Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode was
You can check out last weeks question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to continue answering the next questions regarding James’ and Christine’s Dad in ICU who’s had a haemorrhagic stroke.
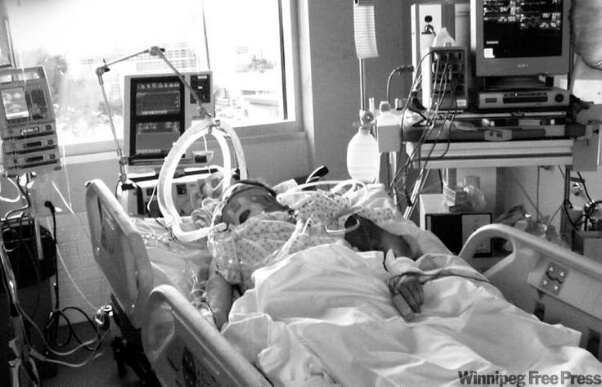
James’ and Christine’s Dad had a brain decompression where they evacuated a large bleed from his brain after the haemorrhagic stroke. And their Dad also underwent a craniectomy (partial removal of skull) to decrease the brain pressures after the bleed.
James’ and his sister Christine were getting their Dad in one of the best hospitals in the USA, the Cleveland clinic in Ohio.
In the meantime, their Dad was getting a tracheostomy because he couldn’t be weaned off the ventilator and the breathing tube. He also had a PEG tube for feeding inserted.
He also had ongoing seizures due to the stroke and his anti-seizure medications needed to be optimized so he could “wake up” and progress to Neurology Rehabilitation.
In today’s 1:1 consulting and advocacy sessions with James and his sister Christine, we look at some setbacks their Dad is going through.
He had to be put back on the ventilator due to a Pneumonia and he also ended up with a central line (CVC) and arterial line again.
In the meantime he has come off the ventilator but still has the tracheostomy after over 5 weeks in ICU.
This series of 1:1 consulting and advocacy is a real testimony for getting advice, run with it and get results.
If you want to avoid LTAC and a nursing home for your loved one, you need to read all of the consulting and advocacy sessions with James and Christine!
So in today’s episode of “YOUR QUESTIONS ANSWERED”, I answer a series of questions from James and his sister Christine again that are excerpts from various 1:1 phone/email consulting and advocacy session with me and the topic this week as part of this series of 1:1 consulting and advocacy session with me and the topic this week is
My Dad is having a DVT and he’s now on a Heparin infusion! Will he need an IVC filter?
You can also read or watch previous episodes of 1:1 consulting and advocacy with James and his sister Christine here
Hi Patrik,
Quick question the doctor keeps using the risk of infection of staying in the hospital as the main reason to move him to LTAC.
What is your response to this?
Also, in the meantime the Doctors found a blood clot in my fathers right calf, which is his paralyzed leg.
The Doctors have ordered a CT scan this evening of his chest to check for clots in lungs.
If there are any clots in lungs they may put a filter in his stomach to make sure clots do not reach lung in preparation for his surgery next Friday.
My father is currently on a Heparin infusion.
The infectious disease Doctor came in today and said my father does not have a UTI and there is nothing wrong with him now! They have not done any more labs and have taken him off his antibiotics. His vitals are good nevertheless.
Coincidentally, my father is an attorney and has a few law suits where he has sued Doctors because of clots in legs so he has been verbal about his concerns. He is now back in step down.
Please advise of your thoughts on all of the above. Please let us know what if anything can be done about clot in calf before or after surgery.
Thank you
James & Christine
Hi James & Christine,
Thank you James for the update and thank you for renewing the consultation, I appreciate you as a client.
Hm, with the clot in the leg and the shortness of breath on Tuesday night your time, I am wondering if he had a mild PE (Pulmonary embolus)? I’m glad they are following up with a CT scan
How did they found out about the clot in his leg and when did they start the Heparin?
Also, the clot in his leg could be a result from
- Not enough mobility and lack of movement
- Has he had any ted stockings/compression stockings on his legs?
- Or has he got calf compressors on his legs to keep the blood flowing and circulating?
It’s good to hear he has no infection and they have ruled it out.
Inserting what’s called an IVC (inferior vena cava filter) filter to stop the clot from moving upwards makes sense and seems common practice.
Blood clots are usually managed conservatively (I.e. no surgery), therefore CT scan and potentially the IVC filter make sense.
The Heparin is a bit of a risk for the upcoming surgery and they need to stop the Heparin before surgery to minimize the risk of bleeding.
With the Heparin, do you know how much he’s on and do you know if he requires oxygen via the trachea?
Often during a PE (Pulmonary Embolus), shortness of breath and oxygen levels dropping are symptoms that need to be managed.
If your Dad isn’t short of breath and his oxygen levels are holding, hopefully he doesn’t have a PE (Pulmonary embolus)
IVC filter https://en.wikipedia.org/wiki/Inferior_vena_cava_filter
Also, as far as the transfer to LTAC is concerned due to the higher infection risk in a hospital, once again I question the approach.
Yes, I tend to agree that the infection risk in a hospital is higher compared to other facilities. Nonetheless there is still an infection risk in an LTAC as well.
This is about continuity of care and it’s about managing complications if they do come up. If this complication had come up with the DVT and the thrombus in LTAC there is a high chance that he would have had to go back to ICU or step down/HDU anyway.
LTAC is not equipped dealing with emergencies. On top of that they are not incentivised to transfer Patients back to ICU when emergencies/ complications do occur because they miss out on revenue.
Your Dad is not out of the woods yet as you can see and once again, a transfer would only add on to already high stress levels!
Kind Regards
Patrik
Hi Patrik,
IVC filter going in tonight. Cranioplasty is tomorrow.
My father is getting so much better with his cognition. I need this go to right and we need to be sure.
It’s 9:38 pm and My father is scheduled to have IVC filter sometime this evening.
Do you have any thoughts on the above before his surgery?
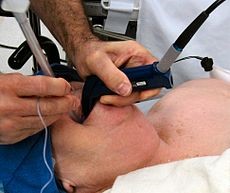
Also. My father will be on ventilator through tracheostomy for his surgery. Please let me know your thoughts on this!
Also. Would you happen to know the difference between a temporary IVC filter and a permanent IVC filter? Or have any opinion as to which one would be better?
James
Recommended:
Schedule your free appointment here
Hi James,
because they have to stop Heparin for the surgery they have to put in the IVC filter to prevent any clots from migrating.
Most Patients in ICU get a temporary IVC filter in with a removal down the line, in your Dad’s situation he may get a permanent one due to the current immobility.
I’m pretty sure I mentioned last week that your Dad will need the tracheostomy for surgery because of ventilation.
Hopefully after surgery they can start working on removing the tracheostomy.
Kind Regards
Patrik
Thank you Patrik,
What are your thoughts on getting him off the ventilator after surgery ?
Do you think he will have to be weaned again ?
Any thoughts?
James
Hi James,
unless there are any unexpected complications it should be smooth sailing.
Ventilation is required due to anaesthesia during surgery.
He should be able to come off the ventilator after surgery.
Kind Regards
Patrik
Hi Patrik,
They could not get the IVC filter in tonight because my father was squirmish on the table and they could not sedate him because they did not stop his feeds early enough so now we are rescheduled for 730 in the morning.
So he will be having IVC filter at 7:30 AM and cranioplasty surgery at 1:30 PM.
They’re stopping to feed tonight.
Please let me know your thoughts on the above.
I’m hoping all of the test being done today and his surgery is tomorrow are not too stressful for him or on his body!
Many thanks
James
Recommended:
Hi James,
not stopping the feeds early enough is amateurish, sorry I hate to say it but that’s the reality.
I think in a sense it’s good that he has it all in one day, so he can go from one procedure to the next.
I don’t think too much is going to change if he has it all in one day, let’s wait and see that’s all you can do for now.
Kind Regards
Patrik
Hi Patrik,
Agreed. So whose fault was that. The nurse ?
They decided to put a filter in around 4:00 pm
So they probably should’ve stop the feeds around 4-5:00 pm in preparation for the filter at 11:00pm.
Who is in charge of something like this? This is a major screwup in my eyes.
James
Hi James,
Definitely a major screw up, the nurses should be in charge of that.
I also don’t advocate for a procedure in the middle of the night if it can be avoided.
The risk for complications after hours is just bigger.
I hope that all went well.
Kind Regards
Patrik
Recommended:
Hi Patrik,
This is the link to the rehab in Chicago. Number one in USA.
Let me know your thoughts.
I think he may be ready for his in two weeks or so after he builds more stamina.
Will be in touch. I always appreciate your feedback and guidance.
You have been a tremendous help !!!
James
Hi James and Christine,
I’ve had a closer look at this section here, where they talk about Stroke recovery specifically.
https://www.sralab.org/conditions/stroke-recovery
It certainly reads well and it talks about all the things we’ve discussed over the phone like speaking, walking, eating, toileting, showering etc…
I think it would be great if they could assess your Dad somehow to see if he’s suitable and what outcomes they think they could get for him and in what timeframe.
They certainly talk all the right language on their website. It might also be dependent on insurance as previously discussed.
At the same time, there must be some alternatives closer to home who offer a similar stroke recovery/rehabilitation service and I think it would be good to talk to them as well.
I do believe the closer you have him to home the better.
Also, it might also help if you could talk to a former Patient or a family who’s been in a similar situation and who went through rehab at any of those places.
Keep talking to your Neurologist and Neurosurgeon and see what they suggest as well.
Also, I do believe he’s in a much better position now than he was a few weeks back to be assessed properly and take the next steps. His recovery to this point should be looked at very favourably by facilities, doctors, insurance and other specialists he’s dealing with going forward.
As I mentioned before, I’m now leaving familiar territory as the rehabilitation side of things is not really my speciality but I know what needs to be done leading up to it.
I hope that helps, please let me know what else you need.
Kind Regards
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!