Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
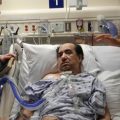
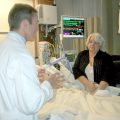
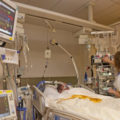
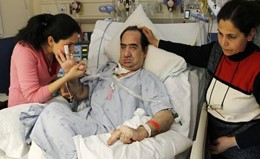
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Mikaela, as part of my 1:1 consulting and advocacy service! Mikaela’s sister is with a tracheostomy in the ICU. She’s now off the ventilator and Mikaela is asking if she should trust that her sister will receive the right nursing care she needs when transferred out of the ward.
Should I Trust that My Sister with a Tracheostomy Will Receive the Right Nursing Care She Needs If She’s Out to the Ward from the ICU?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Mikaela here.”
Mikaela: Hi Doctor. It’s me, Mikaela. Yes what is it that you want to discuss with the family.
Dr. Mark: Hello. Yup, I was to inform you about a request for we got a tracheostomy bed on one of the medical wards where they’re trained with tracheostomy care.
Mikaela: Yeah.
Dr. Mark: So I don’t know whether that’ll happen today or tomorrow.
Mikaela: Yeah, it’s just the only thing was there, Dr. Mark, I mean, no one actually consulted with us, in terms of consultants, that this was going to, I know that was a plan for a few weeks, but not at the time in which we thought it would be in, today or whatever.
Dr. Mark: Well that’s why I’m making this call, is to warn you that that is planned. I don’t know when it’s going to happen.
Mikaela: Yeah.
Dr. Mark: But once patients no longer need critical care support, the normal practice is to transfer them to ward based care.
Mikaela: Is it going to be a tracheostomy ward, did you say then?
Dr. Mark: There isn’t a tracheostomy ward per se. There are wards in the infirmary where the nursing staff are used to looking after tracheostomized patients and neurology patients, head injured patients, all those.
Mikaela: Okay.
RECOMMENDED:
Dr. Mark: And I don’t know which ward it will be. And I don’t know when it’s happening. All the point… This phone call is a courtesy call to let you and the rest of the family know, that that’s the plan for the days ahead.
Mikaela: Okay. Do you know, in terms of her medication that she was on for her arrhythmia, is that going to be continuing as well?
Dr. Mark: Well, she’s had… That’s for cardiologist and other people to say, I mean, just because she had one arrhythmia, doesn’t necessarily mean she needs to be on these things lifelong. They need to have that discussion. I mean, all these drugs have their risks and benefits and the cardiologists need to make a planned decision about whether it’s warranted to leave her on long term anti-arrhythmic drugs. None of the drugs that you would give long term are risk free. So it’s all about a balance of risks and benefits.
Mikaela: Yeah. Okay.
Dr. Mark: Is there anything else that you’re worried about at this stage?
Recommended:
Mikaela: Maybe just the… In the event, should she deteriorate, is there… Because there was a miscommunication about the return to ICU, should she develop any sort of complications?
Dr. Mark: Well, our view has been debated before with you, is that our view is at this stage with her neurological status, as it is, we would be reluctant to resuscitate her further or readmitted her to ICU, but I accept that the family had never accepted that.
Mikaela: Yeah. And we still don’t.
Dr. Mark: We would invite you to reconsider that in the length of time that all this is going on, because I think, in all honesty, the likelihood, even if we try and keep her alive in the longer term, I think it’s very likely that she’s going to get chest infections or other complications along the way. And we’re not saying we won’t admit her to ICU, but we would honestly believe it’s probably not in her best interest to do so if she deteriorates further in the future.
Mikaela: Yeah. I think to be honest, should it come to that, and I’d like to be made aware of that.
Dr. Mark: We will do.
Mikaela: Yeah.
Dr. Mark: But events may over take them another night, but I think what I’d encourage you as a family, once again, is to say, here we are many days down the line, her neurological state isn’t improving. Yes, we can get her to ward. Yes, we can keep her alive probably in the short term, but ultimately, where is this taking her in the longer term and realistically, is she ever going to improve? And I think at this stage, the answer is no. And how much further unpleasant interventions and things do you want us to do just to keep her alive for a few more weeks or possibly a few more months without any useful recovery.
Mikaela: Yeah.
Suggested links:
Dr. Mark: And I mean, there is no right and wrong answer to all of that, but for her sake and indeed the wider family state, I would encourage you to rethink this. And my suggestion is that we get her out of ICU in days ahead, we get her to the ward and ideally we’d have an agreement that she continues to get ward based care, tracheostomy care on the ward. But in the event of her deteriorating significantly, we don’t resuscitate her further, we don’t readmit her to ICU. Personally, I wouldn’t suggest that we should restart antibiotic if there’s a chest infection, but all of these things need to be, ideally we’d have an agreement with the family. So the nursing staff and medical staff on the ward have a clear understanding about what is or isn’t done.
Mikaela: Yeah, but in terms of antibiotics and such, if she had a chest infection, surely, I could be the next person to get a chest infection. I mean..
Dr. Mark: Yeah, but it’s a very different situation that you are up and about in the community, with every chance a recovery if you get a chest infection, then nobody would suggest we shouldn’t give antibiotics to you.
Mikaela: Yeah.
Dr. Mark: But your sister’s in a very different situation here.
Mikaela: Yeah, but if I’m speaking on her advocacy, if I’m speaking on her behalf, then I would say that she’s just as rightful as every other person that’s out there, who should be able to have antibiotics.
Dr. Mark: That’s fine. And I’m not disputing that.
Mikaela: Yeah.
Dr. Mark: But ideally we’d have an agreement about resuscitation, return to ICU.
Mikaela: We’ve already had a discussion about that and the DNRs not..
Dr.Mark: I know you haven’t agreed with that, but if she deteriorates further, do you want us to go through the whole ICU cycle again?
Mikaela: I would hope so, yes. I mean, I don’t even know why we’re having this discussion to be honest.
Dr. Mark: Well, because we need clarity about it, if she deteriorates again.
Mikaela: Oh, I know, then absolutely..
Dr. Mark: And I know you’ve made your opinions clear.
Mikaela: Yeah.
Dr. Mark: All I need to do is give guidance.
Mikaela: Look, at the end of the day, I understand that you guys work with your numbers and such, and how it looks and the figures and turnaround and whatever, on a patient basis, but end of the day, that’s my sister. So if..
Dr. Mark: I know, I appreciate all of that, but we also have to do what’s right.
Mikaela: And this is what she’d want, yeah. I’m sorry, but this is what she’d want.
Dr. Mark: That’s fine. And anyway.
Mikaela: Yeah, sorry.
Recommended:
Dr. Mark: To get back to the original conversation, the purpose of this call is just to warn you that we are planning to discharge her to the ward.
Mikaela: Yes.
Dr. Mark: And I think in the short term, you should see that as a positive, rather than a negative move, because it’s a better environment, the long term care without… With lesser risk for cross infection, patients dying in the next door bed, and all the other stuff that’s going on in ICU.
Mikaela: Yeah. I mean, I’m just more concerned about the level of care that she’ll be getting on the ward, that’s the only thing.
Dr. Mark: I accept that, but ultimately that’s where patients in the physical state that your sister is in end up, because we can’t keep them in ICU in the longer term.
Mikaela: How often would you need suctioning via the tracheostomy?
Dr. Mark: Well, it just depends on the secretion load and the nurses and physicians would be monitoring that on an hour by hour basis.
Recommended:
Mikaela: Yeah. Do you know what size she has of the tracheostomy, and if it has a cannula or anything like that?
Dr. Mark: I’m sorry. Ask the question again.
Mikaela: Do you know if she has… What the size would be of the tracheostomy that she’s got at the moment, and the cannula and stuff?
Dr. Mark: Well, it’s just a standard adult size tracheostomy.
Mikaela: Okay, all right. Yeah. That’s fine.
Dr. Mark: Is there anything else I can answer?
Mikaela: Yeah, sorry, I know you’re in a bit of a rush, but do you know, sort of expectation wise, when that would be, when they would be moving her across?
Dr. Mark: I’ve already said, I don’t. We’ve put out a request to a ward, but I suspect it won’t be to last the weekend, but I don’t know. It all depends with patient flows on the ward.
Mikaela:Yeah.
Dr. Mark: Staffing levels on the ward, which wards will take the tracheostomy patients. All I’m saying is it’s been put out as a request. I don’t know when it will happen.
Mikaela: What was the overall time that she was off with the ventilator?
Recommended:
Dr. Mark: She hasn’t had any, I mean, she’s been connected to the ventilator just for some positive pressure up until 48 hours ago, and before that there was four days with no actual sort of pumping of a ventilator. She was just connected to the humidified circuit. So in essence, all her breathing has been on her own for 7 days.
Mikaela:Okay.
Dr. Mark: So it’s not like we’ve taken her off the ventilator this morning.
Mikaela: Yeah, no. So, you’ve given around, at least a minimum of, well, let’s say 48 hours, right?
Dr. Mark: Yeah, so she has been completely independent for 48 hours and she’s comfortable with a good respiratory pattern and so on. So-
Mikaela: I mean, that would just show that it’s a good indicator.
Dr. Mark: So, I can’t say that she won’t deteriorate in days, weeks ahead. We’ll just have to meet that if or when that happens, but at the moment she’s steady and we believe she’s safe to send to the ward.
Mikaela: Okay. Yeah, that’s fine. Thanks for that.
Dr. Mark: We’ll keep you updated when we know more.
Mikaela: Brilliant. Cheers, thank you very much.
Dr. Mark: Bye.
Mikaela: Thanks for the call, bye. All right, she was sounding well pissed.
RECOMMENDED:
Hey Mikaela,
It’s Patrik here. Thank you for sending this recording through, so I’ve just had a good listen there.
So it sounds to me like your sister has been off the ventilator for at least a few days. I think, the 48-hour mark or the 48-hour box has been ticked. And it looks like if she’s going to the ward after the weekend, then she should meet those timeframes that I was suggesting in terms of a minimum of 48 hours off the ventilator. It’s good that you’ve brought up the NFR (Not for Resuscitation) again and the return to ICU, if needed. Whilst he’s saying all the right things, you obviously have to monitor that they are doing all the right things because, what they say and what they do don’t always match, necessarily.
The other thing is, I would want to know what size tracheostomy she has and Dr. Mark might not even know, that’s why he couldn’t give you an answer. He says a standard tracheostomy of an adult, they still have different sizes. It’s sort of a standard tracheostomy size for an adult is anywhere between 7 and 9 and that could be 7, could be 7.5, could be 8, could be 8.5, could be 9, 9.5 and 10 is rare, but is out there too.
The reason I am wanting to know if she has an inner cannula or not is that, if she has an inner cannula that needs to be changed multiple times a day. And that’s when it really comes down to whether the nurses on the ward are tracheostomy competent or not. If she has an inner cannula, somebody needs to monitor that. Inner cannulas are great, I like them, as long as you know what you’re doing, if you don’t know what you’re doing, they are a risk because if you’re not changing them, they could block off. Dr. Mark probably doesn’t think that way, once people leave ICU out of sight, out of mind. I’m just telling you it’s quite important.
The level of nursing care she will be getting on the ward will not be as much quality as in ICU. She will need to be prepared for that. And I know you probably can’t see her but it’s the more you can watch what’s going on in the ward, the better it is, because the level of care will go down. And I don’t trust that a ward can really look after someone with a tracheostomy. Don’t wanting to be negative, just talking from experience here. Let me know if you have any questions with those comments or if you want to get on the call. Thank you.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!