Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Dad in LTAC Won’t Be Discharged Home Because Of Yeast Infection. What Causes This Infection?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“ I want to answer the succeeding questions from one of my clients Peter as part of my 1:1 consulting and advocacy service where Peter is saying that his dad’s doctors agreed not to do anything, however Peter now has second thoughts and he’s asking if they want to withdraw treatment on his Dad
My Dad was Transferred Back to the ICU Because of Congestion. Why Does the ICU Team Withdraw Him from Treatment?
“You can also check out previous 1:1 consulting and advocacy session with me and Peter here.”
Patrik: You’re most welcome. Let me know if you get stuck, if you want me to talk to the doctor, please let me know.
Peter: All right. I have to wait a minute. Looks like the elevator’s here now. I’m heading up to see him and I’m going to get pounced. Doctor’s going to pounce right on me, soon as I walk in the door. Anyway, I’m going to argue for him to, for him to get those treatments at home and for the, they’re going to be stubborn. All right, I got to go, I got the doctor here.
Patrik: Okay.
Peter: I’ll see you, thank you.
Patrik: Okay, you’re most welcome.
Peter: All right, thank you.
Patrik: Thank you.
Recommended:
Patrik: Hi, Peter. How are you?
Peter: How you doing? How you doing?
Patrik: Very well, and you?
Peter: I guess so. Pat, do we have one or two more days under our-
Patrik: Yes. Absolutely. Okay. What’s going to happen with my …
Peter: This guy’s an intensive care nurse and he helps families.
My mother’s here.
Patrik: Right.
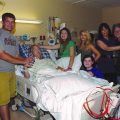
Peter: You know, my father, he’s sort of in a bad position right now. His kidney started working, just ready to go home, and then he got another infection and his temperature dropped. This is a couple of weeks ago.
Patrik: Right.
Peter: He looked good too, and then he started … and then to make the long story short, he’s in and out with his urine input and they tried Lasix and he was… Lasix always helped him.
Patrik: Right.
Peter: And I don’t think they know what they’re doing in here. Right now, if the Lasix doesn’t work anymore and his urine output is almost zero-
Patrik: Right.
Peter: And the kidney doctor says “Well, we’d like to give it time to let the kidneys heal.” Which makes sense but he also apparently has a lung infection, so they got him on a vent just to help him breathe easier but … his saturation aren’t bad, but once in a while he gets … he got this fluid building up because it’s got no place to go.
Patrik: Right. Can you-
Peter: They don’t wanna-
Patrik: Can you just remind me? Last time when we spoke, you said you wanted to send your dad to another facility. Did that happen?
Related Links:
Peter: Well I was thinking of VA, Veterans Hospital, you know.
Patrik: And did that happen?
Peter: But they didn’t have any beds in the intensive care unit.
Patrik: Okay.
Peter: It was just a few days ago though. But what instead, I’m getting a second opinion tomorrow from another one of their doctors.
Patrik: Okay.
Peter: I have a funny feeling … it’s somebody I think that this doctor currently picked, and I have a funny feeling that they’re going to be chummy and they’re going to stick together and-
Patrik: Most likely.
Peter: Long story short is they don’t want to do anymore for him. They put him on dialysis to get the fluid off.
Related Articles:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: Right.
Peter: They don’t want any other … because they’re afraid of that. And then she says it’s to where they’re doing him more harm, what we’re doing is cruel, not letting him go.
Patrik: Sure.
Peter: He keeps trying to… We’re told we’re causing more torture. We’re torturing him and we should let him go in other words.
Patrik: Can I just ask, Peter, is he still in the same hospital than when we spoke last time?
Peter: Oh yeah.
Patrik: Okay. Is he in intensive care?
Peter: Yup. He’s in the medical intensive care.
Patrik: And how long has he been there now?
Peter: Almost 2-3 weeks.
Patrik: Okay. So why did he go into intensive care? Just clarify that for me please, because the last time when we spoke, he wasn’t in intensive care.
Peter: Right. He went back because of his breathing and congestion and-
Patrik: Okay.
Peter: And the fact … has a history of, when he gets these illnesses, his blood pressure drops and then he can’t handle that on the floors.
Patrik: Right. And can I clarify, so they had him on dialysis? Now they’ve stopped dialysis?
Peter: No. They don’t want to put him on dialysis.
Patrik: I see. I see.
Peter: They’re refusing to do it.
Patrik: But his fluids keep building up?
Peter: Well right now I don’t see anything, and his ankles don’t look swollen.
Patrik: Okay.
Peter: His hands don’t look swollen but I guess apparently though, it’s getting into his lungs.
Patrik: It would. It would.
Peter: Although some of the staff they’re suctioning out is kind of thick white mucus or something there.
Patrik: Right.
Peter: They’re taking that… A lot of it could be that. I’m telling you, he did pretty well for a couple of days. His sats came up to 98 but then today they went back down again. Plus he was on Keppra. That kind of knocked him out the last time he was on it so I asked them if they could cut it down. Cut it in half anyway. So, they did that because when they raised his Keppra dose, that really knocked him out a couple weeks ago. So-
Patrik: Right.
Suggested Articles:
Peter: I remembered that. I saw that. “Okay, we’ll cut the Keppra in half.” He was kind of awake at certain times of the day today. Yesterday he was sleeping for the last three days.
Patrik: Right.
Peter: You know, for me … I guess Keppra was knocking him out.
Patrik: Yeah, it would. It would.
Peter: Which I think, adds to the problem.
Patrik: Yes. And what …
Peter: And … so now they’ve … I mean, now that he’s a little bit more on and off … he opens his eyes, and hopefully tomorrow he’ll be better as that concentration comes down of the Keppra. But he’ll be more sensitive though to these twitches he gets in his right shoulder. He gets these twitches from … that’s why they give him the Keppra, to control the … they call it “myco” or “muco …” you know what that’s called?
Patrik: Micro-seizures? Or myoclonic jerks?
Peter: No no no.
Patrik: Myoclonic jerks?
Peter: Yeah, that’s the word. Microclonic.
Patrik: Right.
Peter: Myoclonic.
Patrik: Myoclonic jerks. And what’s your exact question? What’s your exact concern?
Peter: Well, my concern is … I’m at the point where I have a funny feeling that this doctor’s gonna just green stamp her other compadre, and not agree to do anything.
Suggested Links:
Patrik: Yeah, yeah, yeah, yeah.
Peter: They don’t want to do anything more.
Patrik: Right, have they …
Peter: I’m thinking if I should …
Patrik: Right.
Peter: If they do that, then I’m going to push to get him out of there.
Patrik: Okay.
Peter: Yeah, yeah.
Patrik: Now have they talked about DNR?
Peter: Yes, yes.
Patrik: And what’s the status around that?
Peter: Well we don’t believe in that.
Recommended Informations:
Patrik: And has it been … is he DNR?
Peter: No, no.
Patrik: No. Okay, good. Good.
Peter: I’m his healthcare proxy.
Patrik: Okay, good. Good. And you haven’t signed anything.
Peter: No, no, no.
Patrik: Good. Good. So, do you know what other medications he’s on at the moment, and do you know what ventilator settings he’s on?
Peter: He’s on spontaneous, so he’s breathing on his own.
Patrik: Okay, good.
Peter: He’s breathing on his own with a little bit of an assist. The respiratory tech told me they kind of help him to push out the air so that he doesn’t have to struggle to push the air down the hose. Down the hose that he has to breathe down, you know.
Patrik: Absolutely.
Peter: Yeah, I don’t know his exact settings but …
Patrik: Okay.
Peter: I know that he’s … well they had him set to 60 … he was on 40% O2, but his sats kind of dropped down so they put him back up to 50 or 60.
Patrik: And that’s temporarily.
Peter: Temporarily.
Patrik: Okay, temporarily, okay.
Peter: And then 97 O2 are the sats now. And his CO2’s been about 45%, which is good.
Patrik: Yeah, that’s all right.
Peter: Yeah, I didn’t see the other settings like volume settings and all that. And then he’s on some … what the hell is it called … a couple of antibiotics.
Patrik: Still. Okay.
Peter: I took a picture of them.
Patrik: Right. Do you know whether he’s on any medications to support his blood pressure?
Peter: Yes, he’s on that … what’s it called …
Patrik: Norepinephrine?
Peter: Yes. That’s it.
Patrik: Okay. How long has he been on that for?
Peter: Yeah, I’m looking at it right here. Norepinephrine. I got a picture of it.
Patrik: Okay, if you can email it, that would help. How long has he been on the norepinephrine for?
Peter: A couple of days.
Patrik: Okay. Okay.
Peter: I got the settings of the machine. The settings I’m looking at it right now. What settings would you like?
Patrik: How much oxygen?
Peter: Well it was to 40, now it’s up to 50 or 60.
Patrik: Okay. Can you see a PEEP? P, double E, P, can you see a PEEP?
Peter: Yeah.
Patrik: What’s the PEEP on?
Peter: That was yesterday. Yesterday was 7.9.
Patrik: Yeah. And what’s today?
Peter: I don’t know. I didn’t get today’s picture.
Patrik: Okay. Peter, here is what I can see just by what you’ve shared with me. Given that he’s back on the ventilator/breathing machine –and sorry, and just to clarify, he’s back on the ventilator 24 hours a day, is that correct?
Related Articles:
Peter: Yeah, but it’s set to “spontaneous,” so he’s driving it.
Patrik: Yes, of course. He’s driving it with support. So, if he’s on the ventilator 24 hours a day, even spontaneously, and if he is on the norepinephrine, the norepinephrine and the ventilator are two major forms of life support, right? So, what I’m saying is, at this stage, he wouldn’t be able to leave intensive care. You can get him into another hospital, to intensive care. There’s no doubt about that. But with the life support that he’s on, he wouldn’t be able to leave intensive care at this point in time. The norepinephrine can only be given in intensive care.
Peter: Right, but the only reason he’s getting it, though, is because they want his pressure up high enough so that he can make urine.
Patrik: Correct. Correct.
Peter: They’re trying to get his pressure. But his pressure’s low because at the same time, they’re starving him of water. They’re not giving him, they got a hole and … all he’s getting for … what do you call it … all he’s getting for water is just the food that he’s drinking. It’s like, maybe 800 of some Nephro … you might have it, It’s for dialysis. Nephro something. But they’re giving him hardly any water.
Patrik: Okay.
Peter: So normally he’d be getting like, 800 of water on top of the 800 of food, you know?
Patrik: Yeah. You know what they’re doing, Peter? Given that he’s on the ventilator and that his oxygen requirements are going up–50% is sort of … it’s not great. But what they’re probably doing is, they want to keep him dry because for most patients, that they want to get off the ventilator, they want to keep them dry to keep any fluids off the lungs, because if you want to wean somebody off the ventilator, you can’t have wet lungs. I think that’s what’s probably happening. Does that make sense?
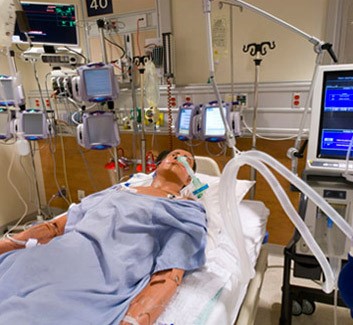
Peter: Oh yeah, yeah, I understand that. But what I’m getting at though is that he’s been off that ventilator many times. And I think if we can get him to clear that stuff out of his lungs and get his kidneys running or dialysis or something, then all that would reverse. You know, he wouldn’t need the ventilator because they can give him more fluids as needed, and get his blood pressure up naturally, you know?
Patrik: Yeah, agreed. Agreed. But …
Peter: You know, that’s my thought, but …
Patrik: Yeah. But there’s another thing, Peter. If he’s getting antibiotics, he must have an infection of some sort. Do you know where that infection is?
Peter: Well, they cultured something in his lungs.
Patrik: Okay. So … okay, right. So, there are two things number one, if he has an infection in the lungs, which might contribute to him needing more oxygen. And number two, an infection is also known to cause low blood pressure.
Peter: Yeah, right.
Patrik: Right. So, at this point in time, with everything that you’re describing, it’s like a catch-22. You’ve got on the one hand, they want to keep the kidneys perfusing. On the other hand he’s got some sort of chest infection, which means you want to keep the lungs dry. Right? So, it’s a catch-22, and balancing that out is fairly difficult. How much norepinephrine is he on? Can you see that?
Recommended:
Peter: Yes. I’ll give you the dose right here. It says … this was yesterday, but 7.2 milligrams …
Patrik: Per hour?
Peter: 7.2 milligrams per hour.
Patrik: That’s sort of an average.
Peter: 7.2 milligrams an hour.
Patrik: Right. That’s sort of an average. Right. That’s sort of …
Peter: And then it says 26.39 hours, not minutes.
Patrik: Right. Right.
Peter: So, I guess it’s 26 hours, 29 minutes.
Patrik: Right. Right. I guess …
Peter: And then it has the volume to be delivered, VTDI, right?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is PatrikHutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!