Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Cathy as part of my 1:1 consulting and advocacy service! Cathy’s mom is in ICU with tracheostomy and Cathy is asking how her mom can have a quality of end of life.
How Can My Mom with Tracheostomy Have a Quality of End of Life?
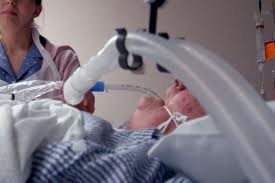
“You can also check out previous 1:1 consulting and advocacy sessions with me and Cathy here.”
Patrik: It’s definitely doable. You got to keep in mind though and again, that’s sort of when other things will hit home later as well. Most of our clients in the home care environment have 24 hour nursing care so there are people around 24 hours a day. So what I believe that’s the right choice for people, it comes at the price and I don’t mean that financially. To a degree you’re giving up your privacy. But I believe the intensive care at home is the right choice for the right clients. It’s still challenging.
Cathy: Right. But again, you get around that. If I have 24 hours, if I somehow are able to make that work, when I’m working, I have an office.
Patrik: Absolutely.
Cathy: If someone else’s here to create that separate. I mean, I don’t know maybe I’m just weird or something but all of that can be taken care of and you don’t have and I don’t have to, it’s the same thing with her in the dementia. At least I didn’t have to worry about someone attacking her in assisted living or nursing home. At least she was here and that’s a load office still doesn’t mean I wasn’t exhausted all the time, but that there was no heaviness that’s going to be in my chest if she’s somewhere else when I can’t even get people to understand, you just can’t go around killing people. So yeah that can be addressed very easily.
RECOMMENDED:
Patrik: Very much so. I’ll just give you another outlook so that we know what could happen. Let’s just say your mother will end up with a tracheostomy. Once she has a tracheostomy, they want her in a, have you heard of Altus?
Cathy: I’ve heard of it. Yeah.
Patrik: They would wander in an Altus as quickly as possible. And that may be a stepping stone, but if you are determined to have your mom at home, you might as well skip Altus and go home straight away.
Cathy: Okay.
Patrik: There could be advantages to Altus though. And it’s something you need to discuss with the neurologist. There are some Altus that focus on neuro rehab besides the ventilation side of things. They are far and few in between but I do believe they do exist. And the question is a lot of it comes down to you Cathy, what are the goals of care for your mother? Do you want to potentially put her through rehab or is it more important for you to have her home and maybe do less intensive rehab at home with some might be private physios, but you have her at home? You’ve got to weigh up what is more important for you.
Cathy: My mother wouldn’t do rehab. That’s been her issue the entire, she had her first stroke 14 years ago. She didn’t do rehab then. And then when she had one in 2017, she wasn’t doing rehab because she just wants to be left alone. And she’s not going to go through all of that. And I guess some people just don’t understand that, I was like, you can’t make people do things. If she doesn’t want to do it, she doesn’t want to do it. So you just deal with where she’s going to be. I mean, she lost the ability to walk but she was fine with that. As long as she could sit on the couch and you left her alone. I don’t see how after 14 years, if she were to regain some type of consciousness that she’s going to want to participate in all of that. I don’t see it.
Patrik: Yeah, sure. So again, Cathy, people talk about quality of life in ICU a lot, and they talk about, most of the time they talk about lack of quality of life going forward. Now, from my perspective they’re missing an important ingredient. It’s not in this situation it could also be about quality of end of life. People don’t use that term. They just use an absolute term, which is quality of life, but even quality of life. What does that mean?
Cathy: Right. Exactly.
Patrik: Quality of end-of-life could simply mean you want to spend time with your mom at home for whatever time she has got left. That is quality of end-of-life. But people in ICU in particular, go down the track much quicker without telling you.
Cathy: Exactly. So for the 24 hour nursing care, is that something that insurance companies pay for?
Patrik: Yes, and no. It depends which insurance, it depends on service availability as much as I would like to offer the intensive care at home service to you we are not in your area yet. But there are other options I can definitely point you towards other nursing agencies. Is insurance paying for it? I don’t know it depends on the coverage of insurance. The issue that I know that some families are dealing with is, I talked about Altus. Altus are designed to save the health insurances’ money.
Cathy: Got it.
Patrik: All right. Home care is potentially more expensive than Altus potentially. So it really depends on the insurance. I know that Medicare in particular and also Medicaid from my understanding the pathway with Altus is pretty much a Medicare on the Medicaid pathway to save money. So then it really depends on the insurance.
Cathy: Okay. And again, that is something that they can figure out. I just don’t understand why they cannot take my direction and move forward with it.
Patrik: Too hard.
Cathy: I told you what I’m going to do. I told you that I think you would be killing her I’m not going to do that. And so let’s see how we get her out of here. You want an extra bed I want her out of there. As far as timing and then with the tracheostomy should I go in and say, I want another seven days, and then after that you can do the tracheostomy and then we’ll talk about Altus versus how do we get her home because I did present that as an option.
Patrik: Yes, I would argue that’s the right approach.
Cathy: Okay.
Patrik: Because what they will bring up inevitably is if you do want a tracheostomy, they will start talking about LTAC and that’s when you bring in home care.
Cathy: Okay. That sounds like a wonderful plan.
Patrik: There will be obstacles to come though, whether it’s on an insurance level, whether it’s looking at issues such as, once even if you can get the finances organized for home care, any nursing service that’s taking on this role there will be issues around medical governance, in terms of who’s taking the medical responsibility. That can all be worked out, but what I am saying is its often not straightforward, that’s all I am saying.
Cathy: You’re right.
Patrik: And it’s the same, you see our biggest challenging organizing 24-hour care for a client is often not so much the finances and the medical governance, we’ve got the experience with that. What our issue often is, can we find staff?
Cathy: Right, exactly.
Patrik: I’m not saying it’s an enormous task, but it’s an enormous task for someone that’s not doing it on a day by day basis.
Cathy: Right. Exactly.
Patrik: I think what is important for you to know as well is if the ICU is pushing towards end of life they cannot withdraw treatment without your consent.
Cathy: Okay.
Patrik: That is really important for you to know, because ICUs are very good to pretend that they’re operating in a vacuum, especially when it comes to end-of-life. They’re very good at pretending like, “Oh yeah, we can do whatever we want”. No, no. There are many ICUs that are operating like Cowboys, really they say, “Oh yeah, tomorrow at one o’clock we’ll stop life support”. And just because I have seen this approach many times and just be mindful that you have rights, that they can’t just stop life support without your consent say with a DNR, they can’t just issue a DNR without your consent.
Cathy: Okay. Yeah. They did ask me that a lot. They said, “Well, if she goes into cardiac arrest again, do you want us to”? I’m like, “Yes. See if you can bring the breath of life back”.
Patrik: Yes. They told you all about broken ribs and all of that?
Cathy: Yes, they did.
Patrik: Sure.
Cathy: I’m like you didn’t break her ribs when all of this time that because she wasn’t really breathing when she left here or they barely got her pulse back before they put her in the ambulance and then she stopped again in the emergency room. You didn’t break any of her ribs then. And so yup, you’re going to keep bringing her back.
Patrik: I think that there is definitely a realistic chance that your mom will get out of there alive. As long as you can put everything in place that you want to put in place, but it won’t be easy.
Cathy: Right. Okay. Nothing has been easy.
Patrik: No nothing has been easy. But it’s doable, if I was you I would contact probably as early as next week, I will send you in an email. I will send you a contact. There is a nursing service, hopefully in your area, I’ll send you that in an email, they would be your first point of contact. They might be able to tell you whether they can facilitate home care for your mother going forward. Because once you know that and if they can’t help you, hopefully they can point you in the right direction.
Cathy: Got it.
RECOMMENDED:
Patrik: Is your mom in a city area, rural area?
Cathy: Small city.
Patrik: Small city.
Cathy: Small city, it’s like a suburb of like a more of a medium sized city. It’s a close suburb but the city is small.
Patrik: Because a lot of it comes down to staff availability. That’s why I’m asking, metropolitan areas are easier than rural areas.
Cathy: Right. Exactly. No, we’re close enough to that city such that they should have, they might not have enough, but they should have some qualified people, that were an option and even if she has to go to LTAC, and that was my other thing, it’s like when can they kick her out of CCU?
Patrik: Yup. I can tell you often depends on a number of things, including but not limited to the insurance plan.
Cathy: Got it. Okay.
Patrik: But one other thing that I always say, let’s just say they come to you and they say, look, we’ve done the tracheostomy. We’ve got another five days and we need to get her to LTAC. Everything in life is negotiable. And it’s also a case of, if you were to go down the track of LTAC as a sort of intermediate step, you would have to look at those LTACs. You would have to look at least at two or three. Altus I don’t know how much research you’ve done. We very much are opposed to Altus, mainly because they are designed to save money. They’re not designed out of key really.
Cathy: Exactly. As most of these places are.
Patrik: Yeah. The other thing that I feel is very important Cathy is, your mother given the situation she is in, in order to get her to respond I also believe she needs to be mobilized.
Cathy: Okay.
Patrik: Especially now that she’s off the vasopressors, she should get out of bed.
Cathy: Okay. But even while she’s unconscious?
Patrik: Well, at least she needs to be sat up. They should be able to get the bed in sort of a chair position.
Cathy: Okay.
Patrik: Is she getting physical therapy?
Cathy: No.
Patrik: They need to start doing that. How do you get someone, you’ve now looked at the Glasgow Coma Scale? How do you get someone to go from a three to an eight or to a 10 or even higher? You’re not achieving that by not stimulating people.
Cathy: Right. Okay. I’ll bring that up tomorrow. Fantastic. Well, this has been great, Patrick. It’s caused some of this pressure to be, just to know that I’m thinking in the right path and I’m not being unreasonable or just they try to make it seem as if you just don’t want to accept that, she’s no longer with us. I would be willing to accept it if she wasn’t over there breathing on her own. I don’t know that’s just me, but yeah, this gives me what I need to move forward and I’m sure I’ll be talking to you again after we see how this goes, but it just gets so well after that first conversation that we had when I was clear about what the parameters were going to be. That this is just really the next step and give me some time to really look into seeing if we can bring her home. I can say she has some really good insurance I don’t know how they would, how things operate around home care. You make sense that they would finance it but we’ll see.
Patrik: Yeah, you will see and also sometimes from experience depending on your insurance, if it’s a private insurance, they may fund some of it and then maybe Medicaid or Medicare might fund another proportion of it. Again, you might have to tap into more than one resource,
Cathy: Right. Okay.
Patrik: To make this happen. You are not unreasonable, there are many, not that I say many, but there’s probably hundreds potentially thousands of people in the world living at home on a ventilator. You are being unreasonable from an ICU perspective, that’s all. But that shouldn’t concern you.
Cathy: I don’t care about them.
Patrik: When I was still working in ICU. And I was trying to launch this service intensive care at home people thought I was a lunatic. But that’s just like any industry, there are always niches that need to be filled always.
Cathy: Right. Exactly. And you know what they’re doing it just doesn’t work. As I explained to people, who are just like, “Well, you need your own life”. I said, one of the things beyond, again, I just believe God put us in families and we’re supposed to take care of each other. Looking at how much those places cost I’m like, I’m not going to give someone $5,000 for my mother to tell them to get out of her room. I’m not going to do this. She can just stay in her own place and pay a fraction of that. I just don’t understand why people think that this is the norm. I was like, you’re killing yourself, trying to pay for this when they can just stay in their own place.
Patrik: The problem Cathy, that I can see as much as every family situation is unique, the ICUs are taking a one size fits all approach. And you know I know that’s not working.
Cathy: Right. Exactly
Patrik: What I’m hearing from you, I hear four times a week. I know it’s very unique to you, of course it is. But I hear this several times a week, I’ve seen these hundreds potentially thousands of times in ICU and they have just having a one size fits all approach, will just let people die, will just euthanize them without saying so and our problem is solved.
RECOMMENDED:
Cathy: Exactly. But it just doesn’t make sense for me, if everyone complains about the cost and all of that, I just don’t understand why you spend all the money on assisted living as a family. You drain every cent when they can just stay in their own house. And if they wander, it’s called putting a lock on the door and you have different people just to sit with them as you need to. But why would you spend that amount of money to be locked up in a facility that does not making any sense to me?
Patrik: No, it doesn’t.
Cathy: So anyway, I think our time is up.
Patrik: Look, you’re on the right track.
Cathy: Okay.
Patrik: You’re the right track, but expect some obstacles and expect some doctors like you’ve already noticed some doctors will be supportive and others won’t.
Cathy: Right, exactly. Thanks.
Patrik: I have sent you in a message here on Skype, I don’t know whether you can see that Bayada nursing service. Can you see that?
Cathy: Okay.
Patrik: So type that into Google when you get time and contact them. And as I said, if they can’t help you hopefully they can point you in the right direction.
Cathy: Okay. That sounds great.
Patrik: Do you have any other questions at the moment?
Cathy: No, not right now, because that was the main call for me, just was I nuts because I’m just trying to transition her to come home and again, I don’t understand all this institutionalizing people got room in your place and you can, beyond needing to know how to read and operate the machinery. You do need that type of skilled care but if I have a life and I dedicate some hours and then I have other nurses coming in, I think I should be able to manage everything here. If I could manage her with dementia, where I had to make sure that she couldn’t get out of here. So that was the main thing that was really stressing me out to how to make that happen and what they’re able to do and you are prepared for them.
Patrik: And what I’ve done as well, I just sent you another link on Skype to our other website, Intensive Care at home, even though again, we can’t help you with that in your area. However, you can use that as a reference point to the hospital as well.
Cathy: Okay.
Patrik: Right. Or you can definitely use that as a reference point.
Cathy: That sounds great.
Patrik: If you need anything, please shoot me an email. And we’ll go from there.
Cathy: That sounds great. And yeah, I’ll schedule other sessions as we get to the next stages that I’m definitely going to come in because you’re right. Because I saw one of the patients, I was like, “What is he sitting in”? But that’s what they did. They had some type of bed or something where he was kind of chair like position. So we’ll go from there. And we’ll be in touch.
RECOMMENDED:
Patrik: Okay. All right, Cathy, very nice to talk to you. And hopefully you can take the next steps.
Cathy: Absolutely. Thank you so much and enjoy rest of your day.
Patrik: Have a good day. Have a good night. Thank you. Thanks Cathy, bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!