Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tony, as part of my 1:1 consulting and advocacy service! Tony’s dad is on a ventilator in the ICU after an open- heart surgery. Tony is asking if a tracheostomy is the right thing to do for his dad if his dad can’t come off the ventilator.
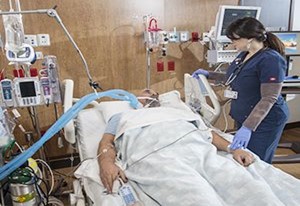
My Dad Can’t Come Off the Ventilator in ICU. Is Tracheostomy the Right Thing to Do For My Dad?
Patrik: Hello Tony. Can you hear me?
Tony: Hi Patrik. Yes I can hear you.
Patrik: All right. Hang on. Get this out. Okay, there you go. Do you have your brother coming in as well?
Tony: Yeah. Let me see if he’d get in.
Patrik: Okay.
Tony: I don’t see him in. Hold on one moment, please.
Patrik: Thank you.
Tony: Moe, get it from your phone for me, please. Ask him if he has a problem. Call him quickly. Ask him, can he join in?
Patrik: He has the link and the Zoom app. He just needs to click on the link. That’s all.
Tony: Yeah, he has the Zoom app. He does meetings from Zoom too.
Patrik: Right, right.
Tony: I’m not sure if he has any other problem.
Patrik: Right.
Tony: I don’t see him there.
Patrik: Hang on. Just give me one second. No, there’s no one waiting. Okay, hold on.
Tony: Moe, you called him? What did he say?
Patrik: I can’t see anyone trying to get into the meeting. I would get a notification.
Patrik: I still can’t see anyone trying to get in.
Tony: Yeah, he asked for the passcode.
Patrik: Mark?
Tony: Yes, that would be him.
RECOMMENDED:
Patrik: Okay. All right, I think now we’re all here.
Tony: Okay great.
Patrik: Okay. That’s wonderful. So we’ve got about 15 minutes of my free time. I do have other options available after the free 15 minutes that are paid options, but why don’t you start with what their challenges are. And then I can tell you how I can help you.
Tony: Okay. My dad had the drooping face one day. It was end of last year when this happened. So we took him to the emergency room. He did not take his blood pressure pill for a few days. And his blood pressure was 235. I forgot the bottom number. So they rushed him in, and they stabilized him and trying to find out every day, what would be wrong, different testing, CAT scan, and so forth.
Tony: They find a vegetable in the aorta. They said there was four aortae and one of them had that vegetable that could, I guess, just go off at any time and caused another stroke.
Patrik: Vegetation.
Tony: Vegetation, yeah. So in order for them to actually prevent a few more strokes from happening at any time, they would go in there, repair the valve, remove the vegetation, repair the valve or replace it. So once they did that, then that was an open-heart surgery.
Recommended:
Tony: We didn’t really see it as an open-heart surgery. But now we know that’s what that was because they didn’t really go into all the details like that, so we won’t be so scared again. So he was fine right before that. I even had a last video of him walking and telling me, “Look, see, I don’t even need a walker. I don’t know why they think whatever.”
Tony: So I have a last video of him fully alive and his face was drooping on one side, which was the left side. So then after the surgery, he did not wake up for at least 10 days. And after two days, they asked us for our final five wishes, his final five wishes and he may not make it. So we didn’t know wishes. We just prayed. And eventually, 10 days later he did wake up.
Tony: So they said he was in a vegetative state and coma. Then they said, “No, who said he was vegetated? And he’s not in a coma. That’s because he woke up.” But when they didn’t think he was going to wake up, they did tell us that he would need tracheostomy and PEG and be in a hospice where death can happen naturally within six months, or what are the wishes?
Suggested links:
Tony: They didn’t say, “Pull the plug,” but I guess that’s what they wanted to know. So now we actually have him okay after he woke up. We were able to even speak to him. They weaned him off the ventilator and he still had things to eat through a little tube, not the real PEG. So after they weaned him off, they tried to do the swallow test to take him to a rehab.
Tony: That’s when he aspirated, they say, and had hypoxia. And then they had to do CPR after a code blue. So now he’s in the ICU and ever since then up until now he’s been in the ICU after the CPR. So three days after the ICU, they asked us to do a PEG, but we were like, “Well, he’s been mutilated. Let’s wait a little bit, see if he gets better.”
Tony: And today they asked for a consent again. I said, “Let me just get some help regarding the PEG.” But they very shortly, talked about then if he’s not getting off the ventilator that he would then need a TRACH. So we’re trying to see, I guess-
Patrik: What are your options?
Tony: Patrik, what’s your opinion on that case? And since we’re already here now, what the options could be?
Patrik: Okay. Are you both the medical power of attorney for your dad?
Tony: I don’t have a written power of attorney. He just had me as the proxy at the hospital by putting my name there. We didn’t really fill out papers, but I’m the proxy and my brother is also added. But because he’s not in town, I’m more of the proxy and he’s the other proxy.
Patrik: Okay. And you are in town with your dad?
Tony: Yes. I’m in town. He’s about a minute from me.
Patrik: Right. And you so far, have been given consent to everything that was happening?
Tony: So far, yes.
Patrik: You are the one more or less giving consent, okay. All right. That’s good to know. And maybe I misunderstood you. I thought he had a tracheostomy already. No?
Tony: No. Only the heart surgery. They gave him CPR, now they need consent for PEG. Eventually, they’re going to start talking about the trach. They didn’t really go into details with that.
Patrik: Yep. And he was off the ventilator eventually?
Tony: He was.
Patrik: Yeah, and he was coherent?
Tony: Well, he just couldn’t swallow. Yes.
Patrik: He couldn’t swallow, but he could talk, he was coherent?
Tony: Yes. He could talk, not much. He would say, “Hi Mark,” which is my brother. Or, “Hi Tony.” He would know everybody. I put everybody on a call, WhatsApp, whatever, he knew everybody. But the voice was too small. All we can hear is, “How you’re doing?” So we didn’t force him to talk too much, but he was very alert and was able to talk if he could have said more.
Recommended:
Patrik: Yeah. How old is your dad?
Tony: 79.
Patrik: And any pre-medical history? Any significant pre-medical history?
Tony: He was diabetic and he needed blood pressure pill. He never had any surgery. They took out a tooth here and there, but he never had any surgery. Although, while talking about the teeth, they did say part of the problem was the fact that there was an unchecked gingivitis. And after this, he was going to get the teeth taken care of. They were going to pull all of them out and then he was going to be in rehab and antibiotics. But it didn’t go that way obviously.
Patrik: Okay. And how long was the CPR for? Do you know how many minutes? Have you got any idea?
Tony: No, but I can ask them how long was the CPR? I think I needed to know how long he was even off before he had it, but I keep forgetting to ask that.
Patrik: Yeah. That would be important information, I believe. Have you spoken to a neurologist?
Tony: Neurologist, no.
Patrik: Look, I know you were looking for an answer and I feel like I’m getting a very incomplete picture. So what I mean by that is, when someone is in a situation like your dad, there are dozens of things happening simultaneously starting from ventilator settings, starting from what medication is he on, does he have any seizures what does the CAT scan of the brain show, which comes back then to an opinion from a neurologist.
Patrik: There are so many things happening at the same time that unless I have more information, I feel like I can’t guide you. I also believe that the ICU is only telling you half of the story. So if you and I were to get on a call with the doctors, I would ask a long list of questions. And then I would feel equipped to say to you, “Yeah, this is probably the best course of action. If you take this course of action, this is what probably the outcomes are going to be.” So I feel like I have incomplete information to guide you.
Recommended:
Tony: Okay. So as far as the CAT scans they did, after he didn’t wake up, they found out he did have multiple strokes. He came for just the left side. After the surgery, the right side was not even responding. He couldn’t respond to any command, but when he finally did move anything, it was the left side, the side that actually had the primary stroke.
Tony: But after the surgery when he didn’t wake up, the right side did not move at all. But right now, they are moving. When he was talking, they were moving. But right now, though he’s down, he moves them because I went in the hospital with a camera and everything else, talking to him and the other people talking to him. But I don’t see any of my notes say the neurologist was the one that talked to me or anything.
Patrik: Whenever it comes to stroke or a brain injury, you need to talk to a neurologist because they are the specialists for the brain. ICU has an opinion. Of course, they have an opinion. But ICUs are there to save lives. And once the life has been saved, then let’s talk to the specialist of what got your dad into the ICU in the first place.
Suggested links:
Patrik: In this situation, the specialists are the cardiologists because it was a cardiac arrest. And the secondary specialist is the neurologist because it involves a brain injury. Am I making sense?
Tony: Yes. I have, yeah. Okay.
Patrik: Right. So again, the ICU is important. That’s where he is at the moment. But ICU wants him out. ICU wants to minimize length of stay, that’s why you’ve got to listen to what ICU has to say, but ICU won’t be dealing with your dad going forward. And that’s why you need to talk to the specialist. But also, again, is the trach the right thing to do or not? I don’t know at this stage. Your dad might need days away from coming off the ventilator and you wouldn’t know, unless you have someone externally assess the situation. If your dad was to come off the ventilator in a few days’ time-
Mark: That’s what I was telling you.
Patrik: He won’t need the trach.
Tony: Okay, we lost you just a little bit.
Mark: Your voice cut off.
Patrik: You’re giving me valuable information, but you’re giving me incomplete information.
Recommended:
Tony: Okay. If I asked them-
Mark: So how can we go from there? You’re asking him, you need to talk to a specialist. So is there a time? Tony, did you know the doctors are in at eight o’clock, aren’t they? Are you working tomorrow? Is there a way that we can schedule that so we can have them on the phone, because I agree that they are not telling us the whole picture? Like you say, they are trying to get him out and the sooner, they could do. It’s just another patient, which they do with patients every day. And for us, that’s our dad. That’s not a number.
Patrik: Absolutely.
Mark: Yeah, so definitely… What is your time like? Because I think the doctors are usually in. I think the time that the doctors are in, from what I remember Tony, was eight o’clock.
Tony: Eight to four or to three. Well, possibly nine.
Mark: No, I’m talking about the time that they’re actually with dad. They usually tell us, “Call at eight.” I don’t know exactly what time they’re in. I mean, if it’s eight to four, you know better than me.
Tony: I can ask them also.
RECOMMENDED:
Mark: But how can we schedule a time where you’re going to be there and then what’s your fees, and how do we go about stuff like that?
Patrik: Tony, how have you been getting updates so far? What does that look like?
Tony: Okay. For the most part, the nurse that’s in charge, will answer me most of the questions. But most of the times, if I just call the number, the extension for ICU, that person that’s there will transfer me to whoever’s my dad’s nurse. But when there is a case where they did do a CAT scan, the person that calls me is the one that can interpret the CAT scan.
Tony: I never did write what was that person’s position. From what I’m looking at here, I just write that, that’s this person that called me and their name and who they are from the hospital. The only person I know I spoke to that was a specialist was actually the cardiologist when he was down, and 10 days later, when he was awake.
Tony: He went and put the iPad video so we could see him. But in between, I called the extension they told me to call. I asked for vitals, I asked for different things and I have the doctor’s name I speak to, not what’s their position, who they are or anything like that. So I’m not sure if I spoke to a specialist.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!







