Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Why Is It Crucial to Have Access to My Mom’s Medical Records in ICU & Track Her Progress?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients, Abby as part of my 1:1 consulting and advocacy service! Abby’s mom is critically ill in the ICU and she is asking if the ICU doctor can withdraw their mom’s treatment without their consent.
Can the Doctor Withdraw My Mom’s Treatment in ICU Even Without Our Consent? Help!
Abby: Hi Patrik! I just want to update you and ask you about my mom in ICU?
Patrik: Sure. Where would you like to start, Abby?
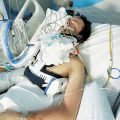
Abby: Yes. What I want to know is if somebody is being intubated, generally, how long with an acute respiratory injury does somebody remain on a ventilator, generally, if it’s really working out versus somebody that may be passing away?
Patrik: Yeah. It really depends. When you say acute respiratory injury, can you specify that?
Abby: Acute respiratory distress syndrome.
Patrik: Oh, ARDS (acute respiratory distress syndrome). Okay. I’ve seen days to many weeks.
Abby: So days to many weeks. So it’s really a long-time thing really. I’m just asking because I’ve got more information I got from them today and I want to make sure it’s being done right because I know they have a business to run in ICU and I understand that. I just want you to know it’s my mom. So you said days to many weeks, what if they have kidney failure with it and dialysis?
Patrik: possibly,
Abby: What?
Patrik: It possibly complicates things.
RECOMMENDED:
Abby: Okay. Could you explain, please?
Patrik: Yeah. So if someone has kidney dialysis, they have a catheter in. That catheter could be in the shoulder, in the jugular vein, or in the groin.
Abby: Okay.
Patrik: You know where it is?
Abby: No. But they can be able to tell you when you call, I’m going to be paying for more.
Patrik: So, for example, if it sits in the groin, your mom wouldn’t be able to sit up, because if your mom is on dialysis and she has the dialysis catheter in the groin and they sit her up, that would kink the catheter and the dialysis wouldn’t work, right? And that would be complicated. If she can’t sit up, more importantly, very difficult to be on a ventilator if you can’t sit up.
Abby: Okay. So what I’m hearing you, I got a thing from the oncology person and the oncology person said that a couple of days ago that this person with multiple myeloma shouldn’t have long-term dialysis but could try it temporarily. How long is reasonable with kidneys if they’re going to be viable versus not viable?
Patrik: If you look at the research, most patients in ICU that receive kidney dialysis are dialysis free after ICU stay. There are some-
Abby: How many days does it take usually to get off?
Patrik: I have seen patients in ICU on dialysis for weeks leaving intensive care without needing dialysis ever again. It’s really difficult to… It’s very hard to predict ICU outcomes, it’s almost a day-by-day thing. How many days has your mom been in ICU now?
Abby: She’s been in there for five.
Patrik: And basically, she’s got an ARDS picture. She’s on dialysis. She’s intubated.
Abby: They said her lungs were clearing up, and then my dad got a report today describing about do not resuscitate. Then, they’re saying they may pull the plug in three or four days if there’s no improvement. They said she wasn’t responding when they unsedated her. That’s what they told me and my dad this morning. I asked him this afternoon, that’s what they told him when he went down there. That they were going to do it in three or four days if there was no response. I wonder if she even has brain activity. I don’t. And my dad got the thing that you could only test if they respond. That she could be brain-dead and she is not living anymore.
Patrik: Are you concerned that she’s potentially got brain damage?
Abby: I don’t know what she has. That’s what’s frustrating me because they’re asking to withdraw… They once told my dad not to agree to a do-not-resuscitate. They also said in three or four days they were going to withdraw life support completely if there was no improvement, and that they concurred with several doctors.
Patrik: Which state are you in?
Abby: Highland.
Patrik: Highland State. Look, very unlikely that they can withdraw treatment without your consent assuming you or your dad are the power of attorney and assuming you and your dad do not agree with that.
Abby: So they can’t do it unilaterally. That is something that I want to be, I want to… That’s something that my dad, I’ll let my dad know, he’s in the background. They cannot do it unilaterally and we have the right to make a decision.
Patrik: 100%. Did you ever speak to your mom about if a situation like this ever occurred, what she would want?
Abby: Yes, I did. And if she could recover in a… And it was just an acute illness, yes, but she did not want to be permanently in a vegetative state. She did not want to have a thing where none of her organs were working. She did not want those kinds of things. If it was something where recovery could happen, yes. It’s hard to say. It’s not like something that’s a terminal illness. This is an acute thing from sepsis. She had sepsis and influenza and pneumonia, and then she went downhill and her breathing and then she developed an acute respiratory distress syndrome.
Suggested Links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: Okay. So do you think that the respiratory distress syndrome is a result of the multiple myeloma? Is that what they’re suggesting?
Abby: No. I don’t. I think it’s because of the sepsis and illness.
Patrik: Yeah. Are the sepsis and illness a result of potentially chemotherapy?
Abby: Possibly.
Patrik: Is she neutropenic?
Abby: What do you mean by neutropenic? Can you describe what you-
Patrik: Yeah. So when someone is receiving chemotherapy, their immune system is being severely weakened most of the time.
Abby: Yeah.
Patrik: That can show up with a low white cell count or it can show up with having no neutrophils.
Abby: They’ve had to do blood platelets transfusions when she’s been in the hospital several times.
Patrik: Yeah. Do you know if your mom is in a negative pressure room?
Abby: What do you mean by that so I could understand what you’re trying to say? Thank you.
Patrik: I’m sorry. I’m just-
Abby: No. I don’t know. I’m speaking from somebody who’s autistic and there’s lingo and if I don’t know the language, it doesn’t help anybody.
Patrik: Yeah. No. No. No. I’m putting bread crumbs here and I know you need to follow. So when someone is neutropenic, it means their immune system is basically non-existent.
Abby: I think she’s had some immunity, but I think it’s probably weakened because she’s been in the hospital twice in the last month.
Patrik: Yeah. So the reason I’m asking if she’s in a negative pressure room and if she’s neutropenic, she would be in a negative pressure room. Hang on. No. No. No. Hang on. In a positive pressure room. In a positive pressure room so that no bacteria can get in from the outside, because she has no immune system whatsoever. I would think they would’ve told you if she’s in a positive pressure room. I would think they would’ve told you, if they haven’t told you, it’s unlikely that she’s neutropenic.
Abby: Yeah. I haven’t heard anything.
Patrik: Unlikely that she’s neutropenic. But her immune system… From what you’re describing, when was the last time she had chemotherapy?
Abby: Just before she went in the hospital. She went on a drug called POMALYST, multiple myeloma, and Dexamethasone.
Patrik: Dexamethasone.
Abby: Dexamethasone. Yeah. I’m having a hard time pronouncing it. It’s DEX, for multiple myeloma and it killed a lot of the cancer, but she hasn’t been with it since August.
Patrik: Okay. I’ll tell you what I’m seeing here, Abby. Your mom has chemotherapy a few days before she went into ICU.
Abby: Correct.
Patrik: I argue the chemotherapy has weakened her immune system so severely that she ended up with pneumonia/ARDS and she ended up in ICU. I’ve seen this many times.
Abby: Yeah.
Patrik: I think that’s what it sounds like to me.
Abby: Okay. It’s probable.
Patrik: How often does she have chemotherapy?
Abby: They were going to have her on for two weeks, and then two weeks off for POMALYST. They lowered it to one. I looked at her dosage on the medication and the doctor gave her the maximum dosage amount, a four-milligram POMALYST pill.
Patrik: POMALYST. I need to-
Abby: There’s other pills that she could have taken in POMALYST like one, two, and three that would’ve been lighter dosages and they gave her the four milligram one.
Patrik: I’ll just quickly Google POMALYST.
Abby: Correct.
Patrik: I haven’t heard of it or I know it on that different name. POMALYST. Hang on. POMALYST, Pomalyst or without…
Abby: And DEX, Dexa Sodium
Patrik: Are you sure it’s Dexa Sodium or Dexamethasone?
Abby: Yeah. It’s what I think it is.
Patrik: Dexamethasone. That’s a steroid.
Abby: Yeah.
Patrik: Yeah. POMALYST, I can see that now. POMALYST is a prescription taken along with medicine dexamethasone used to treat adults with multiple myeloma, who have previously received at least two medicines to treat multiple myeloma. Okay.
Abby: She had cancer for 20 years and has done reasonably well until recently.
Patrik: And with that cancer for 20 years, chemotherapy on and off?
Abby: Stem cell transplant. And then, she had chemotherapy 10 years later.
Patrik: Okay. So this is basically the first time where she doesn’t respond to treatment?
Abby: She did respond and killed the cancer, but that’s a whole another problems.
Patrik: Yeah. But the first time where I’m saying, yes, she did respond to treatment, but now she’s so immunocompromised she ends up in ICU with all sorts of life-threatening-
Suggested Links:
Abby: You’re right on the head. Yes.
Patrik: Okay. So what else is happening? Five days in ICU, is in an induced coma, still?
Abby: Yes.
Patrik: She’s on vasopressors or inotropes. Do you know what I mean by that?
Abby: She’s been on some machine to make sure that her blood pressure doesn’t go too low. And they said yesterday that if they took her off the machine for two minutes, her blood pressure would drop.
Patrik: Okay. Do you know whether they’re treating the drop in blood pressure?
Abby: I don’t know specifically, when you call, I’ll pay for it, to call and get more information.
Patrik: Okay. Because I tell you where a lot of your answers lie, a lot of your answers lie within what else is happening. We know of two forms of life support. One is mechanical ventilation the other form of life support is dialysis. Now if she has a low blood pressure and they’re treating it with medications such as inotropes or vasopressors to increase the blood pressure, that it would be a third form of life support.
Abby: Okay.
Patrik: Which would sort of make it even more difficult. It’s not to say that she can’t come out of it, but it would make the situation more complex.
Abby: Yes. Do you have any other questions?
Patrik: Yes, I do. So I’ve just looked at my notes when we first spoke on Friday, I believe.
Abby: Yes.
Patrik: You did mention she was in prone position?
Abby: Yes.
Patrik: Is she still in prone position?
Abby: No. And they said her lungs had cleared initially.
Patrik: Okay.
Abby: And then, I got information today that they said they unsedated her and she didn’t respond.
Patrik: Okay. Yeah. But that’s not unusual after five days of induced coma. You stop sedation and you don’t wake up . There’s nothing unusual in there. So-
Abby: Thank you.
Patrik: … that can take days. That can take days.
Abby: How long does it usually take to wake up if it’s going to work?
Patrik: Yeah. Do you know what she was on in terms of, do you know what she was on in terms of sedation?
Abby: No. I don’t. And you can find out when you call.
Patrik: Yeah. Do you want to do the following? And this is up to you, Abby. Do you want us to call them now and try and get someone on the phone and we can ask questions? What do you reckon?
Abby: I’d like you to talk with them separately. And then, I want to have a follow-up meeting.
Patrik: Okay. Sure.
Abby: I think having somebody on the line is kind of intimidating with it. I have her cancer doctor, I have her general doctor, and I can give you the ICU doctors in that hospital if you would like, where you could have questions asked.
Patrik: Okay. Yeah. Okay. Has there been, so obviously the prone position must have helped.
Abby: Yes.
Patrik: The prone position must have helped, otherwise they wouldn’t tell you… I mean this is really good sign. You’re telling me that they were proning her, they’re doing dialysis and-
Abby: They said the dialysis wasn’t working after one day.
Patrik: Oh. Why not?
Abby: They wouldn’t tell me. They haven’t told my dad anything. I’d like to know what’s happening as I said.
Patrik: Okay. Look, there could be a number of reasons why dialysis isn’t working. The filter might have clotted. They didn’t give her enough anticoagulation. There could be a number of reasons why dialysis didn’t work.
Abby: That’s where you come in. I’m just giving you background information.
Suggested Links:
Patrik: Right. Right. But do you know with the dialysis not working, is she producing urine? Do you know?
Abby: They didn’t tell my dad anything. Again, you would need to ask.
Patrik: For sure. For sure. Okay. Right. What else is happening that you think might be important?
Abby: I don’t know. You’ve given me some hindsight of what may have caused her to maybe go to ICU. That we do have the right to make decisions that they don’t have the right to make a decision here.
Patrik: 100%. 100%.
Abby: As I said, with your help, I think you could help us. I appreciate everything that you’ve done. I was very comfortable the first time and the questions you’ve asked have been very helpful.
Patrik: Right. No. Thank you. That’s good to know. So who is involved in your mom’s care? It would be the ICU team. Is the oncologist involved?
Abby: She went to the hospital to see her, but I don’t think she’s involved in her care right now. If you want to talk with the oncologist, you can, and if you want, you need that information I can give other doctors if you need more information.
RECOMMENDED:
Patrik: Look, the reason I’m asking is the oncologist involved, I’ll tell you why I think this is important. ICU strictly looks at your mom’s situation from an ICU perspective. They look at organ failure, they think the lungs are failing, the kidneys are failing, and maybe the heart is failing. I don’t have enough information to say that, whereas the oncologist probably has a longstanding relationship with your mom. Is that fair to say?
Abby: Yes. And so has her general doctor.
Patrik: Right. So they know your mom as a person.
Abby: Thank you.
Patrik: That the ICU-
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!