Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM , where we instantly improve the lives of Families of critically ill Patients in Intensive Care, so that you can have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question that our readers ask quite frequently and the question was
“How long does it take to wake up after an induced coma?”
You can check it out here.
In this week’s episode of “YOUR QUESTIONS ANSWERED”, I answer another question from one of our readers and in this Kathrine from Sydney, Australia is asking
Kathrine writes
“A FAMILY MEMBER OF OURS IN HIS THIRTIES IS DYING IN INTENSIVE CARE AND WE’RE NOT SURE WHETHER IT’S THE ONLY OPTION, PLEASE HELP!”
Hi Patrik,
Thank you for your website, it is really helpful!
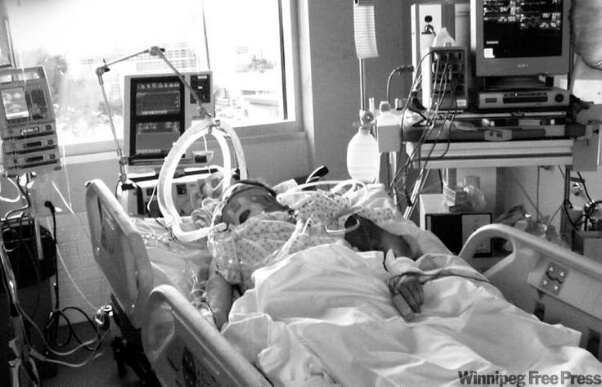
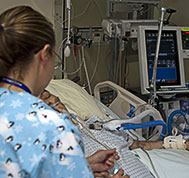
I am just wondering if you could assist me with my question please. One member of my family (on my husband’s side) is being put to sleep…for good…, after a shocking operation on his chest. He had a tube in his mouth and that was helping him with his breathing and the machine was just assisting him…
However, just two days ago, me and my husband visited him. Our Family friend was active and alive, he wanted to talk to us, but he was given more drugs to calm him down… And now, two days later, we found out that he will die…So we are extremely shocked to find out that apparently nothing can be done to save him…Why did the doctors not insert a Tracheostomy tube…?
Please see the photos attached. Our Family member is only young and in his thirties. We know that he was trying to breath by himself and that only 1/4 of his lungs are functional…Does that mean that there was no other options?…But to put him to sleep and let him die?…His father has got all the decision making authority, but I am unsure whether his father understands the whole situation.
So what was happening, all sudden our dear nephew felt pain in his chest…So he was rushed to hospital and then they discovered a huge tumour in his chest…He had 2 operations, but the surgeons could not remove it all and put him on a drip for a cancer treatment…Sorry I don’t know the right terminology, but this is what was happening…And I was sure he can survive.It is very confusing, as we don’t know what went wrong! Sorry, it’s very hard time for us right now…Thank you for your website anyway, it did made me feel understood and heard…
Thank you,
Kathrine
Dear Kathrine,
thank you for your question.
I am shocked and appalled by how you are describing how your Family member has been dealt with.
In the pictures that you’ve sent he looks far too young and healthy to be left to die and just because he “only” has 25% of his lungs functional is no reason to “put him to sleep” and let him die, without looking whether the right decisions have been made and also without your Family member being involved in the decision making process.
On the pictures your Family member looks like he would be quite capable in getting involved in the decision making process about his own end of life at such a young age. The unfortunate reality however is that the Intensive Care team doesn’t really want to talk about the issues of death to the Patient. Even for the Intensive Care team it feels hard, difficult and awkward to speak to a Patient about their death, so the easy way out is to “just put him to sleep”.
Even though the Intensive Care team is dealing with death and end of life situations frequently, doesn’t mean that they are good at talking about it and it certainly doesn’t mean that they are not willing to cut corners in order to drive their agenda forward.
The questions you need to ask are
- Have there been family discussions taking place before the actual decision was made “to put him to sleep”? If there haven’t been any Family discussions, the Intensive Care team is probably in breach of policies and legislations, let alone not respecting basic human rights
- Did your Family member know what was happening? Has any of your Family or the Patient himself been involved in any decision making about whether they want to live or die?
Recommended resources:
Having only 25% of lung capacity working is certainly not a good starting point, however that doesn’t necessarily mean that your Family member needs to be put to sleep straight away.
Often, what happens is that the Intensive Care team sees a quick death, as an “easy way out” of the dilemma and Families are being “sold” on the idea that death is in “the best interest” of a critically ill Patient, whereas in reality death is “the best interest” for the Intensive Care team, because they have many competing interests such as
- Wanting to have an empty bed in Intensive Care for another admission
- The perceived non- financial viability of your Family member’s Intensive Care stay
- Wanting to free up staff for the next admission
- Research interests. Your Family member may not fall into a research category and the Intensive Care team has a bigger interest in treating other Patients that fall into a research category and therefore attract 6, 7 or 8 figure funding
In the meantime read the following articles that shed more light on the decision making process around end of life and/or withdrawal or limitation of treatment.
Other recommended resources:
Also read our advice regarding Family meetings with the Intensive Care team
Also check out our “blog” and the “Your questions answered” section for more tips, strategies and for more questions answered.
But if you can please specify whether your Family member is dead already or not, I can certainly point you in the right direction about the options!
Thank you& Kind Regards
Your Friend!
Patrik Hutzel
How can you further leverage your level of power, influence and control whilst your loved one is critically ill in Intensive Care and how can you be in control of the situation?
You’ll get to that all important feeling of power, control and influence when you download your FREE “INSTANT IMPACT” report NOW by entering your email below! In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to get real power and real control, PERACE OF MIND and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE ‘INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is dying in Intensive Care! Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below!
In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care!
In your FREE reports you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 “killer” tips& strategies helping you to get on the right path to PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care(it’s not what you think)
Thank you for tuning into this week’s “your questions answered” and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also check out our Products section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 consulting!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!
Sincerely, your Friend
Patrik Hutzel
Related Articles