Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
My Mom Is Unconscious And Ventilated In ICU. How Can My Mom Come Off The Ventilator?
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Cathy as part of my 1:1 consulting and advocacy service! Cathy’s mom is critically ill in ICU and Cathy is asking why the ICU team wants to withdraw treatment for her mom.
My Mom is Critically Ill in ICU and the ICU Team Wants to Withdraw Treatment. What Should I do? Help!
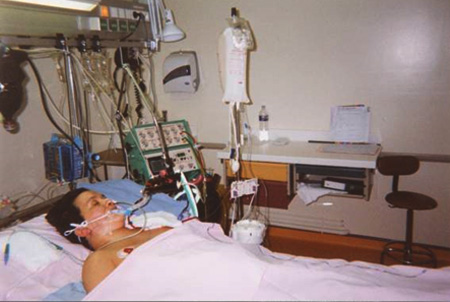
“You can also check out previous 1:1 consulting and advocacy sessions with me and Cathy here.”
Cathy: But I’m not going to do that because I straight up told the nurse practitioner, I’m like, I’m not going to kill her. And if you’re going to ask me to relieve the ventilator and all of that, you’re killing her and I’m not really trying to do that. And she kind of backed off.
Patrik: Good.
Cathy: That’s how I feel about again all of that. And again, this is if God has put the breath of life and I told her that, I said, and what I was trying to get at is at what point can you bring her home? I said, because if she stabilized enough and I’m trained on some things, and then I have some other people in here and we kind of work all that out, she can come home. And every time I say things like that, people just are like but what about your life? And I’m like, it’s about God’s will, my life is to be about what he would have for me to do. I have been looking after my mother’s health issues for 14 years. I had to kind of move in with her against her will. She had a blue body dementia or has it, and she was hallucinating and all that kind of stuff it had just gotten out of control beyond her like losing her keys and all that.
RECOMMENDED:
Cathy: So I had to try to step in, but my intent was always to get her to a point where she could be independent, she wanted to, because that is one thing about my mother. She is very willful. She wants to be left alone. She wants to be by herself and she just wasn’t realizing, I didn’t realize how bad she was because I lived in Ohio for many years. And she is in Florida and I manage everything from there for all those years. And then when it just became and you don’t really realize what’s going on because you’re talking to them over the phone as long as they sound normal it’s like okay, it’s normal. And then I came down here and I’m like this is not good. And she really started hallucinating and she would go outside and lose her balance and busted her teeth. But that will was still there, I tell people, I’m like you say all of these things about people in dementia, there is a part of their mind still there.
Cathy: I mean, if you know anything about them, you can see it. And that part of them is true. And she just, I couldn’t put her away because I just don’t think that’s what you should, that’s why we’re in families. We take care of each other, it’s hard but that’s what you try to do. And especially here like the past three years my mom, my grandmother was like this too. They want to sit in the house and they want you to leave them alone. As long as they can do that and they go to church on Sunday, they’re fine. And most people would say well, that quality of life you need to do. That’s not what she wanted to do, that’s not what she wanted to do. I tell people, all these people have relationships with God. You don’t know what’s going on I’m just trying to be helpful and supportive and as the kid I have to be obedient to her as my parent doesn’t mean it’s going to be easy.
Cathy: There’s not been one minute, she fought me every single day on everything because she did not want anyone here. But at the same time, I wasn’t going to lock her up. And that’s what I was telling nurse practitioner, if she’s in the other room in her bed and she just spends the rest of her life looking out the window at the sunshine. If God has given her breath, then that’s what she was meant to do and I’m fine with that. And they never can get over this, but even people, my family’s like you had to stop and give up your life. My life was taking care of her then, not saying that it was easy at all. You get so exhausted you can’t even cry. You can’t do anything. I have been completely exhausted for these past three years.
Cathy: But I’m here to do what God tells me to do. And he’s just has not told me to leave her or do anything like that. And it’s the same thing with this. So what’s like, how can I find the person that gets beyond. You just can’t give up your life like that. I’m not giving up my life that has now become my life to look at, God has given that as my job now. I look after her so I was like if you all can’t see that, then this is not the place for her and she can just come home. So how do I make sense?
Patrik: Yes.
Cathy: That’s what I’m trying to get them to understand and they’re just shell shocked.
Patrik: Yup. I do believe I have answers to all of that. Let’s just say worst case scenario, your mom ends up with a tracheostomy and on a ventilator. Let’s just say that’s the worst case scenario. Again, that’s what we do with our service here, we look after now dozen of people at home instead of intensive care with intensive care nurses on a ventilator with a tracheostomy. That’s what we do. As I said it’s not mainstream yet, but it’s there so it’s definitely possible. The other thing, better case scenario your mom wakes up, doesn’t need a trach goes to rehab, goes home without a ventilator, goes home without a tracheostomy would be so much easier. And that’s why I’m saying look, I agree that she may not wake up to the degree or she may not be able to live the life she lived before but again, if it’s meaningful for you and if it’s meaningful for your family, then it’s not for the ICU to make a decision.
Cathy: Exactly.
Patrik: So there are options. Do you feel like all of them are on the same page, the doctors intensive care doctor and urologist, are they all on the same page?
Cathy: Yeah, I’d definitely say like the person who runs the CCU, the neurologist he’s kind of one minute he’s like, “Well just let us know we’re just going to wait for her to wake up and you just tell us what you think she would want you to do”. And then the next he’s just like, “There’s no response. She’s not responding”. So I don’t know what to think and again, as I said because, and that was after I had that initial conversation with you and really prayed about it. And God was like, if I believe the breath of life, they’re alive. I’m like, okay, we’re going to move forward with that.
Cathy: And that’s when they sent the nurse practitioner in to talk about me. And it was quite obvious because she’s been in there before just for various high blood pressure issues. And they always come in like again, it’s not like on TV. It’s not like, “Oh, we’re going to attack this problem to get you healthy”. And it’s like, the other issue I’m dealing with is realizing that this whole CCU situation is not about making you healthy. That is not their goal. You’re there to extract money out of them. It’s like I’m embattled to get her out alive or just with some dignity.
Patrik: Yep. Well, this is very unfortunate, one way to get money out of this situation for them is to let your mother pass away as quickly as possible and let the next patient come in. You know that there is a huge demand on ICU bed unfortunately even before COVID, now it’s even worse. There was a huge demand on ICU beds. You don’t need COVID to justify the need for ICU beds. So unfortunately one way for ICUs to make money is high patient numbers rather than lower patient numbers with long term stays, they’re more or less loose, the longer a patient is in ICU the more money they generally speaking loose.
Cathy: Correct.
Patrik: And here is another thing ICU staff I believe are desensitized.
Cathy: Right. Absolutely.
RECOMMENDED:
Patrik: So your mother dying. Okay, well she’s just a number, she’s just another patient. We don’t know your mother from what her life was like before. We don’t think it’s worth living for her, end of story. And also ICU, I tell you another sort of framework that ICUs operate in, ICUs are very good, what’s happening in ICU as soon as the patient leaves ICU, they have no idea what that patient’s life looks like in six days, six weeks, six months or six years they have no idea. Absolutely no idea so they’re very poor at looking outside of their little bubble. And they also have no idea what people are prepared to do outside of ICU to keep their loved ones alive.
Cathy: That’s it. Yeah, because they’re not about keeping you healthy. They’re not about keeping you alive. It’s easier just to say there’s no hope goodbye. I’m like, that’s not what they do on TV. I guess my question is how do I determine when they’re going to try to force the issue because I’m comfortable with going in and saying, “Okay, well she needs more time”. Because the doctor that came in today, he was like, “I understand that you want more time and that is not unreasonable at all”. He’s totally different from the other ones that I’ve been dealing with. And he’s going to be there all next week.
Patrik: Sorry. What did he say?
Cathy: He said that I understand that you want to have more time with her, and he said that’s not unreasonable.
Patrik: Okay, great. And who is this, the intensivist or the neurologist?
Cathy: He is an intensivist.
Patrik: Great. So look, why have they not forced the issue yet? Some ICUs are quicker than others. Some ICUs they would have forced the issue by now. It will come up inevitably unless your mom shows signs of improvement. Now I do believe when we last spoke, I think I mentioned to you that I would send you a Glasgow Coma Scale and I think I never did. I’m very sorry.
Cathy: It’s okay.
Patrik: Did I mention this to you last time?
Cathy: Yes.
Patrik: Do you have access to your email right now?
Cathy: Yes.
Patrik: Can you have a quick look, I sent you a Glasgow Coma Scale just a minute ago because I think it’s important for us to quickly look at this. That would give you some guidance.
Cathy: Okay. I’ve got it up.
Patrik: Okay. So have a look at this and it’s very much self-explanatory. Where would you say your mother sits and you go through the eye opening?
Cathy: She’s no response. Verbal, no response. Motor response, no response.
Patrik: Okay, so she’s a three?
Cathy: Yeah.
Patrik: So that is the lowest score of a Glasgow Coma Scale. Have they brought up the Glasgow Coma Scale at all?
Cathy: No.
Patrik: Okay. I’m surprised that if she’s Glasgow Coma Scale of three and she is on no sedation and she’s in a natural coma, I am actually surprised that they haven’t brought up the topic of brain dead, have they?
Cathy: They just said we have not declared her brain dead, but we might do that at a later time.
Patrik: Right. That’s a very confusing statement from my experience. You’re either brain dead or you’re not, and you can determine that neurologic with tests.
Cathy: Yeah. And when I asked for an explanation of the test, I get what we want to look at is there, examining them and seeing their physical response as opposed to trying to decipher a test because they did an EEG and a CT scan.
Patrik: Yeah. But there are other tests. Have you seen the CT scan report and have you seen the EEG report?
Cathy: I have not seen the report. I asked the nurse about it and she kind of summarized it, but I haven’t seen the report.
Patrik: Right. If I was you I would, you can request them. I would read through them if I was you.
Cathy: Okay.
Patrik: If your mother was brain dead, I do believe they would have tried to determine that by now because that is unfortunately the quickest way to get somebody out of ICU. And also if somebody is brain dead in most States and countries, people are legally dead. There is an exception to the rule and there are people who have challenged that in courts successfully. But in other it depends on the state you’re in, I know somebody challenged this successfully in California a few years ago. But I also know that people challenge it all the time, sometimes successfully most of the time unsuccessfully. So that’s what I’m saying if the brain dead route if determined, it’s the quickest way to tell somebody is going to “die”, even though heart is still working kidneys are still working, but the brain is actually dead. There is a difference between someone being brain dead and brain damaged there is a difference.
Cathy: That’s a good point.
Patrik: I would argue with that your mother at this point in time is deemed to be brain damaged.
Cathy: So the fact that she is breathing on her own she could still be brain dead?
Patrik: Well that is the question. Is she breathing on her own? Do we know that?
Cathy: Yeah. He changed the setting. I think it’s called the apnea setting.
Patrik: Yeah.
Cathy: So they set it for what, nine or 12 breaths a minute. And if she’s not hitting that, then the ventilator kicks in. And so specifically during like a two hour period, it might’ve had to kick in twice.
Patrik: Yup. So that is a sign that she’s not brain dead then because if somebody is brain dead they’re not triggering any breaths.
Cathy: Okay. So that’s where we are and again, the kidney is still functioning. And even the person, the nurse in ER before I got the doctor down there to talk about anything, she was just like, I was expecting her lungs to be so much worse than they were. She’s not diabetic, she’s been taking the nutrition well, she’s still having bowel movements. Again, she’s maintaining the temperature that had been a big issue. It took them a long time to get her warm back up, but she’s been maintaining her temperature, potassium, and magnesium are all in right levels. Liver enzymes were trending down.
Patrik: Yep. Good.
Cathy: So I mean like her blood work is fine. She’s just is not responding. And my thinking is with dementia patients and all of that, she didn’t want me here and all of that, she just stopped eating and lost a ton of weight.
RECOMMENDED:
Patrik: Right.
Cathy: A ton of weight.
Patrik: Leading up to this?
Cathy: Yes. And she could hardly speak because she has a mass on her thyroid, it’s genetic it runs in the family. And so she kind of stopped talking, but I be like, “Good morning ma” and she just didn’t want to speak to me and that was just like prior. I was like, I haven’t done anything, but I guess that’s just part of the dementia and that’s fine. But yeah, even before that she was just really weak and frail and there was just those situations there’s just nothing you can do.
Cathy: And that was the other thing when I was praying about it, it’s like she’s still breathing and that’s when I told the nurse practitioner and she’s like, “So you want to see if we can wean her off”? And I’m like, “Well, if I just told you that, I believe that if there’s breath in her than there that there’s life in there, you might want to answer the question of whether or not she could breathe on her own”. And it wasn’t until this particular doctor today, he came in and re-said it, just so it was triggering when she didn’t take the right amount of breaths that you can see that she’s breathing on her own for the most part and everything else is working.
Patrik: Now that’s good. Looking ahead as well, Cathy, let’s just say she will end up with a tracheostomy. No, let me ask you another question. If she wants to stay like she is today over the last week and she did have a tracheostomy and she could now maintain an airway with the ventilator potentially. Would you still want her at home?
Cathy: Yeah. If it’s something that I can handle and monitor that’s the question for me is, what does that entail? I mean, like you would have to have someone constantly looking at her vitals?
Patrik: Look, is that something you can handle by yourself? I argue, no.
Cathy: No.
Patrik: It does require special skills, such as intensive care nurse, intensive care respiratory therapist and so forth. Is it doable? Absolutely. But it wouldn’t be, and that’s, I have not seen transitioning people home successfully on a ventilator with a trach and the family managing it all by themselves I just haven’t.
Cathy: Yeah, no.
Patrik: But it’s definitely doable with the right support.
Cathy: Right.
Patrik: Definitely doable with the right support.
Cathy: The way that I look at this is I do my work from home. So I have two different jobs that I can do from home. So it’s not an issue of having to go to work. Right now I’m just so stressed out that I can’t do anything. And the stressful part is again, I don’t trust you people unless I’m there to keep her alive because you’re not listening to me. It’s not a bad outcome if she is not dancing, if she has the breath of life, she’s good. I’m good. And so that is a stressful part for me, again, even that I have to say to you, can we see if she can breathe on her own because I was looking at all of the other lab work and saying, these are all in the normal ranges, you expect in situation that organ start failing they have not. Am I missing something here? And so the only thing left is that there’s swelling in her brain, which will take time and no one knows how long that could be, that could be another decade. I’m fine with that.
Patrik: Very much so.
Cathy: So can we just see if she can breathe and if we get to that point, does she have to go to rehab or is there a way for her to come home because I’m not going anywhere. I haven’t gone anywhere and that’s the other thing is like, do you not hear me people I have been watching her for two and a half years. Not necessarily always that I’ve been the constant presence for two and a half years. I’m well trained in this so if we all here in this little house together until the Lord actually calls her home, I’m fine with that. So can we focus on getting her to that point? So yeah, my only question would be, I still have to have those times where I work because it only works if I can work a little bit.
Patrik: Sure.
Cathy: I don’t want her in one of those facilities because I can’t watch them and that was part of the mistake that I made with her having her with dementia is again, because she was so adamant, I don’t want anyone else in the house and no nobody is going to bathe me and no I’m not going to let anybody be feed me that I had to do that all by myself. It was more than rough. I know that this is a different level and I would need help, but I would totally be fine with I’m here, she’s here. And you’re just going to keep living that way. I’m fine with that. Just want to know if it is doable.
Patrik: It’s definitely doable. You got to keep in mind though and again, that’s sort of when other things will hit home later as well. Most of our clients in the home care environment have 24 hour nursing care so there are people around 24 hours a day. So what I believe that’s the right choice for people, it comes at the price and I don’t mean that financially. To a degree you’re giving up your privacy. But I believe the intensive care at home is the right choice for the right clients. It’s still challenging.
Cathy: Right. But again, you get around that. If I have 24 hour, if I somehow are able to make that work, when I’m working, I have an office.
Patrik: Absolutely.
RECOMMENDED:
Cathy: If someone else’s here to create that separate. I mean, I don’t know maybe I’m just weird or something but all of that can be taken care of and you don’t have and I don’t have to, it’s the same thing with her in the dementia. At least I didn’t have to worry about someone attacking her in assisted living or nursing home. At least she was here and that’s a load office still doesn’t mean I wasn’t exhausted all the time, but that there was no heaviness that’s going to be in my chest if she’s somewhere else when I can’t even get people to understand, you just can’t go around killing people. So yeah that can be addressed very easily.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!