Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Can you Fight for Your Loved One’s Life if the ICU Team Says Your Loved One is Brain-Dead?
You can check out last week’s question by clicking on the link here.
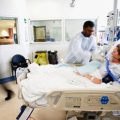
In this week’s episode of “YOUR QUESTIONS ANSWERED”, I am here with a live stream today, where I want to answer your questions if you have a loved one in intensive care. And this is one of the most commonly asked questions for families in intensive care and it’s a question that we get all time. And today’s live stream is about how long does it take to wake up after an induced coma?
How Long Does it Take for your Loved One to Wake Up After An Induced Coma?
So first, I want to encourage you to call into the show if you like and you can call me on 415 915 0090, if you’re in the United States or in Canada. If you’re in the UK, you can call me on 0118 324 3018. And if you’re in Australia, call me on 041 094 2230 and you can call live into the show.
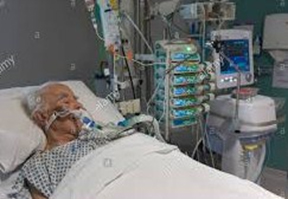
So many families in intensive care when they have a loved one in there, a majority of patients in intensive care end up on a ventilator with a breathing tube/endotracheal tube. When someone ends up in intensive care with a ventilator and an endotracheal tube or a breathing tube in their mouth, they need to be induced into a coma.
Simple reason for that is, this breathing tube or endotracheal tube is so uncomfortable, that it can’t be tolerated while on a mechanical ventilation. Plus the breathing tube is very uncomfortable. It’s obviously needed for intensive care treatment, if patients have a pneumonia, if patients come into ICU post-surgery when they were in the operating room, in the operating theatre and had anesthetics for surgery they can’t be woken up without a ventilator straight off. So that’s the background there.
RECOMMENDED:
Unfortunately in intensive care, some patients end up on a ventilator for longer than others. In the ideal scenario, you ventilate someone for less than 24 to 48 hours. Short-term, you wean off sedation. Hopefully a patient is neurologically intact and then can be extubated. From there, extubation is the removal of the breathing tube.
So that’s the background there, if someone can’t be extubated quickly and they end up on sedatives as well as opiates. Then, chances of a delay in waking up are definitely there. The longer someone is in an induced coma, the higher chances that there are delays when waking up. And that’s when all the questions are asked: “Why is my loved one, why is my mom, my dad, my brother, my sister, my spouse; why are they not waking up after an induced coma?” So that’s the sort of background there.
Recommended links:
And then it also depends obviously how severe is the critical illness. For example, is ventilation and the breathing tube temporary for, let’s just say open heart surgery. An open heart surgery, such as bypass grafts, coronary artery bypass graft, or valve repairs, and valve replacement. If it’s straightforward, then someone should be extubated after 24 to 48 hours at the most. Sometimes even after 12 hours, if all goes well.
If someone is in an induced coma, and a breathing tube and things are not straightforward, such as maybe a severe pneumonia such as ARDS/lung failure, multiple trauma, a head injury, or in a Guillain-Barré syndrome. The list is endless. I would say that anything that’s above 72 hours, 96 hours, three days, four days and if you’re trying to wake somebody up then it’s often not a straightforward process and it can take some time.
Now, it also often depends on what sedatives are used. Let’s just quickly break this down so you understand this. The majority of sedatives that are used in intensive care for an induced coma, Propofol also known as the Diprivan. It’s a white substance that’s given intravenously. Propofol or Diprivan made highlights many years ago when Michael Jackson died. Because apparently Michael Jackson’s doctor prescribed him Propofol for home use, which is unheard of.
If someone needs Propofol, it needs to be in a monitored and safe healthcare environment such as in an ICU, emergency room, or theatres. And that’s where Propofol can be given safely because you can’t really give Propofol without intubation or without ventilating someone because people stop breathing and it can ultimately lead to death, which is what happened in Michael Jackson’s case.
Propofol is also known as short-acting, which means it has a very quick onset. It sedates people very quickly. It puts them to sleep very quickly. And when you stop it, it also stops working fairly quickly. And if all goes well, people should wake up within minutes really.
Main side effects of Propofol are hypotension, which is also known as low blood pressure. In many patients in intensive care, you got to be very careful how much Propofol you’re giving, and if you’re giving a bolus because it can cause the blood pressure to go down.
Now, the advantages of Propofol are simply again, that it’s short-acting, and if you want to sedate someone and ventilate someone for a few days, and given that it’s short-acting, the chances of someone waking up after giving Propofol is higher than with any other medications. And I’ll come to that in a minute.
So when someone is induced into a coma, they often also end up with opiates/opioids. Opiates/Opioids are strong pain medications, such as Morphine, Fentanyl, Remifentanil, and Hydromorphone. Those are the most common opiates being used in ICU when someone is induced into a coma.
And again, the reasons for that is that the breathing tube or endotracheal tube in the throat is very uncomfortable. Patients are often in pain after surgery or after trauma, head injury or any other critical illness. It often goes hand in hand with pain unfortunately. So therefore you need to give strong opiates as well.
Now, the opiates come with undesired side effects, one of which is addiction. Especially when it comes to prolonged use of Morphine or Fentanyl. Other undesired side effects are respiratory depression.
Suggested links:
Now think about this, you have someone on a ventilator with a breathing tube or an endotracheal tube and the ultimate goal is to wean them off the ventilator. And now you’re having to give opiates such as Morphine or Fentanyl, and they have the side effect of respiratory depression.
Now that is a real concern because you want to get someone off the ventilator as quickly as possible and yet they are getting a drug that has respiratory depression as a side effect. So that is a real concern. And unlike Propofol, Morphine or Fentanyl are not short-acting. They stay in the system for a little bit longer. Some patients in intensive care go into kidney failure or liver failure. Thus, it takes even longer for Morphine or Fentanyl to be metabolized and again potentially delaying the waking up process.
It’s also important to notice that waking up in intensive care is often a process and not an event, especially when there are complications. Especially when someone has been in a prolonged induced coma. And I would argue that anything above three or four days in an induced coma, I would consider it as a prolonged induced coma.
Let’s just say someone is in an induced coma and it needs to be more long-term for whatever reason, maybe patients are awaiting surgery or are in situations such as ARDS which is very common at the moment with the COVID pandemic still going on. And then Propofol may not necessarily be the first drug of choice anymore. The drug of choice for a prolonged induced coma might actually be Midazolam, also known as Versed or Dormicum. And Versed or Midazolam is a benzodiazepine, and it’s more on the long-term acting drug classification. Whilst it has a quick onset as well just like Propofol, it stays in the system much longer and it takes a lot longer for patients to wake up.
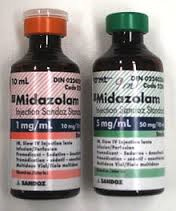
Now it doesn’t have the side effect such as hypotension or low blood pressure like the Propofol has. But the other effect that it has is, it is addictive as well, especially when it’s being used over long periods of time. So just from what I mentioned before, you have the combination of Propofol and Morphine or Fentanyl. And then you’re having Midazolam in combination with Morphine or Fentanyl.
Now, whether you’re using Midazolam and Morphine or whether you’re using Midazolam and Fentanyl, both are highly addictive. And when someone wakes up from an induced coma or is trying to wake up from an induced coma with those highly addictive substances, they may go through a withdrawal from those substances first before they can actually wake up and before you can assess their neurology properly.
Why is assessing someone’s neurology so important? So when someone comes off the ventilator, is trying to come off the ventilator, is trying to come out of an induced coma, you got to make sure they’re neurologically intact. They can obey commands. They can move all limbs. They can poke out their tongue. They can cough. Try to do all the right things. Why is this important?
Well, it is important, not only have you got to talk them through the breathing process, they got to be trained to breathe by themselves. They got to be shown how to cough again maybe. And you’ve got to make sure that all senses are there, because once you take the breathing tube out and they can’t maintain their airway, because they’re neurologically not intact, you’re having a big problem. Because you’ve got to put them back on the ventilator again.
So your time window to take someone off the ventilator and to get them out of the induced coma, to take the next steps towards getting them off the ventilator is time-sensitive. And you’ve got to choose the right time. So when you take the ventilator out or the breathing tube out, that people can continue without needing the breathing tube or endotracheal tube back in.
And what a lot of people have also reported, I have obviously seen it probably hundreds of times when I was at the bedside in intensive care as a critical care nurse. When someone does wake up, they’re often getting very agitated. They’re often breathing against the ventilator. They’re often coughing. They’re very irritated. And then one might think, “Oh, they’re awake. Why can’t you just take the ventilator out?” Well, the problem there is that, if you did that and they’re not following commands, there’s a very good chance they can’t maintain a safe airway and they’re not cooperative. Unfortunately you need patients to be cooperative and only then is it safe to take out the ventilator.
Recommended:
Now, if a situation like that occurs, some families report, they’re not trying long enough, they’re not trying hard enough. And I probably agree with that, that you can’t just take sedation off for a minute or two. And then someone breathes against ventilator, is coughing, and seems very agitated, potentially aggressive. And then you put the sedation back on again. I totally agree with that, that you need to give this some time. From experience, I would say at least 30, 40 minutes. And that’s a challenging period. Especially if someone is not cooperative. You need to possibly have a second nurse there and you need to talk to people. You need to talk to your patient. You need to calm them down if you can.
Problem is when they’re waking up, it’s very hard to assess what’s going on in their head. They often have no recollection of why they are in ICU. They have no recollection of what’s happened. They’re waking up, they’ve got a tube in their throat and they can’t make sense out of the situation. They can’t talk. It’s a horrible situation actually if you think about it. And they’re in ICU because they’re critically ill and therefore they may need the ventilator for longer than anticipated.
In any case, it is definitely something that many families have seen. They have seen that and they’re wondering, “Why is my loved one not waking up?” Again, all those medications they’re getting, whether it’s Propofol, Morphine, Fentanyl, Midazolam or Versed. Again, they all have side effects such as hallucinations. And when people are waking up, it’s not straightforward. Those drugs are also known that if given over a long period of time, they’re also known to induce ICU psychosis, ICU delirium.
Now I’m not suggesting that someone who’s been in ICU for three or four days ends up with ICU delirium or ICU psychosis. There’s enough research out there that suggests that the longer someone is in a drug-induced coma, the higher the chances they end up with issues such as ICU delirium or ICU psychosis.
Just coming back to what I described to you, that if someone is coming out of an induced coma, but is not waking up appropriately, is not cooperative, is breathing against the ventilator, is potentially aggressive and so forth. Another reason that might happen is simply that it might have a neurological event happening.
So what do I mean by that? When someone is waking up after let’s just say, head injuries or brain injuries, you’re almost expecting that waking up is not straightforward. But when someone, without neurological deficits or without a neurological pre-medical history, is not waking up appropriately and can’t follow instructions, can’t move all limbs, can’t poke out their tongue, can’t squeeze hands, can’t wiggle their toes, or whatever you ask them, then chances are they might have had a neurological event such as a stroke.
And then the next step is, that after maybe a few failed attempts of waking up, and with ongoing neurological deficits, the next step is to rule out a neurological event such as a stroke or maybe also another neurological event such as seizures.
Suggested links:
How do you do that? Well, next step usually is to do a CT of the brain and find out whether a stroke might have taken place. You should definitely make a neurologist or a neurology referral. That the experts need to look at that. So that would be another concern obviously, and it is something that needs to be addressed.
The bottom line is this, I can’t stress enough that waking up after an induced coma is a process and not an event. And therefore this can take time. And there are no firm timelines around this. Now I can understand your frustration completely because the longer it takes for your loved one to wake up, the more negative the ICU team will be and the more doomy and gloomy they will be. And they’re giving you all these negative and doom and gloom scenarios that you don’t really want to hear about. And at the end of the day, even if someone is not waking up for a week in ICU, after an induced coma, it’s still not a long time.
I can’t stress this enough that a week in ICU, even two weeks is not a long time and things like that simply take time. So, then the question is how long is too long? I’ve seen patients that all sedation has been off and then they’re not waking up for a few days. And you’ve ruled out a stroke, you’ve done a CT of the brain. There’s no stroke. And they’re still not doing anything.
So that’s when it really becomes tricky. But then again, you got to be patient in those situations. Problem is that, the longer someone does stay in an induced coma, the more deconditioned they get. The more time it takes for them to recover. You’ve got to do the physiotherapy, the physical therapy, or you got to get them mobilized. There’s definitely undesired side effects that come from not waking up after an induced coma, in a timeframe that seems appropriate. But again, the other issue that I believe is happening there is that, not only are patients being weaned off the sedatives and the opioids, they also had a critical illness.
And when someone is critically ill, the body more or less shuts down and simply needs time to recover, even without sedation and in induced coma. People are not machines and they just need time to recover. They just need to take time for themselves to let the body recover in their own time. And I believe that’s always a big issue as well, that it simply takes time to wake up.
So if God forbid, someone doesn’t wake up and therefore also can’t come off the ventilator, the next step in this situation is to do a tracheostomy. But even before you do a tracheostomy, if you think for whatever reason maybe a patient had too many opiates, too much Fentanyl, too much Morphine, and too much Midazolam in particular. Not so much of the Propofol because Propofol, the body can metabolize pretty quickly, but all the other medications namely Morphine, Fentanyl, and Midazolam or Versed, the body could take much longer to metabolize.
And then sometimes you may also have to consider whether an antidote needs to be given such as Narcan for Morphine in particular. That reverses the effect of Morphine. The same is happening for Midazolam. If Midazolam or if you think a patient had too much Midazolam, another medication or antidote medication that you can give for Midazolam is Flumazenil. Flumazenil is used to reverse some of the actions of the Midazolam in particular.
Other things that can happen when someone is not waking up after an induced coma or they’re confused, they’re not working with you, they’re not cooperative and so forth. You have to consider whether they are going through withdrawal. They’re going through withdrawal from the Midazolam or Versed, or they are going through the withdrawal from the Morphine or Fentanyl.
Another is, for whatever reason they have been drinking heavily before the ICU admission or they have been drug users, they might be withdrawing from alcohol, they might be withdrawing from drugs. And then that’s when you need to consider, “Okay, what are your next steps? How are you dealing with a potentially withdrawal situation?” And if you are dealing with a withdrawal situation, you might have to consider medication such as Clonidine or also Precedex, also known as Dexmetomidine that can help with withdrawal from medication or substances situation. So those are the things that are important.
One other thing that is important when someone is not waking up after an induced coma is sitting them up. That’s the bare minimum someone needs to do. You got to sit them up in the bed. That’s the bare minimum. Ideally, you can sit them in a chair. You can get them in a tilt chair or maybe even in a recliner. I know most ICUs, we’ll dispute that for some of our health professionals that are watching this, but I have worked in ICU where we have mobilized patients as quickly as possible even with breathing tubes. Is it more risky that the breathing tube will come out? Absolutely yes, but it can be managed safely. And it’ll just stimulate patients and it’s easier for them to wake up. It’s easy for patients to get familiar with their surroundings. There’s touch going on. Nurses are touching them when they’re getting mobilized. It’s just more of stimulation.
Other things that need to happen when someone is waking up after an induced coma is simply physical therapy or physiotherapy. Arm movement, leg movement, breathing exercises, and changing the ventilator settings during physiotherapy is important. And again, it helps stimulate patients.
RECOMMENDED:
I do want to leave it there today. It’s just a quick refresher. We have done many other videos and podcasts around, how long does it take to wake up after an induced coma? It’s just a quick refresher. Not much has changed from my perspective. I think if anything has changed, I want to leave you with that, especially for those of you that have family members in ICU with COVID and ARDS.
I think if anything, patients during the COVID pandemic have unfortunately being kept in an induced coma for much longer, because the option of a tracheostomy has often been delayed. Especially for COVID patients, because the risk for intensive care health professionals to contract COVID has been very high. Because of aerosols going into the atmosphere when doing a tracheostomy, therefore induced comas have been prolonged and the undesired side effects of an induced coma have come more and more to the forefront, which is even often a bigger delay in waking up after an induced coma.
So I hope that helps for today. This was a short summary. Go and like this video, comment down below what questions that you have if you have any follow on questions and subscribe to my YouTube channel for more of these videos for quick tip videos, for questions answered. And I’m planning to do more of these live stream videos, where people can either type their questions in the chat pad or where people can also dial into the show and I can answer their questions live.
If you have a loved one in intensive care, go and check out intensivecarehotline.com. Send me an email to [email protected] where I and my team will get back to you with some answers to your questions.
The shortcut really is to call me directly. If you’re in the U.S. call 415 915 0090. That’s again U.S. and Canada 415 915 0090. If you’re in the UK, please dial 0118 324 3018. That is again for our UK viewers and listeners, 0118 324 3018. And for our Australian viewers, please call me on 041 094 2230. That is again for our Australian viewers 041 094 2230.
There’s also a section on our website where you can schedule an appointment with me and then we can go on a phone call or on a Zoom call. And I also have a Skype account that you can see on our website, intensivecarehotline.com. You can also connect with me via Skype.
It’s a pleasure helping you and your families.
This is Patrik Hutzel from intensivecarehotline.com and I will talk to you in a few days. Take care for now.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!