoing client of mine and we spoke regularly over the phone, so here is a phone consultation that has followed after the emails.
Peter: Hello?
Patrik: Hi, Peter. It’s Patrik speaking here from IntensiveCareHotline.com. How are you?
Peter: I didn’t get you too early, did I?
Patrik: I’m still on the night shift, but that’s okay. I’ve got some time to talk. It’s okay.
Peter: What is your situation there? Are you in bed?
Patrik: No, no. My situation for me, it’s 4:00 a.m. at the moment, and that’s okay.
Peter: Oh, Jesus.
Patrik: No, no, no. It’s okay. No, no. Let me explain.
Peter: I gotta learn to … So, if it’s noontime here, I subtract eight hours? Is that how it works?
Patrik: No, six. It’s okay.
Peter: Oh, Jesus.
Patrik: No, no. It’s okay.
Peter: I didn’t mean to …
Patrik: No, no. Let me explain. I am doing one shift a week in ICU, and I’m actually in ICU at the moment at work, and I’m on a break.
Peter: Oh, okay.
Patrik: It’s all good. I’m not in bed. I’m not in bed.
Peter: Alright.
Patrik: So how can I help you?
Peter: Well, you know what happened? Yesterday Dad’s urine output started fading. He was putting out 600-and … Something like that, and I happened to notice his hourly output wasn’t like it usually is, because I watch everything like that, you know?
Patrik: Yeah, mm-hmm (affirmative).
Peter: So, I said to the nurse, when I pushed the call, right? And I say, “You know, I’d like to see … “I’m worried about his kidneys, and what his urine output is.”
So, one nurse kind of boisterously marches in and says, “Don’t worry about his kidneys. His kidneys are alright. He’s putting out enough urine,” or something like that. “His kidneys are okay.”
And overnight last night, his kidneys stopped putting out. Now he’s not making any urine.
Patrik: Right.
Peter: And there’s blood in the urine, and now he’s not making any urine.
Patrik: Right, okay.
Peter: And they say that his creatinine went from 1.1 and 1.2, now it’s 2.-something. 2.-whatever. I don’t know what it is, but …
Patrik: Yeah, yeah.
Peter: So this is what I’ve always worried about him, and they says, “Well, no, we will try to …” They gave in 1500 of saline last night, and it only produced maybe 100 of urine or something. That means retaining fluid, and they say it’s all in his legs, and in his system somewhere, it’s not getting pulled into his circulation, into his … what’s the word they call it? Not getting pulled out from now on, so whatever.
The bottom line reason I called, is because they had said that he was doing alright, and not to worry and all this other … And the doctor told me, you know that Erica?
Patrik: Yes.
Peter: The one you talked with yesterday?
Patrik: Yes.
Peter: She told me this morning, “Oh, well, you know, that he has third-stage kidney disease, didn’t you?”
I said, “Nobody ever told me that.” I would’ve told you that-
Related links:
Patrik: Yeah, absolutely.
Peter: … when I gave you his history.
She says, “Oh, you knew that, didn’t you? It’s in all of his records.”
I said, “It’s not in any discharge summary that I’ve ever seen.” You know, they list your diagnosis. They list all your medical conditions. You know, your discharge?
Patrik: Yeah.
Peter: They didn’t list nothing to that effect of third-stage renal disease. I’d have had him seeing a kidney doctor a long time ago.
Patrik: Right.
Peter: And I did visit one a while back, but not for that. He was for some other reason. Anyway, he was a little dehydrated, because …
This one here, now we got this added to the mix. Now he’s starting to wake up a little bit.
Patrik: Oh, good, good.
Peter: His eyes are open a little bit today. Sitting in a chair. He doesn’t have any strength in his arms yet, but he did tug me a little bit.
Patrik: Right. So he’s-
Peter: Sort of. They took away that seizure medicine yesterday.
Patrik: Mm-hmm (affirmative). That’s probably why-
Recommended:
Peter: Didn’t give it to him last night. Didn’t give it to him this morning.
Patrik: Yeah.
Peter: So maybe that’s helping him too.
Patrik: Yes, for sure. For sure.
Peter: Keppra has the side effect of sleeping.
Patrik: Oh, absolutely.
Peter: But he’s still got some junk in his lungs and stuff, that they’re suctioning out.
Patrik: They do-
Peter: So he’s not out of the woods yet, but …
Patrik: No. They do still suction him?
Peter: Oh, yeah. They’re still suctioning him.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!