Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tim as part of my 1:1 consulting and advocacy service! Tim’s mother had surgery, a history of COPD and is in the ICU for pneumonia and he’s asking why does the ICU team push for palliative care for his mum.
My Mother Had Surgery and is in the ICU for Pneumonia. Why Does the ICU Team Push My Mum Towards Palliative Care?
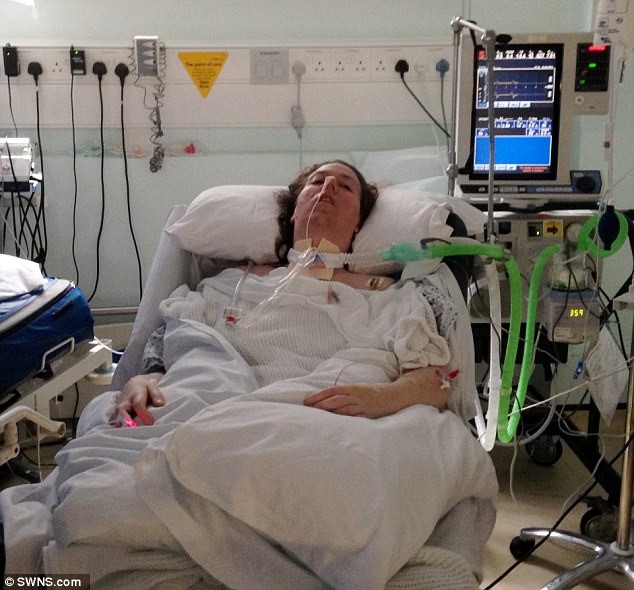
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tim here.”
Patrik: Hey, Tim, how are you?
Tim: Oh, yeah, Patrik. Sorry it’s taken so long to get back to you. Since then, I’ve been there really late and then been in there really, really early. So, my mum’s still in ICU. She’s gone to… She’s been sprinting.
Patrik: Right.
Tim: For about two days now.
Patrik: Mm-hmm (affirmative)-
Recommended:
Tim: But they’re talking about having another family meeting at 12:30.
Patrik: A meeting at 12:30?
Tim: It’s a family meeting. Yeah. And I said about moving it to another ward. I’ve just had a funny feeling. I want to take it to a palliative care ward, but she has a critical… She has that critical illness, but she’s come really far. Like, she’s moving her arms… Her fingers. She can wash her own face. She understands everything I’m saying. I had the round this morning and the doctor… We all had the same feeling. She lifted her leg up, and she’s been out in a chair every day all this week, so I haven’t been pushing to get her going.
Patrik: Is she off the ventilator?
Tim: No. That’s the problem. That’s what I’m worried about.
Patrik: So… So… Well, the bottom line is this… I mean, if she’s on a ventilator, I mean… They can’t look after her on the ward.
Tim: That’s what I thought. Or maybe saying that.
Patrik: I mean… You know… I mean. In order to, look after tracheostomy and ventilation. Somebody who hasn’t-
Who is not an ICU nurse is not qualified to do that. The chances that your mum is deteriorating on the ward is huge.
Tim: Yeah.
Patrik: Have you looked into potentially getting her private?
Tim: We did, but then the problem is, you got to get someone to admit mum in there. That’s just hard from here. But then in the ICU… Because they changed their direction after that meeting… The last time we spoke, they sort of changed direction from palliative to more corrective-
Patrik: Mm-hmm (affirmative)-
Tim: -stuff but now I think that it’s going… Honestly, we can’t be in ICU forever, but it just seems strange, because they’ve turned the temperature down to 27 on the ventilator. On the sprinting machine thing… But then they turn it back up to 36, and mom’s getting really hot and she just looks-
Patrik: Okay. So-
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Tim: I saw her this morning, and they’re saying all, “Well, that doesn’t really matter at all.” And the staff-
Patrik: It does… It does matter a big deal. So, what happens is… When somebody’s on the ventilator with a tracheostomy, the temperature needs to be around 36… 37. With the humidifier.
Tim: Oh, okay.
Patrik: If somebody… If she sprints… So, when she’s sprinting, they would put her on oxygen and take her off the ventilator right?
Tim: Yes. Yes.
Patrik: And then they can turn the temperature down to about 32, but not when she’s on the ventilator. That’s really… You can point that out to them. That’s just… All the other thing she said to you is, they’re telling it doesn’t matter… It does matter a big deal.
Tim: I’ve just got a sinking feeling the ward they’re going to move her to is a palliative care ward.
Patrik: Well, if I were you, I would… Okay. If I were you, I would do the following. I mean you… I would tell them in no uncertain terms that as long as she’s on a ventilator with a tracheostomy she needs to stay in ICU. Because on the ward, they can’t look after her.
Tim: They said… And they did say… I did say that, and just this morning, they said, “Now we’ve got doctors. We’ve got nurses and doctors there on duty”.
Patrik: No. That’s a whole lot of crap. It’s… You’re probably right that they’re moving her to a palliative care ward. You’re probably right there.
Tim: They don’t do corrective stuff in there, do they?
Patrik: No. They can’t wean her in there because the nurses are not trained to that. They’re trained to do that in ICU. I mean, they need the bed, right? That’s the reality.
Tim: Yeah.
Recommended:
Patrik: The way forward as far as I… Have you spoken to HCF anymore?
Tim: I haven’t. I sort of let it all go on the back burner because I didn’t know what was happening. There’s so much happening. I just have… I really haven’t left mum, so all of this.
Patrik: Yeah, yeah, yeah, yeah, yeah.
Tim: Sort of just ducking out now, and… So, you know… I was going to text her at night. You get a text at bloody midnight and all that. I don’t get reception in the room.
Patrik: Mm-hmm (affirmative)-
Tim: It’s like a fortress in the ICU.
Patrik: Any more talk about NFR?
Tim: NFR? I don’t know that one.
Patrik: “Not-for-resuscitation”.
Tim: No. I think that’s all going to come up today. Because I just didn’t talk to them when you said that… You said to back out… Tell them I’m not interested.
Patrik: Well.
Tim: I won’t change.
Patrik: Yeah, yeah. Yeah, yeah. They will walk… Who’s going to be in the meeting? Just you?
Tim: Me, my step-father. But he’s no good. He… He’s half the problem. The social worker told me yesterday that he… Sort of very negatively pitched her about everything.
Patrik: Right.
Tim: He doesn’t want… Well, he doesn’t want mum home unless she’s… You know… Able-bodied and everything else.
Patrik: Sure. Sure, and that may or may not happen.
Look… I give you a quick example. I had a client at Stamford, must have been about a year ago now. Must have been July last year. Where I said… Very similar situation came up. They were trying to push… It was the lady’s dad at the time. They were trying to push her dad out of ICU, and within 48 hours he passed away.
Recommended:
Tim: That’s bad.
Patrik: It’s… Look, if they’re telling you they have doctors and nurses who can look after your mum on the ward, it’s bullshit.
Tim: Really?
Patrik: Bullshit. They have nurses, but they don’t have any nurses who are ventilator-competent, or tracheostomy competent. If they do… You know… At the moment, she would be getting one-on-one nursing care.
Tim: Definitely.
Patrik: Right? So, on the ward, she will bet getting one-to-six or one-to-four, or… There’s nobody going to wean her off the ventilator. It’s not going to happen.
Tim: It only happens in ICU, does it?
Patrik: Only happens in ICU. You know, and-
Tim: Do they… Sorry, they came in before the operation. He’s actually on holiday. They tell me that he came around this morning, and I said, “Good, good.” And they said, “Probably try and get your mum moved pretty quickly. Might happen today. “And I said, “Oh. Where to?” I said, “Because I remember our last conversation. “I said, “You know… No one’s competent around… You know… This is the area in the ICU for ventilators and stuff like that. “And they said, “Oh. No. There’s the respiratory ward.” And-
Patrik: Look. Look. How mobile is your mom? How mobile is she?
Tim: She’s actually not too bad. She can move arms and her legs a fair bit now. She can wash her face. She can put her glasses on.
Patrik: Can she get out of bed? Is she getting out of bed?
Tim: Well, that’s the problem. I’ve asked them if they can sort of sit my mom on the bed. They put her in a chair and like in the last 12 days.
Patrik: Okay. That’s good.
Tim: Yeah. And she’s progressing now, her conversation. I just think another two weeks and I reckon she would be… You know.
Recommended:
Patrik: She would be off the ventilator. Potentially.
Tim: Yeah. Yeah. I honestly believe that.
Patrik: Yeah, yeah. No, no. That’s… And that’s what you should go with, that… But I can tell you… The level of care will go down big-time if she leaves the ICU. It’ll be a disaster.
Tim: Yeah. And I asked them about a… Did she get a vitamin B12 shot? Because I read some stuff that that’s good… And they were all looking at me, and then… Look. That was such a drama. They’re possibly going to do one today.
Patrik: Mm-hmm (affirmative)-
Tim: Just to sort of give her a boost up, and then- and my step dad is getting in their ear, actually.
Patrik: Right. And that’s… From my perspective, she needs to stay in ICU just simply because no matter how good their respiratory ward is… You know… Her level of care will go from one-to-one to… You know… One-to-four at the best. More likely a one-to-six, and probably a one-to-ten overnight.
Tim: Oh geeez.
Patrik: Got to rub that in their face. They’re just playing dumb. They just think you don’t know any… They… You know… They’re telling you, “Oh yeah. It’ll be same. It’ll be the same. It’ll be similar.” It’s not.
Tim: Yeah. I know it won’t be.
Patrik: It won’t be.
Tim: But then… Can they force stuff on us like that, or what’s?
Recommended:
Patrik: Okay. So, I’m… I think it will all come down to how to negotiate… How you negotiate with them. You know… If… If… I tell you something that might sound stupid, but if you think you can, you can. If you think you can’t, you can’t.
Tim: Oh. I hear what you’re saying. Yeah.
Patrik: You know. And if… And I don’t know. I can’t comment on the dynamics with your step-dad, you know? And then if he has a say there as well, that’s something I can’t comment on. If you were the only decision maker, it probably would be easier.
Tim: I think I am the only kin to her.
Patrik: Right. Right. I do believe that… They want her out of ICU because it’s a public ICU. They need the beds. I just feel very strongly that a bed in the private ICU is a way forward. You may have to ring the private ICU and ask for that. Ask whether they would have… And probably ask the question… If you have an admitting doctor in the private hospital, would they take your mum? And the… You know… And they will then ask you, “Does she have private health insurance?”
Tim: She does. Yeah. It’s reasonable.
Patrik: Though… You now… So, with that… If you have an admitting doctor, they will take your mum. There’s no doubt about that. But you will need an admitting doctor.
Tim: And that’s the only option, is it? Because it’s just-
Patrik: Um-
Tim: Apparently 31 days is what the limit is, isn’t it? So-
Patrik: Nah.
Tim: Because she’s’ reaches that, you know?
Patrik: No, no, no, no. I’ve seen… I’ve seen… She’s HCF, isn’t she?
Tim: Yeah.
Recommended:
Patrik: Yeah. I’ve seen HCF patients in ICU for six months. Who’s telling you about those 31 days? Who’s telling you that?
Tim: So, I just… I just heard from nurses.
Patrik: What do you mean by-
Tim: The nurses of someone said 31 days-
Patrik: Don’t listen to any of that garbage. There is… I’ve seen HCF patients in ICU for six months.
Look… I used to manage a couple of ICUs in the private sector in the past, right? I’ve dealt in HCF. I’ve dealt with private insurance. I’ve dealt with… If it’s clinically necessary, they’re not going to cut off ICU care. What they are doing now is, they’re cutting off the ICU bed because they need the ICU bed.
Tim: Well, it’s funny because they made a point of this. Yesterday, they said it’s a full house and they had patients’ downstairs that need to come upstairs.
Patrik: Sorry. Say that again.
Tim: They said there’s a full house. Apparently, Sunday night or Monday… Sunday or Monday night’s a really big night in ICU, and… Around here it is apparently. They said they had a full house, you know? It’s full of patients’ downstairs that are needing to get upstairs.
Patrik: So, what? So, what?
Tim: They’ve all been doing double shifts.
Patrik: Yeah, but so what? I mean, that’s not a reason to get your mum out of ICU.
Tim: No.
Recommended:
Patrik: You know? I mean, that’s… Just because… Yes, we know that’s happening. But that’s not… As long as your mum is on the ventilator, she needs to be in the ICU. I think your best way forward is to look… To go… That you can go over to the private hospital. That’s what I believe is your next step. And they will help, if you stand your ground and say, “Hey, I don’t want her to go to the respiratory ward because she’s on a ventilator.” And you will say, “But I’m considering getting her over to the private ICU.” See what they say. That would be the approach if I were you. The level of care will drop by 100%.
Tim: Yeah. So, what… I don’t have to decide and agree to anything right there.
Patrik: You have… You don’t have to do anything. You don’t. And you can… And I think you should oppose it. You should buy time. You can give them the reasons that… You know? She’s on the ventilator She can’t be looked after by people who don’t have that experience… And they know that. Yes, they may deny, but you can tell them you’ve done your research… Blah, blah, blah… You know?
Tim: I’ll tell them what what I said last time.
Patrik: You don’t need to mention anything. It’s up to you, you know? I mean.
Tim: Yeah. Well apparently, a couple of the nurses looked you up. Yeah. And they said they didn’t even know you existed. I said, “It’s really big in Victoria.” I said, “It’s bloody not that big up here at the moment, but”.
Patrik: Yeah.
Tim: They want this to make it bloody happen, but.
Patrik: Yeah. I think… I think you need to… You need to talk to the private hospital. I think you do, okay. I think… Before you go into the meeting, I would… I would talk to the private hospital. I would ring up the bed manager. If you ring up or go over… I think it’s just next door. If you go to reception-
Tim: It is.
Patrik: Yeah. If you ring up reception and say, “Hey. Can I talk to the bed manager?” Talk to the bed manager. Say, “Hey. Look, my mom is in the public hospital, but she’s got private health insurance. If I had an admitting doctor, would you take her into the ICU?” Right. And if they say, “Yes, if you have an admitting doctor we would consider that.” That’s the information I would tell the public. Does that make sense?
Recommended:
Tim: Yes. So, if they… Yeah… So, how do they… What… They must tell us what type of ward it is, do they? Because I said, “Where about?” And they said, “Level five or level four.”
Patrik: That’s not what you want to know. That’s not… You want to know what specialty it is.
Tim: Yeah. That’s it. Exactly. And another thing is… I don’t understand why… I’ll be honest with you. I don’t think they know how to wean patients.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!