Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How To Stay Positive Whilst My Sister Has Severe Brain Injury in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Mikaela, as part of my 1:1 consulting and advocacy service! Mikaela’s sister has a brain injury in the ICU & she is asking if her sister’s tracheostomy can be removed.
My Sister Has a Brain Injury in the ICU. Is it Possible for Her Tracheostomy to Be Removed?
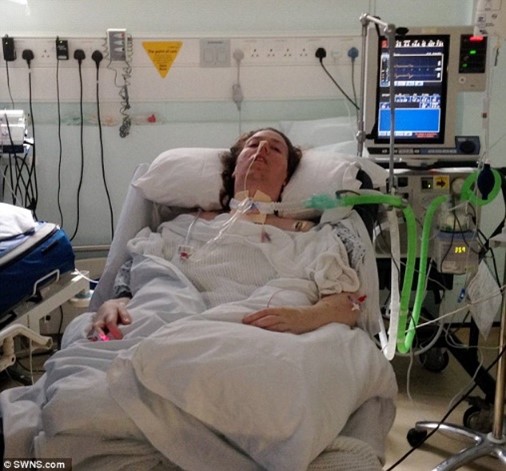
“You can also check out previous 1:1 consulting and advocacy sessions with me and Mikaela here.”
Rinzzie: So, I guess… So, what we’ve been doing, we’ve been using non-meaningful stimulus. These could be objects, mirrors, balls, touch, voice, those kinds of things, and we do it in a very standardized and structured way, because that allows us to repeat it and see if we can see any consistency, and we use different tools to do that. And that helps us produce a score, and also just compare where your sister is at. And then, what we also introduce is what we call experience of meaningful stimulus, absolutely… The recordings that you’ve left, music that your sister likes, things that are important to her, names, places, those kind of things. And then other things we’ll probably use are things like pictures, the things that she is interested in, sports. Whatever it might be that makes her who she is, we would also incorporate those things, as well, to see whether those stimuluses, do they make a difference in the case of someone’s level of processing?
RECOMMENDED:
Rinzzie: So, we’ve been doing that for probably about two or three weeks now, and at the moment, what we’re seeing is at the lower end of those things, those more reflexive behaviours, those similar patterns to responses to any kind of stimulus, which, I would agree with Dr. Rich that we’ve definitely had your sister with her eyes open more. She moves her eyes a lot more. I’m not seeing her move her eyes to a particular stimulus, so I feel like, at the moment, it’s quite automatic, again.
Rinzzie: But what we’re looking for is to see, does that… Is there any change? Can we see those subtle changes to see if your sister can demonstrate, or has the ability? It’s whether her brain can recover enough to show that, and that’s something we don’t know. This might be the best we get, we don’t know. We might get a little bit more, but I think, even if we got to the level of minimally conscious, which is that low level response, we’ve still got things like, has your sister got a cognitive impairment? Does she have memory problems? Is she orientated? Can she move? Because one of the things we have been seeing is, your sister doesn’t move her arms, and when she does move them, they move in a very unwanted pattern, if you like, so… And that causes stiffness and things, and… So, that’s another thing, we’ve got to keep our eyes on that physically, whether she can make any recovery that’s going to be comfortable for her in the future. That’s where we are at the minute.
Recommended:
Mikaela: How often are you physically getting her out of the bed, if at all?
Rinzzie: So, she is… Yes, she is… She’s having physiotherapy, they see her every day from a movement point of view. I think, because of your sister’s level of dependence, her age, her exercise tolerance, her cardiac condition, it’s very, very short. But yes, she is having experience of sitting on the side of the bed with four or five of us supporting her to sit, and..
Mikaela: Yes, it’s just because I feel like… Obviously, such things as bedsides and stuff. I know you’re aware of that, but you’re turning her over, and what not.
Rinzzie: She’s getting moved.
Mikaela: I feel like, sometimes, being in a position hours on end can be really uncomfortable for anyone, so if you can just perhaps get her up whenever you can.
Rinzzie: Yes, she’s moved very frequently, she will be sitting. At the moment, she couldn’t tolerate sitting in a wheelchair or a chair, for example. She just doesn’t have that ability just yet. And then, she’s having experiences of being sat on the gravity with support from us to what… What I would say is, she’s getting what can tolerate, and she’s getting what’s right for her at the minute.
Mikaela: So, in terms of… You say wheelchair and stuff, is it not okay… So, she’s able to… If she was given the assistance to be able to sit in the wheelchair, she can do that. So, it doesn’t have to be a case of can she, or has she got the capability to sit in a wheelchair?
Rinzzie: So, she’s not got… So, if we were to sit her in a wheelchair, she would very quickly develop fatigue, and that wouldn’t be good for her at the moment. So, we need to think about what she can tolerate.
Mikaela: Yeah.
Rinzzie: Yes. For example, what happens after 10 or 15 minutes, her head starts to really pull down, obviously, from the fatigue. But we really are working. She’s not gonna be able to then participate again. So, we do it in a way that’s best for her, and what I said about… She’s getting what she needs, and what she can tolerate.
Mikaela: Yeah.
Dr. Rich: Although, I know you understand, there’s a process that works up towards that.
Mikaela: Oh, yes, no, absolutely. I know, that’s fine, I totally get that. It’s just-
Dr. Rich: Her physical stamina can improve even if she’s not… They’re getting her muscles going again.
Rinzzie: Yes, just the sitting in bed is..
Mikaela: I feel like… Yes, because generally, she is quite active, isn’t she? She just-
Joseph: Yes, very active as well. When she was well, she took walks three, four miles a day, yes.
Mikaela: Yes, she did a good few walks, and they’re good two and a half, three mile walks. All kinds of that.
Joseph: We already talked about it, but she’s always been healthy.
Mikaela: And this is what probably contributed to it as well, when she was so active that she didn’t really consider her… Maybe, her weight, as well. The fact that she was quite overweight, and she drank quite a bit as well.
Recommended:
Joseph: I think… Yes, I think the heart problem, she’s never had any heart problems.
Mikaela: No.
Dr. Rich: It’s one of those things that just..
Joseph: Yes, and I know you probably will disagree with me, but as soon as she had the second vaccination, the Pfizer one. That’s when she said to me… I remember the week that she had it and she said, “My heart’s not feeling right, I’m… It’s going too fast.” So, I just ignored it, and I said, “Just calm down, it’s probably going to improve or something.” And then the next week, then she had it.
Mikaela: Yeah.
Dr. Rich: We just can’t know at this stage. There’s no way of looking back.
Joseph: Yes, and this is such a shock to us, because the heart it was never a problem.
Dr. Rich: It doesn’t look like it was actually a heart attack. It doesn’t look like it was a blood vessel that blocked.
Joseph: No?
Dr. Rich: No, I think it’s..
Joseph: It just came out of the blue, and this is why..
Dr. Rich: Yeah and actually, a lot of the time, you don’t get to the bottom of it. We see people who’ve just had a cardiac arrest, out of the blue. But for your sister, no idea what caused that, absolutely no idea. Nothing we could find that was the matter, and just like that, she had it.
Joseph: Yes. No, it’s just a shock to us, because she was so active. She was on the go all the time.
Suggested links:
Dr. Rich: Yes, we do see this. I think we just have to follow up with this process. And I worry about it, because this is going to be a long, really difficult road.
Rinzzie: I just feel because… I know you’re probably thinking, well, you’re prolonging her life, in a sense.
Joseph: But that’s what she wanted. She loved life, she wanted to live. We’ve had these conversations quite a number of times as a family, and I think all she said was that she absolutely loves her life, and wants to carry on, even if… We used to talk about people being disabled in the wheelchairs while shopping, and stuff like that. And she’d used to say, “Well, if they’re happy, then why have you got a concern?” So, this..
Dr. Rich: I absolutely agree. I’ve worked with the disabled plenty of times, many of who have a very good quality of life. I think our question is, if she can’t make any decisions for herself and you’re fully dependent, that’s different..
Rinzzie: So, that’s why were giving her the chance to..
Dr. Rich: I don’t know.
Rinzzie: We have to..
Dr. Rich: Yes, we’re in this situation. What I’m saying is, it’s not… We can describe what it should look like. What it actually tends to be, in our experience, it’s messy, its… What will happen is that your sister get infections along the way, her physical tolerance is being tested and the assessments are really designed for people being sat out in the chair, and that’s what we’re aiming towards, but how much… And how much of that she’ll be able to tolerate moving forward… Again, it’s a rehab goal that we’re working towards is to get her sat, regularly, daily. But that’s… There’s a process that takes time, whether that ends up being achievable or not, there’s a… We will look at whether it might be possible, and it is sometimes. Even in these circumstances, it’s possible to get her tracheostomy out. That’s, again, a very long and involved process for somebody who is as unconscious as your sister is. And I think it’s more than likely that we’ll do it, but it’s not to say we..
Joseph: There was something taken out the other day, something that was taken out of her?
Dr.Rich: It’s like an inner tube. There’s a plastic tube, and then there’s the inner tube, and they take out the inner tube and change it, or clean it, or whatever, to put it back in. There’s also a cuff inside.
Suggested links:
Rinzzie: I think they would manage it or something.
Dr. Rich: Sorry?
Rinzzie: The nurse said that she managed it quite well.
Dr. Rich: If you want to wean somebody off the tracheostomy, the first stage is to let the cuff down so that air is coming in and out the tracheostomy, but can also get passed up into your face and your nose and your mouth, and that’s one of the early stages of tracheostomy weaning. I wouldn’t anticipate there would be much of a problem with that. The other difficulty is, if she doesn’t have a good cough and things. If we leave that cough down for too long, then potentially, saliva and things can then get down into her airway, and cause chest infections. So, there was a bit of finding balance. I did do some injections into her salivary glands to try and hopefully reduce the amount of saliva.
Dr. Rich: It takes a couple of weeks to kick in, so we haven’t seen yet, but-
Dr. Rich: Because she’s not swallowing her saliva, it tends to just sit in a pool above her tracheostomy, and pool in the top of her esophagus. So, the only thing we can do about that is just to reduce the amount that it makes, so there’s less around, there’s less to get. We do re-aspirate some saliva in normal circumstances in small, very small amounts. So a little bit’s okay, but if you’ve got heaps going down, it’s just a medium for bugs to grow on, and you get chest infections. So, the reason for the Botox injections is we get less saliva.
Recommended:
Rinzzie: Also, she’s got quite big tonsils in her throat.
Mikaela: Yes, that’s always an issue. Yes.
Rinzzie: Yes. Do you think? Is that… Could that improve by removing them?
Dr. Rich: No, I think it’s not that.
Joseph: She’s always had that problem, though. She’s always coughing. Once… I think tonsils haven’t been a problem all her life, and she always said, “I wish I had got them removed.” And… But they are quite big.
Dr. Rich: Okay. We’ll have a look. If it gets to the stage where we think we need to remove it then..
Joseph: They’re quite big. Even I noticed them.
Dr. Rich: To be honest, I think, unless we see a significant step up in her cognition, I think it’s highly likely that tracheostomy needs to stay indefinitely.
Joseph: So, she’s moving to a ward, did you say, as well?
RECOMMENDED:
Dr. Rich: To the intensive care. It’s just because there’s a lot of other people.. We don’t want too many people in the wards with tracheostomies, because that’s how we can manage them all.
Joseph: For me, it’s the visitation, really. I can’t really go and see her. I haven’t seen her for the past two and a half weeks, now, which is a long time, and I’d like to see her today for half an hour.
Dr. Rich: Yes, I know where you’re coming from. Her brain will either be at this lower level stage, that’s where we’re assessing… What we’re doing is rehab. There’s nothing that can be done, it’s just trying to pick up on any early signs of recovery. We’re really in an assessment stage.
Rinzzie: It’s just been so difficult. It’s just been horrible.
Mikaela: Is there any such thing as a timescale for this thing? So like when you sleep too much?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!