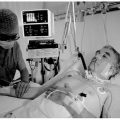
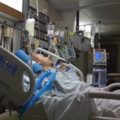
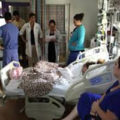
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Why is the ICU Team Saying That My 54-yr old Wife is Not a Candidate for ECMO?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Jay, as part of my 1:1 consulting and advocacy service! Jay’s wife is with a breathing tube and diagnosed with ARDS in ICU. Jay is asking why the ICU team is trying to limit their treatment for his critically ill wife in the ICU.
Why Does the ICU Team Try to Limit their Treatment for my Critically Ill Wife in the ICU?
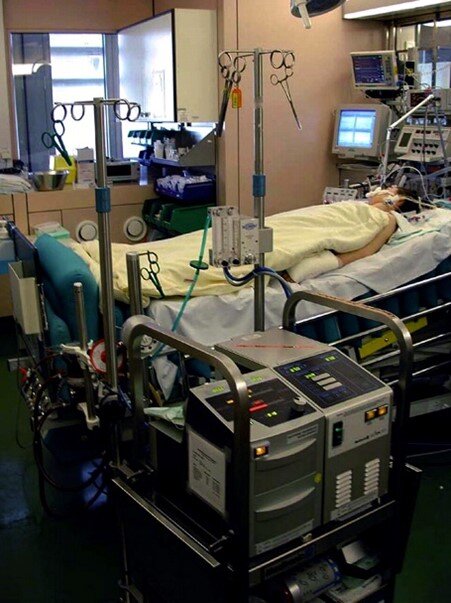
Dr. Tom: The current… I believe I’ve addressed these things.
Patrik: No you haven’t. No, you haven’t. Send us the policy around your decision making process, who you put on ECMO and who you don’t. What do you have to hide around that? What’s so difficult…
Dr. Tom: It’s not that algorithmic, sir. The decisions on who can go on ECMO is a clinical judgement, based on our ECMO physician reviewing the case. There are not hard and fast… I think I’ve said what I’d like to say on this topic.
Patrik: Yeah, what you’d like to say. Not what we need to know to make…
Dr. Tom: No, I said what I’m going to say. She is not a candidate because of her platelet count.
Patrik: Plenty of people going on ECMO with low platelet count. That’s fine. You say what you want to say. It would be good to have those discussions that you had with your team in writing. So we can see that you are making decisions that are in the best interest of Jay’s wife. We’re talking about a 54 year old. We’re talking about a 54 year old woman. Yeah.
Dr. Tom: I’m very aware of that. So I feel like you think I’m trying to keep something from you.
Patrik: Yeah, absolutely. Absolutely. Tell me how many ECMO beds do you have and how big is your ICU and many COVID patients do you have on with ARDS? Make those numbers transparent. What do you have to hide?
Dr. Tom: So I’m not the head of our ECMO program. And I don’t know that that is information that is public knowledge. Well
Patrik: Well, maybe… Well…
Dr. Tom: No matter what those numbers are… So I’m not trying to keep it secret. I just also don’t want to divulge information that I’m not able to. I’m certainly not the right person. Even if we were going to share that information, I’m not the right person to do that. No matter what the answers to those questions are, she is not a candidate for ECMO based on her medical picture, her clinical picture.
Jay: Patrik, perhaps that’s a conversation that we could get with the gentleman that made that decision.
RECOMMENDED:
Patrik: Sure. Absolutely. I think we should.
Dr. Tom: Okay. I will call that physician and make her aware that you would like to have a conversation with her.
Jay: Thank you for doing that, doctor.
Patrik: Thank you.
Jay: Know that we are on the same side, we are working diligently for my wife. If you can only… You can’t, you said, and I appreciate that, that you can’t imagine and you can’t. And so my heart is not to disrespect. It is not to bully. It isn’t. My heart is out of utter concern for the fact that I will probably lose… I have the potential to lose my wife soon. So you, I hope you can understand that.
Dr. Tom: I respect you.
Jay: Thanks.
Patrik: Thank you.
Jay: I hope you have a good afternoon. Thank you for getting in touch with that lady. What is her name?
Dr. Tom: Her name is Dr. Patricia. I’m going to let her know that you would like to have a conversation with her.
Jay: Thank you so much.
Patrik: Thank you so much. Thank you. I appreciate your time.
Dr. Tom: All right. Thank you.
Patrik: Thank you.
Jay: Thanks, bye. So, Patrik.
Patrik: Yeah?
Jay: So based on all of that information I think that… Let me just discuss, I guess, what… Okay, one, I think I’m going to have just kind of call my lawyers right away if that allows the timing and we can get her what I’m asking and it makes a change then that’s what I’m going to push for. Because it’s really… It’s worked for others and I’m going to put it in God’s hands but I’m going to make some calls.
Patrik: Yeah, I would do that if I was you. But I agree with her that it’s not a clear cut situation who will go on ECMO and there are many variables. I agree with her on that. But one of the variables is also how many ECMO beds are available, how many patients need ECMO. That’s one of the variables.
Jay: Sure, sure. That makes sense.
Suggested links:
Patrik: You know, but they still need to be transparent around that. And that’s where I think, yes, we can talk to this Dr. Patricia or whatever, however, they would need to… They would’ve discussed this and somebody would’ve taken notes. And if I was you, I would ask your lawyer to get access to those notes. You want to know why they’re saying what they’re saying.
Jay: Yes. Okay. Yes, that’s good. I’ve got that written down. So, that is what I’ll… Would you be available if she called for me to put you on the phone call?
Patrik: Yeah. Okay. All right. So what do you think she will do? She will get Dr. Patricia to call you, do you think that’s the next step?
Jay: I mean, at this point I have to think that she will. And if not, I can always call back and ask for her but I think I want a few moments to get ahold of the lawyers and say, “This is who we’ve hired. This is who we have on our side. What are we doing to move forward?” And see where that’s going and then we wait and then we also wait and pray for my wife at the same time. I realize there’s a lot of balls in the air. Any other suggestions from you?
Patrik: No, the suggestion at the moment is… So, at least she’s answered most of our questions. I mean, the only question she hasn’t really answered is around ECMO. I do understand it would be a number of doctors making that decision, I get that. It’s very rarely clear cut. But all other clinical questions she answered. I agree with her that your wife’s life is, for lack of a better term, it is hanging at a thread. It is definitely hanging at a thread. She’s on a 100% of FiO2 (fraction of inspired oxygen), the support on the ventilator is at the maximum. They can’t give her more support on a ventilation level, which is why they’re proning her. You might have heard me ask about the ABG, the arterial blood gas, you might have heard us talk about the pO2 of 55. That’s critically low. If it was to drop any further, she is at risk of going into cardiac arrest.
Jay: Okay.
Recommended:
Patrik: So…
Jay: Do you suggest that I go to the hospital? I mean, do you think it’s… I’ve been at the hospital most of the day.
Patrik: Yeah. I would suggest yes. I would suggest, yes. The question that you need to ask yourself is the risk for yourself with COVID.
Jay: Oh, they’ve been cleared. She’s been cleared. I…
Patrik: Oh, she’s been cleared. Oh, okay.
Jay: Yes, almost four weeks ago.
Patrik: I see. So she’s been cleared of COVID.
Jay: Yep.
Patrik: Okay. Great. Well then, I think…
Jay: I hadn’t been able to see her.
Patrik: Oh, when was the last time? When was the last…
Jay: I haven’t been able to see her for about 14 days since they found it.
Patrik: Oh, you haven’t seen her for 14 days.
Jay: When they intubated her. Well, and she got intubated 3 days ago, 4 days ago now, and I was able to go see her. So now I’ve been able to visit with, I mean… Visit. I mean, I’ve been able to see her.
Patrik: Sure. Look, I would spend time with her if I was you, it’s looking pretty grim at the moment, but I would spend time with her. Even if she does improve, I think she needs you now.
Jay: Okay. I mean, I have been. I just had a hard time going in there this morning, so… I’m going to go. I guess I’ll be on my way. Is there anything that I should know, anything that… I mean… I guess we can talk to the nurse. We were going to talk to the nurse about what would they allow. I’ll talk when I’m there. I’ll go. I’ll go there. And I’ll talk. And I’ll ask what’s allowed. Is it usual… I mean, do you know if they let, family members in? I mean, they have policies, but..
Patrik: Yeah, they have policies. I tell you what a lot of it depends on at the moment. A lot of it depends on how many COVID patients do they have. Some ICUs are more lenient than others. Just because your wife has been cleared of COVID, there might be the next COVID patient just next to her. I don’t know. I don’t know what their layout is.
Jay: Okay. So I’ll find out then. I’ll find out from the nurses.
Patrik: Find out from the nurses. The only last thing that I want to mention. I know you asked about lowering sedation. They can’t lower sedation at the moment. She wouldn’t be able to tolerate any of this without sedation.
Suggested links:
Jay: Okay, okay. I understand. I just didn’t know.
Patrik: No. That’s okay.
Jay: Okay. Well, I guess at this point, I’ll get in touch with you.
Patrik: Yeah, please get in touch.
Jay: And if Dr. Patricia calls, I will call you.
Patrik: Yes please do that. Please do that.
Jay: Okay. Thank you so much.
Patrik: Thank you so much.
Jay: For everything.
Patrik: Thank you so much.
Jay: Bye.
Patrik: Bye bye.

Jay: Thank you. Just a moment, I’ll merge us.
Patrik: Thank you.
Jay: Hello doctor, this is Jay. Thank you for calling me back.
Patrik: Hello?
Dr. Paulo: Hello?
Jay: Hello.
Dr. Paulo: Hi, Jay, this is Dr. Paulo. I’m not sure if you remember me but I was speaking to you about procurement a few weeks ago.
Jay: I remember, I think I remember talking with you on the phone, thank you.
Dr. Paulo: Yeah, so I am on an ECMO service from today onwards and I know Dr. Patricia and my colleagues saw Karla yesterday, and Dr. Marian had just started seeing Karla, and she asked me to reach out to you guys to see what questions you have for me.
Jay: Patrik, I know you have a couple of questions. Is ECMO something that can only be used when a patient is on a ventilator?
Dr. Paulo: Most of the time, yes.
Jay: But it doesn’t have to be?
Dr. Paulo: No, it’s not. As of now 99.999% of ECMO has been done on the patient while ventilated.
Jay: Okay.
Dr. Marian: Jay, I think I know where you are coming with this. We would never initiate ECMO on someone who isn’t intubated. It’s that people who are on ECMO and doing well can sometimes have the breathing tube taken out, but it would never be initiated before a ventilator.
Jay: Okay, that helps me, it does. When the decision was made, when she was intubated last week, was there a consult that afternoon when her… If I look back, I don’t have the information right here in front I’m in my car. When I look back on last week at her platelet count and she was in respiratory distress, what was discussed that day and was her platelet count enough that it could have been initiated?
Dr. Paulo: That’s a good question Jay. Let me just review her images, so we do have a certain criteria for what we call a failure of pro-ventilator therapy. Then after we initiate them and…
Dr. Paulo: Can you go back, there’s a couple of cases, I think they’ve been intubated. I think that was her call. Okay, I think one thing right now is that we were able to provide her enough oxygen and get the carbon dioxide out within a safe ventilator setting, so at that point of time she didn’t require an ECMO. Let me put a different way, at that point of time she does not fulfill the criteria of going on ECMO.
Recommended:
Jay: Can I ask? Again then tell me what is the requirement for a patient, I know doctor, when you read stuff you think, “Oh, that seems to be the requirement.” Can you give me specifics?
Dr.Paulo: Sure, sure, so we at our center and most of the centers follow particular criteria, those are known as CESAR criteria, specifically index for lung function or P/F ratio less than 80 for more than 6 hours, and P/F ratio less than 60 for more than 3 hours. The P/F ratio is the arterial partial pressure of oxygen (PaO2) divided by the fraction of inspired oxygen concentration (FiO2). I think that more than anything, most of the time things are, unless like yesterday something happened.
Dr. Paulo: Okay, so all of our provider are kind of educated about when is the time to call the ECMO team, is that they follow that criteria and guideline.
Jay: So as soon as her platelets started going down, would that then be an indicator and then before they got too low, in order to be able to do it, I guess I’m a little bit confused, and is that not something that you discuss? Is it only something you discuss amongst yourselves or is that something that you at least up as an option or because you decided it wasn’t option then it’s just no? I’m asking. I just really don’t know.
Dr. Paulo: So I’m not able to get Dr. Marian in, but let me put it a different way, unfortunately for her, her P/F ratio started going down at the same time her platelets started going down.
Jay: What issue? I don’t understand, I’m sorry. What issue at the same time as the platelet issue?
Dr. Paulo: The P/F ratio.
Jay: The P/F..
Dr. Paulo: I can offer you an explanation.
Jay: Thank you.
Dr.Paulo: The P/F range went up at the same time her platelets started going down.
Jay: Okay, and at that moment you felt that wouldn’t help her?
Recommended:
Dr. Paulo: Based on such a low platelet count, Marian prefer if you don’t put them on an ECMO, because what happened is that it’s an excellent subject, so we have to give them a blood thinner and putting patients with a low platelet count, we really believe that they can bleed in the brain.
Jay: Okay. Patrik, you have a little bit more insight, I mean.
Patrik: Yeah, just a few more questions. I mean, I understand your rationale with the platelet count, obviously the risk for bleeding, but by the same token, you put someone on heparin when someone goes on ECMO, so the risk for bleeding is there anyway. You’d be aiming for an APTT, sometimes 60 to 80, depending on your goals, and you have the risk for bleeding anyway. I mean, I’ve seen patients on ECMO with a brain bleed dying because the heparin is not hydrated accordingly and you’d be having the same risk with a low platelet count, so tell me what’s the difference?
Dr. Paulo: So the thing is, you brought up a good point and the thing of course we have decided is we will not be able to put anyone on ECMO when their platelet count is less than 100, 000, less than 75, 000.
RECOMMENDED:
Jay: Do you remember what day she fell below that?
Dr. Marian: Yes, so on the 20th, 4 days ago, the day after she went on the ventilator, when was on 70% oxygen, her platelets were 79. The day before, they were 88 and the day she got intubated, they were 95, so she was already, even the day after she got intubated and then the subsequent day really on the borderline and then only went down from there, unfortunately that was also when her oxygenation was declined as well. I’m not sure if they happened similarly, the time course.
Jay: Patrik, do you have any other questions?
Patrik: Yeah, so obviously you’ve made that decision, but I mean, who was involved in making that decision now? Surely it would’ve been a team of doctors that looked at that. It wouldn’t have just been one or two people looking at that. Or is it? Who was involved in making that decision? Is it just yourself or was it a team of ECMO specialist? Was it a team of ECMO specialist plus respiratory or pulmonologist? Who is involved in that decision making process?
Dr. Paulo: Yesterday, Dr. Patricia saw her, she’s a former ECMO director and I’m taking over from her service. I will be here for next one day.
Patrik: Right, so are you saying that you personally haven’t been involved in that decision making process because you weren’t on duty?
Dr. Paulo: Let me put it in differently, I just came on today and I evaluated her and she is still not a candidate for any form of extracorporeal life support.
Patrik: Okay, but what I’m hearing is that you personally weren’t involved in the decision making process, is that correct?
Dr. Marian: Yesterday.
Dr. Paulo: Yesterday?
Dr. Marian: Yes, yesterday were you involved in that?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!