Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Why is my Mom Better in Intensive Care at Home than in a Nursing Home?
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Bob as part of my 1:1 consulting and advocacy service! Bob’s dad is in ICU ventilated and they believe that his dad has a fighting chance to survive. Bob is asking why the ICU team thinks otherwise.
My Dad in ICU has a Fighting Chance to Survive but the ICU Team Thinks Otherwise. Help!
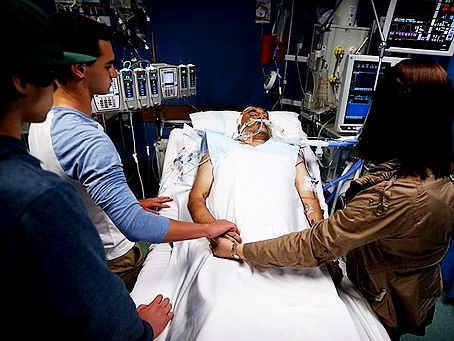
Hi Patrik,
I just found your website.
We’ve kept chronological notes on dad’s progress daily since this began and recorded as much as possible in regards to doctor’s phone calls and even a few of the rounds.
April 16, 2020, my dad who is 64 went in for an esophagectomy to remove a cancer from his esophagus. He had zero issues with chemotherapy and radiation that began October 8th. They took out 7cm of his esophagus and stitched it up. From day 1 there was a hole left in him.
He had woken up from the surgery and talked on the phone last with us 14th and was in terrific terrible pain. He developed a massive sepsis over 6 days. The hole was not found by 2 CT scans and was confirmed when the Gastroenterologist for the hospital got back from vacation.
He was admitted into ICU on April 22 and had swollen to about 5 times his size with all the fluids they put into him. On April 23 they rushed him into surgery and did the Esophagectomy again. Cleaned out a bunch of infections while they had him open.
RECOMMENDED:
At some point between 18th and 23rd, dad got a laceration on his left eye (hospital admitted it was probably someone being careless moving him around or in surgery) and an ulcer on his coccyx. Infections developed at both of those sites.
Also my dad’s kidney’s failed during the sepsis and as a consequence he got severe gout. He is currently on a slow 24-hour dialysis and was previously on a once daily dialysis. There was a bladder scan a week and a bit ago that indicated some urine had made it to his bladder but follow up scans have seen nothing.
Dad had severe respiratory failure initially and a pneumonia developed when he was admitted into ICU and was intubated. He also has had Afib problems with his heart and had to be paddled initially when he got to ICU. I’ve also been told he had an oxygen loss where he was out for a minute. 3 CT scans have revealed his brain structure looks okay.
After the second surgery they put in 7 drains for infection in his chest and other places. As of today he still has 4 drains. They put in a drain a couple weeks ago to clear out his gall bladder and 3 of his initial 7
drains were still there. Two drains are draining infection. One drain is draining a pocket of air and the other is doing nothing and they’re looking at taking it out.
I’ve been told he has a diffuse sepsis and still has pockets of infection all over the place including in the mediastinum between the lungs. He also has infection on his liver which the doctor today described
as “clots” from his last CT scan yesterday.
They’ve been monitoring his liver for a while which had a small infection that was apparently too small to drain. They believe the infection on his liver is causing problems clearing other infections. I’m not sure what their plan is for the liver but will be asking the doctor who comes on duty tomorrow.
Sedation ended in mid-May and he was re-sedated during his second pneumonia in early June.
At the end of May, my dad was making gains and infection was going away and it looked like his esophagus was healing. One day the ICU shoved a feeding tube into his stomach removing him from the TPN and feeding him via a tube going into his stomach.
They did this for about 4 days and another small leak developed his esophagus. I’ve heard the opinion from one of the doctors that it may have been caused by acid reflux. They put a stent in his esophagus to help protect it but it makes it difficult for the CT scans to show progress. They put him back on TPN and have no plans to change that.
At the end of May, my dad had contracted a drug resistant pneumonia from one of his lines and fought through it. They did a complete change of his lines and have been culturing them every few days.
They removed one drain and a follow up CT scan had a pocket of air in his chest on his left lung. Pockets of infection remain all over and he’s still in septic shock. My dad is having blood pressure drops when they rotate him, move him or do anything with him. My dad can’t take Tylenol 3 due to seizure issues so they’ve given him regular Tylenol and now Hydromorphone for pain management.
Suggested links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
As for his Coccyx ulcer they told us last week it was healing and drying out. 2 days ago they had a specialist come look at it and said it was starting to get necrotic. They put in a consult for plastic surgery
yesterday. Today I’m told they’re not going their yet and they’re going to try some other therapies.
In regards to his eye, from day one in the ICU we noticed his left eye became red and inflamed. Being sedated, my dad had poor blinking mechanics and we asked for someone to look at it. Someone finally came in May and prescribed high powered drops to both eyes to clear infection.
Dad was promptly forgotten about and not followed up. Dad’s eyes and especially his left eye dried out because no nurse was giving him any eye lubrication. An emergency visit by an ophthalmologist from a neighboring hospital was done 2 weeks ago and he prescribed my dad hourly lubricating eye drops and had his eyes covered by patches.
Eye cultures were taken from both eyes and the infection seems to have cleared, but a dead patch of eye on the left eye has developed. My dad’s right eye is looking okay. His left eye is now sewn shut except for a part to allow eye drops and lubrication and the right eye is allowed to be open with hourly lubrication.
Last week my dad developed a Pseudomonas infection in his lungs. He’s apparently clearing that and his lung functions are better. O2 most of this week is 97 to 99 usually with 25% Oxygen. His Peep is 10 and Pressure support was down to 12.
June 3rd the ICU consulted the infectious disease specialist who changed up Dad’s antibiotics to overcome things becoming resistant.
Tonight the Ophthalmologist visited and they sewed dad’s left eye shut with two stitches to help it keep closed. Ended patching for both eyes. Dad is now free to open his right eye and look around. The dryness of that eye will be monitored Hourly lubrication for his eyes will continue. They recommended this for 2 weeks and put in a dissolving stitch and one permanent stitch.
Recommended articles:
This week dad has been running daily white blood cell counts from 17 to 22. There have been periods before he was fed through his stomach were his counts had dropped down to 4 and 5.
Also of note, Dad has been the most awake I’ve seen him this week and opening his eyes for longer periods of time. He’s also moving his mouth lots like he’s trying to talk but can’t make any sound. I’ve also seen him blink on command for small periods of time and he can track you with right eye.
He’s only had limited time opening his eyes as they’ve been patched and only allowed to have his right patch off when visitors are around. He’s very weak and can’t move anything from the neck down but can feel stimulation when you touch his hands and feet. I’ve also heard him make what sounds like a snore.
The RT’s say dad has a very poor cough mechanic. Yesterday during rounds they were very happy with my Dad’s lung functions so they tried trach cradling him from the ventilator yesterday for 2.5 hours and he had blood pressure issues going back on the vent and he’s had trouble with heart rate and BP since. He’s been running a fast heart rate today and had a white blood cell count of 22 which is his highest that I know of.
Also today they hooked a new IV up to my dad and started giving him Sodium Bicarbonate. I’ve been told that this is to help remove Carbon Dioxide from his blood. They’ve also limited his range of motion exercises and stopped putting him in the chair due to blood pressure problems.
My mom and I believe that dad still has a fighting chance to heal. We need to come up with a plan to let dad heal up his insides, get rid of his ongoing sepsis related infections and get him off the ventilator. I
believe he will wake up and resume life when he is better. I feel devastated that we feel like the hospital is purposely fighting us and obfuscating the care that my father needs.
I do need help Patrik. I’ve been on a roller coaster wave of emotions since this began and living in fear of the ultimate phone call of my dad passing. I feel as I’ve been gas lighted by one doctor in particular and struggle between the weekly changes of doctors and daily changes of nurses.
Related articles:
Not to mention I’m struggling with taking care of my Mom through this and dealing with how she feels. I’m still learning about the ICU every day and catching on to things way too late. I don’t trust the ICU social worker and figured out early on that she works for the ICU’s interests and not me my mom and my dad.
I’m currently at work today and tomorrow. I have a 12 hour job which makes things difficult, but I would like to have a phone consultation.
I have been watching your videos and found the ICU Family meetings video really struck a chord with me since we’ve been through a few now and as I type this they want to do another family meeting.
I’d like to make a plan for dad’s treatment, make sure he gets that treatment. I do believe barring the catastrophic he can recover.
Regards,
Bob
Hello Bob,
Thank you for writing in and sharing your dad’s current condition.
Please find the details below. I have made a summary of the clinical information you provided. Assessments can be seen as well and my comments. For any questions, please feel free to ask.
Thank you.
Clinical Information Summary:
April 16, 2020
– Went for an esophagectomy to remove cancer from esophagus. Removed 7 cm of his esophagus and stitched.
April 17, 2020
– A hole left in him. Woken up from surgery.
April 18, 2020
– Talked over the phone, he is in terrible pain. Treated by pain management.
April 22, 2020
– Developed massive sepsis, hole not found on 2 CT scans until GI came back. Admitted in ICU and became edematous (swollen) because of all fluids.
April 23, 2020
– Rushed him into surgery and did the Esophagectomy again. Cleaned out a bunch of infections while they had him open. Had laceration over left eye (careless moving him around or in surgery?) and an ulcer on his coccyx. Infections developed at both of those sites.
ASSESSMENT:
Neurological:
– 3 CT scans have revealed his brain structure looks okay.
– Sedation ended in mid-May. Re-sedated in early June during his 2nd pneumonia.
– (+) seizure issues. On regular Tylenol and Hydromorphone for pain.
– Most awake this week, opening eyes for longer periods, moving his mouth, attempt to talk but no sound, blinking on command and tracking with right eye.
– Very weak and can’t move anything from the neck down but can feel stimulation when you touch his hands and feet.
– (+) snoring.
Patrik: Have they’ve been telling about his current GCS (Glasgow coma scale)? The Glasgow Coma Scale (GCS) is a neurological evaluation tool that allows the nurses and doctors to consistently evaluate the consciousness level of your loved one. It is important that they are monitoring your dad’s GCS on a routine basis.
You can read this article to know more about GCS and its importance. https://intensivecarehotline.com/questions/how-to-assess-glasgow-coma-scale-gcs-in-adults-and-children/.
Respiratory:
– With severe respiratory failure initially and pneumonia developed when he was in ICU and was intubated.
– June 3, 2020 – (+) Pseudomonas infection in the lungs. He’s apparently clearing that and his lung functions are better.
– FiO2 of 25% with O2 saturation of 97-99. PEEP is 10 and PS down to 12.
– As per RT, with poor cough mechanic.
– Yesterday, lung function is good, weaning off vent for 2.5 hrs done, heart rate and BP issues developed since then.
– Currently on sodium bicarbonate to remove CO2.
Patrik: Provided that your dad became positive for pseudomonas in his lungs recently, it is very important that he is receiving the right kind of antibiotic for that type of bug and that the nurses or RT should maintain aseptic technique while doing suctioning for your dad.
Moreover, if permitted, the RT should provide chest physiotherapy also for your dad. Furthermore, any recent ABG (arterial blood gas) results? Why is he having high CO2 in the blood? Have the doctors explained it to you? Are they doing routine suctioning for your dad?
Recommended links:
Cardiovascular:
– (+) Afib Paddled initially in ICU. (+) Hypotension when moved.
– Running a fast heart rate today
Patrik: Any cardiovascular specialist consult? Have they done any ECG or ECHO for that matter? Is you dad on any inotropes/vasopressors to keep BP within acceptable parameters?
Nutrition:
– TPN stopped, feeding via tube in his stomach X 4 days, (+) leak in the esophagus, caused by acid reflux? Stent in the esophagus placed to help protect, TPN resumed.
Genitourinary:
– Currently on slow-24 hour dialysis, on once daily before.
– With kidney failure, Got severe gout.
– Bladder scan done a week ago, with some urine -> follow up scans, no urine.
Patrik: How frequent are they doing the labs for his kidney function?
Skin:
– (+) Coccyx ulcer. Last 2 wks, healing and drying out according to them.
– Specialist came 2 days ago – ulcer is starting to get NECROTIC.
– Plastic surgery consult done, will try other therapies.
Patrik: Is your dad on any special form of bed that will prevent development of pressure ulcers? With the ulcer getting necrotic, any wound care consultation done? What therapies or medications are they giving now? They need not to neglect this because this can also develop as infection later on.
Suggested links:
Drains:
– 7 drains (chest/?) after 2nd surgery.
– Currently having 4 drains. Drain to clear out his gall bladder. 2 drains – draining infection. One drain – pocket of air draining. Other drain – for removed.
Patrik: Drains should be monitored on a routine basis and if drains are not needed, it is best to remove them one by one to prevent further development of additional infections.
ID:
– Diffuse sepsis. Pockets of infection all over the place including the mediastinum between the lungs.
– Infection on the liver – clots from last CT scan – too small to drain. The doctor to give plan regarding liver infection.
– End of May, infection subsiding, esophagus healing.
– End of May, with drug resistant pneumonia (?) from one of the lines. All lines changed, cultures done every few days. Still in septic shock.
– June 3rd, ID consult done, antibiotics changed to overcome things becoming resistant.
Patrik: Good that Infectious Disease Consultation done but they need to be aggressive in managing his infections.
EYE:
– Day one in ICU, left eye red became red and inflamed. Poor blinking due to sedation. Asked to be seen.
– Only by May, eye seen by the specialist, prescribed drops started to both eyes to clear infection. Dad was promptly forgotten about and not followed up.
– Left eye dried out, no eye lubricants being given by nurses.
– Emergency visit by ophtha from the other hospital 2 wks ago, hourly lubricating eye drops prescribed, eyes covered with patches.
– Eye cultures done, no infection? Dead patch of eye on left eye developed. Left eye sewn shut, small part open for eye drops and lubrication. Right eye is okay and open, on hourly lubrication. On monitoring X 2 wks.
Patrik: It’s obvious that they have neglected this part as well because it has developed since Day one in ICU and you have asked for someone to see it but only in May, the eye has been seen. Eye lubricants if prescribed by the doctor should be given routinely by the nurse, so if there’s a doctor’s order for that and they are not giving it to your dad, that is negligence on their part and that should not be tolerated especially if it progressed to complications like the one that happened to your dad’s left eye.
RECOMMENDED:
LABS:
– WBC: 17-22. With episode of 4-5 when fed through his stomach?
– WBC today: 22
Patrik: High WBC indicates infection. What are the trends of his WBC? What’s their treatment plan for this? WBC’s should also be routinely checked. If WBC remains high, the doctor may need to adjust his treatment. Once the WBC count shows a normal range, and clinically your dad looks okay, it indicates that the treatment is working.
ACTIVITY:
– Limited ROM exercises.
– Stopped mobilizing to chair due to BP problems.
Patrik: It is very important to mobilize your father once he is able to. Mobilization is the physical activity that, performed with the appropriate intensity, produces physiological benefits for your dad, acting on the circulation, central and peripheral perfusion, ventilation, and state of consciousness.
I hope this all helps.
Regards,
Patrik
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!