Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
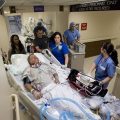
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Cathy as part of my 1:1 consulting and advocacy service! Cathy’s mom is still in the ICU ventilated and unconscious. Cathy is asking how her mom can come off the ventilator.
My Mom Is Unconscious and Ventilated In ICU. How Can My Mom Come Off the Ventilator?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Cathy here.”
Patrik: Hello Cathy.
Cathy: Hello Patrik.
Patrik: How is your mom today?
Cathy: Well, she is not taking enough breaths per minute and for the most part she’s been breathing on her own, there still is no response. My feeling on all of this, I approached this from a religious perspective is that, if there is still breath in her, there’s still life and her. I don’t want to turn anything off and that’s where we left it. I guess they came in and talked to me on Thursday and I just told them that I was like, as long as there’s the breath of life in her I don’t. Anything that goes against God’s word and that’s how I’m looking at all of this. Because I mean, from the beginning you were so right in some of the videos that you said, I mean, just so negative, she’s not going to make it.
RECOMMENDED:
Cathy: I mean this is even before they even gave me the option to do the therapeutic hypothermia. It was just like what’s her quality of life going to be like, and I said if she sits in the bed for the rest of her life and I have to take care of her for 24, that’s what I’m going to do. I’m just trying to get her to that point. And I don’t feel like they’re that’s ever been what they’ve been trying to do. It’s like they’ve been speaking death over her the entire time. So my question is really like how do you, if someone is still not conscious, can they even get off of the ventilator?
Patrik: Not while they’re unconscious in order to get off the ventilator they really need to be conscious. Having said that there is just something that remind me your mom doesn’t have a tracheostomy.
Cathy: No.
Patrik: So and that’s where it’s probably getting a little bit more nuanced, but bear with me. So somebody coming off the ventilator needs to be conscious more or less. Sometimes they are conscious and can come off the ventilator, but can’t be without a breathing tube. And the reason for that is they can’t maintain a safe airway. Now you can’t leave a breathing tube in the throat really for more than two weeks that’s sort of the guidelines. After that two week mark someone can come off the ventilator for whatever reason. Or if they can’t maintain a stable airway even though they can breathe by themselves, the next step is to perform a tracheostomy. Is it the first time you’re hearing about tracheostomy?
Cathy: Yes.
Patrik: Right.
Cathy: Yeah. And what’s the difference between the tracheostomy and the ventilator?
Patrik: Yep. So you have seen your mom, you’re not restricted with the COVID?
Cathy: Yeah. Not restricted at all.
Patrik: Yep. Great. So you would have seen the breathing tube in the mouth?
Cathy: Correct.
Patrik: That’s attached to the ventilator, you with me?
Cathy: Yes.
Patrik: Okay. So when, and that is very uncomfortable even though it may not look like it at the moment, but generally speaking if patients are more awake that’s incredibly uncomfortable. It’s one of the reasons why patients need to go into it an induced coma if they need mechanical ventilation, because they can’t tolerate the breathing tube in their throat. Now, in your mom’s situation because she is more or less, sounds to me like she is in a natural coma.
Cathy: Right.
Patrik: It sounds to me like, all sets of sedation have been off and she’s not waking up, which means she is more or less in a natural coma. Would that be an accurate description from your information?
Cathy: Yes. That’s correct. They have not sedated her at all the entire time.
Patrik: Okay. So now let’s just say she is breathing up even though she’s in the natural coma, let’s just say she’s breathing up but she still can’t follow simple instructions and she can’t wake up. The next step is to do a tracheostomy, okay?
Cathy: Okay.
Patrik: The tracheostomy is a breathing tube in the neck. It is much more comfortable. It is a much more stable airway. For example, if your mom was to cough a lot, there’s a very high chance she would cough out the breathing tube, much slower chance of the tracheostomy to come out. And it’s just a much safer airway people if they are awake, can often learn to talk again. It’s just painless, it’s just a lot easier. Also, no matter if your mom wakes up or not, it can prolong life and tend to give people time to wake up in their own time. There’s a time limitation on the breathing tube. Whereas with a tracheostomy I know of people Cathy for decades. Now I’m not suggesting that to be your goal, but I’m just giving you a perspective.
Cathy: Exactly. Okay. That’s very helpful.
RECOMMENDED:
Patrik: And then if your mom can’t come off the ventilator, she can still have a tracheostomy and be connected to the ventilator. So the tracheostomy and the breathing tube are similar devices that just is sitting in different locations, that’s all. Has anybody mentioned DNR withdrawal of treatment for hospice?
Cathy: No.
Patrik: The reason I’m asking this is you got to watch their words but even more so you’ve got to watch their actions. So it’s one thing to paint the negative picture it’s another thing not to bring up the next steps if you are painting such a negative picture. And the next steps, if you are painting such a doom and gloom picture is really talk about the goal of treatment, talk about hospice and talk about DNR. Do you know what I mean by DNR?
Cathy: Yes. The Do Not Resuscitate.
Patrik: Yeah. Alright. So I’m a big proponent of don’t worry so much about what they’re saying. Look at what they’re actually doing.
Cathy: Okay. Got it.
Patrik: So that in my mind is a positive sign that they haven’t brought that up. Do you have any thoughts around that in terms of either you expecting this to come up soon, do you have any thoughts around that?
Cathy: It’s hard for me to have any thoughts because I’ve had to come up with how I think about this by myself. Because she had the cardiac arrest, they’re saying it’s from a blood clot that went to her lung. And I get the emergency room people kind of come in and out, but don’t really say anything and maybe six hours after she’s been there, then I get this doctor that it’s like, “Oh yeah she’s not going to have good quality of life. She’s probably not going to wake up. But there’s this thing induced therapeutic hypothermia”. I’m like, well I would like to try to see if we can bring her out of it. And then he’s like, “Oh, well we better get started”. We need to do it within six to eight hours. It’s just like this lackadaisical attitude I don’t know what to think because I’m not going to listen to someone. I have to pull everything out of you.
Cathy: You don’t really tell me what’s going on and then I’m going to listen, then you say something that’s just totally divorced from logic. You haven’t provided me with any reasoning like what I know I’ve had to pull and do my own research and then come in and tell me, well, she’s not going to wake up, it’s not good. So it’s hard for me to gauge what that initial doctor was like. I just don’t know what to think about what they do. I mean because they sent in a nurse practitioner. So she’s in ICU, there was the emergency room doctor, I guess he was the intensive care doctor who kind of followed her up when they started the hypothermia. And then there is the Oh, I don’t even know what the guy that runs CCU and then the neurologist. I’m not very hopeful, not seeing any signs but nobody’s like no, like my whole well is she’s breathing then we’re not pulling anything. But no one’s like, okay that’s a good way to think about it, let’s see what that would look like.
Cathy: So I don’t know if they’re just like afraid because I’ve put up that kind of this is kind of the line here and then they’re not going to approach the subject. It’s just odd, all I can say is they have great TV programs because that has not been my hospital experience that you had this person that comes in educate you about what’s going on. It’s just like, so obviously.
Patrik: What do you mean when they say they have great TV programs, what do you mean by that?
Cathy: I’m a very logical person. So on television, you go in and they make a diagnosis and they talk to you about what it could be this, and it could be that, and this is why we’re going to try to do this. I’ve never gotten any of that I mean beyond my mother.
Patrik: I see what you mean.
Cathy: So my expectation, I’m always like there’s got to be something else coming from you, but there never is. It’s just me trying to figure out what’s going on with my mother is the reason why I’m so knowledgeable about her health issues. Because other than her primary care physician, that’s a whole other story about her refusing medical care. Everything I’ve had to research myself, there’s never been that moment where like on TV, where you had this doctor that like breaks down everything that’s going on. So that’s why I say it’s just so hard to read them. And I’m looking for it.
Patrik: You looking for guidance.
Cathy: Has someone has this happened before? What does it mean that you didn’t have to give her a sedative this entire time? Is her body just naturally protecting itself? It’s like, but you can come in all day and tell me that well, she’s not going to make it. And then the other thing that annoys me is just, they’re not even listening to what I’m saying. They’re like what type of quality of life and I’m like, you never know the purpose that God has for you. Sometimes people are just here for the love them. It doesn’t necessarily mean that the life doesn’t mean anything because they can’t go out and do salsa tomorrow. If they’re alive and breathing, then God has a purpose for them. That’s how I think about it.
Patrik: Yup. I’m with you on that one Cathy, I’m with you on that one.
Cathy: So given that then come back to me with options for how to make that happen. And she did kind of mention but the same thing as being negative, it’s like, well, we’d have to talk about doing a tracheostomy and then see about a long-term care facility. And they’re located here and there, but I don’t know if they would accept her. We’ll figure that out because I’ve already told you all the pathway we’re going to follow. But it wasn’t until I said that, that anyone thought to see can she breathe on her own, can we like use a machine to try to figure that out? I know I’m rambling I just.
Patrik: No. You’re not rambling. I’ll take everything that most of the things that you’ve just said and I believe I can map out the next steps.
Cathy: Okay.
Patrik: Because unlike the ICU team, who’s not telling you what’s going to happen, I believe I can because I’ve seen it so many times and I do believe that ICUs are so incredibly poor at looking at issues such as, okay what does it mean to you? What does it mean to your mom? What does it mean to your beliefs, religion, culture, spirit name all of that. Post ICUs have no time to engage on that level unfortunately. I tell you, and just remind me this happened last Monday, a week ago.
Cathy: Yes.
Patrik: Okay. So from my perspective, Cathy it’s still seven days in ICU, not waking up after a cardiac arrest with probably a hypoxic brain injury. Do you know what I mean by hypoxic brain injury?
Cathy: Yeah. She didn’t get the oxygen that she needed.
Patrik: Yeah. So probably has some form of brain damage. A week in ICU is still nothing, if you came to me in seven weeks instead of seven days and you had nothing, then I would say, okay we’ve got a serious problem here. Now once I agree with the doctors in terms of that she probably won’t go back to where she was before I also strongly agree with you that there is a purpose. And that from my perspective it’s not for the doctors to keep or take life.
Cathy: Right.
RECOMMENDED:
Patrik: That is a strong belief for myself as well. It’s one of the reasons, not the only reason but it’s one of the reasons why I’m doing what I’m doing. I could not stand any longer what was happening in ICU, what I could see with my very eyes and what I was at some point willingly, and then also down the track unwillingly participating in. I just couldn’t agree, when you’re young and you learn ICU you’re focusing on the clinical of course. But as time goes by you understand the politics and you understand how ICUs operate and then you can make up your own mind whether you agree with it or you don’t. And also before I map out sort of the steps that I can see take place where I am, we are running a community service intensive care at home. We are basically looking after ventilated patients at home. Sometimes our clients only have a tracheostomy and they’re not ventilated. And sometimes they don’t have a tracheostomy, but they are ventilated.
Patrik: So I know that there is life beyond the intensive care for long-term intensive care patients. Now this is not mainstream what we do, but it’s certainly getting more and more accepted. And we have referrals from ICU directly. So I know for a fact that there is life beyond ICU. I’m not talking about what other people think is a good quality of life. What I am saying is there is life beyond the ICU and there is meaningful life beyond ICU but other people might think wouldn’t be meaningful to them but that’s not for me to judge. My goal is always to give people options. But looking ahead let’s just say your mom doesn’t wake up, maybe another week goes by she’s not waking up, same situation. Then now she either will need a tracheostomy or the discussions around end of life might need to be looked into but with your input. And if you decide you want your mom to have treatment withdrawn, then it needs to be on your terms not on their terms.
Cathy: Okay.
Patrik: And as I said, I’m not here to make a judgment about what’s best for your mum. What I think is very important is for you to know that there are options one way or another. I tell you another thing, let’s just say end of life discussions come up from a hospital point of view. There is a very fine line between stopping treatment, which would be stopping ventilation, which would be, do you know whether she’s on any vasopressors like epinephrine still?
Cathy: Yeah. They’ve been off for a while.
Patrik: That’s good. So the reason that’s such an important question, whether the vasopressors are still going, they suppress us as much as well as ventilation is considered life support. If she was on vasopressors such as epinephrine and you would stop the vasopressors she would probably die. So now, knowing that she’s not on vasopressors the only form of life support with the information that you’ve shared is the ventilation.
Cathy: Correct.
Patrik: And she’s not on dialysis or kidney failure?
Cathy: Nope. Kidneys are hanging in there.
Patrik: Okay. Good. So that means we have established she is on one form of life support, which is the ventilation. If people are on multiple forms of life support and all the ICU team could just come to you and say, okay, we are in multiple forms of life support. We’re not improving let’s just stop life support and let your mother pass away. That would be one option. But even if they would stop life support now with the ventilation there is no guarantee that your mom would just pass away, there’s no guarantee for that. So then you could argue what is the right decision to make, stop life support and let your mother potentially suffocate to death or continue with the trach and give her the option to heal/recover in her own time. Now there are no timelines around that.
Patrik: But here is another issue where ICUs I believe are incredibly poor at communicating. So let’s just say they took out the breathing tube with the expectation that your mother would pass away. What would that look like she might suffocate, she might drown in her own secretions now in order to avoid that they both give her medicine to make her comfortable such as morphine, fentanyl and they’re not the strong sedative like midazolam. Now I don’t want to get too medic in here, but the crux is this if they were to do that from my experience and from my perspective, that is euthanasia. Are you familiar with the term euthanasia?
Cathy: Yes. Familiar with the term.
Patrik: Yeah. It basically means they’re hastening death by withdrawing artificial life support. But on the other hand also to keep her medicine that help her stop breathing and then she would die. And again, in ICU unfortunately this is common practice, but nobody calls ICUs out that this is euthanasia.
Cathy: Right. Exactly.
RECOMMENDED:
Patrik: Then people realized when it’s happening, ICUs are very good at making it look like, “Oh yeah, she’ll be comfortable and she’ll be she won’t feel anything”. Yeah that may be the case, but on an ethical/moral potentially religious even legal ground euthanasia is illegal in most countries in most States within countries. There’s very few countries where euthanasia is legal. Have you considered that at all so far?
Cathy: Considered?
Patrik: The end of life, potentially being hasted by ICU and that it could potentially go down a euthanasia track, but nobody actually calling it euthanasia?
Cathy: Yeah. I’ve considered it in that I don’t want to do it.
Patrik: Okay.
Cathy: I’m aware of what you’re saying but you meaning ICU if they were to bring it up?
Patrik: Yeah.
Cathy: But I’m not going to do that because I straight up told the nurse practitioner, I’m like, I’m not going to kill her. And if you’re going to ask me to relieve the ventilator and all of that, you’re killing her and I’m not really trying to do that. And she kind of backed off.
RECOMMENDED:
Patrik: Good.
Cathy: That’s how I feel about again all of that. And again, this is if God has put the breath of life and I told her that, I said, and what I was trying to get at is at what point can you bring her home? I said, because if she stabilized enough and I’m trained on some things, and then I have some other people in here and we kind of work all that out, she can come home. And every time I say things like that, people just are like but what about your life? And I’m like, it’s about God’s will, my life is to be about what he would have for me to do. I have been looking after my mother’s health issues for 14 years. I had to kind of move in with her against her will. She had a blue body dementia or has it, and she was hallucinating and all that kind of stuff it had just gotten out of control beyond her like losing her keys and all that.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!