Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Should I Trust the Rehab Facility in Taking Care of My Critically ill Sister After ICU?
You can check out last week’s question by clicking on the link here.
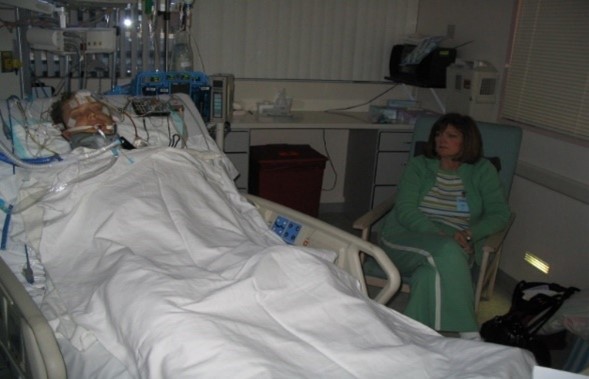
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Albert, as part of my 1:1 consulting and advocacy service! Albert’s sister is on a ventilator in the ICU and he is asking why they transferred his sister to the rehab facility and comes back to ICU in a worse condition.
Why Do they Transfer My Sister to the Rehab facility & Comes Back to ICU in a Worse Condition? Help!
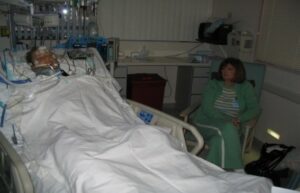
“You can also check out previous 1:1 consulting and advocacy sessions with me and Albert here.”
Val: See, that’s the game they’re playing though, because the good ones or the decent ones with the hospital and the doctors and things like that are not accepting. Or they’re playing the game of, “Oh, she’s on the waiting list.” Then they come up with the worst review, the worst … And then they’ll come up with one and say, “We found you one.” And then we say, “No. We’re not accepting that.” And then they’ll say, “Oh, you keep refusing. And if you keep refusing, we’ll go to court.”
Patrik: Yes, they might. But I don’t think they will be succeeding. And don’t get me wrong, a hospital going to court is also a last resort for them. It’s not that the hospital will drag you to court willy nilly. It’s a last resort for them. Just as a lawyer would be a last resort for you.
Val: Right.
Patrik: Okay? So they will try and resolve this amicably if they can. Right? And it’s not that if they don’t have her out by Wednesday that they will be going to court. It’s usually a process of escalation.
Val: Right. It’s a last resort.
Patrik: It’s a last resort. I guess-
Val: They got to have a good case too.
Patrik: That’s right. They have to have a good case. They are probably preparing for what they consider as a worst-case scenario. And so do you.
Val: From what she heard, from her condition, she sounds like an Intensive Care Unit (ICU) patient. Right?
Patrik: Absolutely.
Val: So, I don’t think they have a good case to say a person with an ICU condition should be going to a nursing home. I don’t think they’ll go to court.
Patrik: There’s no mandate for that. There’s no mandate for that.
Val: Yeah, the discharge policy, will we find it online?
Patrik: You may. You may. You can go onto the hospital’s website and you can see it possibly from there. Some hospitals have their policies publicly available online and some don’t.
Val: Mm-hmm.
Albert: We can ask them for it.
Patrik: You can ask them. You can ask them. But, if you do find it online, you can just hold it in their face and say, “Look, we’ve done our research. Here is what your policy says, and you are breaching your own policy.”
RECOMMENDED:
Albert: Yeah. And then another thing, that I want to tell you from the beginning after they sent her to the rehabilitation center, she seemed very abused seeing her body. You see her look so dark for a while, because they pushed to put her in some kind of lifting. It’s so hard for her. And then, it was so worse. And then, after that she got so sick. And then it started from them. One of the nurses, she told me, “I work for 18 years, I have never seen a pneumonia like this. How they send them here like this?” She told me that over the phone. And then she said, “Maybe the insurance.” I said, “No, I don’t think so.” And then I think at that time, maybe the insurance pushed them, because I changed it. And then later on I changed it, the standard. And then, because of that. And then you’ll be sorry when you see her, how she was bruised.
Patrik: I’m so sorry. I’m so sorry. Well, that is definitely another argument for you.
Albert: Yeah.
Patrik: That is definitely another argument. I mean, you can confidently say that, her going to a rehabilitation facility, she came back in a worse condition.
Albert: Yes. Yes. Five emergency room. After she left there, she went to four or five rehabilitation centers. After they send her here. They can keep her until she’s fine, because they send her early before she was stable. That’s what happened since then and she came back to them. Now, she came back to them. She had a kidney failure, heart failure, again and lung failure, mostly here.
Recommended:
Patrik: Yeah. Okay. I think you’ve got enough arguments here. You just got to watch them and-
Val: Yeah. You just got to watch them. And here is another tip. And I need to go in a couple of minutes. Here is another tip.
Albert: Yeah.
Patrik: So let’s just say they ask you for a meeting. Okay? Let’s just say they ask you for a meeting. My recommendation is do ask for a written agenda of the meeting first, and only after you’ve seen a written agenda of the meeting, will you decide whether you’ll be joining or not?
Val: Mm-hmm.
Patrik: Because they’re very good. They’re very good at telling families, “Oh, we got to have a meeting at three o’clock this afternoon.”
Albert: Yes. Yes. Yes.
Patrik: Don’t play that game. Don’t play that game.
Val: Okay.
Patrik: Unless it’s an emergency. Unless it’s an emergency, of course. But, if it’s not an emergency, if your sister’s condition has not changed and they ask you for a, “urgent family meeting”, get a written agenda first.
Val: What is it? Origin of agenda or original agenda?
Patrik: No. No. A written. A written, in writing.
Val: Oh, written. Written agenda.
Patrik: Sorry. Yeah. In writing.
Val: Oh. Okay. Okay. A written agenda. Gotcha. Gotcha.
Patrik: Yeah.
Val: One quick question again. I asked-
Patrik: Please.
Suggested Links:
Val: About the tracheostomy, the leak. I keep asking about that.
Patrik: It worries me. It worries me. There should not be a leak. There should not be a leak.
Val: So, we should press on it so they can change it to the right size? Right?
Patrik: That’s what I’m saying. It’s either not the right size, or there is something with her anatomy, which is why I asked earlier, does she have a short neck? Does she have a long neck?
Val: The only thing they said was from her first tracheostomy, her.. what do you call it? Expanded. So, they have to get a bigger balloon.
Patrik: Yeah. Yeah.
Val: That’s what they said. So-
Patrik: There should not be a leak. What size, do you know what size tracheostomy tube she has?
Val: I think the last, do they give her a seven?
Albert: Yeah. They give her seven first and then they change it, because it was leaking again. They change it and they give her eight. So, what happened was when I called some places they told us to go. And then I spoke to them, one of the respiratory therapists he told me, “We did weaning here very well. We have working for a long time. And the reason they didn’t change it for her, because we have 10 and nine, and then they supposed to do that for her?“ She told me.
Patrik: What’s your sister’s physique? Is she tall? Is she slim? Tell me a little bit more.
Val: She’s slim. She’s tall. She’s about, let’s say, around 5′ 9″. Five ten or so.
Patrik: Okay. Just with that alone, I would say she will need a size eight. So, I’m not surprised that the seven was leaking. But if an eight is still leaking, I don’t think she’s big enough for a nine. But then they could try, for example, there’s also 8.5.
Val: Can you hear a leak on the tracheostomy?
Patrik: Yes. I tell you how you can hear it. It’s not so much that you can hear it. If there’s a leak, I could see it on the ventilator, because let’s just say someone is getting 500 mls per breath and there’s a leak. The volume would only be 300.
Val: Mm-hmm.
Albert:Yeah.
Val: Gotcha. Gotcha. So, it’s more from the machine, not from-
Patrik: Yes. But, that means she’s under ventilated, potentially.
Val: Right. Right. Right. So that could cause a fatigue as well,
Patrik: Could cause fatigue. Could cause under ventilation, could delay the weaning process.
Val: Right. Okay. Okay. Okay. All right. Okay. Thank you so much, Patrik.
Patrik: It’s a pleasure. It’s a pleasure. Look, if you can forward me the information, then we can take the next steps.
Albert: Yeah.
Patrik: Okay?
Albert: tomorrow?
Patrik: Yeah. Over the weekend.
Albert: Yeah.
Patrik: That’s fine.
Albert: Over the weekend we will do it.
Patrik: Yeah. It’s fine. It’s fine.
Val: Excellent.
RECOMMENDED:
Patrik: Okay. I got to go.
Val: Thank you Patrik.
Patrik: It’s a pleasure. It’s a pleasure. Nice to meet you all. Nice to meet you all. Take care.
Val: Thank you for what you do. Yeah.
Patrik: Thank you. Thank you. Bye-Bye. Bye.
Albert: Bye Patrik.
The 1:1 consulting session will continue in next week’s episode
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!