Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
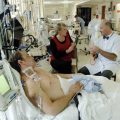
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Mikaela, as part of my 1:1 consulting and advocacy service! Mikaela’s sister is with a tracheostomy in the ICU and is now off the ventilator. Mikaela is asking how to stay positive whilst her sister has severe brain injury in the ICU.
How To Stay Positive Whilst My Sister Has Severe Brain Injury in the ICU?
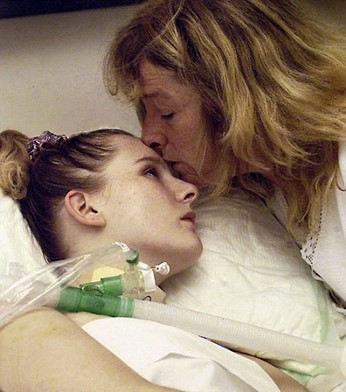
“You can also check out previous 1:1 consulting and advocacy sessions with me and Mikaela here.”
Dr. Rich: Hello Mikaela. I’m Dr. Rich.
Mikaela: Good morning!
Dr. Rich: Sorry, yes, I’m the physician for rehabilitation medicine, Dr. Marie is the Intensive Care consultant, and Rinzzie is the senior specialist occupational therapist. We have a long history of looking after people with disorders that comes in over the years.
Dr. Rich: So, as I started talking about… your sister has been in for 6 weeks now, she’s got a very profound brain injury as a result of blood supply not getting to her brain during the cardiac arrest. She’s obviously been quite unwell in the intensive care unit for a lot of that time, but we are at a stage now where she’s off all sort of life support things, she’s not requiring assistance to breathe. She is at a stage where she can’t manage her own airway, she’s got an artificial plastic tube in her neck and tracheostomy, and that’s because people who are drowsy as she is… If you’re asleep and you get into a position where you’ve locked your airway off, your wakefulness would increase a little bit, and you’d just move, and unblock your airway, and then carry on being asleep sort of thing. But when you’ve had an injury like this, you don’t have those same protective mechanisms. So potentially, if your sister got into a position where her airway was blocked, your sister wouldn’t be aware of it, and then potentially even go back into a respiratory arrest again.
RECOMMENDED:
Dr. Rich: And so, that’s the reason why that tracheostomy is inserted primarily, I think it’s that at the moment. There are also other things why she’s got a tracheostomy that are secondary to that, which is, she doesn’t have the normal ability to cough and clear all the normal secretions, partly because she’s very recumbent. She’s on her back, and again, the drowsiness means that she doesn’t cough and protect her own airway. We also have bits of things that go down your airway, and potentially that becomes a medium for bacteria to grow on as a source of infection. And so, the tracheostomy allows us to, in a sense, take over that function of coughing and clearing her airway out so that we can put catheters down to suction her airway to try and remove secretions. I wouldn’t say it’s not nearly as good as your own. But it protects her, to some degree, from further chest infections. Although I think, as we talked on the phone, nevertheless, even with that, it’s very likely that she will get chest infections in the long line just because of this reason, really. Because it can’t get right down into the base of her lungs and clear it out, it can only get so far down.
Dr. Rich: The suction can’t… And so, that’s the reason why I started tracheostomy in, and we’re now at a phase where, because she’s not needing breathing support and life support measures, we’re starting to try and make assessments of what the extent of her brain injury is. And on a Glasgow coma scale of consciousness, from somebody being completely comatose to somebody being, as we are now, walking, talking and fully conscious, we’re just relying on that scale. And this is the first part of the process of working out where she is from a brain function point of view, but also, over time, as you do those assessments, and you see how things are changing or not changing, it allows you to start predicting for the future where she might be. And so there are lots of discussions about what her future is going to look like, but it’s a way of making a more numerical quantitative assessment of where somebody is on that scale, and to allow you to prognosticate for the future.
Dr. Rich: So, I think that’s where you and I come in. I think, primarily, it’s just to talk… It’s that we wanted to talk to you a bit about how that process goes. It’s tied in with rehab more generally, which is about looking at physical function, and looking at… It’s basic functions like swallowing, and coughing, and all the normal human functions, and making some plans more generally around that, because they all tie into each other. It’s easier to assess somebody who’s more upright, for instance. So, if we could sort all on those things, it makes it a bit easier.
Dr. Rich: So, that’s where we are, and part of the conversation is about what we plan to do when the inevitable is to come, which there will be along the way. So, that’s an outline of what we wanted to cover today, and maybe some plans moving forward about what we might want to do about her airway management in the long term, proceeding in the long term, what we do about medical complications as and when they occur along the line, and really come to an understanding of where we are. So, does that sound a reasonable plan?
Mikaela: Yes, it’s fine.
Recommended:
Dr. Rich: Anything you want to ask here?
Mikaela: Are the cardiologists supposed to be a part of the meeting, as well?
Dr. Rich: I primarily wanted this meeting to talk a bit about neuro rehab. I can talk to you a bit about what the cardiology.
Mikaela: Oh no, it’s fine. It’s just, I’m under the assumption that maybe the cardiologist maybe might be a part of the meeting, as well.
Dr. Rich: So our priority now is the neuro rehab. I think, from their point of view, their feeling is that this was probably a primary arrhythmia, which is going to… She’s not really in a fit state to further investigate at the moment. She’s obviously been in hospital for 6 weeks, and we’ve not seen any more disturbance within that term.
Mikaela: How about on a few occasions, from probably what you are notified of.
Dr. Rich: Nothing very significant, we see some changes in a patient’s heart rhythm all the time, and that’s just part of being admitted in the hospital, and stuff like that.
Mikaela: Yes, that’s what the nurse said, as well.
Dr. Rich: But nothing that would require an electric shock to be delivered to get back into a normal heart rate. And I think… My understanding, from a cardiology point of view, is that, if she was well and had made a good neurological recovery, then it’s maybe something they investigate further, but there’s a right time to do that.
Mikaela: Yes. That’s what we discussed, yes.
Dr. Rich: Yes. So, we are in early days, and starting to get a feel of how… Essentially, it’s difficult because you can only measure what your sister does, and what we do to stimulate, and what reactions we get. And then, you’ve got to work out… And I think I talked to you a little bit on the phone about… There’s sort of a pathway of, from second to second, you take in information from the world around you. So, what you’re seeing, what you’re hearing, what you’re experiencing from your own nerves, and those things. And so, the first thing is sort of getting input in from the world. Then, you integrate that with what your brain already knows about the world. So, it’s got a lot of stored information about what you know what you know about the world, and you get information all the time coming in, and you put it all together, and you integrate what you’re seeing, what you’re hearing, what you’re feeling with what you already know to make sense of everything that’s coming in. And then, you decide to make actions in the world.
Dr. Rich: So, there’s information in, processing of information, actions out. From a very simple thing like, if I throw a ball towards you, you work out from your vision… You have, “This ball, it’s coming towards me,” and then you do an action to get out of the way, or catch it, or whatever. So, that’s… So, we in a sense, we don’t know what’s going on inside somebody’s brain, because there’s billions of brain cells, and trillions and trillions of connections, so you can’t measure on an individual cell level. But you can look at what somebody is doing and measure that, and we can try and structure the way that we give inputs so that we… We take away as much as possible, and we give something at a very simple level. That’s what we’re doing at the moment.
Recommended:
Dr. Rich: And so… And if you get a consistent response to something, then a lot of information seems to be processed to produce that response. The goal of all of this, and really, the purpose of an assessment of somebody with a prolonged disorder of consciousness, which is what she has, is to look at whether there is any consistent response, whether somebody might be able to make a differential response to something. Essentially, do this for one thing, and do that for another thing, so that they could choose something. And then, the idea is can we in any way establish any form of communication, or any form of… Is somebody able to ask for something, or indicate a need, or those kind of things? I must say, we’re very long steps towards that.
Dr. Rich: But I would say, if we’re thinking about disability or severe brain injury, usually people would say that quality of life in the future would come from independence, and being able to do things for yourself, and being autonomous, which is about being able to make choices about things. So, you can have somebody who’s paralyzed, but nevertheless, has a means of communication. So, they have a lot of control over their own life, even if they have a lot of care needs. So, it’s that two things. People can have a high quality of life with good autonomy even if they’re very dependent on other people, but if you have neither independence… So, everything is done for you, you can’t look after yourself, and no ability to make choices about the world, you’re, in a sense, very much at the mercy of everything else. And I don’t know in situations, might understand of the world around them, but if you can’t influence the world around you, and you can’t do anything for yourself, then your quality of life is obviously very poor, I would say.
Dr. Rich: So, we’re looking at windows into that, but it’s a stepped process. I don’t know if I’m explaining this very well, my partner Rinzzie’s probably the expert on… But that is, essentially, the purpose, and that is a process that takes time. And it’s a process that’s… It’s involved, and it’s difficult, and it will be particularly difficult in this circumstance, just from our experience of looking after over the years, and quite a number of people have come through who are… she’s very much in the older range of somebody who survives this kind of injury. So, the average age of people that we see either with traumatic brain injury or hypoxic brain injuries is usually quite a bit younger than this, because people of her age group and older usually don’t survive to this stage.
Dr. Rich: So… And what we find in the older age group is that their stamina and tolerance of some of the physical things like sitting, and the ability to maintain wakefulness to be assessed is a lot worse than if somebody is in their 20s, for instance. So, we’re anticipating this is going to be difficult process, but it’s… We’re just in very early phases, and we’re spending quite a bit of time over the last couple of weeks trying to just get some baseline assessments, as far as catching your sister when she’s at her most wakeful time as best we can in the hours.
Suggested links:
Mikaela: We’ve seen that as well, at the most wakeful… At the most… Times that she’s most awake. Say, if one of the nurse will call in with the nurse to say, “Look, if she’s got her eyes open, that’s good enough for us,” and then we can talk to her. Although, she might not be able to see, I don’t know. That’s just one of them.
Joseph: It’s very difficult, because we’re not there to touch her.
Dr. Rich: No, I know, yes.
Joseph: And have that stimulation.
Dr. Rich: Right.
Joseph: So, it’s really difficult to actually get that going, in that sense, too.
Mikaela: I think it goes back to what you say as well, because how… You say you don’t have that… You don’t know what’s going on in someone else’s brain. It’s… I don’t know, she might respond to that in her way, but the feeling that we give, the touch that we give, it may trigger something in the back of her head somewhere.
Dr. Rich: There’s much more personal to that. There are structured and objective assessments which we use for every patient, and we very much do try and incorporate things that are very… So, we deliberately do things that are not specific to that person, and deliberately do things that are very specific, even if it’s family photos, or voices from your family, even if they’re through phone, or recordings, or whatever. So, there are ways that we can do
Rinzzie: No, it’s fine. No, you’re doing a great job, yes.
Dr. Rich: There’s an absolute… I don’t know. A bit of expertise.
Rinzzie: If I just… Yes, if I explain what we’ve been doing. So, going back to what Dr. Rich was saying, so we’ve got this scale of somebody who is in a coma state.
Recommended:
Mikaela: Okay.
Rinzzie: Yes, or they’re just not responding, not… And you’ve got someone like us, who can make choices on what to do. And then you’ve got… Whereas, we’re looking to see, where is your sister on that scale? So, we know very clearly where she’s not at the moment. So, we know she’s down the end of the scale, the coma side of the scale. And I guess, with a disorder of consciousness, it basically means that, does someone have awareness of themselves in their environments, or does someone know that you’re there? Does someone know that you’re talking to them? Does someone know where they are? Very, very basic level care. And what we do is, we try and assess to see whether someone has that awareness of themselves or the environment. We do it in lots of different ways.
Rinzzie: So, we look at how they’re processing visual information, auditory and sounds, tactile and touch. We have other measures we use, as well. We look at different parts of the day, so if they are awake at certain times of the day. And what do they do? How do they respond to that stimulus? And we have five different levels of responses that we’re looking at. So, we firstly have no response. So, we’d stimulate your sister in a particular way, and maybe there’s no response to that stimulus. It might be we get something called a reflexive stimulus, which basically is a very primitive response that requires no awareness. So, for example, it might be a pattern of movement, so you may have seen… What your sister commonly does, is sometimes, when you stimulate her, or if there’s a sound, she has this movement where she brings her shoulders in, she moves her arms down, and she starts to chew a lot. So, that’s… We would call that a reflexive response. So, it’s a pattern of movement in response to a stimulus.
Recommended:
Rinzzie: We then have something called withdrawal, which is where you would move away from a stimulus. So, for example, if I try to tickle her nose, I try to move her arm, would she move away from that stimulus? So, those three stimuluses and those three responses correlate to something called a vegetative state. I don’t know if you’ve heard that term before, I hate the name but that’s what it’s called. And what that means is that somebody isn’t aware of themselves or their environment, and their response is very automatic, and there’s not a choice being made, there’s not a processing element to that response.
Rinzzie: The next response is where someone might start to be able to have some level of awareness. So, we’re still talking really low-level here. We’re not talking about being able to make a big choice or anything, we’re talking about someone’s processing something. So, base level is the level of processing. So, what we’re looking at there is if she localizes to something. But that might be they can look and scan something, they can give eye contact, they can… Something else you might see, they may move towards a stimulus. I might tickle that person again, and they might look towards where that stimulus is coming from. And then, you’ve got what we call differentiating, which Dr. Rich touched on. It’s where they can choose between two objects. So, for example, they might be able to look between two objects, or discriminate between one or two different things. And we call that minimally conscious. It’s still at a very low level, but it tells us that somebody is making some level of processing, and is able to sort of demonstrate that in a very basic way.
RECOMMENDED:
Rinzzie: So, I guess… So, what we’ve been doing, we’ve been using non-meaningful stimulus. These could be objects, mirrors, balls, touch, voice, those kinds of things, and we do it in a very standardized and structured way, because that allows us to repeat it and see if we can see any consistency, and we use different tools to do that. And that helps us produce a score, and also just compare where your sister is at. And then, what we also introduce is what we call experience of meaningful stimulus, absolutely… The recordings that you’ve left, music that your sister likes, things that are important to her, names, places, those kind of things. And then other things we’ll probably use are things like pictures, the things that she is interested in, sports. Whatever it might be that makes her who she is, we would also incorporate those things, as well, to see whether those stimuluses, do they make a difference in the case of someone’s level of processing?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!