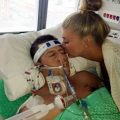
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
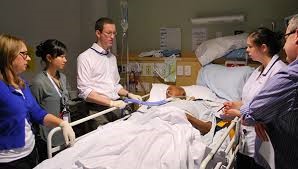
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Rosie, as part of my 1:1 consulting and advocacy service! Rosie’s dad is with a tracheostomy and is on a ventilator in the ICU. Rosie asks if her dad will still wake up if the ICU team is giving her dad too much sedatives.
My Dad Gets Too Much Sedatives In the ICU. Will He Still Wake Up from an Induced Coma?
Patrik: I’ve never seen that, never heard of it. Worked in ICU for 20 years I’ve never, yeah Nimbex sure, a common drug, last resort drug, temporary. Why is it-
Linda: That’s what they told us.
Rosie: He’s been on it for a whole month.
Patrik: Cool. What happens if-
Rosie: He kept on having this synchrony when they would get him off of it and they keep him back on it.
Patrik: Sure.
Rosie: That’s been the whole thing all the way through.
Patrik: Yeah.
June: So they attempted to take it off two weeks ago, two separate occasions. But at that time he was still intubated.
Patrik: What is he now? He’s not intubated?
June: He has a trach.
RECOMMENDED:
Linda: Tracheostomy.
June: Trach now.
Patrik: Okay. That’s good.
June: Yeah so when he was intubated I don’t think he could tolerate the breathing tube when they were taking off the Nimbex. So maybe that was also a factor at the time that he couldn’t be taken of the Nimbex because the discomfort from the throat, no?
Patrik: No, not really. Look with the ARDS has he been in prone position?
June: They’ve proned in the past I don’t think lately he has been proned no.
Patrik: When was the last time he has been proned?
June: Probably a couple of weeks.
Patrik: Okay.
Linda: They said they’re doing it very sparsely because I think one of the doctors we had brought it up a few times and he said with his because obviously at that time he was intubated still with the ventilator, they said it’s a whole orchestration-
June: Orchestration.
Linda: … and they definitely don’t have. He said there are some patients that would benefit more than the others from it so what they were saying is they do it a little bit sideways a few times they’ve done it but not consistently.
Patrik: Okay, what about ECMO? Have you heard of ECMO?
Linda: Yeah I remember ECMO.
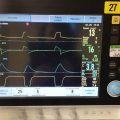
June: Yeah that’s … So his settings on the ventilator it’s 40%, okay the FiO2.
Patrik: Fi02 is 40% yeah.
June: His PEEP is five.
Patrik: Okay.
June: So you know I don’t know if he needs an ECMO, that’s basically a lung bypass right?
Patrik: Lung bypass absolutely yeah.
Linda: This hospital doesn’t have it. We asked about it they said that their hospital doesn’t have it.
Suggested links:
June: Yeah so he’s saturating in the high 90s at FiO2 of 40.
Patrik: Okay well just looking at the numbers a PEEP of five Fi02 of 40 doesn’t sound too bad. What happens if they took off the Nimbex though would those numbers change? I would argue they would.
June: Yes.
Rosie: Yes.
Patrik: Right. Do you know what they change to?
Linda: 80 at one time-
June: 70, 80s.
Linda: … they do give him 100%.
June: But you know he starts breathing faster.
Linda: Over the ventilator.
June: He starts coughing. Maybe he’s thinking he’s drowning because it’s probably a lot of fluids still because he has edema everywhere.
Patrik: Edema
Patrik: Is he on dialysis?
June: No. They’re giving him Lasix to drain him out currently. The problem is they haven’t been very consistent with the Lasix so at times he falls behind and then it starts building up again. So, right now again they’re using Lasix. He speed maybe almost three liters yesterday.
Patrik: Okay.
June: Today, day shift, his urine output was 750 mls so far.
Patrik: Yeah. Sure.
June: So he might even pee another three liters today, total in 24 hours.
Recommended:
Patrik: Okay, why do they think he’s fluid overload? And have they given you … Is his heart, does he have a heart condition?
June: No.
Rose: He has edema everywhere. He had pitting edema everywhere.
Linda: So yeah.
June: So you know the doctor said, his kidneys is probably 60 to 70% clear right?
Linda: 65 to 70% function kidney function.
June: So it could be that is the reason. Also he’s malnourished right now.
Patrik: Yes of course.
June: His gut has only been taken in so much maybe 20%, 30%. So, for the last months, he’s been malnourished. So now the new doctor wants to put him on what did they call it?
Patrik: TPN.
June: TPN.
Linda: TPN. Yeah and you know for the fluids we asked them this question today, is how much fluid intake is he having. Because now we know the output, so he said before, a few weeks ago they were giving him about 2.5 liters of IV and all of that stuff and then now he said that he’s down to about one liter a day. But then he cautioned us that with the TPN, his intake will go up again because it’s like a feeding tube like IV right?
Patrik: Correct. What’s your dad’s weight roughly?
June: 130 maybe 140.
Patrik: Okay.
Linda: 140, yeah.
June: He’s not obese. Yeah he’s not obese.
Patrik: Yeah no he’s not obese.
Linda: Yeah he’s shorter. He’s a 5’1
Patrik: Yeah sure. Okay, I’m not surprised he’s malnourished because on the Nimbex because it’s a paralyzed agent, the gut mortality slows down and he can’t absorb feeds because he’s basically not digesting because the gut’s paralyzed, everything’s paralyzed right? I am surprised the TPN should have come in-
June: Sooner.
Patrik: … a few days into the Nimbex.
June: Yeah.
Patrik: Right? So it’s not only that he’s malnourished it’s also he’s losing out on proteins, calories. To fight a critical illness, you can’t starve a patient to fight a critical illness right? What are their plans? What are they telling you?
Suggested links:
June: So this new doctor, he just got a new doctor this week. He is more experienced, the last ones are very young and they were just taking day by day firefighting each day. This new one has some sort of a plan and he’s more experienced. So, TPN right away.
Patrik: Yeah good.
June: Starting that.
Linda: Yeah get him stable on the ventilator without Nimbex and more intubation.
June: So he wants to get him off Nimbex and that’s to priority, okay?
Patrik: It needs to be top priority.
June: So he’s going to give him another sedative. At first, he’s mentioned Haldol
Patrik: Haldol okay.
June: Actually by the way he’s already on a very high dose of fentanyl, okay and a very high dose of versed.
Recommended:
Linda: Ativan.
June: So you said-
Patrik: Is it ativan or?
June: No not ativan.
Rosie: No, just versed.
June: Just versed.
Patrik: Can you-
June: So he’s going to add a third one to make sure he’s even more sedated. He mentioned haldol but then later called me with something called Salpril, I haven’t heard of that.
Patrik: I’ve not heard of it but it probably might be generic name, how do you spell that?
June: You know I wish I took the spelling I just went based off his pronunciation and wrote it down but I can’t find it on the internet.
Patrik: Salpril.
Linda: Salpril.
Suggested articles:
June: Salpril I heard Salpril something like that.
Patrik: Okay hang on, just give me one second. I just quickly need to google it myself. I have not heard of it. They didn’t mention-
June: He said it’s in the same class of drugs as haldol.
Patrik: Okay. Can I just say, haldol is not a sedative. Haldol is an antipsychotic medication. If you google haldol-
June: Yeah I saw that.
Patrik: … it will tell you, it’s an antipsychotic medication. It’s definitely not a sedative. I would assume your dad doesn’t have a mental health issue?
June: He suffers from depression.
Patrik: Right okay but Haloperidol it’s an antipsychotic drug. Did you say salpril?
June: Salpril. So he’s not going to use-
Linda: Haldol.
June: … haldol anymore he said salpril he changed his mind.
Patrik: Right, okay.
June: He said Haldol had some side effects like sometimes you would get a fever.
Patrik: Right, yeah, I don’t like haldol. How much-
June: But he would use it as a step to help him get off –
Linda: Nimbex.
June: Yeah, Nimbex.
Patrik: Of course. Do you know how much versed he’s on, do you know how much?
Linda: So I know it’s says four, it says fentanyl I wrote 400 dose of fentanyl.
June: Rosie is that right? Is that what you heard or is it 200?
Rosie: No it’s 200 fentanyl and it was 20 of versed.
Patrik: That’s a lot.
Rosie: Yeah.
Patrik: He would be having-
Linda: No it’s 400. Because today-
June: I heard 200.
Recommended:
Linda: No today even … No.
June: It’s 200. Rosie has a good memory.
Patrik: It’s still a lot. 200, even if it’s only 200 it’s still a lot.
June: Yeah.
Patrik: He’s been having that basically for weeks.
June: For a month.
Rosie: Yeah.
Patrik: Okay and he thinks that just by adding in the Salpril that would be enough to get the Nimbex off is that what he thinks?
Linda: He thinks-
June: That’s what he thinks. You know he’s-
Linda: To wean him off.
June: He said he’s had several patients like this in this situation.
Patrik: Okay good.
June: So he’s not his first rodeo from the way he made it sound.
Patrik: Okay, good.
June: So the other doctors to be honest, I think they’re just young and inexperienced. But this one at least has a vision to where to take him.
Patrik: Yeah.
June: Even though it’s maybe a little risky which we have to take risk right now.
Patrik: Of course well he needs to get off the Nimbex. How big is this ICU how many is this a big hospital? Is it a small hospital?
RECOMMENDED:
June: It’s a massive company with many hospitals.
Patrik: Right. How big is this ICU specifically? Is it five beds, is it 10 beds is it 30 beds?
Linda: So he’s in-
June: Overflow.
Linda: … overflow unit. Maybe I don’t know. Maybe Sarah knows, Sarah do you have an idea of how big the ICU’s are?
Sarah: I’m googling it right now.
Linda: Okay.
Patrik: The reason I’m asking how big the ICU is, because I’m well aware that all ICUs are having makeshift ICUs at the moment because of the demand. But let’s just say during normal times this is a five bed ICU which would be really small okay? I would argue any ICU less than 10 beds is a small ICU, okay. Small ICUs generally speaking deal with less critical patients, with fewer critical patients. They are still dealing with critical patients. But you know you look at a big metropolitan ICU 30, 40, 50 beds they have exposure to ARDS all year round, irrespective of COVID.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!