Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Mom is in the ICU for Septic Shock. Is My Mom at the Last Stage of Treatment?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Laura as part of my 1:1 consulting and advocacy service! Laura’s mother is in the ICU for Septic Shock and Laura is asking if the ICU Team’s plan of care is in line with her wishes.
My Mom is in the ICU for Septic Shock. Her Vasopressin is Off, Does This Mean a Full Recovery?
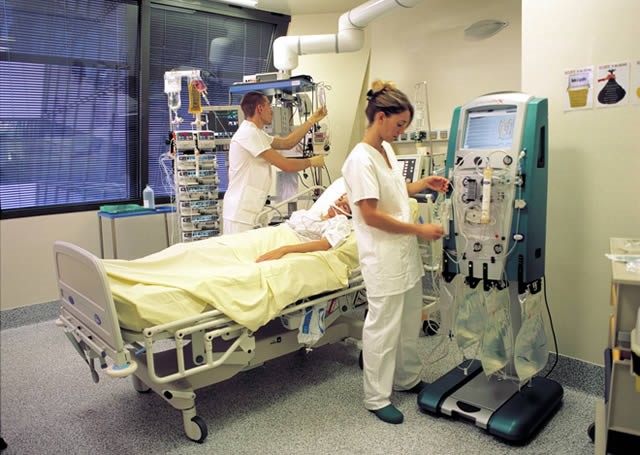
“You can also check out previous 1:1 consulting and advocacy sessions with me and Laura here.”
Laura: I talked to the Medicare lady and those were the words I used to her when I thought they were discharging us early. I did make some complaints about the treatment of the admitting doctor and the doctor in the ICU to the … What’s the name of the person who helps… supervisor? I made some complaints there, but I might need to up that complaint for everyone.
Patrik: I think you need to because it’s coming to a point where you don’t know what they’re going to do. Anything is possible and you sort of must prevent the worst-case scenario and one way is to starting using stronger language. How do you feel at the moment? You keep talking about the nurses. It’s probably a stupid question. Is it very tense, the situation? Or do you feel like-
Laura: Yes, it is.
Patrik: All right. Do you feel like there’s anybody on the team who’s compassionate towards you?
Laura: Not a whole lot. Not too much. The admitting doctor and the ICU doctor both are very intimidating and talking to me … from the beginning they’re doom and gloom, no hope and talking to me like I’m torturing my mom and just disrespectful and not caring or kind.
Patrik: Sure. Just let me ask again. The admitting doctor, is that the kidney doctor?
Recommended:
Laura: No, it’s not. The admitting doctor is the hospitalist. In some emergency room.
Patrik: Okay, I see. No, that’s fine. Please try those steps and get back to me. I would be very happy, that if you do have meeting, to be there over the phone.
Laura: Yeah.
Patrik: I would be very happy to be there and get your point across. Now that it’s three o’clock in the afternoon, I would almost argue that one of your next steps is to ring the Supreme Court, so you get them during business hours.
Laura: Yes, I will do that.
Patrik: Okay. Let me know what you get from there and then we’ll take the next steps.
Laura: Sounds good. All we’re trying to do is get her some time to see what happens and they’re just trying to cut it off.
Patrik: To see what happens, that’s exactly right. To see what happens.
Laura: Okay, well thank you-
Patrik: You’re very welcome. Let me ask you another question quickly. How big is this ICU? How many beds?
Laura: Good question. I want to say at least 20.
Patrik: Are they busy?
Laura: Yes.
Patrik: Do you think they’re full?
Laura: I think so. I think they’re pretty full. I think maybe four or five empty. I don’t know. Perhaps 75%, 80% capacity.
Patrik: Sure. Sometimes if they’re maximum capacity, they’re really pushed for beds. But even if they have a few beds empty, it still could mean they’re full because they don’t have staff. It’s all of that coming into play there potentially. All right, look, let me know how you go with the things we discussed and then please get back to me. We’ve got some time left and we’ll map out the next steps.
Laura: Awesome. Okay, thank you, Patrik.
Patrik: You’re very welcome.
Laura: Talk to you soon.
Patrik: Bye.
Laura: Bye-bye now.
Recommended:
Laura: Hello Patrik.
Patrik: Hi Laura, how are you?
Laura: Okay.
Patrik: They are giving you a second opinion and you’re thinking of should you take it or not.
Laura: Yes, because I’ve seen this doctor here before with the main doctor at ICU and that’s probably his buddy.
Patrik: Yeah, yeah. What are the timelines around this, in terms of-
Laura: I don’t know exactly but I spoke with the House Manager yesterday and I think it’s going to be a different House Manager today. I need to check in with them but there were saying they’re giving us some time and a grace period. She said even perhaps until the day after Christmas. But she said, “Not 100% sure.”
Patrik: Yeah, yeah. Okay. Okay.
Who did you speak to regarding that? Who did you speak to regarding this? To the doctor himself or did you get that second hand? Where do you get the information?
Laura: No. No, I got it firsthand from the House Manager. That was the number I was given by the head charge nurse in the ICU. So, I called her, her name’s Mona, she said … I said … I checked up again a second time yesterday. I said, “What is the status, or do we need more time?” She said, “Well, you can have her stay or we’re going to look into it.” She said that ITQ would keep me apprised to talk with them. Updates or whatever but I’m going to check in every day that we’re here with the House Manager just to make sure that we’re being heard but I don’t know if I should accept the second opinion because I feel like it’s almost a conflict of interest.
Patrik: Very much so. Very much so. What’s your mom up to? Has anything changed clinically since we spoke yesterday?
Recommended:
Laura: I noticed the Vasopressin is gone. That she’s only on the Levophed.
Patrik: Okay.
Laura: Yesterday was Vasopressin.
Patrik: Hang on-
Laura: It is .04 then yesterday was 15 Levophed. I think it’s Levophed now. Yes, just Levophed.
Patrik: Do you know how much Levophed?
Laura: And she’s- I think it’s the same, 14 or 15. I’ll have to double check, yeah.
Patrik: Sure.
What else has changed? Do you know? Is she still awake? Is she responding to you?
Laura: Yes, she’s awake. She is upset because she’s a very strong woman. She’s trying to tell me something with that tube in her mouth. Something is uncomfortable. The tube or some other issue. She’s more aware that she’s at a capacity level trying to communicate with me.
Patrik: Yeah, yeah. Are they talking in front of her? Like would they be talking about the overall situation in front of her when you are not there? Do you know?
Laura: I don’t know but I feel like … When they came in a moment ago with the new doctor, I was agreeing to it. I feel like I need to get back in there and say, “No, I don’t feel that this is the right second opinion that you’re throwing my way. It might be a conflict of interest.”
Patrik: Yeah, yeah. Absolutely. Okay, okay. What else happened in between when we last spoke? Did you manage … You spoke to the House Manager. Did you speak to the Supreme Court by any chance?
Recommended:
Laura: I tried to do that. I called the Supreme Court and she told me that I need to go to my county, which here at Los Angeles. She said you have to go there first. Then I was on a wild goose chase online and it was coming close to the deadline. I said, “Well I just … I have other avenues in place. I’ll have to go with those. You know second opinion and talking to the House Manager. I’ll just go that route right now.”
Patrik: Okay. Yeah, yeah.
What happened if you went back to them and said, “Look I’m not happy with this second opinion? Can I keep looking for my own second opinion?” What do you think will happen if you do that?
Laura: That’s my gut feeling, it’s what I should do. I don’t care what they say. I have rights.
Patrik: Exactly.
Laura: I want to exercise them.
Patrik: Exactly, exactly.
Laura: You can’t kill my mother by pulling these things off. You know?
Patrik: Correct. Correct. That’s number one. I think you should keep exercising your right. The other level you should argue on is your mum is awake, right?
Laura: Mm-hmm (affirmative).
Patrik: I mean, how can you terminate life support on an awake person because now your mum is potentially in a situation where she should be asked.
Laura: That’s right.
Patrik: You know?
Laura: Yeah.
Patrik: Your mum is in a situation where somebody can talk to her and say, “Hey look this is the situation.” We think this is what’s in her, “best interest” but let’s ask your mum.
Recommended:
Laura: Right. Now I feel like my time is of the essence. I’m going to have to cut this a little short Patrik.
Patrik: Yeah, yeah.
Laura: Something comes to mind I want to run by you, and I need to run by my family, is the breathing tube. We’re pretty much up to the 14 days. She’s breathing on her own every day. It’s a little pressure support but they’re not going to put it back in.
Patrik: Yeah, yeah. They-
Laura: Right?
Patrik: Are they … Have you heard of the term like one-way extubation? Have you heard of that term?
Laura: Yes. Yes, we have. Mm-hmm (affirmative).
Patrik: Are they using that term?
Laura: They’re not. I feel like they’re a little afraid to communicate with me or they don’t like to communicate with me because they … You know what I mean? The doctor even sent a nurse in yesterday to get my answer. He didn’t come directly to me. He’s very anxious, very rushed, very high strung. I can’t deal with that kind of stuff. That is terrible communication.
Patrik: Sure.
Laura: But what I’m asking is, if she’s coming to the end of the line on her 14 days of being intubated and she’s breathing on her own quite well, I wonder if she can just keep going with oxygen line, or CPAP, or support?
Patrik: Is she having … What’s the situation with nutrition? Is she still having no nutrition?
Recommended:
Laura: Yeah, no nutrition because the nutrition was sitting in there. I don’t know if it has to do with the bilirubin and level of consciousness that they say were rising. I don’t know if-
Patrik: Most likely. Most likely. That’s why … Did you see in one of my emails that I said she needs TPN?
Laura: No, I haven’t seen that. What is it PPN?
Patrik: TPN. T for Total, P-
Laura: Oh.
Patrik: Yeah, TPN. T for Total, P-
Laura: That’s P for Patrik?
Patrik: Yeah. N for nutrition.
Laura: Nancy. Nutrition.
Patrik: Yeah. And Nancy. What that means its basically intravenous nutrition. They’re basically starving your mum.
Laura: Yes.
Patrik: Right? I said that in one of my emails in the last couple days.
Laura: You did.
Patrik: She needs TPN urgently.
Laura: All right. I’m going to tell them to do that.
Patrik: You do. Also, by withholding nutrition, again, they’re starving her. They are, in essence, withholding life support. Not … People can go without nutrition for a few days, but she needs that nutrition now.
Laura: Yes. I agree. Okay. Is there anything else that comes to mind? I probably should-
Patrik: Yeah, yeah. Yeah, yeah.
Laura: … say no to this new doctor.
Recommended:
Patrik: Absolutely. Absolutely. Say no to this new doctor. I almost feel like … Have you … I almost feel like you need to ask for a meeting. No, no. Only ask for a meeting if they don’t accept your doctor. If they don’t-
Laura: Okay, say that one-
Patrik: Yeah, yeah. If you can buy time by looking for your own doctor that’s fine.
Laura: Yes.
Patrik: But if, for whatever reason, they don’t agree with that you need to ask for an urgent meeting.
Laura: Okay. Number one, we need time to find our own doctor. Number two, if they don’t agree to it then we need to ask for a meeting.
Patrik: Yeah, number three, have you … I’m not saying that you should be doing it, but you might have to taste the water. Have you threatened them with legal action?
Laura: I did in a smaller preliminary way. I said I’m going to get my legal team.
Patrik: Okay. What was their response?
Laura: Mister flighty man, he says, “Go ahead. Go ahead.” He’s so nervous.
Patrik: Nervous?
Laura: Yeah.
Patrik: Okay.
Laura: His name is-
Patrik: I think-
Laura: Dr. Charles. He’s the head of the ICU.
Patrik: Yeah, yeah. Okay. I think keep doing that as well. Keep referring to your legal team. There’s no point in doing that as yet but I think you should keep referring to that.
Laura: Yes. I agree.
Patrik: Keep them on their toes.
Laura: Okay. Well that’s good. Could you send me a little recap email?
Patrik: Yeah, yeah. I will.
Recommended:
Laura: I’m going to go back in there. I got to say no before they start-
Patrik: You will have to say no.
Laura: Thank you Patrik. I’ll keep in touch.
Patrik: Okay. All the best for now.
Laura: Okay.
Patrik: Bye.
Laura: Thank you so much. Bye-bye.
Patrik: You’re welcome. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!