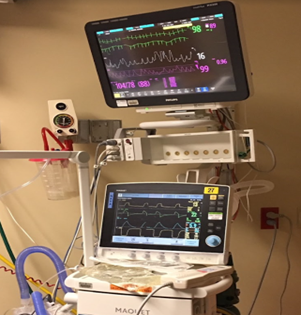
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Is it Safe to Transfer My Sister to a Nursing Facility Directly from ICU? Help!
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Albert, as part of my 1:1 consulting and advocacy service! Albert’s sister has a tracheostomy and is critically ill in the ICU. Albert is asking why can’t they help her to recover.
My Sister is Critically Ill in ICU with Tracheostomy & Why Can’t they Help Her to Recover?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Albert here.”
Patrik: Yeah. So, if she needs surgery, let’s just make up a scenario, let’s just say she needs surgery and she can’t give consent herself. Are you the one giving consent?
Albert: Yes. Yeah.
Patrik: Okay.
Val: Her husband.
Patrik: Okay. Her husband is giving the consent.
Val: Her husband is there too. So, they are the proxy, right?
Patrik: Okay. They’re the proxy.
Val: Yeah, yeah.
Patrik: And you have a document to confirm that?
Albert: From the hospital? Yes.
RECOMMENDED:
Patrik: What about from your sister herself?
Albert: Yeah. I just let her sign last time, and then went to the bank and then did the power of attorney.
Patrik: Okay.
Albert: Because at the time she can’t do it. So, I don’t know what to do, so if you-
Patrik: Do you have a written document from an attorney, that you are the power of attorney?
Albert: No, we don’t have it. So, can we do that?
Patrik: Urgently, urgently. And look, I am not a lawyer, I’m a clinician. However, I’ve worked with enough clients all over the world. It doesn’t matter where it is, America, Canada, here in Australia, UK, the power of attorney documented is critical. And I’ll tell you why. And the person that can do that for you is a family lawyer.
Albert: Okay.
Patrik: Right? I’ll tell you why this is so important, especially they’ve now given you the warning that they might threaten you with taking away your power of attorney. And that is definitely a warning sign that they might be doing that, and you need to secure the power of attorney, on a legal level.
Albert: Right. Okay.
Patrik: So why is this important? So, it might come to a point where you say, “No, no, I want her here.” And the ICU is saying, “No, no, we want her there.” And if a resolution can’t be found, one way for the hospital to take control is trying to get power of attorney over your sister, which is madness. I’ve seen it.
Albert: Yeah.
Val: Mm-hmm.
Patrik: And if that happens, you have no right whatsoever. You can just watch things from the sidelines. It’s terrible.
Albert: Mm-hmm, yeah.
Patrik: So, if you can sort that out. And the reason they will try and get that is they will say to you, “Well, you don’t act in the best interest of your sister. We are the ones acting in the best interest of your sister.” And a court might say, “Yep, we think that’s the case. You are not acting in the best … ”
Albert: Yeah.
Patrik: I’ve seen it.
Val: So that also applies for a husband, as well?
Patrik: Anyone. Children, spouses, anything. Anything.
Val: But in this case though, in her condition we’re talking about, and they’re trying to send her to a senior’s home or some kind of rehab. So the reason they brought that up is because they tried to send her to a senior’s home where there’s no doctors and nurses. And we said, “No, she cannot go there.” That’s when they brought up the court situation. So, do they have a base to say, from her condition?
Suggested Links:
- Why Does my Brother Keep Getting Infections in ICU& How to Prevent it! Quick Tip for Families in ICU
Patrik: With what you’ve shared with me, I don’t think they have a base. But again, I am not a lawyer.
Val: Right.
Patrik: I am not a lawyer. I do not know the laws around guardianship. They’re fairly similar in English-speaking countries, from what I’ve seen.
Val: Yeah.
Patrik: But it’s not my area of expertise. What I can 100% tell you is, if the hospital gets guardianship or power of attorney, your rights have gone out of the window for good.
Albert: Yes.
Val: So, I guess the main question is, number 1, is to get that power of attorney? But that power of attorney, it doesn’t guarantee you from court taking away your right, right?
Patrik: No, that should pretty much … They can then challenge it, but it’s much less likely that they will get it. What I have seen is, if the power of attorney situation is not clear, that’s when they often do a power grab.
Val: Mm-hmm.
Patrik: If the power of attorney situation is crystal clear, Albert, her sister, her husband, whoever, is the power of attorney guardian, it is very difficult for them to get that. But if the power of attorney situation is in limbo, that’s when I’ve seen the power grab, from hospitals.
Val: So, for example, with Albert, that’s her sister, and her husband, once they have that in their hands, do they notify the hospital? Do they submit that? Or what do they do?
Patrik: No, you only need to present that to the hospital, really, if it’s ever coming into question.
Val: You go to court.
Patrik: That’s right, if you’re going to court or-
Val: The reason I’m bringing that up is because one of our fears is, you talked about discharge policy, is that can they one day, without our consent or her husband’s and my aunt’s consent, just take her and put her to …
Patrik: If they have power of attorney, yes. If they don’t have power of attorney, it’ll be very, very difficult for them.
Val: I see.
Lorie: One of the things that we are worried about is, without us being present as well, to try and communicate with her, that they would get translator to come and ask if she wants to leave. Or if-
Val: And many of the family doctor’s meetings, not many, but a few times, they have asked us and suggested … Because she’s up and down, right? When she has surgery, sometimes she’s down. So, they asked us, “If something was to happen, do you want nature to take its course?” And we made it very clear that, no, absolutely not, for many different reasons. And they just see the physical side, but there’s also the spiritual, there’s just so many different things.
Patrik: Absolutely.
Val: And belief. And they were just disregarding it. They kept pushing us on that direction very much. Not once, but many times. And we made it very clear to them and then at the end they said, pretty much saying, “You know what? We’re going to ask her ourselves.” kind of thing. “We’re going to get a translator and ask her themselves.” And I said, “You can ask her, but make sure we’re there when you ask her because we don’t know what you’re saying to her.” And apparently, they went behind our back and talked to her.
Patrik: What was the outcome of that conversation with her?
Recommended:
- What are My Mom’s Chances of Survival After Double Heart Attack, Failed Extubation & Kidney Failure?
Val: I don’t think they got anything for her because she’s a very family-oriented person. She believes in her family; she wants her family to take care of her things. So, they didn’t get much. But when we found out that … She didn’t really respond to them, she was pretty much saying, “Talk to my family.” And it’s very, very frightening because there’s COVID. The visitation time is only certain amounts and we’re not there to fight or anything, we just want her to get better, get her treatment and get out. It’s just scary, that’s what I’m trying to say.
Patrik: Absolutely. So, two questions there. (A), can you visit?
Val: Yes. Now we can.
Patrik: Now you can. Unlimited?
Val: No. Certain hours. I believe it’s from 3:00 pm to 8:00 pm. So how many hours is that?
Patrik: Okay, okay. So you can-
Val: About five hours now.
Patrik: Right, okay. At least you can visit. (B), as part of you having access to the medical records, Albert, have you found any documentation in there where the doctors say, oh, they’ve spoken to her and she doesn’t want to be resuscitated, for example? Is that part of what’s documented?
Albert: No, no. It’s not documented, I didn’t see anything. They just do it behind of us. They just call the people translating. One of the doctors, he told me, “I cannot help her. Personally, I cannot help her.” I said, “You’re still helping her, why you say that?” He said, “I’m telling you, I’m telling you.” And then one of the church ladies, they send her, and she came and she said, “We have to have a meeting because they don’t want to give her anything and they want her to die.
Patrik: Yep.
Val: So I just want to go back to that story. So, when she did her PleurX tube, when she did the surgery, everything went well. And then an hour later, her blood pressure dropped. When her blood pressure dropped, all of a sudden, they called a meeting. And again, that topic came basically to, if something happened not to resuscitate and things like that. And, my two aunts there made it very clear that we don’t accept that. But they kept pushing, and the doctors are saying things like, “We can’t help her. Something can happen the next day.” or just nothing great anyways. And then. I think it was a few days later, like she said, a chaplain or a priest or somebody came, without our request. They approached and they wanted to talk to us. And the whole situation is just frightening, to be honest.
Patrik: You have now seen how they really are. And unfortunately, that is how they really are.
Val: My goodness.
Albert: They even told us, “Why don’t you just let her tell goodbye, and then-”
Val: Yes, those were the words.
Patrik: Look, why do you think I’m doing what I’m doing? I’ve been part of the system. I’ve been part of the system; I’ve seen it all. I know how they are. I was part of it, at some point. I know how they are. If they were doing all the right things, my business should not exist.
Albert: Yeah. Not only the business, you are helping people. Trust me.
Patrik: Yeah, yeah. No, I know.
Albert: That’s a very good job that you do.
RECOMMENDED:
Patrik: Yeah, I’ve seen it, I’ve been part of it. I know what they’re like. It’s frightening and it’s terrifying. And that’s why I’m saying, from their perspective, they’re so busy. They have people queuing up for the ICU bed. Their problem will be solved if your aunt or your sister has gone, whether she’s dying or whether she’s going to another place. They just want to have the problem solved, unfortunately.
Val: For them, she’s just another patient, yeah.
Patrik: Another number, another number. That’s it.
Val: Yeah.
Patrik: They are so desensitized. If someone dies, well, it’s just another number for them, unfortunately.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!