Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM, where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question last week was
How long does someone stay in Intensive Care when having a lung transplant?
You can check out the answer to last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer the next question from Belinda
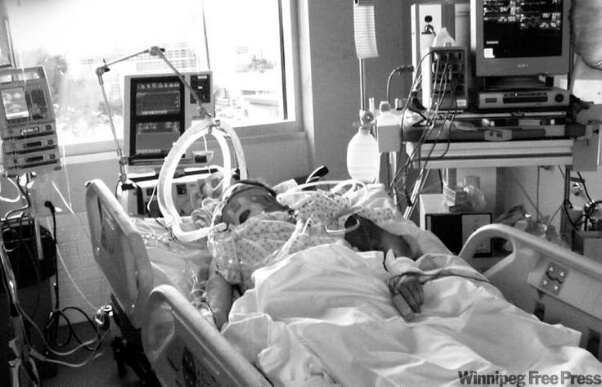
My 84 year old Dad has been in ICU for three months! He’s ventilated with a tracheostomy, the doctors want to let him die and turn off the ventilator! We want to take him home instead, what are our options? (PART 4)
You can also check out PART1, PART 2 and PART 3 of this series by clicking on the links.
This series of questions are excerpts from a 1:1 phone/Skype counselling session and a series of email counselling and consulting
Hi Patrik,
after much debate unfortunately they won’t allow us to take him home. They say that there are no services in our area who could make this happen for Dad.
His oxygen levels drop with each little movement.
My Dad’s access for dialysis was clotted and they did us not allow to open it, they forced us to put in a permanent catheter that I’m still upset about that they decided for me.
I think they wanted to bug us to move Dad to LTAC(=long-term acute care).
But my Dad aspirated tube food while he got turned and he got fever again and he’s back on antibiotics.
His blood pressure is low and his white blood count is going up.
They are waiting that God forbid the catheter won’t work for dialysis and…
The want their room available…
We are hanging in there…
Many thanks for all of your help and advice!
Belinda
Hi Belinda,
I’m sorry to hear that things are not moving forward.
It sounds like things are getting worse if anything.
Surely if your father is de-saturating(drop in oxygen levels) he can’t be ready to go to LTAC. I’m also not certain how the LTAC would cope with the Dialysis aspect as well as with your father’s oxygen levels and blood pressure dropping.
Especially with low blood pressure, your father would most likely be on Inotropes or vasopressors and those medications can only be given in Intensive Care.
I still don’t quite get how they can make certain important decisions without your consent.
They can’t just put a new line like a permanent catheter in without your or your fathers consent.
Nothing happens in Intensive Care without Patient or family consent unless it’s a life threatening emergency. Putting in a new catheter for Dialysis requires written consent from you or your Dad, there are no two ways about it.
Again, they are most likely breaching their own policies and you need to call them out on it.
Surely they want to empty their precious and “in-demand” ICU bed by either sending your Dad to an LTAC facility or they may wait until he’s so weak that he may die.
Unfortunately it is what’s happening in most Intensive Care Units that if a critically ill Patient is exceeding their desired length of stay that the Intensive Care team is trying to “push people out”.
And that can be by trying to withdraw treatment and let your father die or it can be by trying to send your father to LTAC.
One way or another you need to stay strong and do what you believe is the right thing to do, but you really need to call them out on their BS(excuse my language) by not asking you for written consent.
It also sounds to me like despite your father having setbacks like aspiration, white cell count going up, infection, IV(=intravenous) antibiotics and low blood pressure that he’s hanging in there. That’s a good sign.
But it’s certainly disappointing that they “won’t allow you” to take him home.
I know it doesn’t help you when I say that with my service INTENSIVE CARE AT HOME your Dad could go home… Unfortunately I can’t help you with INTENSIVE CARE AT HOME in your area.
But let’s focus on more realistic solutions in your situation. Have you listened to the interview from Charles Atkinson here?
He’s really giving great insights of what’s doable in challenging situations, even when ventilator dependent. Charlie is a remarkable man who managed to discharge himself home on a ventilator with tracheostomy by being extremely resilient and also by being forward looking!
The next thing that I would strongly recommend is Physiotherapy. Has your Dad been receiving Physiotherapy?
Arm and leg movement, chest Physio, sitting out of bed etc…
Yes, you might say he’s too weak to have Physio, however every Patient in ICU should be receiving Physiotherapy irrespective of their current condition. If he’s not getting the Physio he’s not having the stimulation he needs.
Also, have you thought about or considered to have him moved to another Hospital/ Intensive Care Unit?
One way or another you need to change your approach with the Intensive Care team in order to get what you want.
You really need to start managing the Intensive Care team before it’s too late.
At the moment they are not giving you any options and they are not giving you choice to have your Dad looked after on your terms!
Your current approach still isn’t working.
One strategy that’s working for most of my clients is to really become “difficult and demanding” when dealing with the Intensive Care team, especially when the situation has become has difficult and challenging as yours.
Related article/video:
The reason this strategy is working is simply that Intensive Care teams are not used to being challenged by families.
I think you haven’t quite stepped into your own power as yet and I think to a degree you are still held back by your believes of being inferior to the Intensive Care team or you might even feel intimidated by the Intensive Care team.
Recommended:
Once you step up to the level where you start to pro-actively “manage” the Intensive Care team instead of them “managing” you that’s usually when the dynamics start to change.
The reasons the dynamics are changing when you start to pro-actively manage the Intensive Care team so that they don’t manage you is that 99% of the families of critically ill Patients in Intensive Care make no informed decisions, have no peace of mind, no control, no power and no influence and they certainly don’t try and “manage” the Intensive Care team.
That’s usually beyond their beliefs that this is even a possibility because they tend to be so intimidated by the “perceived power” and the “perceived authority” of the Intensive Care team that they usually don’t have the guts to even try and change the dynamics of the relationship.
Given that your Dad has been in ICU for now over three months and the situation is getting more and more complicated you now almost have nothing to lose but to try and exert your power and authority on to the Intensive Care team.
Given that you have clarity about what you want for you and your Dad, you now need be very firmly standing your ground and just by you educating yourself about the dynamics in Intensive Care you can find a way out of the dilemma.
The worst thing that can happen to you and your Dad is that he may be dying in ICU and you haven’t been heard.
It will leave you full of bitterness and resentment towards the whole situation.
I know you are not giving in, but I believe your approach towards the Intensive Care team has almost been too soft!
“Hanging in there” might not be enough at this stage and I can only imagine how tired and exhausted you may feel after three months of watching your father suffer in Intensive Care!
Therefore, you may want to take some time out for a few days if you can in order to get some rest before you make another attempt getting care and treatment on your terms.
The dynamics often change when you start changing your communications style and it often changes when you are clear and precise in your communication.
This includes speaking to the Intensive Care team in non-ambiguous terms and making your expectations very clear.
This includes but is not limited to letting the Intensive Care team know that you want their “withdrawal of treatment” policy or their “DNR”(Do not resuscitate) policy by a certain time and date. I.e. “Tomorrow by 3pm”.
Just by doing that they all of a sudden realise that you are serious about your attempts in getting care and treatment on your terms.
You’d be surprised what happens if you draw a line in the sand and stick with it. This is crucial in getting what you want.
I do believe by what you are describing that the Intensive Care team has heard your message loud and clearly enough to warrant for them to change their approach.
That’s why it’s so important that you change your communication style and become more “difficult and demanding”!
Kind Regards
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!