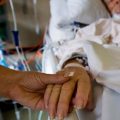
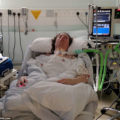
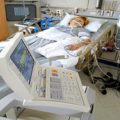
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
How Can My Sister Wean Off the Ventilator in ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Albert, as part of my 1:1 consulting and advocacy service! Albert’s sister has a tracheostomy and is critically ill in the ICU. Albert is asking if he should trust the Rehab facility in taking care of his sister after ICU.
Should I Trust the Rehab Facility in Taking Care of My Critically ill Sister After ICU?
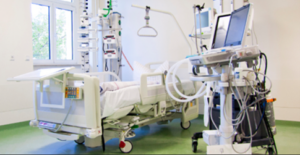
“You can also check out previous 1:1 consulting and advocacy sessions with me and Albert here.”
Albert: Yes.
Patrik: I am very pleased to hear that you haven’t heard from the insurance. If the insurance contacted you, I would be worried. But if insurance hasn’t contacted you, it’s just the hospital pushing, that’s all.
Val: Yeah, it’s just the hospital politics side. You came up with the letter, that’s what I was going to ask you. So we’ve told you what the medical team, the doctors, what they’ve been saying to us. So for example, let’s say you draw us a letter, where would we send it? To the president of the hospital?
Patrik: Yeah, something like that, something like that.
Val: So, would that make a difference? Are they completely different from the medical team kind of thing?
Patrik: Look, my experience is, if you send it to the ICU, they may take it into consideration. But again, they are clinicians, whereas the hospital CEO or the hospital president, whatever their title is, they’re business people. They want to have happy customers.
Val: Mm-hmm. Okay, I see. So, they might have a completely different view from-
Patrik: They often do. Look, I have been a hospital administrator myself, and as a hospital administrator, you can’t ignore complaints from a family.
RECOMMENDED:
Val: Right. Well, there’s a follow up question with that though. Drawing up a letter, something like that, like I said, she’s with them most of the time. So, is there a setback?
Patrik: Yeah. Are you worried about retaliation?
Val: Right.
Patrik: Yeah. Look, can that happen? Yes, it can happen. I do believe the worst thing for you is not anticipating what could happen. And I do believe that anticipating that she could go to a rehab facility in this condition, anticipating that they could potentially kick her out, in my mind, is worse than the fear of retaliation.
Val: Right.
Patrik: Can retaliation happen? Yes, it can. But it doesn’t happen as often as you think it does. If I have found one thing, that if you put your foot down, yes, they won’t like it. Don’t get me wrong, they won’t like it. But if you are consistent in your approach, eventually you will get respect from them. Eventually. It doesn’t happen straight away.
Val: Right. With that, I’m just going to jump to the rehab.
Patrik: Carry on, carry on.
Val: I’m just going to ask one more question about rehabs. So, there was a moment when she was doing much better, and we wanted her to go to rehab and of course and things like that. But there was a lot of trouble because most of these … Some of these rehabs also do have doctors and things like that, it’s kind of like a hospital. But for some reason, I don’t know, because of the insurance, there was a lot of rejection. They wouldn’t accept. Or what they would say is, “Oh, she’s on a waiting list.” or “There’s a long waiting list. She’s going to have to wait.” Why would that happen?
Patrik: A waiting list for what?
Albert: For rehabilitation.
Patrik: Oh look, why would that happen? Because there are no beds.
Val: But no. And then we call in and they say, “oh, there’s a whole bunch of beds.”
Patrik: Okay. That’s strange.
Val: Yeah. We’re just completely confused why a whole bunch of rehabs for some reason either say, “Oh, there’s a long waiting list,” or “We won’t accept.” And we’re just wondering is it because of what the doctors are putting in the notes that’s making her not accept them? I have no idea.
Suggested Links:
Patrik: Yeah. Look, it probably depends a little bit on the skill level of a rehab, but their skill levels are not great to begin with, from my experience. Look, if anything ICUs want to send patients out, most of the time they are finding beds. Most of the time. So, I’m a little bit surprised to hear that. My experience is that it often happens too quickly. But there could be some rehabs at the moment. There could be some changes in the environment. What I mean by that is with COVID, I would imagine the rehab facilities are full.
Albert: But what happened, Patrik, what happened was in one of the rehabilitation centers … And they told them to the case manager, she is on the waiting list for six months, and now for three months, for two months. And then, when I called that rehabilitation center, the nurse told me, “Oh, we have a bed. We have a bed.” And when I call in the morning, the case manager says, “We don’t have a bed,” but I know they have a bed, but they don’t want to accept her there.
Patrik: How long ago was that?
Albert: It was last week.
Patrik: Okay. Well, I’m not surprised with what you’ve shared with me. I do believe she’s too unwell.
Albert: Yeah.
Patrik: She’s too unwell.
Albert: Yeah.
Lorie: So, basically rehab is not even what they’re offering right now. What they’re offering is some type of nursing home, is what they want to send her to.
Patrik: Have you heard of the term LTAC?
Albert: Yeah.
Lorie: Yeah.
Patrik: Right. So LTAC is where many patients from ICU go with a trach and a ventilator. Now, LTAC stands for Long Term Acute Care. It’s being sold often as a “step-down ICU”. It’s never been advertised as a nursing home. Now, from my experience, it’s the better version of a nursing home, but it’s pretty bad. So, if you’re telling me they’re only offering her a nursing home, that’s even worse. That is even worse.
And given that to me, by the sounds of things, she’s on the right path. That’s what it sounds like to me. Yes, she’s got some challenges. Nothing unusual, nothing that I haven’t seen before with someone being in ICU long term. These are the challenges that a long-term ICU patient is going through, struggling, weaning off the ventilator, not sleeping at night. She’s swollen, she’s got flu. Nothing that I haven’t seen before. It just takes time and it takes patience and it takes effort. And nothing in a situation like that happens quick enough for an ICU. I get all of that. But, on the positives, I do believe just by what you’ve shared with me, I think she’s on the right track. And, if they were to interrupt her slow recovery and let her go somewhere else, that would set her back.
Val: And then come back to the same ICU. Right? It just doesn’t make sense.
Patrik: She will bounce back in a worse condition.
Val: Right. Okay. So, just to recap, I guess, what we talked about. Number 1 is dealing with the power of attorney situation. That’s the most important thing.
Patrik: That’s the most important thing for now.
Val: Yeah. And, number 2, we’ll gather up as the medical situation. So, maybe you can draught us a letter and then we can submit that.
Patrik: Yeah. Yes. Absolutely. It would be good, Albert, if someone could send me some medical records. That would be good, so we can have a good look. It would won’t be only me. I’ve got people working with me, where we can have a look and draw out some information and then write a letter and go from there.
Lorie: Definitely will be done.
Recommended:
- Quick tip for families in ICU: Should I get access to my critically ill loved one’s medical records?
Val: Okay. So, with the medical care. And then maybe tomorrow we’ll just take a picture of her …
Patrik: Please. Picture of the ventilator. Picture of the monitor.
Val: Okay.
Patrik: It would be great to get a list of medications. It would be great to get blood results, chest x-ray results, list of medications. The more information the better.
Val: Okay.
Albert: Okay. So, I will do that. And the medication and then I’ll take a picture of that. And, if you send us, we can sign the consent that you can read and we can write the letter for us. And we’ll do that. And then as soon as we can because this people are just … Today they’re calling me and then they say, “Did you cancel the insurance?”, because that holding them to not send her. It’s holding them.
Patrik: That’s terrible.
Albert: Very terrible. Yeah. So, Patrik, after you do that, after helping us with that, what are we going to do to get after that attorney? Or what we going to do? I mean, after you have-
Patrik: Yeah. Yeah. Look, to be prepared for the worst-case scenario, and number 1, ask for the hospital discharge policy.
Albert: Okay.
Patrik: Ask for that. Number 2, you probably need to have a lawyer on standby almost.
Albert: Okay.
Val: And what type of lawyer would that be?
Patrik: You see, I couldn’t tell you whether there is medical negligence. With what you’ve shared, I can’t see that there’s medical negligence. I tell you what you might do, when you speak to a family lawyer, ask them if they know someone. You’ll probably get a better answer from them than you would get from me.
Val: Okay.
Albert: Yeah. There are malpractice lawyers too.
Patrik: Yeah. The other thing that we’ve done, and we’ve done that, whether it’s in the U.S. or in Australia, even in the UK, if … Let’s just again take the worst-case scenario. They want to kick you out on a weekend. Let’s just take that as a worst-case scenario. You could go to court and you often can go to court over the weekend with an injunction. I’ve seen that successfully. Again, it varies a little bit from state to state, but there are ways of stopping them. But now that we can anticipate that this is what they might want to do, I think having a lawyer almost on standby for the worst-case scenario is a good idea.
Albert: Yeah. Patrik, do you think they will do that before we know they’re going to send her somewhere?
Patrik: No. I’ll give you another hint. So, let’s just say they tell you by next Wednesday, “We have a bed for her in this facility.” Okay? Let’s just say they do that. Okay. Your response to that is (A), you’re not consenting. (B), you want to see the hospital discharge policy. And (C), you want to have a look at the facility yourself. Right? (D), have a look at online reviews. Those online reviews will most likely be very negative. Right? So, you can go back to the hospital, and you can say, “Look, we’ve done our research. Look at those reviews. There’s no way we are going to send my sister there.”
RECOMMENDED:
Val: See, that’s the game they’re playing though, because the good ones or the decent ones with the hospital and the doctors and things like that are not accepting. Or they’re playing the game of, “Oh, she’s on the waiting list.” Then they come up with the worst review, the worst … And then they’ll come up with one and say, “We found you one.” And then we say, “No. We’re not accepting that.” And then they’ll say, “Oh, you keep refusing. And if you keep refusing, we’ll go to court.”
Patrik: Yes, they might. But I don’t think they will be succeeding. And don’t get me wrong, a hospital going to court is also a last resort for them. It’s not that the hospital will drag you to court willy nilly. It’s a last resort for them. Just as a lawyer would be a last resort for you.
Val: Right.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!