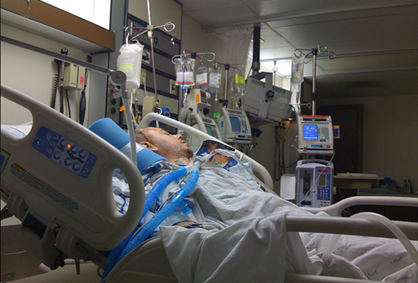
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Joy, as part of my 1:1 consulting and advocacy. Joy’s dad is on a ventilator and just had a tracheostomy and she is asking why did they move him out of ICU so fast.
My Dad is on a Ventilator & Recently had a Tracheostomy, But Why Did They Move Him Out of ICU so Fast?
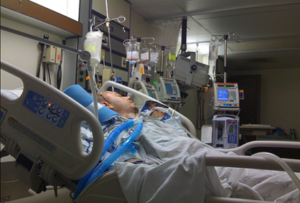
Joy: Hi Patrik! So nice to meet you.
Patrik: Nice to meet you.
Rey: Okay, good to meet you. Good to be talking to you.
Joy: Yeah.
Patrik: How can I help you?
Joy: Let’s see. Rey, do you want to go ahead and start?
Rey: Okay. Well, currently, they had my dad… He’s been moved out of ICU. He’s in the pulmonary ward because he’s on a ventilator, lung issues and things. Well, he’s able to spend 18 hours off of the ventilator and then sleeping with the ventilator on. However, Joy told me that she told you a little bit about what’s been going on. They put the trach in him and with the ventilator, he’s not able to eat. Our goal originally was for him to be weaned off of the ventilator. That was our goal.
Patrik: Should always be the goal, always.
RECOMMENDED:
Rey: Yes, yes. However, moving him out of ICU, they’re saying that they don’t try to wean him off from ventilator in the pulmonary ward. They only do that in the ICU. So, the pulmonary only maintains what the ICU set up, which means 18 hours off and then the remaining on, six hours on the ventilator. Is it a full 18 hours off, Joy, or is it 16 hours off?
Joy: Oh, I just know they told me they had gotten him up to 12 hours of being off of the ventilator, I didn’t realize they had gone all the way up to 16, successfully, where he was able to sustain breathing, healthy breathing.
Rey: I don’t know if they had gotten all the way up to that. I know that he sleeps with the ventilator on, so it might not be 16 or 18, it might be less. My concern about that is that he has only had full nutrition through the feeding tube, if you can call that full nutrition, for a little over a week. Hasn’t it been a little over a week, Joy?
Joy: Yeah.
Rey: There was an interruption in the beginning where there was some bleeding around the tube. But as far as his having full health and then being able to heal from having full health, it’s only been two days since they’ve tried to wean him off of the ventilator. And we feel that they should be giving him more time. But we already feel that they’re trying to lean us toward getting into another facility, like a step-down facility where they can maintain the ventilator and the feeding tube.
Patrik: Right, I see. Joy, did you want me to admit you again with another device? Sorry. Okay, tell me a little bit more about the timelines. Joy, I do remember when we spoke this week, I think your dad had an early tracheostomy, from memory, is that correct?
Joy: Yeah.
Patrik: He had a tracheostomy after about two days in ICU. Is that correct, from memory?
Joy: Yeah. Because it’s only been about 10 days altogether, I believe. Right, Rey, since he’s gotten the surgeries for both the feeding tube and the tracheostomy?
Rey: Yes.
Joy: Yeah. And the tracheostomy, right. It’s been about two weeks since he’s been on the ventilator.
Patrik: Okay. Initially BiPAP (bilevel positive airway pressure) with a mask?
Joy: Yes.
Rey: And the BiPAP, yes.
Patrik: BiPAP with a mask. Then the tube. Well, cannula, BiPAP, tube in the mouth and after about two days of the tube in the mouth, tracheostomy.
Joy: Right. No, it was maybe about three or four days of the trach.
Patrik: Right.
Rey: Yeah. I think it was more than two.
Patrik: Right, okay. Still very early. Still very early.
Joy: Yeah. But you said it would only be seven days?
Patrik: 14, 10, days max. At the minimum. Sorry, at the minimum. Especially with COVID last year. Before COVID, you would’ve said day 10, day 14, if you can’t get someone off the ventilator. With COVID, that got longer and longer, for all sorts of reasons. And that’s why I was surprised to hear from you day two, even if it’s day four, it’s very early. But there may be legitimate reasons for it. I don’t know all the details, but generally speaking, nine times out of ten, you try to delay because if you can avoid the tracheostomy and get them off the breathing tube in the first place, that should be the goal.
Rey: Yes.
Suggested Links:
Patrik: That’s why I was a bit surprised to hear. And remind me, Joy, your dad had COVID as well?
Joy: He did.
Patrik: Yeah. Yeah.
Joy: He had COVID and he’s also having multiple myeloma and it seems to have progressed. However, the cancer team does not want to do anything in terms of the chemo. They don’t think he could withstand it.
Patrik: Okay. When was the last chemo he had?
Rey: It was February. I think it was the second week in February. And actually, I think that’s what weakened him enough to where he became susceptible to COVID.
Patrik: He would’ve been proned, with being immunocompromised.
Rey: Yeah. And right after that last treatment, he had a cough that he couldn’t get rid of, and he wound up going to the emergency room for that cough. And then they put him in a COVID ward, and then he was in quarantine. We couldn’t see him. You probably are familiar with the protocols there, they don’t really help you. And he just declined with their protocols. I’ve been doing some research and I know that there are things that can definitely be used to prevent… I mean, he should have been walking out the front door in a couple days, but here we are now, so anyway.
Patrik: Okay. Okay. So, the first COVID diagnosis was early this year?
Joy: Yeah.
Rey: Yes.
Patrik: Right. So how come then, three months later, when he ended up on BiPAP. What happened? Is it the COVID that got his lungs to deteriorate this time?
Rey: Yeah. Yes. He had pneumonia. He had developed a pneumonia. He had COVID. However, we pushed to get him on nebulized budesonide, to include that in his treatment. And he became better. He went from an oxygen dependency of 35 all the way down to-
Joy: Four.
Rey: Yeah. It was down to one but at this point, down to one. But he had developed some lung damage and there may have even been a little bit of inflammation there too, that one of the doctors where he’s at now told us. However, when we first went there, they said, no, he doesn’t have any inflammation. The budesonide, it won’t do any good because there’s no inflammation there and everything. And then weeks later we find out that maybe it could have done some good because he may have had some information. I’m sorry, I’m rambling on.
Patrik: No, no, no. This is all important. But basically, where he’s at now is he’s in the pulmonary ward. He’s not making progress because they are saying, “That’s not what we do.”
Rey: Yes. Right.
Patrik: That’s unbelievable.
Joy: And they just moved him out of ICU, I think really within the last 30 minutes.
Patrik: Right, okay. I see. I see. Okay, right. Let me ask you this. In ICU, was he getting mobilized?
Rey: Mobilized?
Patrik: Was he getting out of bed?
Rey: No.
Joy: No.
Patrik: Okay. Do you think that he could get out of bed with help?
Rey: I think he’s getting stronger now, but he would need more help. He hasn’t moved out of bed in weeks now.
Patrik: In weeks now. Yeah, that’s okay. Look, patients in ICU, even with a trach and a ventilator, can get mobilized. Don’t get me wrong, there are some contraindications, but the contraindications are mainly around fractures, surgery, that sort of thing. I’m old school, I did my training over 20 years ago, but there’s a different generation now of doctors and nurses. We were mobilizing patients everywhere. And if you want to get someone off the ventilator, you need to mobilize them. Simple as that.
Joy: Okay.
Patrik: Right? How do you run a marathon? You run a marathon by training.
Joy: Right.
Rey: Right.
Patrik: Right? And it’s the same, it’s like an exercise, almost like an exercise regime to get someone off the ventilator. Again, there are situations where you can’t get someone off the ventilator, maybe a spinal injury, but for any pulmonary issue, like COVID and pneumonia, those people should get off the ventilator. And that can happen quickly. It can take time. But it, generally speaking, only happens by exercising, by mobilizing them. Common sense.
Rey: Okay.
Patrik: Common sense.
Recommended:
Rey: Our dad, he hadn’t had any handicaps or impairments or anything.
Joy: Patrik, they told us that they are doing some arm exercises, leg raises, in the bed, but I mean, I know he does want to get up. He actually, about two weeks ago, got off the bed and tried to move and he fell because he hadn’t lost-
Rey: He slid out of the bed.
Joy: He slid out of the bed, but he was okay. They got him back in the bed after they found him on the floor. But actually, he’s been there, what, three or four weeks now. He had been released from his first hospital stay, I think I had told you, he went into the skilled nursing rehab and was doing some rehab. And he was sitting up and he was trying to take some steps. So, he feels and wants to get stronger. So, is that something we can ask for?
Patrik: Absolutely. There are so many people that I’m talking to, they can’t fathom that you can actually mobilize someone on a ventilator. And what I mean by mobilizing is you slide them over into a recliner chair and then you sit them up. If you type into Google “mobilizing patients in ICU,” you will see images of people being mobilized, irrespective of what they’re telling you. You will find images online of people in ICU being mobilized on ventilators, trachs, all possible.
So, if he was unstable, which I believe he’s not, because they’re moving him out of ICU, you know that could be another contraindication. If someone is hemodynamically unstable, they have a low blood pressure, they are on medications, so they’re supporting that blood pressure, all of that, that’s another contraindication. But if they’re moving him out of ICU, he’s got none of that.
Rey: Right, right.
Joy: Oh my God. Okay.
Patrik: Right?
Rey: Now also, in that meeting, one of the main things in the meeting that we had met with the doctors yesterday is that they probably give him weeks or months to live because of the cancer. I don’t necessarily take their word at that because they’re, of course, coming from their perspective, and their perspective is that chemotherapy is the only thing that could help him, or maybe radiation, and of course that’s going to damage him more.
So, this morning I had them include more supplements and some flax seed oil in his diet and hopefully some things that seemed to have a beneficial effect before three months ago, before all of this, when he was living at home and things. But that might be one of the parameters or one of the considerations that they’re making these decisions off of, also.
Patrik: Okay. Who is saying that? Is it the ICU or is it the oncologist?
Rey: Not the oncologist. They didn’t give us a date. It was the head doctor over the team.
Patrik: ICU?
Rey: He seemed to be over that. It was the other doctor Joy. He seemed to be over ICU doctors over the whole… He presides over all of the doctors involved in my dad’s case.
Patrik: Interesting.
RECOMMENDED:
Rey: He asked permission if we wanted to know what his thinking was for a time factor that my dad had with the emergence of this. They tell us it’s a-
Patrik: A tumor.
Rey: Cancerous tumor on his forehead, a growth.
Patrik: Like a skin cancer?
Joy: A multiple myeloma.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!