Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
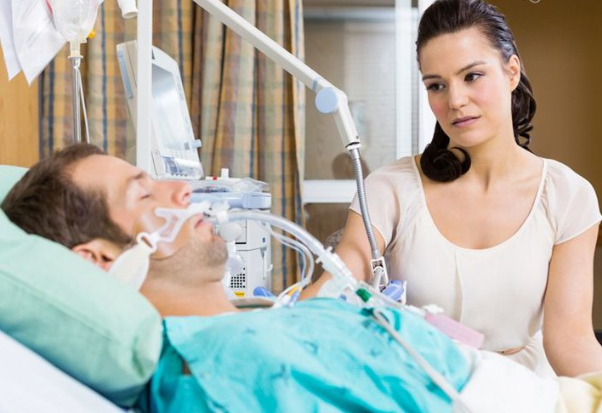
In this week’s episode of “YOUR QUESTIONS ANSWERED I want to answer questions from one of my clients Francis as part of my 1:1 consulting and advocacy service! Francis’ wife had a cardiac arrest and is asking about giving consent to brain death test as per advise by the doctors.
My Wife Had a Cardiac Arrest. Why does the ICU Team Rush to Do the Brain Death Test?
Francis: Hello?
Patrik: Hi. Is that Francis?
Francis: Yes. It is.
Patrik: Hi, Francis. It’s Patrik here from Intensive Care Hotline. How are you?
Francis: Good.
Patrik: I’m just returning your call. Sorry I wasn’t … I was busy earlier. Now, we can talk. You have a family member in intensive care. Is that right?
Recommended:
Francis: Yes.
Patrik: Right. Is it a parent? Is it your spouse? Is it a child?
Francis: My spouse.
Patrik: Your spouse?
Francis: Yes.
Patrik: Right, okay. Why is she in intensive care?
Francis: She went to cardiac arrest, and she didn’t get any oxygen to her brain for … 30 minutes it took for them to revive her.
Patrik: How long ago was that?
Francis: Maybe two days ago now.
Patrik: Two days ago. The cardiac arrest was outside of hospital?
Francis: No, it was at the hospital.
Patrik: Right okay. And they couldn’t resuscitate her to the point where they could reinfuse her brain with oxygen, so you think she had some brain damage, is that what you’re saying?
Francis: Well they just did some testing and they said that those show she has brain damage. They want to do a final test to confirm it.
Patrik: Okay. Did they do a CAT scan of the brain to confirm the brain damage?
Francis: I think they did.
Patrik: You think or you know? Because that’s a really important question.
Recommended:
Francis: I think.
Patrik: Okay. If they’re telling you she’s got brain damage but they haven’t got the evidence, then to me that doesn’t mean anything.
Francis: Okay.
Patrik: How old is your wife?
Francis: She’s 52.
Patrik: 52. That’s very young. Let’s take the evidence aside for a moment, what’s the outlook like they’re telling you? What are their plans for the next 24, 48 hours?
Francis: So their plans are to … Oh, their answer is yes, they did a CAT scan.
Patrik: Okay. You said they did a CAT scan, is that what you said?
Francis: Yes.
Patrik: Okay.
Francis: Yes.
Patrik: Okay. And do you know … have you seen the report? Have they sat down with you and discussed the report?
Francis: Yes. He said they didn’t see … they saw significant damage, right?
Patrik: Okay. And what’s their outlook like for the next 24, 48 hours? What are they predicting?
Francis: Okay so now because of the fact that her kidneys are failing and she keeps excreting some toxins, they want to do something called a brain death test and they wanted some dialysis before they give her the brain death test. But they think that the dialysis may put a little stress on her body, but they need to do the dialysis to remove the toxins so that they can, I guess, read or assess the brain death test.
Recommended:
Patrik: I can tell you that after having worked in intensive care for 20 years, I do understand the brain stem, the brain death test very well. They kidneys have nothing to do whatsoever with the brain death test. You see the biggest problem for families in intensive care is that you don’t know what you don’t know. And you don’t know what questions you need to ask and you don’t know their agenda, and I can already see there is an agenda from their end but we can come to that a bit later. What’s your biggest frustration at the moment?
Francis: My biggest frustration is that I’d like to get the brain death test but I didn’t want to put her under stress and possible have her go into cardiac arrest or any problems with bleeding from trying to get the dialysis done first.
Patrik: Okay. Did you say you don’t want to put your wife under stress for the brain death test, is that what you said? Or did you say you don’t want to put the ICU under stress, I didn’t quite get that.
Francis: I don’t want to put my wife under stress.
Patrik: Okay no, no, that makes sense. Okay. Look, how long was the … Normally when brain damage happens during a cardiac arrest, there is often a time that the ICU refer to as a downtime. Downtime means a potential time where the brain had no oxygen, have they quantified that for you? Have they said it was five minutes, it was three minutes, it was ten minutes. Have they quantified that time for you?
Francis: Well we’ve heard 15 minutes and we’ve also heard three.
Patrik: Okay. Who is in charge of the care at the moment? Because you need to get the facts.
Francis: Okay.
Recommended:
Patrik: It’s not good enough to say you’ve heard. It’s sounding like they’re not very transparent with you. It could be that they’re not very transparent but another missing link is you don’t know what questions you need to ask and you don’t know that there’s potentially an agenda from the intensive care team to tell you one thing, quite frankly to empty their ICU bed as quickly as possible. What’s the ideal outcome that you want?
Francis: Well the ideal outcome that’d I’d like in the situation is to, first of all, make sure that there is everything that needs to be done before we just say … she’s only been here two days so I thought it was moving rather quickly.
Patrik: Absolutely, absolutely. So this happened two days ago which would have been on Sunday, is that correct?
Francis: Yes.
Patrik: Right. And when it happened was he in ICU at the time or did it happen outside of ICU?
Francis: She had it in the emergency room.
Patrik: Okay. And do you know why your wife was admitted to the emergency room in the first place?
Francis: Yes, she got home and she was complaining that she was cold. She had her meal and once she was brought here they said they saw something in her lungs, it kind of looked like it might have been pneumonia.
Patrik: Right. Okay, okay. So the first thing that I can help you with really is, if I was you, I would not consent to brain death testing. Because if you do that, there’s a very good chance … If I was you would get the facts about brain death. From my perspective there’s a CAT scan, so what? Why would you rush into that? As you said before, they need to make sure everything that can be done will be done. And the brain death test is not leading your wife up for that. A brain death test would lead your wife in the complete opposite direction.
Francis: I thought so too.
Recommended:
Patrik: Right. So the first thing that you need to change is you need to change how you interact with them and you need to start asking all the right questions. What’s the rush with end of life? What’s the hurry? This is a life or death situation and they’re just, already, walking all over you. Sorry, I’m a bit blunt here but I’ve worked in the industry for 20 years, I’m talking to people every day of the week in situations like that. I know intimately how ICUs operate, I know their agenda and I know their frustrations. Their frustration is they need beds. The demand on ICU beds is huge, right? The worst case scenario for an ICU is to look after a patient indefinitely with an uncertain outcome. I’ll repeat that because you need … it’s critical for you to understand that. The worst case scenario for an ICU is to look after a patient indefinitely with an uncertain outcome. That’s your wife’s situation.
Francis: Right.
Patrik: And there’s a clear conflict of interests, right? Your conflict of interest, or the conflict of interest is you want everything done for your wife and the ICU is trying to wind down treatment as quickly as possible.
Francis: Well the way they were approaching me, they were telling me that they have enough evidence from the CAT scan and other things to conclusively say she has brain damage and that they didn’t have to do the brain death test, it’s not something they’re having to do, they were doing it as a favour to give us peace about it. And that, pretty much I guess from here, because with the CAT scans and things that they have, they could go ahead and declare him-
Patrik: No.
Francis: That’s how it has been.
Recommended:
Patrik: Are you the medical power of attorney for your wife?
Francis: Yes.
Patrik: Okay, that’s good, that’s good. So the first thing we need to do is we need to change the way you’re interacting with them. The next thing that’s really important to understand, critical, critically important to understand that. You mentioned two important terms now, you mentioned brain damage and you mentioned brain death. Okay. At the first glance, those two terms could be mixed up. Now here is what’s really important to understand. There is no correlation whatsoever between brain damage and brain death. Let me repeat that because, again, it’s so important to understand. There is no correlation whatsoever between brain damage and brain death. They are two completely separate issues. Okay, they’re two completely separate issues. What happens from an ICU perspective is they like to mix the two terms to put pressure on you. Now if they asked you, if they came to you and said, “Oh Francis, would you jump off that bridge tomorrow?” You wouldn’t jump off that bridge. So now they’re telling you, “Oh you need to consent to this, this, this and this and we need to do brain death testing blah blah blah.” Your response to that needs to be no, they can’t force you to do anything.
Francis: Well what we were concerned with is if we don’t do it what happens next?
Patrik: No, no. So I’ll tell you how we can help, right? So we provide a consulting and advocacy service for families and because we know intensive care inside out and we know the politics, we know the dynamics, we know the agendas of ICUs, we can help you with that very quickly. We can guide you with that very quickly, we can make sure that your wife will get best care and treatment, no brain death testing until you agree to that. Until you’ve had time to digest everything that’s happening. You haven’t even had the time to digest everything that’s happening. At the moment you only know 10% of what’s happening.
Francis: Right.
Recommended:
Patrik: They’re painting this picture very one-sided to you without … what we need to do from our end, we need to spend another half an hour on the phone and we need to go through everything that’s happening and then we need to talk to the doctors and we will ask some questions. Your biggest challenge at the moment is you don’t know what questions you need to ask, you don’t know the terminology and you can’t make a clinical argument. What they want is they want to do the brain death testing as quickly as possible, then they want to declare your wife brain dead, then the next step is they want to harvest her organs and let her die. I’ve seen it dozens of times, I know exactly which boxed they’re going to tick.
Francis: So what do we need to do?
Patrik: Yeah, so what we need to do is, as I said, the first thing that we would need to do is we would, you and I, need to get on the phone and talk more about what’s exactly happening and we need to talk about how you need to position yourself in there, how you need to change the way you communicate with them. We will look at very specific questions that you will need to ask and then the next step is you and I would have to get on the phone to the doctors and we will, you know, challenge them on everything that’s been happening and we will make sure that your wife is getting standard care and treatment. And if in four or five days there is no improvement, fair enough, then let’s look at other options. But for now, stopping and withdrawing treatment and doing the brain death testing is highly inappropriate. There is no evidence besides the CAT scan. You know a CAT scan doesn’t mean anything, the reality is in the first CAT scan after an event like this, most of the time all they can see is swelling, right?
Francis: She said that there may not be a problem.
Patrik: Say that again?
Francis: She said that what they found can be wrong.
Recommended:
Patrik: Right, right. So besides the swelling they probably can’t see anything. I would really like to talk to them and find out on what basis they want to do the brain death testing. So where to from there? If you want me to help you with that I do charge a fee, I need to be clear about that, but I do believe your wife is in a life or death situation. If you don’t know how you need to conduct yourself and how you start to ask the right questions and push back on them, they will walk all over you.
Francis: Okay so what is the fee?
Patrik: So I have a number of options, sometimes I do some travelling when people ask me to work with them one-on-one in person, then my daily fee is like $5000 but I have phone options and I know I can help you over the phone. I have a seven day option that gives you seven days unlimited access to me over the phone 24 hours a day including talking to the doctors, talking to the nurses or potentially a social worker, whoever else is involved in this process at the moment. You don’t have to use that seven days in a row, you can use it at your own pace, that’s for $699. I have a four day option for $499 and I have an hour option for $119. And that one hour option can be credited towards the four day and the seven day option if you wanted to proceed with that. But I do believe that in an hour we can achieve a lot. Because at the moment you’re, from my perspective, they’ve got the upper hand and they’re doing what they’re doing with every family in a situation like that who doesn’t know what needs to be done in a situation like that.
Francis: So in the case that we’re in now, that we have limited our options if they start it in the case like we’re already in now.
Patrik: Say that again please?
Francis: If I took the hour option to start from tomorrow they will still be coming to me in the morning and start this whole test.
Patrik: No, no. You would have to give consent to that, right? You would have to give consent to that, that’s number one. Number two, once we start the consulting process and the advocacy process we will go back to them and we will ask for certain things, we will ask for evidence and we will also ask you on a policy level. You see one thing, they’re telling you things at the moment but what they’re not telling you is how they make those decisions. And they need to follow protocols and processes to make those decisions and we will argue on that level. Have they followed those protocols and policies? And there’s a good chance they haven’t. That’s how we will argue.
Francis: Okay.
Recommended:
Patrik: But you see, in a situation like that Francis, they’re talking about brain death. I have an understanding now that your wife’s kidneys are failing but from my perspective, also from my experience, the kidneys have nothing to do with the brain. It’s a completely separate issue. It’s another organ, right? And it’s got nothing to do with the brain death. And I can’t stress that enough. They’ve done one CAT scan of the brain. Nine times out of 10, the first CAT scan of the brain after a cardiac arrest, it doesn’t show anything besides swelling, right? Do you know if your wife is on sedation? Do you know what I mean by that?
Francis: No I don’t know if she’s on sedation.
Recommended:
Patrik: Right, do you know what I mean by that?
Francis: Yes. It’s a.. they are using something to keep her sleepy.
Patrik: That’s right, that’s right. Do you know whether she’s on that or not?
Francis: No, I don’t.
Patrik: You don’t, okay. That’s another thing that we’d have to find out because if she’s on sedation and she’s not waking up, that’s masking everything that’s happening. See this is why I keep saying you don’t know what you don’t know, you don’t know what you need to look for and you don’t know what questions you need to ask. They’re giving you a very one-sided picture. Because intensive care is such a complex area and it’s such a specialised area, I would really want to know what medications is she on. What else have they done besides the CAT scan? It doesn’t sound like a lot has happened besides the CAT scan and that’s not enough evidence to even think about brain death. Are they very busy in that unit? In that ICU? Is that a busy place?
Recommended:
Francis: Yes, it’s very busy.
Patrik: Right, right. And who is in charge of the medical care? Is it an ICU doctor? Is it a neurologist? Is it the cardiologist? Do you know?
Francis: We’ve seen a neurologist, also we’ve seen a cardiologist.
Patrik: Okay. And do you know who’s the main driver behind all of this?
Francis: No.
Patrik: Right. Have they had any formal meetings with you?

The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!