Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
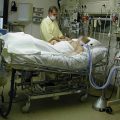
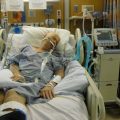
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the questions from one of my clients Peter, as part of my 1:1 consulting and advocacy service, saying that his intubated dad is having airway swelling and the ICU team is rushing for his Dad to have a tracheostomy.
My Dad in the ICU is having airway swelling. How come the ICU team is rushing him to have a tracheostomy?
“You can also check out previous 1:1 consulting and advocacy session with me and Peter here.”
Peter: Yeah.
Patrik: Hi Peter. It’s Patrik here of intensive care hotline. Is that better?
Peter: You know what I was gonna try? See I’m on the hospital …
Patrik: Right.
Peter: … router system. I just disconnected from it and I’m thinking maybe that’s why it didn’t work. But we did it the other day and it didn’t work so I don’t know.
Patrik: Right.
Peter: So let’s just stay here.
Patrik: Right. Okay. All right. So I’ll just repeat what I said when you probably couldn’t hear me. So from my perspective … Did you hear what I said about the steroids?
Peter: Just basically I heard it, and we got cut out for about a minute.
Recommended:
Patrik: Okay.
Peter: You can give the steroids a chance and then maybe you wanna … they’re them a chance. They don’t wanna spend the time of them on the steroids.
Patrik: And that’s so bad. They are pushed for beds, and what they wanna do is they wanna take the easy way out, they wanna do a tracheostomy and send him on maybe to a long term weaning facility, you know, want to send him home, rather than doing what’s right for him. A tracheostomy is just another layer of complexity that he doesn’t need. If everything fails, fair enough, but at least they’ve tried.
Suggested link:
Peter: He has glaucoma though, don’t you have to watch steroids if you’re on glaucoma medicine? Isn’t that so?
Patrik: Yeah, steroids can be given for a number of things including … patients who have sepsis, they often get steroids. Patients with cancer often get steroids. So steroid use is fairly common in ICU.
Peter: What about glaucoma though? I thought it was, you shouldn’t get steroids if you have glaucoma.
Patrik: Probably not. Right. Is your dad having glaucoma?
Peter: Yeah he’s got bad glaucoma.
Patrik: Okay. Well that’s probably a good point. At the same time this is, and it’s probably something you’d have to discuss with the doctors, if it were for your dad to get steroids for a few days and avoid the tracheostomy, would that be worth the effort? I see a tracheostomy as something that should only be done as a last resort.
Peter: Yeah. The way I was sort of explained was that it would be just sort of an emergency.
Patrik: Right.
Peter: They’re not sure. They were worried about getting that tube back down his throat because they had trouble getting it in at first. The exam room was kind of a little bit torturous. They said that they were concerned that, you know, trying to get it down again.
Recommended articles:
Patrik: Yep. And that is a concern.
Peter: And that they wanna have that as a safety. I mentioned the prednisone. And they mentioned a couple of other things about why they didn’t want to do cortisone. Something … forget what they said.
Patrik: Sugar? Sugar issues?
Peter: I’m thinking the reason …
Patrik: Is your dad, is he a diabetic?
Peter: I don’t know.
Patrik: Is your dad a diabetic?
Peter: I don’t know
Patrik: Is your dad a diabetic? Can you hear me? Peter, can you hear me?
Peter: Yeah, I gotcha. I can hear you now. The speaker got disconnected.
Patrik: Right. Is your dad a diabetic? Does he have diabetes?
Peter: Yes.
Patrik: He does. Okay that …
Peter: It’s well controlled though.
Patrik: Right. That could be one of the reasons why they don’t want to give the steroids, because steroids increase the blood sugar levels.
Peter: Oh, is that right?
Patrik: Yeah. Yeah.
Peter: There’s one other thing they mentioned too.
Recommended links:
Patrik: Sorry?
Peter: I don’t know if had to do with …
Patrik: I can barely …
Peter: There’s something else they mentioned about steroids.
Patrik: Right. Right. The main side effect of steroids are really high sugar and you know, sometimes the skin can get a little bit irritated. Other things that I think … you know, I mean, you mentioned, it’s only been an hour, isn’t it? That they told you with the airway swelling, is that correct?
Peter: Say again.
Patrik: They only told you an hour ago, about the airway swelling. Is that correct?
Peter: Yes. Yeah, they said it happened yesterday.
Patrik: Right.
Peter: When they decided to wean him … decided to see if they could get him off of the machine and they worried that if he … plus the fact they say, he needs a little bit of an assist. Like, the machine kind of makes him breathe in and breathe out a little better. Even though he’s breathing on his own, the machine kind of helps him a little.
Patrik: Oh yeah.
Peter: And they just worried if they take it away, they don’t want to be caught not having anything there, you know?
Patrik: And I agree with that. And I agree with that. However, what needs … you know, the airway swelling could come down just by waiting a couple of days. All right? That could just happen by waiting another couple of days. If I were you, Peter, I wouldn’t rush into a tracheostomy. I just wouldn’t.
Related Info:
Peter: No.
Patrik: You know? It could.. A tracheostomy can wait for another week, right? I mean, the goal should always be to get somebody off the ventilator without doing the tracheostomy. That should always be the goal.
Peter: But see, they’re worried that if they try and take him off, he might do okay they said one day or so, but they’re worried that he might go down this road again with the breathing difficulty and with the sleep apnea they say he has, where he stops breathing. Central apnea. Where he’s, like they said yesterday, he stopped breathing for a full minute.
Patrik: Right, right.
Peter: He didn’t breathe. And the machine had this … they had to turn on a machine and get him … ’cause normally that happens if he’s in a like, a deep sleep.
Patrik: Yeah. Yeah.
Peter: You know? But the machine we have at home, we have a VPAP. I don’t know if you’ve ever heard of VPAP.
Patrik: I have. I have.
Peter: It’s more advanced than a CPAP. It’s more advanced then BiPAP.
Patrik: Yeah.
Peter: It actually breathes eight times a minute if you don’t breathe.
Patrik: Yeah.
Peter: It’ll give you some breaths if it doesn’t sense you breathing.
Patrik: Yeah. I know you mentioned that.
Peter: But anyway, we have that up tonight. That’s a nice machine we have, for that purpose.
Patrik: Right, right. And look Peter, you’re probably right that … you’re probably right that there is a relatively high chance of your dad might need a tracheostomy down the line. But until you’ve sussed out all the options, you know, a tracheostomy is often permanent, especially at your dad’s age. So that means he might find himself in a position with a tracheostomy, where he might not be able to talk for the rest of his life, and where he might not be able to eat or drink for the rest of his life, right?
Suggested links:
Peter: Well he can’t eat or drink.
Patrik: He can’t?
Peter: No.
Patrik: Well of course not. But I mean, imagine you’re living, you can’t talk, you can’t eat and drink.
Peter: Yeah. Well he … he could … oh, I thought the people with trachs put their finger over their trach to talk.
Patrik: That is often an option, but it’s a matter of, are they strong enough to overcome that resistance to talk? Because there’s a lot more resistance to overcome in order to talk once you have a tracheostomy, compared to if you don’t have a tracheostomy. You know? It’s much more …
Peter: Why? What does the trach …
Patrik: Much more difficult.
Peter: What does a trach look like?
Patrik: I can send you a picture. I’ll send you a picture once we come off this call.
Peter: Okay. I mean, ’cause it’s … I thought it was just sort of like, a hole that they put a little plastic adapter in. That allows them to hook up the ventilator.
Patrik: Right. What it is, Peter, it …
Recommended article:
Peter: Go ahead now.
Patrik: It looks like, it’s similar to a breathing tube. It just, it’s similar to a breathing tube, but it’s just in the neck instead of in the mouth. Right?
Peter: So, so I don’t understand. Does this tube block anything from above coming down?
Patrik: Yes, it does.
Peter: Well yeah, I suppose it would have to, because you’re not supposed to get … so when he tries to talk, that won’t block his talking ability, right?
Patrik: Well the problem is that with a tracheostomy, the vocal cords don’t work most of the time. They’re paralysed, more or less. The majority of patients with a tracheostomy can’t talk.
Peter: I thought they put their finger over the trach and they …
Patrik: Yep. Is your dad … okay, can your dad move his fingers so that he could put pressure on his tracheostomy? Do you think he’ll be able to do that?
Peter: No. He’s really weakened, you know, he’s a poor guy. He’s been through so much. He was pretty awake today though. You know? I mean, he’s trying to lift his arm a little for me. But he’s just been so run down.
Patrik: Right.
Peter: For the foolishness from some of these workers in here. You know, the ones that took out the catheter, you know, put the catheter replacement, caused all that bleeding. It set down for two … for three days he was in bed. Four blood transfusions.
Related links:
Patrik: Right. Right.
Peter: I don’t know.
Patrik: Look. I think there’s a very high chance that your dad might need a tracheostomy, but I still think it’s way too early to make that decision. Unless they have maximised … you know, unless they’ve tried really hard to get that breathing tube out, you know, I’m almost bound to say “wait.”
Peter: Well they talk like it’s not a big deal to take it out. They’re worried about if they have to get it back in if he can’t breathe.
Patrik: Yep. And that …
Peter: They’re very worried about taking it out.
Patrik: Yep, yep. And that’s a concern. And look. I’ll tell you my concern. Most … if your dad was much younger, I would say “Yep, let’s do a tracheostomy and let’s … you know, it’ll come out.”
Peter: Mm-hmm (affirmative).
Patrik: I guess … you know, at your dad’s age, there is a risk that he may stay with that tracheostomy for the rest of his life. And I understand where they are coming from. I get that. And there is, you know, I can see why they’re worried. I can see that. You know, but at the same time, if in a couple of days, you know, he’s still sort of not thriving, if the airway’s still blocked, then I’d say “Yep, it’s much safer to have that tracheostomy.” But my concern would be..
Peter: I want to take..
Patrik: Go on.
Peter: I was wondering if they could use the inhalers with the cortisone.
Patrik: Very much so.
Peter: You know, the … spray inhalers.
Patrik: Yep, the nebulizer.
Peter: Yeah, that, but the local stuff, you know?
Patrik: Yeah.
Peter: Other than the systemic prednisone. Yeah, that might be helpful.
Patrik: Absolutely, it would.
Peter: You know, really want to … what are some of the examples … do you know any examples of the cortisone inhalers?
Patrik: Yeah, I can tell you there are no … just give me one sec. Just give me one sec. I don’t think … just give me one sec.
Peter: That’s okay. I could get these answers from …
Patrik: No, no. So yeah, so you can get hydrocortisone nebulizer, and I will send you that in an email. You can get hydrocortisone nebulizer, but you could also get an adrenaline nebulizer. And again, I will email you that. But I would hope, I would hope that they’re doing that already. That’s what I would hope.
Peter: No.
Patrik: You know, that would be almost standard treatment.
Peter: I don’t know. Huh. Well, I’m just thinking ahead here. Just trying to get some answers.
Recommended links:
Patrik: Absolutely. Absolutely.
Peter: And I’m leaning towards the trach because I’d hate to have to bring him home and then find him going into respiratory arrest and have no way of helping him.
Patrik: Yeah, yeah, yeah, yeah, yeah. Yeah, no no, that, mm-hmm (affirmative). Mm-hmm (affirmative).
Peter: You know, Patrik, that … I mean, they say “Oh yeah, he’s probably …” they talk like “Yeah, he probably could get by on his own,” but they’re worried about, they always say “to a point,” you know? I mean, they’re worried about a withdrawing the tube.
Patrik: What are they worried about?
Peter: Oh, just withdrawing that tube.
Patrik: Yeah, yeah.
Peter: And having him have some kind of a spasm, and not being able to put it back.
Patrik: Yes.
Peter: That’s what they’re worried about.
Patrik: Yes. And that’s …
Peter: And they’re leaving it up to me to make the decision. “Do we pull it or not?” And then it’s like you’re damned if you do, you’re damned if you don’t. And then we say “Well we can’t leave that tube in him too much longer, because that’s irritating his throat.”
Related articles:
Patrik: Well, do you think …
Peter: My father’s chewing on it too, you know?
Patrik: Right. Do you think that it’s irritating …
Peter: He’s waking up and chewing on it. What’s that?
Patrik: Do you think that he’s irritated by the breathing tube? What’s your feeling?
Peter: I think he … he’s chewing on it.
Patrik: Okay.
Peter: The way he woke up today, he was pretty awake today for about an hour or so.
Patrik: Okay.
Peter: On and off. And it looks like he was just trying to get back to himself and he kept biting down with that thing in the way, you know?
Patrik: Right, right.
Peter: And just, I’m thinking that we definitely gotta get that out of his mouth.
Patrik: Okay, yep. No, no, I hear you. I hear you. That’s all fair enough, and in some cases, I’m the first one to advocate for a tracheostomy, you know, I’m the first one to say “yep, a tracheostomy is the right thing to do.” What I … especially with airway swelling, I do believe maybe just waiting a couple of days might solve the problem.
Peter: I’ll ask about that.
Patrik: Yeah, ask them about that.
Recommended information:
Peter: I’ll ask them.
Patrik: Because what you’ve got
Peter: Although he’s gonna be here for a few days anyway, because we gotta wait for the fluid to come off him.
Patrik: That’s exactly right. That’s exactly right. And you know, once..
Peter: So … and they’re gonna have to come by and talk to me first, so I think we got some time going on here.
Patrik: Right.
Peter: We got some time.
Patrik: Good, good, good. And you see, the problem, Peter, is … and I’m dealing with a similar situation with another client at the moment. So you know, once the patient has a tracheostomy, they all want to send them out, right? And once they send them out, they go on to long-term acute care, long-term weaning. You know, but that’s … the word is in and of itself, “long-term,” right?
Peter: Yeah, I want to bring Dad home.
Patrik: Yeah, great. Great. I should be able to help you with that, even. But we could discuss that down the line. And I think that …
Related articles:
Peter: But how could … oh, you mean you’re familiar, I mean, help me with the operating the machine.
Patrik: Yeah, absolutely. Absolutely. But that would be another conversation to have.
Peter: Yeah.
Patrik: I think for now, I think the goal should be to see whether they can get rid of that breathing tube and breathe by himself without any tubes.
Peter: To me, he’s getting better. He’s at 100% oxygen.
Patrik: Great.
Peter: Without any extra … she told me he’s at a 30 or 40% from the machine, breathing on his own at 100%. Now that’s not bad.
Patrik: No, that’s not bad at all.
Peter: Yeah, I’m thinking maybe the tube itself, maybe it causes swelling, you know?
Patrik: Yes. The question that I would have for them is, what size tube does he have? There are different sizes.
Peter: Yeah.
Patrik: So that would be my..
Peter: Well I’m sure that the anaesthesia used the right size. I don’t know.
Patrik: Right.
Peter: They talk like he’s got twisted airway.
Patrik: Right. Well you’d hope that they used the right size. But you know, mistakes happen.
Peter: Yeah, believe me, I’ve seen it.
Patrik: Yeah. Yeah. Mistakes happen. And …
Peter: Anyway, I don’t know. Now people that have a trach, right? Is that stitched into the skin? How does that work?
Suggested articles:
Patrik: Okay. Very good question. So I can tell you what happens here in Australia and I can tell you what happens in the US. In Australia, most tracheostomies are done in ICU by an ICU specialist. And it’s … you know, it’s … for an experienced consultant it’s a 30 minute procedure. And tracheostomies are not stitched in. Now, in most cases in the US, for whatever reason, they take patients to the operating room, and do it in the operating room and stitch it in. Right? So you may want to ask …
Patrik: So you may want to ask how they are planning to do it. Right, right. So you want to ask how they do it, are they going to stitch it in. From my perspective there’s no need for stitching it in. They’re very safe without being stitched in.
Peter: Yeah, so I … and how do they … what’s the word? Are they plastic or metallic?
Patrik: Plastic. I’m sending you some pictures once we come off this call. They’re plastic.
Peter: And just a cap on the end, I take it, right?
Patrik: A cap on the end, or.. In some, you know, a tracheostomy is being used to have a ventilator connected.
Peter: Right.
Patrik: Right?
Recommended links:
Peter: But I mean, when you’re not using it, they were saying that you could use it just for night sleeping.
Patrik: Well, yeah, it depends. It depends. So …
Peter: So I take it you have a cap, right? It’s got a cap on it, right?
Patrik: Yes, but the cap is open. The cap is there to filter the air, because otherwise the cap can’t be closed, because otherwise your dad couldn’t breathe.
Peter: Oh. You mean that the access to the upper airway is totally gone?
Patrik: Very much so. Very much so.
Peter: Why?
Patrik: Well, because people are … they’re generally not strong enough to breathe through the nose or through the mouth, whereas with a tracheostomy, you know, the distance to breathe, to inhale air is much shorter, because it’s basically just taking air in from the neck. But the other issue is, patients are often not strong enough to cough, to protect their airway. And another advantage that a tracheostomy has is, you can suction secretions through the tracheostomy.
Peter: All right.
Patrik: Right. So you got to think about those things as well.
Peter: And what about when he has this … his throat sometimes, he gets some saliva in his throat, what about … where does that go?
Patrik: Well at the moment it’s either going in his stomach or it’s going down his lungs. Either/or. It shouldn’t go down his lungs because the airway is blocked.
Peter: Oh. How do they block off the airway with the …
Patrik: Yep, there’s a balloon. There’s a balloon.
Peter: Oh, and where does the balloon go? Above the … it goes above the trach adapter?
Patrik: Below. Below. If you have a look, I don’t know whether you can access this now. I just sent you some images of a tracheostomy on Skype. I don’t know whether you can … I have to send you that now. I don’t know whether you can access it. You can have a look now if you like.
Can you see it?
Recommended:
Peter: Oh yeah. How come now that communication went through?
Patrik: Look, I don’t … because it’s just sending a picture. I don’t know. Should we try Skype again? It would be much clearer.
Peter: Yeah, go ahead.
Patrik: I’ll try Skype. I’ll just try it now.
Not coming … for whatever reason it’s not coming through. I’ll try one more time. I’ll try one more time.
Can you hear me calling?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!